Lyon College officially finalized locations for its School of Dental Medicine and School of Veterinary Medicine in Little Rock and Cabot respectively. Renovation and construction on both campuses is scheduled to commence this year, with the Lyon College School of Veterinary Medicine and Lyon College School of Dental Medicine expected to enroll their inaugural classes in the fall of 2025 and summer of 2025 respectively.
“After thorough consideration, the Lyon leadership decided to split the vet and dental schools based on proximity to related entities,” said Dr. Melissa Taverner, president of Lyon College. “The dental school in Little Rock will be located close to existing medical institutions; and the veterinary school in Cabot will be located adjacent to the planned Cabot Animal Services Center and will have space for future programmatic expansion. We are beyond thankful for the time and collaborative efforts of so many who worked in good faith to open these schools.”
The Lyon College Faculty Assembly and Board of Trustees approved proposals to develop dental and veterinary schools in March 2022. In November 2022, the Higher Learning Commission Institutional Actions Council approved the college’s requests to offer the Doctor of Veterinary Medicine and Doctor of Medical Dentistry professional degrees. The college is pursuing accreditation with both the American Veterinary Medical Association’s Council on Education and the American Dental Association’s Commission on Dental Accreditation.
“As Lyon College continues to expand its academic offerings and strengthen its footprint as a leader in higher education, these new schools will play a vital role in shaping the future of healthcare in Arkansas and beyond,” said Victor Werley, Lyon College Board of Trustees chair. “We could not be more excited to be establishing a presence at two thriving locations in central Arkansas.”
For more information about Lyon College and its upcoming initiatives, please visit lyoninstitute.com.
Lyon College School of Dental Medicine
Lyon College, working in tandem with its Little Rock partners, has announced the Lyon College School of Dental Medicine will be located at 5 Allied Drive in Little Rock’s Riverdale neighborhood.
“We are excited to welcome the Lyon College School of Dental Medicine to Arkansas’s capital city, where it will be an excellent addition to a world-renowned medical ecosystem that serves the entire region,” said Frank Scott, Jr., mayor of Little Rock. “It has taken a total team effort among city officials, business and community leaders and developers to bring the state’s first dental school to Little Rock. I appreciate Lyon College for its partnership and commitment and look forward to the arrival of the first class of students in fall 2025.”
The Lyon College School of Dental Medicine will occupy floors 1-6 and 12 in Riverfront Plaza Building 5, which formerly housed Arkansas Blue Cross and Blue Shield offices. The building will be renovated to include space for classrooms, offices, and patient care and simulation clinics.
“We are honored to work with Lyon College to locate the state’s first and only Dental School,” said Kevin Huchingson, chairman and CEO of Colliers | Arkansas. “The building and location are perfectly situated for future students and faculty, and we look forward to helping Lyon build this into a state-of-the-art educational facility.”
“Recognized as the state’s hub for healthcare, Little Rock offers unparalleled opportunities for students to gain practical experience and expertise in oral health and dental medicine,” Taverner said. “We are excited to work with our many partners in Little Rock to bring the Lyon College School of Dental Medicine to fruition. Specifically, I want to thank the team at Colliers for securing this facility, and I want to thank our friends at the City of Little Rock, the Little Rock Regional Chamber of Commerce, the Downtown Little Rock Partnership and the Clinton Foundation for their efforts to open this school in Little Rock.”
In 2022, Lyon College signed a memorandum of understanding with the University of Arkansas for Medical Sciences to foster joint efforts in both entities’ respective missions and identify opportunities for joint teaching, research, graduate education and professional development to benefit students and faculty. Lyon College is also partnering with the Arkansas Department of Health and Arkansas Oral Health Coalition to increase awareness of oral health in Arkansas.
“While our location is changing, our commitment to Arkansans remains the same. We remain committed to addressing the oral health needs of the underserved across Arkansas and I am excited about the new possibilities that this location offers us to positively impact the community, improve oral health literacy, and increase access to quality oral health care,” said Dr. Burke Soffe, founding dean of the dental school. “Lyon College’s new school will feature cutting-edge facilities equipped with advanced technology, fostering innovation and collaboration among students and faculty.”
In March, Sen. John Boozman championed a $15 million federal appropriation for the Lyon College School of Dental Medicine. The college has also worked with the Arkansas dental community to secure educational support for the school.
Lyon College School of Veterinary Medicine
Lyon College and the City of Cabot announce that the Lyon College School of Veterinary Medicine will be located on a newly formed multi-acre campus located at Exit 21 in Cabot, adjacent to Game Time at The Grounds city park. The Cabot Animal Services Center will also be constructed on this campus, which will help aid in the school accreditation process.
In the plan approved by the Cabot City Council Monday, Cabot will lease facilities to Lyon College to develop the veterinary school.
“The City of Cabot is thrilled to welcome Lyon College's School of Veterinary Medicine to our community,” said Ken Kincade, mayor of the City of Cabot. “Cabot’s commitment to fostering excellence in education and healthcare aligns perfectly with Lyon's mission. Together, we are creating a hub for veterinary excellence that will not only benefit our residents and animals but also contribute to the advancement of veterinary medicine regionally and beyond. This will be the first graduate program for veterinary science in the state of Arkansas, and we are proud to have it here in Cabot.”
“Cabot offers a dynamic community and access to diverse ecosystems, providing an ideal setting for students,” said Taverner. “With outstanding facilities and a commitment to excellence, the Lyon College School of Veterinary Medicine will prepare future veterinarians to address the evolving challenges in animal health and care. We are extremely grateful to the city council, Mayor Kincade and our partners in Cabot for making the school a reality.”
Last year, the City of Cabot and Lyon College signed a memorandum of understanding signifying the commitment of both institutions to collaborate on community outreach, educational programming and the provision of care and support services at the City of Cabot Animal Services Center.
“As a veterinarian devoted to this profession and veterinary dean, I find Arkansas’s enthusiasm for the new veterinary school truly heartwarming,” said Dr. Eleanor Green, founding dean of the Lyon College School of Veterinary Medicine. “We had previously signed an MOU with Cabot for a mutually beneficial relationship to support its Cabot Animal Support Services where veterinary students would experience immersive learning opportunities. The plan is for Lyon College students to have access to hands-on experiences in animal care, health management and community engagement, contributing directly to the welfare of animals and residents in Cabot. The location in Cabot provides the ability to construct a large barn and classroom space that will allow expansion of outreach to students and civic groups across the state.”
“We are excited to see Lyon College's School of Veterinary Medicine become a reality in our community,” said Alicia Payseno, director of economic development for the City of Cabot. “This partnership signifies a significant step forward in Cabot's commitment to education, healthcare and economic growth.”
About Lyon College
Lyon College, a private, liberal arts institution founded in 1872, is the oldest college in the state with its original charter. Ranked by US News & World Report as a 2023 “Best College,” Lyon currently enrolls almost 600 students from 26 states and seven countries. Students can tailor their education, selecting from 24 majors as well as select graduate, pre-professional, and individualized options. Learn more at lyon.edu.





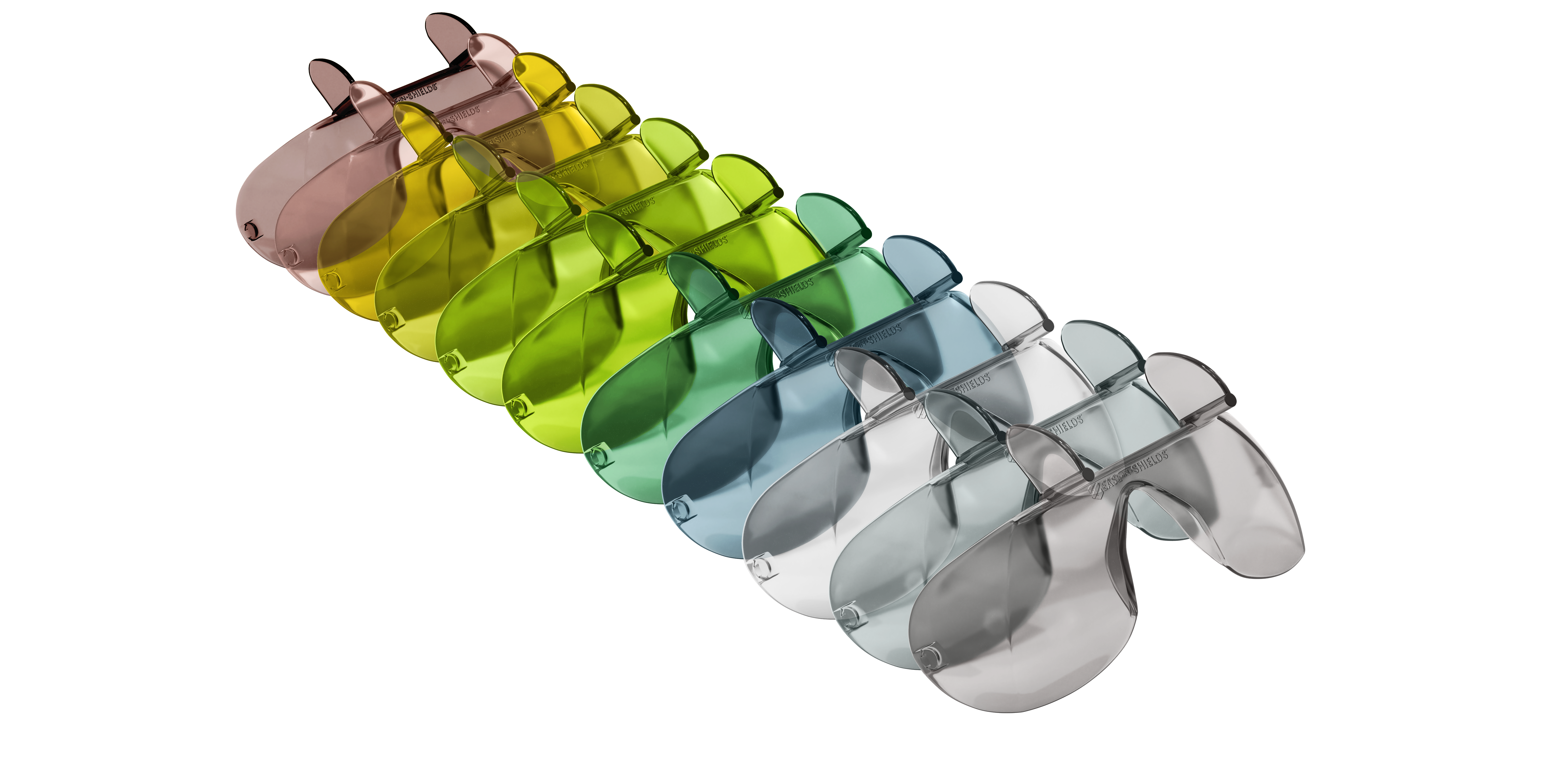 Ultradent proudly announces the acquisition of Ease-In-Shields™ from ViewMax Solutions, LLC. Ease-In-Shields provides unique eye protection for laser and curing light users, with their double patented shape, allowing the shields to fit into most loupe and eyewear shapes for maximum safety.
Ultradent proudly announces the acquisition of Ease-In-Shields™ from ViewMax Solutions, LLC. Ease-In-Shields provides unique eye protection for laser and curing light users, with their double patented shape, allowing the shields to fit into most loupe and eyewear shapes for maximum safety.

 Synergy Dental Partners
Synergy Dental Partners
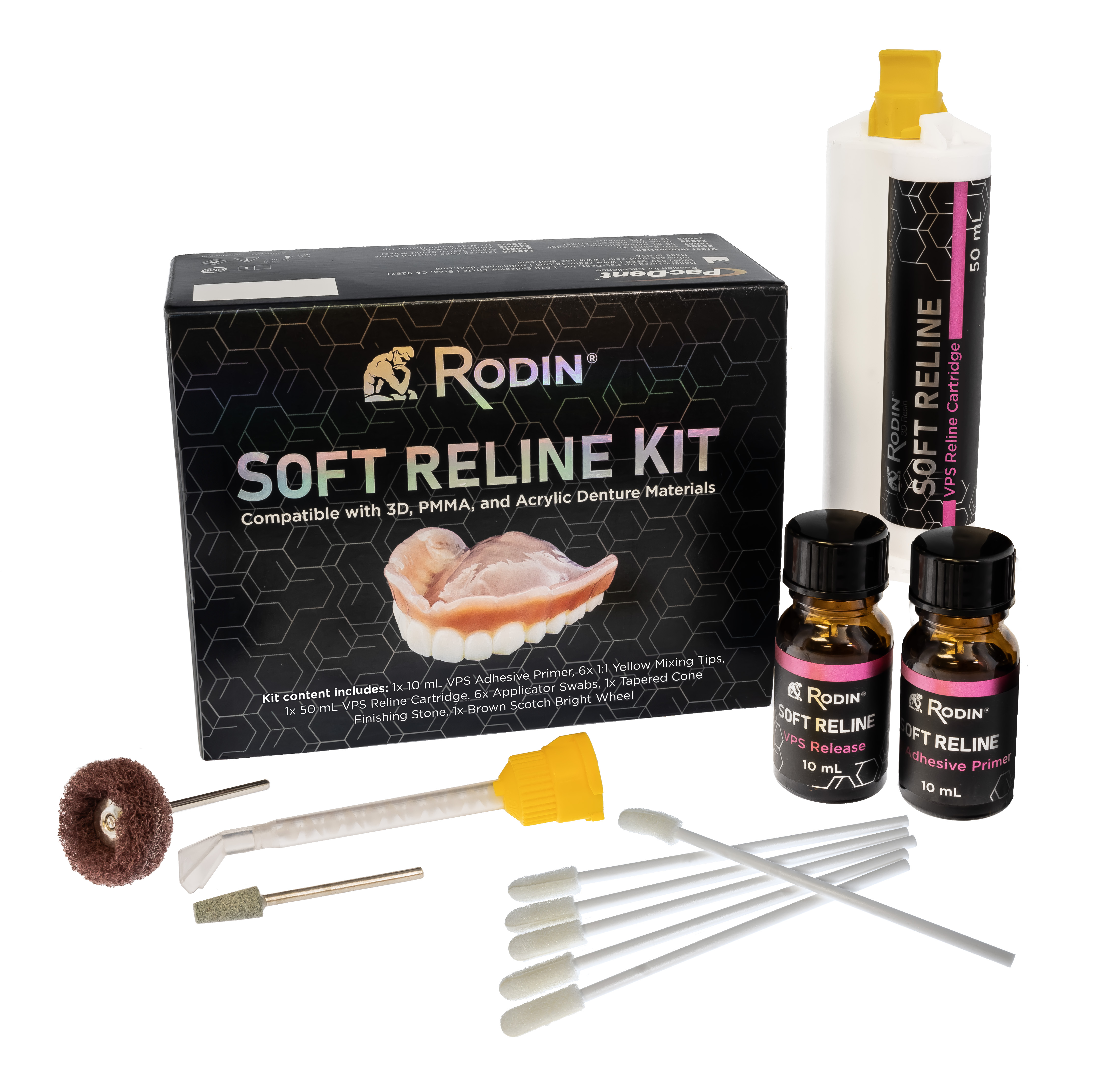 Pac-Dent, Inc. is excited to announce two expansions to its innovative line of Rodin® 3D Resin Printing Materials: Rodin® Soft Reline and Rodin® Flexisplint. These products signify our commitment to the continued integration of innovative products into dental workflows.
Pac-Dent, Inc. is excited to announce two expansions to its innovative line of Rodin® 3D Resin Printing Materials: Rodin® Soft Reline and Rodin® Flexisplint. These products signify our commitment to the continued integration of innovative products into dental workflows. Rodin® Flexisplint seamlessly integrates esthetics, durability, and user-friendliness with exceptional flexibility to ensure a snug, comfortable fit that minimizes discomfort and enhances the patient's overall experience. These characteristics create an ideal candidate for printing comfort night guards, occlusal bite splints, and snoring appliances.
Rodin® Flexisplint seamlessly integrates esthetics, durability, and user-friendliness with exceptional flexibility to ensure a snug, comfortable fit that minimizes discomfort and enhances the patient's overall experience. These characteristics create an ideal candidate for printing comfort night guards, occlusal bite splints, and snoring appliances. Founded by a team of industry pioneers, OrthoFX™, announced the new generation of advanced clear aligner polymer, NiTime™ Clear Aligners. NiTime is the first and only clear aligner system explicitly designed for shorter wear time and cleared by the U.S Food and Drug Administration (FDA) 510(k), and is now available nationwide for doctors to treat all classes of dental malocclusions. OrthoFX will showcase the new breakthrough material at the AAO (American Association of Orthodontists) Annual Meeting in New Orleans, May 3-6, 2024.
Founded by a team of industry pioneers, OrthoFX™, announced the new generation of advanced clear aligner polymer, NiTime™ Clear Aligners. NiTime is the first and only clear aligner system explicitly designed for shorter wear time and cleared by the U.S Food and Drug Administration (FDA) 510(k), and is now available nationwide for doctors to treat all classes of dental malocclusions. OrthoFX will showcase the new breakthrough material at the AAO (American Association of Orthodontists) Annual Meeting in New Orleans, May 3-6, 2024. 3Shape launches Unite 3rd Generation, allowing dental professionals to access and work with their digital impressions and patient cases anywhere, anytime, via any mobile, tablet (Android, iOS), or web device. This update enables seamless and secure cloud storage for all 3Shape TRIOS intraoral scans and patient data.
3Shape launches Unite 3rd Generation, allowing dental professionals to access and work with their digital impressions and patient cases anywhere, anytime, via any mobile, tablet (Android, iOS), or web device. This update enables seamless and secure cloud storage for all 3Shape TRIOS intraoral scans and patient data. Synchrony (NYSE: SYF), a consumer financial services company, today announced a multi-year renewal with
Synchrony (NYSE: SYF), a consumer financial services company, today announced a multi-year renewal with 
