Coordination of a Prosthodontic Case for Improved Function and Esthetics
Dental assistants are key to helping patients reach a full understanding of their treatment
As healthcare workers, dental assistants continue to acquire knowledge as they encounter new cases and provide hands-on treatment to patients. The following prosthodontic case is an example of a comprehensive treatment plan during which the assistants, as treatment coordinators and clinical assistants, had an extensive opportunity to learn by asking questions of clinicians and technicians, in addition to observation and experience.
In this author’s experience, proactive communication with lab technicians, clinicians, and other staff not only increases the dental assistant’s knowledge, but improves patient care.
Case Report
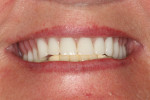
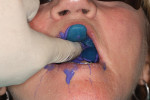
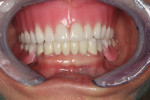
A 64-year-old female patient presented with a loose upper denture (Figure 1). The patient also had a lower partial, and she was not comfortable with the way that they fit together. The upper denture was approximately 4 years old, the lower partial about 10 years, and a lower anterior bridge was over 20 years old.
The clinician and clinical assistant coordinator met with the patient first in a consultation room to discuss her concerns. Often a patient’s stated concerns may differ from the dental team’s observations. In this case, the loose denture had more problems than she realized, until the team communicated their observations.
After the team confirmed that the patient was generally pleased with her upper denture other than its fit, a panoramic X-ray and periapical images were taken. Decay under her existing bridge was discovered, which could compromise the quality of lower reconstruction.
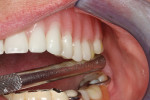
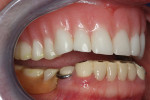
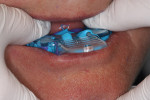
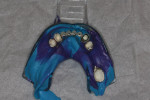
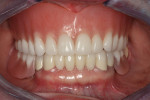
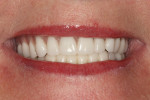
Upon examination of the patient’s smile and bite, the team noted that the occlusion on the right side of her denture was significantly lower than the left side (Figure 2 and Figure 3) compromising the curve of Spee and curve of Wilson (see sidebar). It appeared that the upper denture was originally designed to match the occlusion of the lower partial, which was significantly worn on the right side. In addition, it was noted that the lower left second molar, tooth No. 18, had drifted forward into first molar, tooth No. 19’s space.
The patient affirmed that she was happy with the color and shape of the denture teeth, however she had noticed that they were misaligned. She was informed about the decay under her lower bridge and advised that it would compromise quality of care and that restoring it at this time would be optimal. The final treatment plan included remaking the upper denture, crowning teeth Nos. 18, 21, and 28, fabricating a new bridge and lower partial. Precision (ERA) attachments would be placed on teeth Nos. 18, 21, and 28 on which the partial would snap down. The laboratory would provide a new partial with an improved occlusion for the patient. Because the patient’s teeth were badly worn, the plan was to restore them to her natural bite.
For this treatment plan, the practice worked with two different laboratories, one for the crowns and another for the removable prosthetics. The case coordinators/dental assistants served as liasons between the laboratories to ensure everything fit correctly. Careful written records were kept, including the laboratory technician’s instructions to the clinician.
In this practice, a clinical case coordinator discusses the plan with the treatment coordinator, who details the clinician’s recommendations and the patient’s expectations (for example, changes in the shape of the teeth). When the patient returns for treatment, the coordinator reviews the plan to ascertain if there are any questions or changes before treatment commences.
Preoperative impressions of the upper denture and existing partial were taken to send to the respective restorative laboratory.
At the first appointment, in preparation for the bridge, impressions (Precision®, DenMat, www.denmat.com) were taken of the patient’s existing partial and upper denture, and preoperative models were sent to the laboratory along with the impressions.
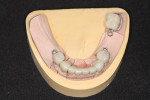
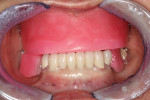
Temporary restorations (Protemp™ Plus, 3M ESPE, solutions.3M.com) were made for tooth No. 18 and Nos. 21-28. When the bridge and the crowns with the ERA attachments were ready (Figure 4), they were tried in temporarily. Pre-seat X-rays were taken to assure everything was seated properly. Once the fit was satisfactory, denture and partial impressions were taken (Figure 5 through Figure 7), the crown and bridge were removed and sent to the second laboratory along with the impressions needed for the prosthetics (Figure 8). The removable prosthetic laboratory would pour the models and make partial to fit the precision attachments.
The patient returned in 2 weeks for her wax rim on the upper denture and the framework try-in on the lower partial (Figure 9).
At the following appointment, the patient’s temporaries were removed, the completed crowns were placed with temporary cement, and the upper denture and lower partial were tried in with the precision attachments. The patient was pleased with the fit, shape, and color (Figure 10).
Once the appearance and fit were approved by the clinician, as well as the patient, the occlusion was checked. Some excess wax was removed from the frenum area because it was a little high, and the prosthesis was returned to the lab for processing and completion.
A few weeks later, the patient returned for the final seating. The temporary crowns were removed. The anterior bridge and crown on No. 18 were permanently cemented with RelyX™ (3M ESPE). Next, the lower partial was locked into place and the upper denture was delivered. Digital photographs were taken. The patient returned one week later for a postoperative check, and minimal adjustments were required.
At the patient’s regular hygiene appointment 6 months later, she relayed that although she was satisfied with the appearance and fit, food was catching in open spaces on both sides of the partial. After impressions were taken (Identium®, Kettenbach, www.kettenbach.us) acrylic was added to close the anterior spaces, solving the problem (Figure 11 and Figure 12).
Conclusion
As demonstrated in this case, patients really value what the dental team can accomplish for them. They do not always know or understand the capabilities of today’s dentistry; engaged communication can educate them on the possibilities for improved function and esthetics.
In this respect, dental assistants are key team members in helping patients reach a full understanding of their treatment options and plan. Once there is communication on both sides, then the patients can be ready to move forward with dentistry that’s done optimally.
About the Author
Tina Calloway, CDA
Greensboro, North Carolina