The Role of the Diagnostic Wax up in Fabricating Provisional Restorations
David Avery, CDT
The optimum esthetic restorative outcome can only be achieved through proper communication between the patient, clinician, and technician. The best way to ensure this level of communication begins with basic information gathering during the initial examination. A complete set of records must be acquired, including the following:
- A complete set of radiographs
- Periodontal evaluation
- Maxillary and mandibular study casts
- Occlusal registrations (centric relation, centric occlusion, protrusive, right and left lateral excursion, and facebow)
- Full series of intra- and extraoral photographs
- Patient interview to discover patient expectations (whiter, straighter, longer, shorter teeth, etc)
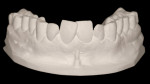
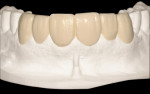
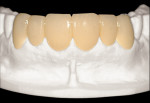
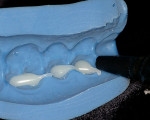
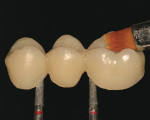
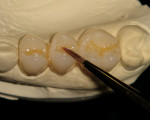
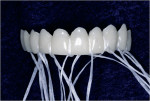
Upon establishment of a healthy oral environment, the diagnostic phase of treatment can begin. Articulation of the study casts should be accomplished with a facebow transfer to a semi-adjustable articulator. The articulated casts should be evaluated to determine if the occlusion is in need of correction. After any needed equilibration and reduction is accomplished, Radica® provisional material (DENTSPLY Prosthetics, York, PA) may be applied to the stone teeth as needed to complete ideal centric occlusion and appropriate occlusal guidance. The wax-like handling characteristics of this material make it ideal for this process. After satisfying the functional requirements, Radica is then applied to correct any esthetic discrepancies, such as diastema closure, adding length, changing shape, etc (Figure 1a, Figure 1b and Figure 1c).
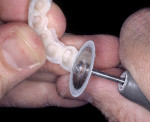
The traditional use of wax to provide the contour corrections has a limitation of poor durability. The substitution of wax with Radica or a light-cured composite provides “toughness” and durability, eliminating the level of concern for damage of the corrected casts that exists with wax. It can be shaped with rotary abrasives and added to as needed. It is less likely to get damaged or broken during the putty matrix fabrication, maintaining the corrected results of the diagnostic mock up for future use.
Once the desired occlusion and esthetics are accomplished on the casts, Regisil® silicone putty (DENTSPLY Caulk, Milford, DE) may be applied to the “mock up” capturing the corrected result. This putty matrix may be used at the chair to generate the direct provisional restorations in the traditional manner.
Preoperative Technique
On larger cases, the clinician may prefer the provisional restorations to be fabricated preoperatively. In these cases, the corrected cast(s) are duplicated with alginate and poured in dental stone. The clinician prepares the abutment teeth on the duplicate cast, making certain to remove less tooth structure than the final intraoral preparations will exhibit. A separating medium is applied to the cast to prevent the Radica from sticking during curing (Figure 2a).
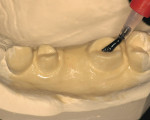
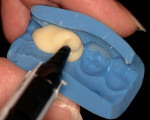
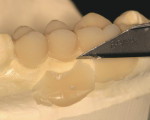
The appropriate shades of Radica syringes are placed in the heating unit for 20 minutes. A small amount of incisal material is syringed into the matrix of the facial-incisal area (Figure 2b). The body shade is then syringed into the restorative areas of the matrix (Figure 2c). The matrix is seated onto the cast, ensuring a complete seat, and a rubber band may be wrapped around the cast for stability. After cooling to room temperature, cooled excess “flash” resin may be trimmed, and a VLC sealer is applied (Figure 3a, Figure 3b and Figure 3c).
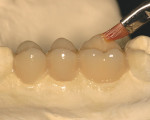
The cast is placed in the curing unit (Figure 4a). After curing is accomplished, the cast is removed from the unit and the putty matrix is removed. The restoration is removed from the cast and any needed minor finishing and polishing is completed. A sealer layer may be applied as a glaze (Figure 4b). Stains may also be applied for characterization where needed (Figure 4c).
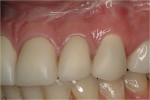
Upon intraoral preparation of the teeth, final impressions are captured. The prefabricated provisional is tried in to confirm occlusal and interproximal contacts. Bis-Acryl provisional material (Integrity™, DENTSPLY Caulk) is syringed into the provisional, seated over the prepared teeth, and cured. After curing is complete, the provisional is removed and any marginal discrepancies are corrected by adding bis-Acryl material, reseating, and curing. Final finishing with attention to marginal contours and the emergence profile is crucial to the periodontal health of the teeth during provisionalization (Figure 5).
Direct/Indirect Technique
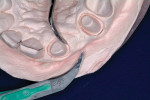
This technique is more involved and time-intensive, but produces the best periodontal and functional result for larger cases, especially if the patient is expected to be in provisionals for an extended period of time. The same preoperative procedures are followed to the point of completing the putty matrix. After the teeth are prepared, an intraoral hydrocolloid impression is captured and poured in properly measured quick-set stone (Figure 6). The tissue is carefully trimmed to expose any margins that may not be visible, while ensuring that the margins are intact (Figure 7). The trimmed putty matrix is tried on the cast to ensure an accurate transfer to the new cast (Figure 8). An acrylic separating medium is then liberally applied to the cast. Radica or Integrity bis-Acryl is placed into the putty matrix, placed onto the stone cast, secured with a rubber band, and cured. After curing is complete, the provisional is removed from the matrix. Proper trimming at the margins and embrasures is critical to good gingival health. Finishing and polishing are minimal because of the accuracy of the putty matrix and provisional material. During placement, an easy cement clean-up technique tip is to tie dental floss around each connector at this stage, which eliminates the need for floss threading after seating (Figure 9). A tissue-friendly provisional promotes optimum gingival health and an easy, predictable delivery day (Figure 10).
At the successful completion of either process, you are now ready to deliver a treatment template that captures all of the essential details to your dentist and to the patient for review and discussion. On multiple-unit anterior restorations, a study cast poured from an impression of the patient-approved provisionals should always be shared with the dental laboratory creating the definitive restoration. This greatly enhances clinical communication, and ensures that the results from the technician are the same as the patient’s expectations.
Conclusion
Both the patient and the overall dental team benefit from using straightforward indirect techniques. The patient’s expectations are clearly set, and everyone benefits from the collaborative review and approval of a lifelike and esthetic diagnostic/provisional restoration. Patients are also able to “test-drive their smile” using these durable provisionals. The dental team benefits from a clear evaluation of the patient’s clinical situation, and prognoses and treatment planning are enhanced.
References
1. Gürel G, Bichacho N. Permanent diagnostic provisional restorations for predictable results when redesigning the smile. Pract Proced Aesthet Dent. 2006;18(5):281-286.
2. Ewoldsen N, Sundar V, Bennett W, et al. Clinical evaluation of a visible light-cured indirect composite for long-term provisionalization. J Clin Dent. 2008;19(1):37-41.
3. Malone M. Smile design and advanced provisional fabrication. Gen Dent. 2008;5(Spec Iss):238-242.
About the Author
David Avery, CDT
Director of Training and Education
Drake Precision Dental Laboratory
Charlotte, North Carolina