Perfecting the Assistant-Driven Class II Composite
Empowering dental assistants to perform this work benefits patients and practices alike
In a growing number of states, dental assistants are being allowed to place restorative materials. There is no doubt that a properly trained dental assistant with the right tools should be able to be successful in placing a restoration.
That being said, the Class II composite resin restoration was, for many years, difficult for experienced dentists to place. However, recent improvements in the materials and tools used in placing Class II resins have dramatically changed and improved. Now it is possible for dental assistants to achieve the same successes they have in placing Class II amalgams with Class II resins.
The following is a review of the latest tools and materials available that can be valuable in aiding dental assistants in improving the quality and consistency of placing their Class II composite resins.
Isolation
The first critical step when restoring a Class II restoration is proper isolation. Contamination with blood or saliva will virtually guarantee the failure of a composite resin restoration.
The universal standard of care is the use of a rubber dam (Figure 1). A rubber dam, when properly placed, will help ensure that saliva and blood will not seep into the restorative field.
Other alternatives to the rubber dam can work to provide excellent isolation. The Isolite system (Isolite Systems, isolitesystems.com) has demonstrated to be very effective at preventing salivary flow into the restorative field. In addition, it provides light, suction, and a bite block, making it a popular product with dental professionals.
The biggest benefit for use of a rubber dam or an Isolite for the dental assistant who is placing the restoration is that it functions similarly to a second pair of hands. Cotton roll isolation is challenging if, for no other reason, that when the dental professional turns to pick up an instrument, restorative material, or curing light, the patient can close the mouth or move the tongue and contaminate the restoration.
Matrix Systems
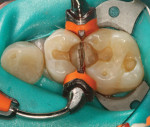
An excellent matrix system is critical for the clinical success of a Class II composite. Recently two sectional matrix systems have been introduced that can help improve the success rate of Class II resin restorations. The Garrison Composi-Tight® 3D ( garrisondental.com) (Figure 2) and the Triodent V3 and V4 (Triodent, triodent.com) (Figure 3) systems have helped to make Class II restorations more predictable. Each system consists of a sturdy ring clamp that helps to obtain intimate adaptation of the matrix to the prepared tooth, as well as provide separation between the teeth. This allows for a consistently tight proximal contact. In addition, each system provides an anatomically correct matrix band that allows for proper emergence angles and placement of the proximal contact in the proper area of the tooth.
Many options with wedges are available. A modern version of a traditional favorite is the Contoured Wooden Wedges by Clinician’s Choice (Clinician’s Choice, clinicianschoice.com). Triodent and Garrison include well-designed plastic wedges in their matrix system kits.
Bases or Liners
The purpose of a base or liner with a Class II composite is to provide thermal protection of the pulp and/or to medicate the pulp should the preparation be in close contact with the pulp.
For many years, glass ionomers have been used for liners under composite restorations. Glass ionomers are placed before the bonding process. This can be done because glass ionomers have a slight adhesion to dentin. In addition, glass ionomers are gentle to the pulp, can provide a level of thermal insulation, and will release some fluoride. GC America ( gcamerica.com) has a line of products that can be used as a base and has been a market leader in this area for years. Also, SDI ( sdi.com.au) and 3M ESPE ( 3mespe.com) have popular glass-ionomer liners.
In the past, a calcium hydroxide paste (Dycal®, DENTSPLY, dentsplymea.com) has been used under amalgams, especially when a preparation was close to the pulp. This is called an indirect pulp cap. The idea is that the calcium hydroxide would act as a mild irritant to the pulp and would stimulate the pulp to create dentin in the area where it was close to a pulp exposure. However, when using composite, a calcium hydroxide paste does not work well.
Recently, Bisco (bisco.com) has introduced TheraCal LC®. This product is a resin-modified calcium silicate that releases calcium that will stimulate the formation of dentin, and an alkaline pH that can promote healing and will act to provide thermal insulation. Although still a new product, the results from the research are looking very favorable. Clinically, when the dentist sees that the caries is close to the pulp and is concerned with the proximity to the pulp, he or she may direct that a liner such as TheraCal LC is used.
In the past year, Voco (voco.com) has brought Calcimol LC to market. This product appears to have similar properties to TheraCal LC and may be worth researching as another option as a liner under composite restorations.
Bonding Systems
Numerous bonding systems are on the market. What the dental assistant uses will be at the doctor’s discretion. However, it is important to understand the basics of the different bonding systems. Bonding systems can be divided into 3 basic systems: total-etch, self-etch, and universal.
Total-etch systems involve the use of phosphoric acid to prepare the preparation to receive the bonding resin. The important part of a total-etch system is to know that the tooth preparation needs to be etched for only 15 seconds, and then requires the etch to be completely cleaned off. The other critical aspect is to understand that after the etch is rinsed away, the preparation needs to remain moist. That means that no or very minimal air is used after the rinse. Ideally, the excess water is removed through what is taken away with the high-speed suction. Over-etching or over-drying at this step can potentially lead to postoperative sensitivity. Popular examples are: OptiBond FL® and OptiBond Solo Plus™ by Kerr ( kerrdental.com), Prime & Bond® NT™ by DENTSPLY Caulk, All-Bond by Bisco (Bisco.com), and Adper™ Scotchbond™ MultiPurpose by 3M ESPE.
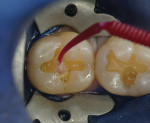
A self-etch system does not have the phosphoric etch step. These bonding agents are popular because of a historical reputation of not causing postoperative sensitivity. These systems rely on the application of a very weak acid within the bonding liquid to provide for the mechanical and chemical retention of the bonding agent to the tooth (Figure 4). Critical here is that the directions are followed exactly. The chemistry in each product is slightly different, so adherence to the companies’ protocols is paramount. Popular examples are: Adper Prompt™ L-Pop™ by 3M ESPE, Clearfil™ Liner Bond 2V by Kuraray ( kuraraydental.com), Futurabond® DC by Voco, and iBond® by Heraeus Kulzer (heraeus-kulzer-us.com).
A new category of bonding agents has been recently introduced; universal bonding agents give the doctor the ability to decide whether he or she wants to etch the tooth preparation while still being able to use the same product. This would look to be the direction of the future of bonding agents. A universal bonding agent will enable the dentists to choose to use phosphoric etch without having to bring a different product out of the drawer. While testing appears promising, it is important to understand that this is still an emerging category and long-term results are yet to be known. All-Bond Universal by Bisco, Prime & Bond Select by DENTSPLY Caulk, and Adper Scotchbond Universal by 3M ESPE are examples of universal bonding agents on the market.
Composite Resins
The keystone to the Class II composite restoration is the composite itself. Volumes could be written about composite resins and the techniques involved. For the purposes of this discussion, we will limit our focus to the use of the popular category of bulk-fill composites.
Bulk-fill composites have become popular because of the simplicity of the technique and the increased speed in which the composite can be placed. Previous concerns regarding the use of a bulk-fill technique have been addressed, and today, this category of materials is seeing increased popularity. The ability to cure as deep as 4 mm and the reduction in polyermization shrinkage now allows for composite to be placed in bulk similar to an amalgam-like technique. This more simplified technique allows for this to be a more “assistant friendly” procedure.
Many companies now offer bulk-fill composites. SureFil® SDR® by DENTSPLY Caulk, Tetric EvoCeram® Bulk Fill by Ivoclar Vivadent (ivoclarvivadent.us), and Venus® Bulk Fill by Heraeus are some popular examples.
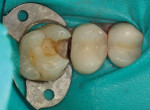
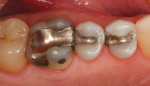
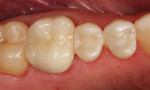
In our office, the material that we use most frequently and the one that the assistants enjoy working with is SonicFill™ by Kerr. SonicFill is unique in that the composite is sonically activated in a special handpiece. The sonic activation creates a flow characteristic in the material that makes it easy to place and manipulate while getting excellent marginal adaptation. Then once in place, it starts to change from a consistency of a very thick flowable composite to that of a more traditional composite allowing for contouring of the material before the final cure. Figure 5 and Figure 6 are the before and after of a SonicFill restoration that was placed by one of our expanded-duty dental assistants.
In our office, we have found the combination of a Garrison or Triodent matrix, the Bisco All-Bond Universal bonding agent, and the SonicFill composite to work best for us.
Finishing and Polish
Once the assistant has fully polymerized the composite with the curing light, the dentist will perform the final occlusal adjustments. Typically, most of this contouring is conducted with a football-shaped 12- or 16-fluted carbide. To further develop more anatomic detail, a R.A.P.T.O.R.® bur (Axis Dental, axisdental.com) can be used to create secondary anatomy.
The dental assistant can accomplish the final polish. Many excellent polishing systems are available. In an effort to increase our efficiency, we will use either a two-step (Venus® Supra, Heraeus) or a one-step (Duet-FP™, Komet, kometusa.com; or PDQ™, Axis Dental) polishing system.
Conclusion
In the states that allow dental assistants to place restorative materials, the ability of having the materials and techniques for assistants to consistently place high-quality restorations is a significant advantage to the practice and patients alike. To be able to free up the dentist to see other patients while the restoration is being placed creates the opportunity for the dentist to be able to serve more patients. Therefore, the office can be more profitable, but also because the dentist is able to be working in another operatory, it creates the potential to minimize the composite fees for patients. What we see in our office is that our assistants enjoy placing and creating composite restorations. They take great pride in their abilities. I believe it leads to more job satisfaction and enhances the patients’ perception of the dental assistant when they see that the doctor has placed a high level of trust in this individual.
Offices considering allowing dental assistants to place Class II composites should provide them with the right materials and proper techniques. By creating a system that focuses on using excellent materials and providing superior training, a qualified dental assistant can successfully place high-quality Class II restorations.
About the Author
Gary M. Radz, DDS
Associate Clinical Professor
University of Colorado School of Dentistry
Denver, Colorado
Private Practice
Denver, Colorado