Fighting Plaque with a Healthy Back
How musculoskeletal health can impact a dental assistant’s life and work
Assistants face a very different set of ergonomic challenges than dentists and hygienists. Unable to position their knees under the patient, they often cannot freely re-position their chair to different “clock” positions, and must maneuver to accommodate the dentist’s positioning, often with an unnatural twisting motion. Combine these issues with poor operatory layout or delivery systems, and it is understandable why assistants report the highest prevalence of low-back pain among the dental team.1,2 In addition, assistants commonly experience right-sided neck and shoulder pain, as well as hand and finger pain that is worst in the first and second fingers. If ignored, this pain may result in muscle imbalances, ischemia, nerve compression, or disc degeneration.
A healthy and well-trained assistant can easily boost a practice’s productivity and decrease stress for the dentist. Any dentist who has had a trusted, long-term assistant miss work or leave the practice knows this well. An excellent assistant requires an investment of training on the part of the dentist, which takes time, money and, usually, some stress. A well-trained assistant is a valuable commodity for the team, and should not be viewed as a “disposable” member who can be cheaply replaced if body parts begin to fail. Investment in proper ergonomic training and equipment for the dental assistant can yield big benefits for the team’s productivity as well as the assistant’s job satisfaction and career longevity.3
To maintain optimal musculoskeletal health, assistants must understand the unique muscle imbalances to which they are prone and how various postures, positions, ergonomic equipment, and exercise can positively or negatively affect their musculoskeletal health.
Posture and Movement
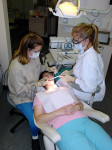
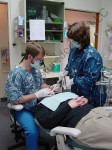
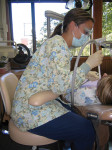
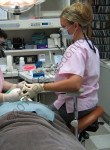
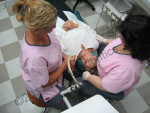
When doing four-handed dentistry, the primary operating tasks of an assistant include keeping the mirror clear, retracting soft tissue, rinsing and drying the field, instrument and handpiece transfers, and light adjustment. To gain a direct view of the oral cavity, assistants often cannot maintain ideal neutral posture, which is ear, shoulder, and hip vertically aligned. Viewed from the back, posture of the neutral spine is straight. The upper arms should abduct out to the sides no more than 20°, and reach forward a maximum of 25°.4 The shoulders should be relaxed, not elevated. Assistants should avoid reaching across their midline with the right arm and hand (Figure 1 and Figure 2). When holding suction devices, wrists should be as straight as possible—neither flexed nor extended. The more the body deviates from neutral postures, the more strain is placed on muscles, tendons, ligaments, joints, and spinal discs.
Frequent forward and side-leaning postures favoring one side are a potent combination and help explain the assistant’s increased risk for low-back pain.5,6 But the assistant also faces the challenge of not being able to easily change chair positions around the patient. Therefore, assistants should seize every opportunity to change their posture and move—either by standing or stretching chairside. This is imperative to the assistant’s musculoskeletal health.
The Seated Assistant
An area of great controversy for the assistant is use of the dental-assisting stool. Specially designed assistant stools have been around for a long time. The unique features of these stools are supposed to increase comfort and help support assistants while they work. The stool should help stabilize the assistant without impairing movement, or inhibiting access to the patient. The variety of features can make the selection process confusing.
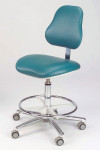
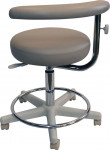
Dental-assisting stools vary greatly in design; there are those with a backrest only, a torso support bar only, both a backrest and a torso support bar, and saddle-style stools (Figure 3, Figure 4, Figure 5 and Figure 6). Seat pans differ in size and shape. It is probably due to the variety of assistant stools and positioning challenges that such a wide array of seated postures are observed among assistants. Unfortunately, many of these postures contribute to cumulative trauma disorders (CTDs). Features and benefits of different assistant stools include:7
• Wide range of height adjustability. Cylinder heights vary widely among manufacturers. The cylinder should adjust high enough to avoid the need to lift the arms up and out to the sides.
• Foot ring with adjustable height. Screws should tighten securely to prevent the foot ring from slipping down to the pedestal.
• Torso support bar that ratchets or pivots toward center of seat pan. Assistants receive support while sitting centered on the seat pan.
• Easy, quick adjustment of torso support bar height. Allows assistants of various heights to use the same stool and still receive torso support. Avoid models with screw adjustment, which is time-consuming and tedious.
• Seat tilt or saddle seat. Places the pelvis in a more neutral position, which allows the spinal curves to balance more easily and requires less external support.
Often, assistants of varying heights and sizes will use the same stool. In such cases, ease of adjustment should be a priority in the selection process. The torso-support bar, foot ring, and/or backrest may need to be adjusted each time a different assistant uses it. A backrest-only design may eliminate re-adjustment of the torso bar; however, the backrest height may still need to be adjusted.
The torso support bar should adjust inward toward the side of the assistant for optimal trunk support (Figure 7). This inward adjustment is achieved with either a ratcheting torso support bar or one that pivots inward. Torso bar designs that swing in a circle around the edge of the stool cannot be adjusted inward to provide proper trunk support at the side of smaller assistants. This forces smaller-framed assistants to sit on the edge of their seat to use the support bar.7 Larger-framed assistants may not need this inward adjustment, as the support bars located at the periphery of the stool may already contact their torsos.
Adjusting Stools with a Torso-Support Bar Only
Sit all the way back on the seat or saddle. Adjust the height of the support bar to just beneath the elbow so the weight of the arm is fully supported. Ensure the bar is not too low or it will encourage leaning on the elbow. Position the bar to the front-left side of the assistant. Ratchet the bar inward so it snugly supports the assistant at the side. There should be enough torso-support bar in front of the assistant’s left arm to allow it to rest periodically. Adjust the height of the stool so the assistant’s eye level is 4 to 6 inches higher than the dentist’s eye level. Adjust the height of the foot ring to securely support the feet. Thighs should be level or sloping slightly downward.
Adjusting Stools with a Backrest and Torso-Support Bar
Sit all the way back on the seat pan. Adjust the backrest height so the most convex portion nestles in the low-back curve. Adjust the seat tilt. On most assistant stools, one lever controls both seat tilt and backrest adjustment. Tilt the seat very slightly forward, no more than 5° to 10°. Adjust the height of the support bar to just beneath the elbow, so that the weight of the arm is fully supported. Ratchet the support bar toward the front of the abdomen. Adjust the height of the stool so the assistant’s eye level is 4 to 6 inches higher than the dentist’s. Adjust the height of the foot ring to securely support the feet.
Stools with both a backrest and wrap-around abdominal support bar typically do not adjust inward toward the assistant’s left side to provide trunk stabilization. This often causes the assistant to position the stool directly facing the patient and slump forward over the bar, bending the spine into a “C” shape (Figure 8). This causes weakening of the postural stabilization muscles and can lead to low-back pain. On the other hand, the saddle stool allows the closest proximity to the patient and promotes the most neutral posture (Figure 9).
Assistants may need to raise the stool slightly higher with treatment of the lower arch. Shorter assistants working with tall doctors may find that their stool will not adjust high enough. If the cylinder cannot be raised high enough, consider purchasing a different model. Unlike operator stools, which are frequently available in multiple cylinder heights, manufacturers typically offer only one height cylinder for their assistant stool; however, this height varies widely among manufacturers, ranging from 27 to 35 inches.
Seated Assistant Positioning
To maintain neutral posture, the assistant must be seated close enough to the oral cavity to avoid leaning forward. Ideally, the assistants should be seated with their left hip at the patient’s left shoulder, and knees angled toward the patient’s head (Figure 10). Most patient chairs are tapered toward the head of the chair and facilitate this position. Thighs parallel with the long axis of the patient is not recommended, as this obviously requires more twisting of the assistant’s trunk.
Close positioning may cause the assistant’s and doctor’s knees to make contact when the dentist is in the 11 o’clock or 12 o’clock position, especially if the dentist or assistant is long-legged. In certain cases, interlocking knees may enable both the dentist and assistant to maintain better positioning during procedures (Figure 11). Some dentists and assistants may be uncomfortable with this amount of contact. Overcoming this hesitancy requires professionalism and communication between the dentist and assistant regarding the goal of this positioning, which is to preserve the health of the assistant and deliver quality patient care.
The Standing Assistant
As mentioned previously, a seated assistant is less able to move around the head of the patient and is more vulnerable to the damaging effects of prolonged static postures. Assistants should, therefore, try to stand for up to half of the treatment time. Alternating between standing and sitting moves the workload from one group of low-back muscles to another and may help reduce low-back pain.8,9
Keep in mind that the assistant should still be 4 to 6 inches above the dentist’s height—even when standing. Certain height combinations will work better for this than others. A medium-height or tall dentist and a shorter assistant is ideal, because the assistant will not have to bend over while standing. If the dentist is too tall, the assistant can stand on a short platform.
Perhaps the worst combination for standing is a short dentist and tall assistant. Again, effective communication between dentist and assistant can help each attain better posture and positioning.
Assistant Delivery Systems
The assistant’s handpieces and instrument tray must be in close proximity. The instrument tray is best positioned directly in front of the assistant, preferably extending over the assistant’s lap. Positioning too far away will result in repeated extended reaching or leaning forward. Ideally, all handpieces and instruments should be within fingertip reach when the arm is comfortably extended, without leaning.
One type of assistant delivery is on a fixed counter at the 1 o’clock position. These are frequently located too far away from the assistant and cause excessive reaching. If instruments are out of comfortable reach, try swiveling the patient chair 10° to 20° counter-clockwise. This may place the assistant closer to the delivery system.3 A better solution when using a fixed counter is to mount the assistant’s work surface on a swiveling tray attached to a long arm that swings out in front of the assistant, over the knees. Over-the-patient delivery systems should be placed as high on the patient (close to the head) as possible, to discourage backward twisting of the assistant to retrieve handpieces.
Another type of delivery is a mobile cart (a unit on wheels) that can move freely in the operatory. Mobile units are often an effective, inexpensive modification for certain operatories; however, there must be adequate room so the assistant’s position is not compromised. Mobile carts often solve positioning problems, as they can be moved to the desired position in the operatory. Assistants should be able to position their knees easily under their delivery system.
Additional Considerations
The assistant is highly prone to developing right-sided neck and shoulder pain. This is usually due to frequent reaching across the assistant’s mid-line with the right arm. At times, this may be difficult to avoid. However, using the left arm as a fulcrum can greatly reduce the musculoskeletal strain associated with this positioning (Figure 12). Assistants must also remember that they do not always need to be watching the suction area. Once the suction is properly placed, the assistant should periodically sit up straight to give the body a rest.
The assistant’s position is largely impacted by his/her view of the oral cavity. For instance, the position of the dentist’s fingers on the mirror can force the assistant to assume an unbalanced posture to gain view of the oral cavity. Simply moving the dentist’s fingers up or down on the mirror handle can help the assistant’s view and posture. The dentist asking, “Can you see?” before the procedure can go a long way in improving the assistant’s comfort and career longevity.7 Communication is key to optimal assistant positioning.
Exercise
Due to their susceptibility to low-back injuries, assistants should maintain excellent endurance of the trunk-stabilizing muscles, focusing on exercise that targets the transverse, oblique abdominal, erector spinae, and multifidus muscles. Examples of these exercises may be found at www.posturedontics.com. As with all exercise, always consult your physician before beginning any strengthening or stretching programs.
The assistant is subjected to similar microtrauma resulting from prolonged static postures and non-neutral postures as the dentist and hygienist. For this reason, the assistant should also regularly perform chairside stretches that reverse potentially harmful postures. Stretches that target the low back are especially important for assistants; however, neck, shoulder, and hand/wrist stretches are also important. It is important to know how to stretch safely.
Conclusion
Assistants face unique musculoskeletal challenges during treatment. Using equipment properly, paying attention to proper positioning, and learning about balanced musculoskeletal health all contribute to preventing pain and injuries in dental assisting. Prevention of muscular pain can make the difference between a satisfying, lengthy career in dental assisting or a painful early retirement.
References
1. Murphy D. Ergonomics and the Dental Care Worker. Washington, DC: American Public Health Association; 1998:151-153.
2. Lalumandier J, McPhee S, Parrott C, Vendemia M. Musculoskeletal pain: prevalence, prevention, and differences among dental office personnel. Gen Dent. 2001;49(2):160-166.
3. Valachi B. The ergonomics of dental assisting: Preventing and managing work-related pain. Chicago, IL: American Dental Assistant’s Association: Department of Continuing Education; 2004.
4. Chaffin D, Andersson G, Martin B. Occupational Biomechanics. 3rd ed. New York, NY: John Wiley & Sons Inc; 1999:375-385, 411.
5. van Dieën J. Asymmetry of erector spinae muscle activity in twisted postures and consistency of muscle activation patterns across subjects. Spine. 1996;21(22):2651-2661.
6. Torén A. Muscle activity and range of motion during active trunk rotation in a sitting posture. Appl Ergon. 2001;32(6):583-591.
7. Valachi B. Fighting Plaque with a Healthy Back. Lecture presented at: American Dental Assistant Association National Convention. July 15, 2005; Washington, DC.
8. Callaghan J, McGill S. Low back joint loading and kinematics during standing and unsupported sitting. Ergonomics. 2001;44(3):280-294.
9. Ratzon NZ, Yaros T, Mizlik A, Kanner T. Musculoskeletal symptoms among dentists in relation to work posture. Work. 2000;15(3):153-158.
About the Author
Bethany Valachi, PT, MS, CEAS is a physical therapist, dental ergonomic consultant, and author of the book, Practice Dentistry Pain-Free: Evidence-based Strategies to Prevent Pain and Extend your Career. She is CEO of Posturedontics, ® a company that provides research-based dental ergonomic education and is clinical instructor of ergonomics at OHSU School of Dentistry in Portland, Oregon. She lectures internationally and was invited to speak at the 2009 International Dental Ergonomics Congress in Krakow, Poland. Bethany has been widely published in over 50 peer-reviewed dental journals and has developed patient positioning and exercise videos specifically for dental professionals. She offers free newsletters, articles, and additional continuing education on her website at www.posturedontics.com. For a free article on Exercise for Dental Assistants, please contact info@posturedontics.com or call 503-291-5121.