A Clinical Evaluation Comparing Two H2O2 Concentrations Used with a Light-Assisted Chairside Tooth Whitening System
Abstract
The purpose of this study was to assess the efficacy of two different BriteSmile® hydrogen peroxide (H2O2) gels in a split-arch protocol for whitening teeth in a clinical setting when used in conjunction with a BriteSmile BS4000 lamp. Fifteen subjects were enrolled into a single-center clinical trial. The efficacy of the BriteSmile BS4000 lamp using both 15% H2O2 and 25% H2O2 gel formulations was tested. Study subjects were concurrently exposed to the whitening lamp with the 15% H2O2 gel placed on half of their anterior teeth and the 25% H2O2 gel on the other half for a total light and gel exposure of 60 minutes. The clinical data collected were shade score, gingival health, and dentinal hypersensitivity self-assessment. Changes in tooth shade were better for subjects exposed to the 25% gel and the dental whitening lamp (average 8.0 shade changes) compared to subjects exposed to the 15% gel and dental whitening lamp (average 7.6 shade changes) immediately after treatment. The same held true at the 7-day follow-up (25% gel average 7.4 shade changes versus 15% gel average 7.3 shade changes). However, these differences were not statistically significant. No reports of irritation of gingival soft tissues were documented. The relative changes in mean sensitivity scores were similar for both groups with no significant differences in mean sensitivity scores between the groups. Both concentrations of H2O2 gel and the whitening lamp combined gave study subjects an average of 8.0 (25% gel) and 7.6 (15% gel) shade changes immediately after treatment. The 7-day follow-up examination resulted in a regression of lightest to an average of 7.4 (25% gel) and 7.3 (15% gel). It was concluded that the use of the chairside whitening light and either 15% or 25% hydrogen peroxide gel is safe and effective for whitening teeth in 1 hour.
The pursuit of enhancing one’s appearance by whitening teeth is not a new phenomenon. Reports of dental professionals using various treatment modalities date back as early as the 1880s1 and continue to the present. The media promotes white teeth as one of the characteristics of a beautiful smile. With the ease of access to multiple sources of information, patients are more knowledgeable and inquire more frequently about the various treatment options available to help them achieve an ideal smile.
Dentists can meet their patients’ desired outcome through the use of whitening—one of the most conservative, effective, and safe esthetic procedures possible. Numerous teeth whitening systems have been developed over the past two decades, but the most common systems today use hydrogen peroxide (H2O2), or some precursor to it, as the active whitening agent. The factors that determine which whitening method to use include: type and intensity of staining; how fast the patient wants the process completed; any existing tooth sensitivity; willingness to comply with various protocols; and the investment the patient is willing to devote to a whiter smile.
In general, hydrogen peroxide whitens teeth via a two-step oxidative process.2 In the first step, the hydrogen peroxide molecule is degraded and splits into multiple components, most often hydroxyl radicals. This occurs spontaneously but can be a fairly slow process. In most commercial products, the peroxide product is formulated such that the peroxide degradation process is sped up when applied to the teeth and allowed to interact with the chemical structure of the teeth and/or oral fluids, or via a formulated chemical activation. In the process of degradation, the peroxide radicals formed react with stain molecules (chromophores) within the tooth structure, with the end result being reduced discoloration of teeth.3
In an attempt to accelerate a satisfactory whitening result, many chairside whitening gels are used in conjunction with a light source.4,5 When visible light sources are used, they can react chemically (photocatalyst) within the gel and potentially allow for a safer and more predictable system compared to heat.6
Light-assisted procedures generally require only 1 to 2 hours in the clinic to significantly whiten teeth, whereas take-home products take at least 5 days to produce similar results.7 However, the trade-off for speed is frequently a higher per-procedure cost as well as increased dentinal sensitivity resulting from either nerve irritation due to penetration of the peroxide into the pulp8 or, in some cases, elevation of pulpal temperatures due to the heat.9 Because peroxide concentrations vary widely in whitening gels, the least amount of peroxide needed to achieve desired results (ie, minimum effective concentration) should be chosen.10
The objective of this study was to evaluate the safety and efficacy of a novel BriteSmile® BS4000 lamp (Philips Discus Dental, www.philipsoralhealthcare.com) with two different concentrations of hydrogen peroxide. The null hypotheses were that there was no difference in shade change and sensitivity among the evaluated bleach concentrations.
Materials and Methods
A total of 15 patients were enrolled for an in-office clinical tooth whitening study performed at a single dental practice. All subjects signed an informed consent form adhering to the ethical principles stated by the World Medical Association’s Declaration of Helsinki.11 Subjects were examined before the whitening treatment, immediately after treatment (same day), and 1 week after treatment. At each exam, the following data were collected: subject demographics and medical history (pretreatment only); oral soft-tissue examination; gingival health; shade of maxillary teeth; dentinal hypersensitivity self-assessment; and complications and adverse events.
Inclusion Criteria
Male and female subjects in good general health and between the ages 18 to 80 years at the time of enrollment, with a tooth shade greater than or equal to A3 for all six nonrestored maxillary anterior teeth prior to treatment, were included in the study. Subjects had to be willing to not use any other dental whitening product, including toothpaste, throughout the duration of the study, to refrain from smoking, and to not consume any coffee, cola drinks, dark juice, or other drinks or foods that might stain teeth for 2 hours after treatment.
Exclusion Criteria
Subjects with fewer than six anterior maxillary teeth and those whose anterior maxillary teeth had restorations or dental implants, or those who reported tooth sensitivity on maxillary anterior teeth, were excluded from the study. Subjects with a history of sensitivity to peroxides or glycols and a documented history of untreated caries, recession, abfractions, or cracks on the teeth to be treated, or severely malposed anterior teeth also were excluded. In addition, those with a history of systemic disease, which in the investigator’s opinion could interfere with the assessment of the oral soft/hard tissue, were excluded, as were subjects with a history of photosensitivity or subjects receiving photochemotherapy, systemic antibiotics, anti-inflammatory or immunosuppressive therapy, or who had notable intrinsic staining (tetracycline, fluorosis). Also excluded were those who had previously used professionally dispensed, take-home, or in-office bleaching products. Subjects who were unable or unwilling to complete the study examinations listed herein or who would be relocating or traveling during the course of the study also were excluded.
Treatment Methods
Subjects meeting the inclusion/exclusion criteria were treated in the study. The six maxillary teeth of each subject were assessed using the VITA® Shade Guide (Vita Zahnfabrick GmbH, www.vita-zahnfabrik.com), and that shade was considered the qualifying shade for study entrance. On the day of the whitening treatment, oral soft-tissue examination, VITA shade assessment, gingival health, and dentinal hypersensitivity self-assessment were completed on all six maxillary anterior teeth.
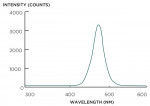
All study subjects were treated with three 20-minute exposures of the BriteSmile BS4000 lamp with 15% H2O2 on teeth Nos. 6 through 8, and 25% H2O2 on teeth Nos. 9 through 11 (BriteSmile® Kit, Philips Discus Dental). The manufacturer’s instructions where followed. A lip retractor and face bib were placed, followed by a light-cured opaque resin to block all gingival tissue. Gauze and masking cream were placed to cover any remaining oral and adjacent soft tissue. The BriteSmile whitening accelerator was applied, along with the bleaching gel, and repeated for a total of three individual 20-minute cycles for a total exposure time of 60 minutes. After each 20-minute session the gel was removed by surgical suction and a fresh layer of gel was applied. During use, the lamp was positioned using the intraoral optical positioner placed within the lamp head approximately 5 inches from the patient’s face. The patient’s and operator’s eyes where protected by filtered glasses. The BriteSmile BS4000 light is a focused, discrete, six-light emitting diode (LED) array system with a spectral range of 400 nm to 505 nm. As indicated in the light-source spectrum in Figure 1, the BrightSmile BS4000 light is essentially monochromatic. This light is equivalent to blue visible light with no significant other ultraviolet emissions.
Relief ACP gel (0.24 % fluoride/5% potassium nitrate, 0.75% amorphous calcium phosphate) application was completed according to the manufacturer’s instructions. The baseline examination was conducted immediately after removal of the gel.
Tooth Color Assessment
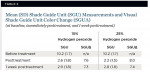
Visual color-matching was performed before whitening, immediately after, and 7 days later. Scores were assessed by two trained and calibrated examiners in a room with color-corrected lighting (5,500-K light bulbs) and under a color-corrected handheld light (Rite-lite™, AdDent, Inc., www.addent.com). The shade-matching distance was 25 cm. The value scale VITA Classical shade guide (Vita Zahnfabrick GmbH) was used to determine the best shade for teeth Nos. 6 through 11. A grey bib was placed over clothing and the dental light was turned off. Any lipstick was removed, and patients were seated in a position where the teeth in the maxillary arch were parallel to the floor during the evaluation. Gradations within the value-oriented VITA Shade Guide were utilized as shown in Figure 2.
Shade change was calculated by determining the change in the number of shade guide units (SGU, difference in the absolute numbers of shade guide “step” in visual evaluation) that occurred toward the lighter end of the value-oriented list of shade tabs. Although the scale is not linear in the truest sense, the changes were treated as representing an ordered series of relationships for the purpose of analysis.
Dentinal Hypersensitivity Assessment
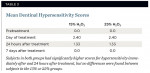
Subjects were asked to self-assess sensitivity (without exogenous stimuli) by recording their perceived sensitivity on each of the six maxillary teeth using a 0 to 10 scale (0 referring to the absence of sensitivity, and 10 to maximum sensitivity), with the pain definitions shown in Table 1.
Oral Soft-Tissue Assessment
Presence of erythema, desquamation, or ulceration of soft tissues, and gross changes in teeth or restorations were documented if present. All teeth were cleaned of all visible plaque with supragingival pumice polish prior to the placement of the bleaching gel. Gingival health for all patients was monitored but was not analyzed for the purpose of this study.
Sample Size and Statistical Analysis
Fifteen subjects were enrolled in this study: 3 females and 12 males who ranged in age from 19 to 78, with the average age of 37 years old. Statistical analysis was performed to compare shade change and sensitivity using the Wilcoxon’s matched-pair signed rank test at the 0.05 level of significance.
Results
Tooth Shade Evaluation
Tooth color evaluation and visual color change according to the VITA Classical shade guide is reported in Table 2. There was a significant color change (lightness) immediately posttreatment (p < 0.01) and 1 week posttreatment (p < 0.01) using either 15% or 25% H2O2. No significant difference in whitening effects could be detected when comparing 15% to 25% immediately posttreatment (p = 0.15) and 1 week posttreatment (p = 0.54).
Dentinal Sensitivity
At baseline (pretreatment), the mean scores for self-reported dentinal hypersensitivity were similar for subjects enrolled (Table 3). Patients in the 15% H2O2 group reported no more sensitivity (2.40) than patients in the 25% H2O2 group immediately after treatment (2.40). At 24 hours, the sensitivity for both groups was reported as 1.33.
Oral Soft-Tissue, Gingival Health, and Sensitivity Evaluation
There were no reports of erythema, desquamation, ulceration of soft tissues, or any gross changes in teeth or restorations documented at any of the study exams by the investigator. Immediately after treatment, 10 subjects reported a mean score of 2.40, and after 24 hours, 7 reported a mean score of 1.33. Five patients reported no sensitivity immediately after, and eight reported none after 24 hours. All 15 patients were pain-free at 7 days.
Discussion
In-office bleaching procedures using 30% to 35% concentrated, light- or heat-activated H2O2 gels were the most common whitening techniques used until the first “at-home” nightguard bleaching system was introduced in 1989.12 During the 1960s and 1970s, bleaching protocols using direct and indirect heat to accelerate the oxidation of the H2O2 were introduced,13,14 but they did not remain popular because of concerns over possible cervical resorption.15,16 Light-and-chemical applications were introduced in the mid-1990s that made in-office bleaching of vital teeth more practical.17
There are inherent safety and efficacy advantages to in-office whitening procedures compared with at-home bleaching techniques, including dentist supervision, control over soft-tissue exposure and ingestion of whitening materials, reduced treatment time, and more immediate results. Today, in-office teeth whitening is arguably one of the most accessible and least invasive cosmetic dental treatments offered by dentists. Efforts to develop and provide painless, quick results using peroxide-based, light-activated, laser, or combined therapies have resulted in the development of new protocols using lower-concentration gels that have been shown to be effective in fewer, if not single, visits.18 A considerable number of studies evaluating the safety and efficacy of both in-office and at-home tooth whitening products and techniques have been conducted and are ongoing.18-25 A 2009 study by Ontiveros et al comparing the use of 25% hydrogen peroxide with and without the addition of light exposure found a significant difference in color achieved after 7 days for subjects treated with the light.24 A review of in-office bleaching has shown conflicting evidence on the effects of supplementary light; this can be attributed to variability with color evaluation, light specifications, and bleaching product formulations.4
The whitening lamp studied emits visible light, primarily in the near-blue and visible blue wavelengths (approximately 400 nm to 505 nm). Thus, despite having a peroxide content that is lower than many chairside whitening gels, the gel studied produced significant whitening with no iatrogenically induced dentinal sensitivity.
The findings of this study demonstrate that the BriteSmile BS4000 dental whitening system is effective at whitening teeth. This is in agreement with the results of previous studies18,21 that reported even lower concentrations of peroxide gel than the 25% and 15% used in this study. No significant gingival problems, dentinal hypersensitivity, or adverse events were noted during the study, indicating that the procedure is also quite safe. Patients in the study reported very mild dentinal hypersensitivity whether they were exposed to 15% or 25% H2O2 gel. These data are significant not only because they demonstrate the effect of a whitening lamp in a controlled clinical trial, but they also demonstrate that a whitening lamp emitting visible light is safe and effective for dental whitening when used as directed. If blocking of the gingival and other oral soft tissues is properly performed, these data indicate that this system can be used to whiten teeth without fearing radiant heating of the teeth, which could raise pulpal temperature and lead to iatrogenic tooth damage.
Light activation of whitening gels has been debated within dentistry for quite some time. Manufacturers of light products have made various claims that whitening of vital teeth can be aided by the use of lamps emitting visible, ultraviolet, or infrared radiation (heat) and lasers. Invariably, these claims are disputed by whitening gel companies or by dental researchers who assert that the lamps are not needed and vital tooth bleaching is simply a result of applying hydrogen peroxide to teeth for a sufficient amount of time. While there may be little or no risk to subjects when using lamps that emit only visible light, there is not much data to demonstrate that visible light has any discernible effect on whitening gels. Hydrogen peroxide by itself that lacks fentonic or similar constituents is not easily light-activated, ie, it does not liberate free radicals that can be used to attack chromophores, unless it is exposed with light having a wavelength of approximately 365 nm26 or less. The application of direct heat could accelerate the reactivity of a bleaching agent and shorten the treatment time. However, the heat alone generated from bleaching lights only provides for a minimal decomposition of peroxide products.20 The system used in this study emits visible light in the blue range of approximately 400 nm to 505 nm. Further studies comparing this system with bleaching gel alone and other lights with different spectral outputs are needed to understand the full effect of the light itself.
Conclusion
The study data demonstrate that a light-catalyzed gel with a concentration of 15% to 25% H2O2 is safe and effective for whitening vital maxillary teeth an average of approximately eight shades in one 60-minute session of light activation. Changes in tooth shade were directionally better for the subjects exposed to the 25% gel and the dental whitening lamp (average 8.0 shade changes) compared to subjects exposed to the 15% gel and dental whitening lamp (average 7.6 shade changes) immediately after treatment and at the 7-day follow-up (25% gel average 7.4 shade changes versus 15% gel average 7.3 shade changes). However, the differences observed were not statistically significant. The 7-day follow-up examination resulted in a regression of lightness to an average of 7.4 (25% gel) and 7.3 (15% gel). Self-reported hypersensitivity was mild and no higher for either group, and resolved after 24 hours. There were no reports of gingival irritation.
Within the limitations of this study, the null hypotheses were confirmed and it was concluded that the BrightSmile light-activated, in-office whitening system used with either 15% or 25% H2O2 gel is safe and equally effective for whitening teeth in 1 hour.
Disclosure
This study was funded by Discus Dental, LLC, a Philips Oral Healthcare Company.
References
1. Harlan AW. The removal of stains from the teeth caused by the administration of medicinal agents and bleaching of pulpless teeth. J Am Med Assoc. 1885;IV(5):123-125.
2. Fasanaro TS. Bleaching teeth: history, chemicals, and methods used for common tooth discolorations. J Esthet Dent. 1992;4(3):71-78.
3. Frysh H. The chemistry of bleaching. In: Goldstein RE, Garber DA, eds. Complete Dental Bleaching. Chicago, IL: Quintessence Publishing; 1995:25-33.
4. Ontiveros JC. In-office vital bleaching with adjunct light. Dent Clin North Am. 2011;55(2):241-253.
5. Joiner A. The bleaching of teeth: a review of the literature. J Dent. 2006;34(7):412-419.
6. Hanosh FN, Hanosh GS. Vital bleaching: a new light-activated hydrogen peroxide system. J Esthet Dent. 1992;4(3):90-95.
7. da Costa JB, McPharlin R, Paravina RD, Ferracane JL. Comparison of at-home and in-office tooth whitening using a novel shade guide. Oper Dent. 2010;35(4):381-388.
8. Gökay O, Yilmaz F, Akin S, et al. Penetration of the pulp chamber by bleaching agents in teeth restored with various restorative materials. J Endod. 2000;26(2):92-94.
9. Baik JW, Rueggeberg FA, Liewehr FR. Effect of light-enhanced bleaching on in vitro surface and intrapulpal temperature rise. J Esthet Restor Dent. 2001;13(6):370-378.
10. Braun A, Jepsen S, Krause F. Spectrophotometric and visual evaluation of vital tooth bleaching employing different carbamide peroxide concentrations. Dent Mater. 2007;23(2):165-169.
11. World Medical Association. Declaration of Helsinki: Ethical Principles for Medical Research Involving Human Subjects. Ferney-Voltaire, France: 2008:1-7.
12. Haywood VB, Heymann HO. Nightguard vital bleaching. Quintessence Int. 1989;20(3):
173-176.
13. Nutting EB, Poe GS. A new combination for bleaching teeth. J So Calif Dent Assoc. 1963;31(9):289-291.
14. Hodosh M, Mirman M, Shklar G, Povar M. A new method of bleaching discolored teeth by the use of a solid state direct heating device. Dent Dig. 1970;76(8):344-346.
15. Madison S, Walton R. Cervical root resorption following bleaching of endodontically treated teeth. J Endod. 1990;16(12):570-574.
16. Latcham NL. Management of a patient with severe postbleaching cervical resorption. A clinical report. J Prosthet Dent. 1991;65(5):603-605.
17. Barghi N. Making a clinical decision for vital tooth bleaching: at-home or in-office? Compend Contin Educ Dent. 1998;19(8):831-838.
18. Tavares M, Stultz J, Newman M, et al. Light augments tooth whitening with peroxide. J Am Dent Assoc. 2003;134(2):167-175.
19. Papathanasiou A, Kastali S, Perry RD, Kugel G. Clinical evaluation of a 35% hydrogen peroxide in-office whitening system. Compend Contin Educ Dent. 2002;23(4):335-344.
20. Hein DK, Ploeger BJ, Hartup JK, et al. In-office vital tooth bleaching—what do lights add? Compend Contin Educ Dent. 2003;24(4A):340-352.
21. Ziemba SL, Felix H, MacDonald J, Ward M. Clinical evaluation of a novel dental whitening lamp and light-catalyzed peroxide gel. J Clin Dent. 2005;16(4):123-127.
22. Kugel G, Papathanasiou A, Williams AJ III, et al. Clinical evaluation of chemical and light-activated tooth whitening systems. Compend Contin Educ Dent. 2006;27(1):54-62.
23. Gurgan S, Cakir FY, Yazici E. Different light-activated in-office bleaching systems: a clinical evaluation. Lasers Med Sci. 2010;25(6):817-822.
24. Ontiveros JC, Paravina RD. Color change of vital teeth exposed to bleaching performed with and without supplementary light. J Dent. 2009;37(11):840-847.
25. Calatayud JO, Calatayud CO, Zaccagnini AO, Box MJ. Clinical efficacy of a bleaching system based on hydrogen peroxide with or without light activation. Eur J Esthet Dent. 2010;5(2):216-224.
26. Baxendale JH, Wilson JA. The photolysis of hydrogen peroxide at high light intensities. Trans Faraday Soc. 1957;53:344-356.
About the Authors
Marilyn Ward, DDS
Private Practice
Houston, Texas
Heather Felix, MSc
Director of Research
Philips Discus Dental, Inc.
Related content:
Learn more about shade matching at dentalaegis.com/go/cced99
Related content:
For more information, read Pre-Bleaching Exam Vital for Optimum Whitening at dentalaegis.com/go/cced98