The Gingiva and Direct Bonded Restorations: Maximizing Your Esthetic Result
Francis G. Serio, DMD, MS, MBA
Abstract
There is more to esthetic dental treatment than the restorative dentistry component alone. This article focuses on the gingiva in the esthetic zone and discusses the manner in which proper attention to the soft tissues will enhance esthetic restorative therapy.
Analysis of the esthetic zone is a complex task. Characteristics and interactions of the teeth, gingiva, lips in repose and movement, as well as the shape of the face, must all be considered. During the early years of development of anterior esthetic restorative techniques, the focus was understandably on materials and how these related to the natural teeth. One of the classical textbooks on esthetic composite bonding made minimal mention of the restoration-gingiva interface.1 In recent years, publications related to anterior direct composites and porcelain laminate veneers have spent considerably more time discussing the importance of the gingiva to the overall result.2,3
The gingiva serves, in effect, at the pleasure of the dentition. First, the characteristics of the teeth have to be determined or planned for, and then the gingiva may be evaluated for its supportive esthetic role. Primacy in planning are given to analysis of the Golden Proportion of the central incisor, lateral incisor, and canine; angulation of the canines relative to the contours of the face, incisal edge length, and relationship to the lower lip line; and spacing or correction thereof. Decisions regarding the soft tissues subsequently follow. Failure to account for the principles of size, shape, and location of the gingiva will lead to an unacceptable result.
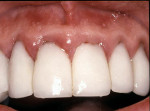
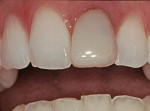
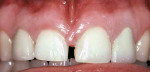
Gingival problems related to poorly contoured restorations may present (Figure 1). In this example, the gingival papilla between the maxillary right central incisor and lateral incisor does not have sufficient volume of embrasure space to exist, the gingival margins are rough and act as plaque retentive areas, and the contact between the central incisors is not properly contoured. It is a challenge for the patient to maintain gingival health with these problems. Even with more esthetic restorations, the inflammation would detract from the final presentation. When anterior direct composite restorations are placed in the presence of inflammation such as that which is evident in this particular case, achieving a good gingival seal may be impossible. The lack of adhesion at the gingival margin will eventually lead to marginal leakage and discoloration of the gingival margin of the restoration (Figure 2).
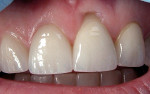
It is also important to consider the thickness of the gingival margins. This thickness will play a role in how much trauma the gingiva can withstand during tooth preparation without ultimately causing recession. While it is critical to achieve a good seal and contour of the restoration at the margin, thin gingiva is more prone to recession, even with relatively minor trauma (Figure 3).
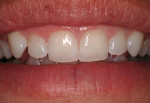
It is incumbent upon the clinician to assess the location of the gingival margins relative to the cementoenamel junction (CEJ) of the teeth and to each other before placing anterior esthetic restorations. The natural relationship of the gingival margins of the central incisor, lateral incisor, and canine are such that the margins of the central incisor and canine are at the same level and the margin of the lateral incisor is either at the same level or 1 mm to 2 mm coronal to the other margins.3-5 An apical location of the gingival margin of the lateral incisor will be unpleasing to the eye (Figure 4).
The natural ratio of the width to height of the maxillary central incisor is approximately 0.8, or the average width of the central incisor is 8 mm, with a height of 10 mm.4 Sometimes teeth look boxy, short, and fat because the clinical crown does not reflect this ratio (Figure 4). Short crowns may result from incisal wear, altered passive eruption, or both; the latter is the case in this example. Lateral tooth dimensions may fit the Golden Proportion, but the teeth still do not appear correct due to this alteration of the clinical crowns.
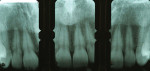
Periodontal surgery may easily correct altered passive eruption (Figure 5a). First, the approximate length of the anatomic crown of the central incisors may be determined utilizing periapical radiographs. This measurement is compared to the clinical crown to determine how much visible crown may be gained (Figure 5b). The patient can be given some indication of the final result using either a diagnostic wax-up or diagnostic digital imaging. Usually, an apically positioned flap with ostectomy and osteoplasty is performed to achieve the desired crown height. Only when the CEJ can be felt with the tip of a periodontal probe preoperatively should a gingivectomy be considered as a definitive treatment. Upon completion of the esthetic crown lengthening procedure, the anterior teeth will have the correct dimensions for the restorations (Figure 5c).
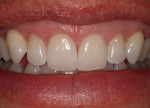
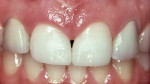
On occasion, compromise is necessary based on patient circumstances. For example, a patient presented who was dissatisfied with the appearance of her diastema (Figure 6a). Ideal therapy would include orthodontics to close the diastema, a frenectomy after the completion of the orthodontics but while the teeth are in fixed retention, and subsequent esthetic restorations. In this instance, however, the patient had crowns that had been recently placed on bilateral peg lateral incisors, so she opted for the frenectomy and direct anterior composite bonding to close the diastema. While much could be said about the dimensions of the central incisors and the lack of adherence to the Golden Proportion, the patient was satisfied with the result (Figure 6b). This case illustrates two basic principles: in esthetic dentistry, patient expectations and satisfaction are paramount and may not adhere to established norms; and comprehensive treatment planning of the entire esthetic zone—not piecemeal treatment—would have produced a more balanced appearance.
Conclusion
Understandably, anterior esthetic treatment is based on the proper execution of esthetic restorations. Attention to the health, biology, and contours of the gingiva will bring that added measure of confidence to produce esthetic results with which both patients and practitioners will be pleased.
References
1. Jordan RE. Esthetic Composite Bonding: Techniques and Materials. St. Louis, MO: Mosby Year Book; 1993.
2. Demirel K, Gürel G. Periodontal considerations in esthetic treatment planning. In: Gürel G, ed. The Science and Art of Porcelain Laminate Veneers. Chicago, IL: Quintessence; 2003:207-230.
3. Gürel G. Smile design. In: Gürel G, ed. The Science and Art of Porcelain Laminate Veneers. Chicago, IL: Quintessence;2003:73.
4. Chiche GJ, Pinault A. Esthetics of Anterior Fixed Prosthodontics. Chicago, IL: Quintessence;1994.
5. Wheeler RC. Complete crown form and the periodontium. J Prosthet Dent. 1978;39:502-504.
About the Author
Francis G. Serio, DMD, MS, MBA
Professor and Chairman, Department of Periodontics and Preventive Sciences
University of Mississippi School of Dentistry
Oxford, Mississippi