Correction of Esthetic and Biomechanical Outcomes after Maxillary Anterior Single Dental Implant Fracture: A Case Report
Ulrike Stephanie Beier, MS, DMD; Heinrich Strobl, MD, DDS, PhD; and Matilda Dhima, DMD, MS
Abstract
Rehabilitation of the single anterior tooth in the esthetic region after a dental implant fracture requires management of contributing biomechanical and/or biological etiologic factors. The multidisciplinary treatment of a fractured maxillary anterior single dental implant with a staged, combined surgical and prosthetic approach is discussed. Alleviation of several, but not all, risk factors eliminated the need for replacement of gingiva with pink porcelain and maintained a stable post implant host complex.
Implant fractures may have a biomechanical and/or biological etiology. The biomechanical factors may be dentist- or patient-mediated. A delayed implant placement protocol with socket preservation and bone or soft-tissue augmentation procedures is recommended for cases with a combination of bone and soft-tissue deformities, thin periodontium, and a history of trauma or infection.1
Biological factors include bone quality and quantity, which clinically present as insufficient bone volume and/or bone loss. The implant fracture seems to occur at the same level as the base of the osseous defect, making it a fulcrum point for bending forces.2,3 A reported minimum bone volume for successful long-term implant therapy has been suggested to be 4 mm in diameter and 10 mm in length.4 Alveolar ridge preservation in the esthetic region minimizes alveolar ridge resorption and preserves bone and soft-tissue architecture for subsequent implant placement.5
Implants with a small diameter have lower mechanical strength compared to those with a larger diameter, increasing the risk of overload.6 Choice of implant material and dimension are important factors that influence clinical outcomes of implant-supported restorations.7
An unfavorable crown-to-implant ratio (C:I) is considered to be a compromising biomechanical factor pertaining to prosthesis design in implant-supported restorations.8 When determining long-term prognosis, the literature is scarce on the validity of the C:I ratio as well as crown-to-root ratio.9 Another potentially significant biomechanical factor to consider is crown height space (CHS), which is determined by measuring from the crest of the alveolar bone to the occlusal surface or incisal edge of the crown.10,11 The clinical C:I ratio is calculated from the segment outside the alveolar bone (because the fulcrum is located at the bone crest) to the implant length residing in the bone.12 A ratio of greater than 1:1 is the minimum acceptable ratio for a prospective abutment, but these guidelines are empirical and lack scientific validation.9,13
Occlusal overload is a patient-mediated biomechanical factor, where the occlusal force on the implant superstructure/prosthesis is directly transmitted to the surrounding bone structure, with the greatest stress concentrated around the neck of the implant,14 further leading to an increased incidence of marginal bone loss.15 Bruxism is defined as an oral habit consisting of involuntary rhythmic or spasmodic nonfunctional gnashing, grinding, or clenching of teeth in other than chewing movements of the mandible, which may lead to occlusal trauma16; it is considered to have a significant role in the frequency of prosthodontic complications.17
In general, it is advisable to carefully treatment plan implant-supported restorations in individuals with incomplete skeletal growth, because implants behave as ankylosed teeth.18,19 Furthermore, implants placed in developing patients lack eruptive potential and do not follow the remaining changes in the growing alveolar process. This can result in relative infraocclusion of the implant and can jeopardize the long-term esthetic outcome.20 Mature adults can exhibit major vertical steps after anterior restorations with osseointegrated implants to the same extent as adolescents or young adults with residual growth potential.21
Clinical Report
A 19-year-old male presented with a chief complaint of a dislodged implant-supported crown in the left maxillary central incisor area. The patient denied any dental alveolar trauma associated with the restoration dislodgement.
The patient’s past dental history was significant for a fall at the age of 8 years, at which time the maxillary left central incisor was avulsed. The tooth was stored in a Dentosafe® tooth-saving-box (Medice, www.medice.de), a container filled with a special storage medium. It was repositioned more than 60 minutes after the accident and stabilized with a flexible wire-composite (Heliosit® Orthodontic, Ivoclar Vivadent, www.ivoclarvivadent.com) splint for 2 weeks. Because of the laceration, the upper lip was sutured with non absorbable 5-0 Polypropylen (Prolene™, Ethicon, www.ethicon.com ) to approximate the wound. Endodontic therapy was completed within the subsequent 6 months. The recovery was uneventful.
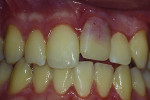
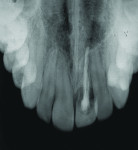
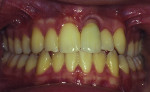
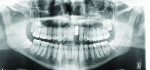
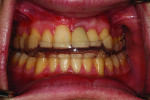
After 11 years, at 17 years of age, the patient expressed interest in a definitive treatment plan to address the associated increased mobility and short clinical crown length of the left maxillary incisor. The clinical examination revealed compromised gingival architecture in disharmony with adjacent teeth, an incisal edge position apical to the incisal edge position of the maxillary right central incisor, and a reduced anteroposterior ridge (Figure 1). The radiographic examination revealed severe root replacement resorption (Figure 2). Treatment options discussed included extraction of the left maxillary incisor followed by placement of a removable and fixed-tooth or implant-supported restoration. A staged treatment approach to maximize esthetic and functional treatment outcome with surgical soft- and hard-tissue augmentation procedures was also discussed with patient and parent but was declined. The patient elected to proceed with extraction of the unsalvageable left maxillary incisor and placement of an immediate provisional removable partial denture.
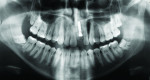
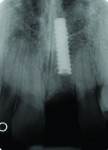
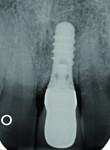
The clinical crown and the remaining gutta percha material were extracted atraumatically by forceps technique followed by immediate placement of an endosseous implant—a 3.3-mm diameter regular neck (RN) 14-mm implant (Straumann AG, www.straumann.com) in the left maxillary central incisor area (Figure 3).
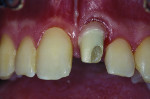
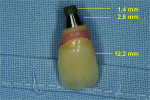
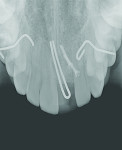
Six months after placement, the implant was restored with a custom zirconium-oxide abutment (Zirkonzahn, www.zirkonzahn.com) (Figure 4) and a ceramic crown with pink porcelain (IPS e.max® Press; Ivoclar Vivadent GmbH), which was provisionally luted with provisional cement (TempBond® NE, Kerr Dental, www.kerrdental.com) to allow the patient to evaluate the esthetics prior to definitively bonding the ceramic crown (Figure 5). After several failed attempts to remove the provisionally luted restoration at the 1-month follow up appointment, the patient did not return until 2009, at which time he presented with a missing clinical crown. The intraoral examination revealed a missing crown on the left maxillary central incisor, as well as an abutment, which was in the patient’s possession (Figure 6). The radiographic examination revealed a portion of the implant inserted 27 months prior with no appreciable pathology (Figure 7). The restoration consisted of an all-ceramic crown (IPS e.max Press) luted with provisional cement (TempBond NE) to a zirconia custom abutment (Zirkonzahn) 27 months prior.
The implant body was fractured into two separate parts. The first portion consisted of the crown, which was still attached to the custom abutment, the smooth neck section, and the first 1.4 mm of the airborne particle–abraded, acid-etched (SLA) surface of the implant (Straumann AG), with a total length of 16.4 mm (Figure 6). The other portion remained in the bone, radiographically measuring 12.6 mm in length (Figure 7). The clinical examination revealed that the fractured portion of the implant body remaining subgingivally was non-movable without bleeding, pain, swelling, or purulent discharge.
Treatment options discussed included explanation of the implant, a removable partial denture, a resin-bonded fixed partial denture, a tooth-supported fixed partial denture, and implant-supported restoration with a staged surgical and prosthetic treatment approach. The patient elected replacement of the fractured implant with an implant-supported restoration following a staged surgical and prosthetic treatment plan. The implant was removed using an explantation trephine especially adapted to the dimensions of the implant (trephine drill, Straumann AG) after full-thickness flaps were labially and palatal reflected. Concurrently, augmentation of the resorbed alveolar crest was accomplished with corticocancellous bone blocks from the mandibular retromolar area and fixed with two titanium bone fixation screws (Modus, Medartis, www.medartis.com). Healing proceeded uneventfully. The patient was provided with an interim removable partial denture (IRPD) while undergoing healing.
Six months after the bone block fixation ridge augmentation procedure (Figure 8), the screws were removed. Visualization of the area was accomplished by reflecting a full-thickness flap with releasing incisions. As sufficient bone volume was available, a two-stage implant placement protocol was followed to place the second endosseous implant (4.1-mm diameter regular neck [RN] 10-mm implant [Straumann AG]) with a cover screw in the area of the left maxillary central incisor (Figure 9). The patient continued to wear the IRPD as he healed uneventfully.
After an additional 6 months, the definitive restoration was designed without the need for pink porcelain. A ceramic crown (IPS e.max Pressy) (Figure 10) was luted with provisional cement (TempBond NE) to a zirconium custom abutment (Zirkonzahn). In an effort to minimize uncontrollable occlusal loads and improve biomechanical stress distribution on the implant superstructure/prosthesis, the patient was provided with a hard acrylic resin (ProBase® cold, Ivoclar Vivadent) custom occlusal device (Figure 10).
At the 21-month follow-up appointment, the implant and implant-supported crown (ISC) demonstrated no clinical signs of mobility, and there was no radiographic evidence of peri-implant radiolucency or marginal bone loss (Figure 11).
Discussion
The implant fracture in the presented patient occurred 27 months after implant placement and 20 months after definitive prosthetic restoration. Some of the factors to consider are implant bone quality and quantity, implant dimensions and material choice, C:I ratio and CHS, occlusal overload, and parafunctional activity. Although the incidence of implant fracture in the esthetic region is low, a combination of local biomechanical and biological factors was greater than the tolerance of the implant, resulting in an implant fracture.
The loss of the maxillary left central incisor at age of 8 years old followed by re-implantation of the tooth resulted in an ankylosed and submerged tooth with replacement resorption and loss of alveolar bone.
The lack of bone augmentation procedures at time of the first implant placement led to reduced peri-implant bone quantity—especially, reduced anteroposterior ridge width, which could only be treated with a narrow implant. Although the prosthetic restoration was successful during the first 2 years of service, hard- and/or soft-tissue augmentation procedures and socket preservation techniques at the time of tooth extraction might have contributed to fewer complications and minimized the need for pink porcelain.
The analysis of the radiographs after the first implantation and after implant fracture (Figure 3 and Figure 7) demonstrates that bone loss of about 1.4 mm occurred in the maxillary implant area. The implant fractured at the base of the osseous defect, where one loss might have made the thin implant more fracture-susceptible.
Additional surgical approaches to maximize esthetic outcomes in this scenario include soft-tissue augmentation procedures, immediate provisionalization, or custom tooth-form healing abutments.1 In the presented scenario, the bone augmentation procedure provided adequate bone volume for implant placement and significantly improved gingival architecture, as shown by the definitive restoration without pink porcelain (Figure 10).
At the time of the first definitive restoration placement, the C:I ratio was 1.1:1. This progressed to a ratio of 1.3:1 (Table 1). The average C:I ratio of a single-tooth implant-supported restoration exceeds that which is considered favorable for a natural tooth.9 In the patient presented, this is an average ratio, which results from the use of a long implant (14 mm SLA surface). The use of a shorter implant would have worsened the C:I ratio. Occlusal overload is another factor to consider. Biomechanical stress distribution in supporting bone around an implant is minimized by reducing nonaxial loading of dental implants.14 After placing implant-supported restorations, it is advisable to provide patients with custom acrylic resin occlusal devices to protect the definitive restorations from occlusal overload. Non-compliance with the device must be discussed with patients as a contributing factor to future complications.
Implants placed after age 15 in girls and 18 in boys have the most predictable prognosis.22 Patients and their families should be informed that implants placed in adolescents lack eruptive potential and do not follow the remaining changes in the growing alveolar process. This can lead to relative infraocclusion of the implant and jeopardize the long-term esthetic outcome.20
Significantly improved esthetic outcomes were achieved by eliminating the need for pink porcelain and improving gingival architecture, despite maintenance of other reported risk factors such as implant material and dimensions.
About the Authors
Ulrike Stephanie Beier, MS, DMD
Assistant Professor
Clinical Department of Restorative and Prosthetic Dentistry
Innsbruck Medical University
Innsbruck, Austria
Heinrich Strobl, MD, DDS, PhD
Professor
Clinical Department of Maxillofacial Surgery
Innsbruck Medical University
Innsbruck, Austria
Matilda Dhima, DMD, MS
Maxillofacial Prosthodontist, Assistant Professor
University of Pittsburgh School of Dental Medicine
Department of Prosthodontics
Pittsburgh, Pennsylvania
References
1. Sclar AG. Strategies for management of single-tooth extraction sites in aesthetic implant therapy. J Oral Maxillofac Surg. 2004;62(9 suppl 2):90-105.
2. Rangert B, Krogh PH, Langer B, Van Roekel N. Bending overload and implant fracture: a retrospective clinical analysis. Int J Oral Maxillofac Implants. 1995;10(3):326-334.
3. Eckert SE, Salinas TJ. Implant fractures: etiology, prevention, and treatment. In: Froum SJ, ed. Dental Implant Complications: Etiology, Prevention, and Treatment. Hoboken, NJ: Wiley-Blackwell; 2010:100-109.
4. Bryant SR, Koka S, Matthew IR. Local and systemic health considerations. In: Zarb GA, Albrektsson T, Baker G, Eckert SE, Stanford C, Tarnow DP, Wennerberg A, eds. Osseointegration: On Continuing Synergies in Surgery, Prosthodontics, and Biomaterials. Chicago, IL: Quintessence Publishing Co Inc; 2008:35-46.
5. Sclar AG. Preserving alveolar ridge anatomy following tooth removal in conjunction with immediate implant placement. The Bio-Col technique. Atlas Oral Maxillofac Surg Clinics North Am. 1999;7(2):39-59.
6. Schwarz MS. Mechanical complications of dental implants. Clin Oral Implants Res. 2000;(11 suppl 1):156-158.
7. Eckert SE, Meraw SJ, Cal E, Ow RK. Analysis of incidence and associated factors with fractured implants: a retrospective study. Int J Oral Maxillofac Implants. 2000;15(5):662-667.
8. Salvi GE, Brägger U. Mechanical and technical risks in implant therapy. Int J Oral Maxillofac Implants. 2009;(24 suppl):69-85.
9. Schulte J, Flores AM, Weed M. Crown-to-implant ratios of single tooth implant-supported restorations. J Prosthet Dent. 2007;98(1):1-5.
10. Nissan J, Ghelfan O, Gross O, et al. The effect of crown/implant ratio and crown height space on stress distribution in unsplinted implant supporting restorations. J Oral Maxillofac Surg. 2011;69(7):1934-1939.
11. Misch CE, Goodacre CJ, Finley JM, et al. Consensus conference panel report: crown-height space guidelines for implant dentistry-part 1. Implant Dent. 2005;14(4):312-318.
12. Blanes RJ, Bernard JP, Blanes ZM, Belser UC. A 10-year prospective study of ITI dental implants placed in the posterior region. II: influence of the crown-to-implant ratio and different prosthetic treatment modalities on crestal bone loss. Clin Oral Implants Res. 2007;18(6):707-714.
13. Penny RE, Kraal JH. Crown-to-root ratio: its significance in restorative dentistry. J Prosthet Dent.1979;42(1):34-38.
14. Ishigaki S, Nakano T, Yamada S, et al. Biomechanical stress in bone surrounding an implant under simulated chewing. Clin Oral Implants Res. 2003;14(1):97-102.
15. Misch CE, Suzuki JB, Misch-Dietsh FM, Bidez MW. A positive correlation between occlusal trauma and peri-implant bone loss: literature support. Implant Dent. 2005;14(2):108-116.
16. The glossary of prosthodontic terms. J Prosthet Dent. 2005;94(1):10-92.
17. De Boever AL, Keersmaekers K, Vanmaele G, et al. Prosthetic complications in fixed endosseous implant-borne reconstructions after an observations period of at least 40 months. J Oral Rehabil. 2006;33(11):833-839.
18. Thilander B, Odman J, Gröndahl K, Lekholm U. Aspects on osseointegrated implants inserted in growing jaws. A biometric and radiographic study in the young pig. Eur J Orthod. 1992;14(2):99-109.
19. Odman J, Gröndahl K, Lekholm U, Thilander B. The effect of osseointegrated implants on the dento-alveolar development. A clinical and radiographic study in growing pigs. Eur J Orthod. 1991;13(4):279-286.
20. Heij DG, Opdebeeck H, van Steenberghe D, et al. Facial development, continuous tooth eruption, and mesial drift as compromising factors for implant placement. Int J Oral Maxillofac Implants. 2006;21(6):867-878.
21. Bernard JP, Schatz JP, Christou P, et al. Long-term vertical changes of the anterior maxillary teeth adjacent to single implants in young and mature adults. A retrospective study. J Clin Periodontol. 2004;31(11):1024-1028.
22. Cronin RJ Jr, Oesterle LJ, Ranly DM. Mandibular implants and the growing patient. Int J Oral Maxillofac Implants. 1994;9(1):55-62.