Simplified Temporary Techniques for Enhanced Esthetics and Patient Satisfaction
Jeff Gray, DDS
Abstract
Before the current revolution in dental cosmetics and adhesion, the temporization phase presented many dental students with a daunting and troublesome challenge. For some practicing clinicians, it still may be the step that holds them back from enjoying the full scope of practice and feeling fully confident in their cosmetic abilities. This article will present various techniques and recommendations to alleviate the challenge and facilitate the process. The author and members of his practice's dental team have found these techniques–a compilation of knowledge the author has gained over years of study with his dental mentors–to be useful in providing satisfactory smile enhancements to their patients. The hope is that readers will find the techniques equally beneficial.
A temporary is never truly just a temporary. It leaves a lasting impression on patients about a dental professional and his or her skills. While the techniques presented in this article may be familiar to most dentists, the expectation is that some of the nuances can be employed to help refine the reader's own procedures.
Temporary Technique for Single-Unit or Small Bridge Restorations When Teeth are Intact
The first aspect to be examined will be the simple single-unit or small bridge temporary, placed either in the anterior or posterior. The advent of polyvinyl siloxane (PVS) impression materials and bisacryl temporary materialsa,b have made this a time-efficient and accurate technique that frequently can be delegated by the dentist to other members of his or her dental team.
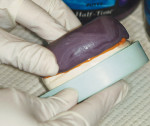
For teeth that are intact, the use of a disposable quadrant tray (ie, in the anterior or posterior) and a quick-setting PVS material (Figure 1), of which there are many available options that can be economically employed, is recommended. The steps for this technique are as follows:
Step 1: Load the side of the tray that will capture the tooth to be restored in the same manner that would be employed for an impression; load the opposing side with approximately one-half to one-third the amount of material.
Step 2: Ask the patient to gently close into this tray and wait for the material to set.
Step 3: Remove and set aside after verifying that the tooth to be restored has been fully captured. Note: the only aspects that require capturing are the opposing occlusal surfaces; these act as locators for reseating the impression at the temporization phase.
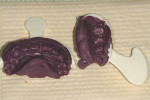
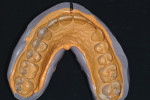
Recommendation: Store this preoperative impression in a sealed plastic bag labeled with the patient's name, date, and tooth identification. The author and his dental team store the impressions alphabetically in the laboratory until the final restoration is completed. This keeps the impressions readily available for creating a new temporary should the patient break or lose the current one (Figure 2).
Temporary Technique for Single-Unit or Small Bridge Restorations When Teeth are Broken
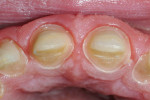
In instances when the tooth is broken, it is preferable to quickly rebuild the tooth back to its original shape using a nonbonded composite,c since this material is simple to sculpt and easy to use. Cure the nonbonded composite for five to 10 seconds so it remains slightly flexible and can be removed easily prior to placement of the rubber dam. Note: should the dentist omit rebuilding the tooth, he or she may simply prepare the inside of the impression with a round bur or diamond to simulate where the broken cusp would have been.
Recommendation: Prior to curing the composite, coat the opposing tooth with a lubricant (ie, petroleum jelly, saliva, etc.) and instruct the patient to bite together gently. This will help shape the occlusion and allow the preoperative impression to closely capture the bite.
Techniques for Temporization
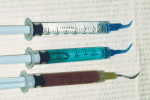
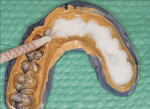
Temporization occurs once the preparation, impression, and bite registration steps have been completed. The steps involved for this process include scrubbing with over-the-counter (OTC) peroxide using a syringe with fuzzy tipsd (Figure 3), then rinsing with water and drying thoroughly. Note: should the tissue still bleed, it is recommended that a ferric sulphate solutione be used at the gingival margin before re-scrubbing with peroxide and re-rinsing with water.
Recommendation: If a composite build-up is used to restore the tooth, the area should be re-prepared, since there may be uncured resin on the surface that can attach to the temporary, making removal difficult.
At this point, the dental professional should instruct the patient to practice closing into the preoperative impression before loading the temporary material into it. This will ensure that both the patient and the assistant are comfortable with the positioning while the patient is numb. It is always helpful to view the opposite side of the mouth to ensure the patient is fully closed.
Load the impression with the desired shade of temporary material (ie, about three-quarters full) and reseat in the mouth; have the patient gently bite together. After approximately three to four minutes, instruct the patient to open. The temporary should still be in place on the tooth.
Gently tease the acrylic off the tooth or out of the impression, if it remains there. Begin the trimming and polishing, as per standard protocol. As a result of an accurate preoperative impression, a minimal amount of work should be required to accomplish these tasks. Any voids or irregularities that may be present can easily be filled in using a flowable composite of similar shade, then light cured.
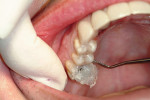
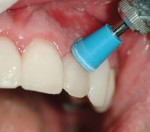
Prior to verifying the occlusion, the teeth surrounding the prepared tooth should be checked for any thin layers of flash temporary material; if any are present, they should be removed (Figure 4).
Before cementing the temporary, clean the preparations according to the previously described process using peroxide and water. Once the tooth is clean and dry, flood the tooth with chlorhexidine from a syringe and dry thoroughly. Note: do not rinse; this allows an antibacterial agent to remain active on the tooth to help prevent the formation of the benign but unattractive black substance that occasionally appears under temporaries.
Cement the temporary according to standard protocol. For posterior teeth, use either a typical cementation productf or a clear, light-cured material.g
Veneer, Full-arch, or Full-mouth Temporaries
It is beyond the scope of this article to discuss how to find the bite to restore the patient's condition or select the position in which to restore the patient. The important tenants in all occlusal philosophies are to keep the patient comfortable, ensure proper function and joint stability, establish that the teeth exhibit equal intensity with bilateral posterior contacts, and promote esthetics of the restorations.
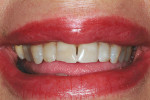
Esthetic anterior temporaries can provide a sense of excitement for the patient while also building confidence in the dentist's skills. Temporaries provide a "trial smile," a term the author first became familiar with at The Las Vegas Institute (LVI) in 1995 through the teachings of Dr. Bill Dickerson and Dr. David Hornbrook. One of the numerous advantages of the "trial smile" is that it enables patients to essentially "test drive" the new look of their smile (Figure 5).
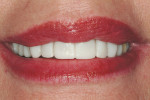
For cosmetic cases, the use of a preoperative wax-up made from PVS impressions is highly recommended. Also, preoperative photographs are essential for the dental professional and the laboratory. At a minimum, images of a full-face smile and close-up smile will be required (Figure 6 and Figure 7). These visual aids will assist the dentist in deciding where to place the maxillary incisal edge. This parameter will also guide the laboratory regarding what length to make the central incisors in the wax-up. In this author's opinion, the maxillary centrals are key to cosmetic success and, according to Dr. John Kois, "step one" in treatment planning.
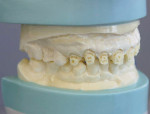
Recommendation: After duplicating the original models or repouring the preoperative impression, the dentist should save the original models for use as a preparation guide, as well as for the practice's records. Instruct the laboratory to gently score the gingival margins and clean out the interproximal areas. The slightly deepened or scored gingival area is necessary to ensure a tighter fit of the putty stint at the marginal area, thereby minimizing excess flash during the fabrication of the temporaries. This simple recommendation will save the dentist or dental assistant significant time during the cleanup and polishing of the temporaries and help ensure enhanced gingival health for the patient. It is also important that the laboratory place some retentive areas in the stone to help secure the wax during stint fabrication (Figure 8 and Figure 9). For full-mouth or full-arch cases, it is important that the laboratory not trim away the tissue behind the posterior tooth and the palate, since these areas will act as the tissue stops and aid in seating the tray properly. No tray is used with this technique; the putty matrix acts as the tray and remains slightly flexible so it can easily be removed from the mouth.
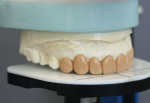
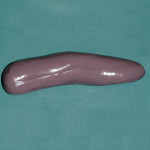
Employing one of the numerous putty wash-type materials available on the market today, a putty hot dog is made and contoured over the wax-up (Figure 10 and Figure 11). This stint will normally be 3.0 mm to 5.0 mm thick. Once the material has set, gently remove it from the model. Now use the wash material and fill the stint approximately two-thirds full and re-seat it on the wax-up; remove and trim any excess when set (Figure 12).
A highly accurate impression of the wax-up is now available. A superior wax-up and tray will allow the dental professional to fabricate esthetic and accurate temporaries in a short period of time. As previously recommended, place the stint in a sealed bag and store it until you have delivered the case. After the dental professional has prepared, impressed, and taken the bite, face bow, and stick bite, he or she is ready to fabricate the temporaries.
Step 1: Rinse and scrub the teeth as previously described. Should the tissue still be seeping or bleeding, this must be addressed and managed. A ferric sulphate solution works well, but it needs to be rinsed thoroughly or it may contribute to the black substance that sometimes forms under the temporaries. Another option that does not contribute to black substance formation is to utilize 35% hydrogen peroxidei; apply this to a small cotton ball and dab or press into the seeping areas. This technique does produce some transient white gums, but these fade within five to 10 minutes, leaving a clean surface. Note: blood, saliva, or ferric sulphate solution on the tooth surface are typically the main causes of the black substance.
Step 2: After rinsing and gently drying, flood the tooth with 2% chlorhexidine gluconatej from a syringe and air dry, but do not rinse. This leaves a layer of antibacterial agent on the tooth that will decrease sensitivity, as well as reduce the likelihood of forming the black substance, without affecting the bonding strength.
Step 3: After marking the midline, practice placing the tray in the mouth until comfortable with the placement (Figure 13).
Step 4: Fill the tray approximately three-quarters full with the material of choice in the desired shade and seat the tray in the mouth (Figure 14). Fill only the area of teeth that are being temporized; allow this to set in the mouth for three to four minutes. It is helpful to squirt a small dab of the material out on a pad and use that as a guide to verify the set so as not to remove the tray before the proper amount of time has elapsed.
Step 5: This is a "shrink wrap" technique and, in most cases, the dental professional will not be removing the temporaries from the mouth; the temporaries will be left in place and not cemented. For today's highly conservative veneer preparations, this technique helps create durable and retentive temporaries. As previously noted, a temporary is not really temporary, but leaves an enduring impression with the patient about the dental professional and his or her skills.
Step 6: Remove the tray by pressing on the lingual or palatal side and gently peeling open the facial (Figure 15). If a bubble or defect is present, the dental professional can simply use a flowable composite of similar shade to quickly repair the area. Should the material become dislodged at this time or during the period the patient wears the temporaries, the temporaries can simply be re-cemented using one of the light-cured temporary cements or a flowable composite.
Step 7: Check for a thin layer of material on the palate, the lingual surface of veneer preparations, and unprepared teeth. To trim the margins or to open any interproximals, the use of a flame-shaped, fluted carbidek is recommended. Applying only minimal pressure to avoid damaging the margins, clean away any excess with a light sweeping motion. Magnification is helpful for this step.
Step 8: Check the bite and then smooth and polish, as per the usual protocol. Note: the author uses a blue composite polishing cupl to fully smooth the margins and refine any other areas (Figure 16). Examine the patient's smile (Figure 17).
Step 9 (Critical): For any veneer case, provide the patient with an irrigatorm and several bottles of solution.n Instruct the patient to use several times a day with warm water and about one to two ounces of the solution in the reservoir. Note: the cost of the irrigator (ie, approximately $80) can be built into the practice's case fee; this price is well worth the savings in bonding time and aggravation, as well as in patient satisfaction with the result–tissue that comes back firm, pink, and healthy (Figure 18).
Conclusion
The objective of this article has been to help dental professionals simplify their techniques for temporaries. Recommendations were offered to aid them in making their practices more enjoyable and predictable when employing the fabrication of temporaries as a tool for creating lasting impressions among patients of the dentist and his/her team and skills.
Acknowledgments
The author wishes to thank his mentors–Dr. Ray Bertolotti, Dr. David Hornbrook, Dr. Bill Dickerson, and Dr. John Kois–to whom he owes a great debt of gratitude; and his talented, carefully trained, and licensed team: Suzanne Gittins, Carla Gomez, and Darcy Hawkins. He also extends thanks to Mike Milner Dental Ceramics for fabricating the wax-ups and restorations featured in this article.
a PERFECTemp II, Discus Dental, Culver City, CA b Luxatemp®, DMG, Hamburg, Germany c Clearfil Photo Core, Kuraray America, Inc., New York, NY d Ultradent Products, Inc., South Jordan, UT e Astringedent, Ultradent Products, Inc., South Jordan, UT f Tempbond®, Kerr Corporation, Orange, CA g Systemp, Ivoclar Vivadent, Inc., Amherst, NY h Panadent Articulator, Panadent Corporation, Grand Terrace, CA k flame-shaped 7901 fluted carbide, Patterson Dental, Milwaukee, WI l Polishing Cup, Cosmedent, Inc., Chicago, IL m The OxyCare™ 3000, Oxyfresh Worldwide, Inc., Coeur d'Alene, ID
n Oxyfresh solution, Oxyfresh Worldwide, Inc., Coeur d'Alene, ID
About the Author
Jeff Gray, DDS
Clinical Instructor, the Kois Center
Seattle, Washington