Feldspathic Veneers: What Are Their Indications?
Abstract
Many different materials and treatment options are available in esthetic and restorative dentistry. Various newer products, such as pressed ceramics, offer enhanced functionality; however, in thinner dimensions, they lack the inherent esthetic beauty of traditional materials such as feldspathic porcelain. As patient demands for better esthetics have increased in recent years, so too has the need for restorative materials that closely mimic the patient’s natural dentition. Initially used for the creation of porcelain dentures, feldspathic porcelain has emerged as the premier esthetic material for custom veneer restorations. In recent years, the use of hand-layered powder/liquid feldspathic porcelain has been revived based on its highly esthetic values and little-to-no preparation requirements. By keeping preparation to a minimum, less tooth structure is lost and procedures are much less invasive, which is exactly what patients desire.
Based on their strength, longevity, conservative nature, biocompatibility, and esthetics, veneers have been considered one of the most viable treatment modalities since their introduction in 1983.1,2 Still in use today, porcelain laminate veneers have undergone a significant evolution, spreading across the globe for treatment of various indications.1 Once considered merely as simple coverings for anterior teeth, the use of veneers has expanded into different indications, including coverage of coronal tooth structures.1
Interestingly, today’s philosophy of using no-preparation or minimal preparation veneers is not new.3 In the early 1980s, innovative concepts of bonding thin pieces of porcelain to teeth with little-to-no tooth preparation were developed to satisfy patients’ needs.4,5 Using layered feldspathic porcelain, these veneers were placed on the facial surfaces of the teeth to create highly esthetic results.5 Unfortunately, due to the advent of pressable materials and computer-aided design/computer-aided manufacturing (CAD/CAM) technology, the customization and high esthetic value typically seen in feldspathic veneers is being lost or diminished.6,7 In some ways, the art of creating beautiful hand-layered feldspathic veneers is akin to the ancient art of Venetian glass blowing.8 For example, a talented and artistic glass blower creates a unique, customized piece that is far superior and much more stunning than something mass-produced and available at a typical retail store. However, just as a talented glass blower undergoes challenges in creating the perfect piece, so do dental ceramists.8
Material Characteristics of Feldspathic Porcelain
Feldspathic veneers are created by layering glass-based (ie, silicon dioxide) powder and liquid materials.8,9 Silicon dioxide, also referred to as silica or quartz, contains various amounts of alumina.8,9 When these aluminosilicates are found naturally and contain various amounts of potassium and sodium, they are referred to as feldspars.8,9 Feldspars are typically modified in different ways to create glass that then can be used in dental restorations.8 Synthetic forms of aluminosilicate glasses also have been developed for use in dental ceramics.8 Whether these synthetic porcelains perform equally or better to naturally occurring feldspar is still debated.8
Original Feldspathic Veneers
Feldspathic porcelain was the key material for creating porcelain denture teeth.8,9 This material provided great esthetic value and demonstrated high translucency, just like natural dentition.9 Experts in porcelain layering and veneering later would stack this fine powder and liquid material onto a core composed of metal, alumina, or zirconia to create esthetic restorations.8
By using a layering and firing process, ceramists then began developing veneers that could be made as optically close to natural teeth as possible.9 When feldspathic veneers were introduced, they presented 0.5 mm of thickness and tapered down to practically nothing at the margins.3 Refractory dies and platinum foil techniques were used to fabricate feldspathic porcelain veneers.8 Feldspathic veneers could be placed conservatively because the porcelain could be layered very thinly.9 Significant loss of tooth structure was not an issue; the veneers were so thin that they could be placed directly on the enamel.9
A major concern with feldspathic porcelain veneers, however, was their strength, which was only approximately 70 MPa to 90 MPa.9 Also, when the veneers were placed without preparation, periodontal problems could occur as a result of overcontoured teeth with unnatural emergence profiles.10 After much research, however, it was determined that feldspathic veneers would last long term, especially when bonded to enamel. Therefore, to preserve the health of the gingival tissues and prevent overcontouring, a slight 0.5-mm reduction of tooth surface was found to work best.3 Because the feldspathic veneers were typically 0.5 mm, the lost tooth structure was replaced and the original emergence profile was nearly restored.3
To solve the perceived issues regarding strength, other types of porcelains were developed by manufacturers.11 However, challenges arose when trying to create very thin, minimally prepared veneers using these new materials.8
Pressed Ceramic Veneers
To correct the low-strength problem, manufacturers introduced products to replace feldspathic porcelains as a veneer material.8 These new materials, termed pressable ceramics, were manufactured to be extremely dense and demonstrated much higher strength ratings, such as flexural strengths up to 180 MPa.8 Due to their improved strength and composition, pressed ceramics were considered ideal for many indications, including inlays and onlays, anterior crowns, bicuspid crowns, veneers, and posterior crowns.8
Pressed ceramic restorations were fabricated using the lost-wax technique.12 The first step was to wax a pattern onto a die, which was then invested and burned out.12 Small ceramic discs, called ingots, were then melted to a thick liquid consistency and pressed into a pattern.12 The final step was to layer powder or liquid porcelains onto the fabricated and pressed restorations.12 This enabled technicians to make the pressed blocks more esthetically pleasing to the patient.12 In addition, pressed ceramics could be waxed to full contour, which continues to be a significant advantage of this type of porcelain.13 However, these full-contour restorations often appeared monochromatic and required superficial surface staining and glazing in order to build in the esthetics. Unfortunately, this process tended to lower the optical “value” of the restoration and, further, these built-in esthetic effects would be lost if any adjustments were needed to the restoration postcementation, or over time as a result of in vivo wear.
As CAD/CAM technologies developed, the availability of computerized pressing and milling machines further simplified this process by developing blocks of pressed materials into the exact size and shape necessary to complete the restoration.8 CAD/CAM technology for veneers, however, is still an evolving, yet promising, modality. These processes were well accepted by technicians and laboratories because they were already accustomed to the waxing techniques that had been used in the past to create metal- and alloy-based restorations and because CAD/CAM machines were becoming more readily available.8,12 These materials, however, required more room for incorporating the optical nuances of dentin and enamel, making more aggressive tooth preparation necessary in order to keep the veneers within the natural emergence profiles.12 Conventional feldspathic veneers required tooth reduction only up to 0.5 mm, and it was possible to work in dimensions down to 0.3 mm.14
Conversely, pressed ceramics required at least 0.75 mm or more of reduction.14 Another issue with pressed ceramics was their tendency to appear less transparent and less esthetically pleasing than traditional feldspathic veneers.9 These new pressed materials tended to appear more opaque and monochromatic and required the addition of extra veneering porcelain to match the natural dentition.8,9 Newer versions of pressed ceramics are more translucent. However, in the authors’ experience, such materials still require an average thickness of 0.8 mm or more for workability and high esthetics.
Today’s Minimal or No-Preparation
Feldspathic Veneers
As patients have begun requesting less invasive treatments and higher levels of esthetics, the use of feldspathic veneers is resurging.6,7 With this comes the desire for thinner veneers and preservation of natural tooth structure.6,7 Modern feldspathic veneers allow ceramists to create thicknesses of less than 0.5 mm, which can be fabricated to a minimum thickness of 0.3 mm.3 Through the use of advanced bonding agents, the capacity to predictably bond veneers to enamel is great as well.6,7 Today, many ceramists are not being trained in the art of sculpting powder/liquid porcelains to form the highly esthetic feldspathic veneers, especially thin veneers.8 This creates a problem because the esthetic value exhibited in these restorations depends on the ceramist’s ability to build depth of color and translucency into the restoration.8 Dentists and their ceramists must also know when it is appropriate to use this slightly weaker restorative material in order to prevent posttreatment fracture issues.8
Indications
Although pure porcelain-bonded restorations are the most conservative and esthetic restorations, they are also the weakest.15 Therefore, important parameters and guidelines must be followed when undertaking a restoration fabricated from powder/liquid feldspathic porcelain veneer materials.15 Generally, feldspathic porcelain materials are indicated for anterior teeth when significant enamel is remaining.8 Occasionally, feldspathic porcelains may be used on bicuspids, but rarely on molars.8 In the case of molars, all risk assessments must present as low as possible.8 Bond maintenance through absolute ideal isolation procedures during cementation, or what has been described as protection of the internal surface of these restorations, is also absolutely necessary for long-term success.8
Of the many factors to consider, space requirement is important and can affect the outcome of the finished restoration.9 When creating a feldspathic porcelain veneer, it is necessary to realize that the space required for shade change ranges from 0.2 mm to 0.3 mm per shade.9 It is also important to consider the condition of the substrate to which the veneers will be bonded.9 To successfully bond feldspathic veneers, the requirements that must be met include 50% or more enamel on the tooth, 50% of the bonded substrate must be in the enamel, and 70% or more of the margin must be in the enamel.8 It is always preferable to preserve the cingulum and lingual marginal ridges, as these anatomic landmarks provide the tooth with more than 80% of its strength.8,16
When deciding whether to use feldspathic veneers, it is also necessary to undertake a flexural risk assessment.8 Flexural risk tends to be higher when bonding to higher levels of dentin because dentin tends to be more flexible than enamel.8 If bonding to enamel, the flexural risk is low to moderate.8 A simple but strong determinant of tooth flexure is to observe mesial–distal craze/fracture lines on the lingual. Tensile and shear stress risk assessments are also necessary when deciding on feldspathic porcelain veneers.8 Generally, higher tensile and shear stresses occur when there are large areas of unsupported porcelain, deep overbites or overlaps of teeth, bonding to more flexible substrates such as dentin and composite, bruxism is present, and the restorations are placed more distally.8 In these higher-risk clinical situations, a pressed or machined glass ceramic should be considered.8 Finally, there must be an absolute low risk of bond and seal failure when placing restorations fabricated from feldspathic porcelain.8
Case Study 1
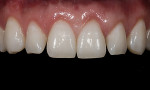
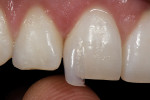
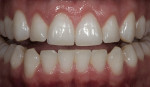
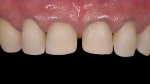
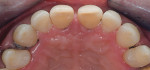
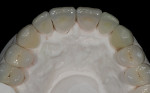
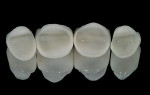
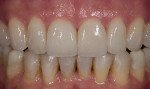
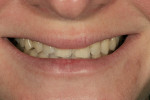
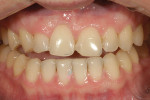
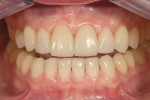
In this case, “mini” no-preparation veneers were used as an alternative to direct composite veneers. The patient presented wanting to close the diastemas (Figure 1). Impression taking required only 10 minutes. At the cementation appointment, the veneers were tried in (Figure 2), and the cementation and finishing protocol required only 30 minutes (Figure 3). Although this case necessitated two appointments, the fact that no preparations were required made the overall restorative process time efficient.
Case Study 2
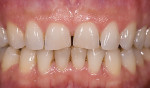
In the case of a patient presenting with a request for longer, fuller teeth and diastema closure (Figure 4), extended veneers with minimal preparations mostly in enamel were planned (Figure 5 and Figure 6). These veneers covered the facial and lingual aspects (Figure 7), and a “taco shell” preparation design was incorporated on the lateral and distal of the central incisors (Figure 8). Overall, this case exemplifies the use of minimal preparation veneers when the criteria for Category 1 ceramic use are met (Figure 9).
Case Study 3
A 35-year-old woman presented with teeth that were unsightly due to chipping, severe wear, unnatural contours, and gingival asymmetry (Figure 10). In addition, pre-existing composite restorations were on the mesial aspects of teeth Nos. 9 and 10, and diastemas also were present (Figure 11). In this era of minimally invasive dentistry, tooth preservation should be every clinician’s goal. Due to the severe damage and occlusal pathology evident in this patient’s dentition, an occlusal equilibration and composite mock-up for more than 5 months was performed as trial occlusal therapy to test the proposed new length and contours.
The patient was comfortable and stable during this time.
Using a putty matrix fabricated from the diagnostic wax-up, a bis-acrylic preparation guide was applied to the teeth. Preparations consisted of placing 0.5-mm depth cuts into the incisal and facial aspects of the bis-acrylic preparation guide. A modified prepless veneer preparation (ie, according to a classification system developed by one of the authors) was made on teeth Nos. 6 to 8, with the depth-cutting grooves minimizing the potential for overpreparation.
With minimal preparation and based on the patient’s desire for maximum esthetics, stacked feldspathic porcelain veneers (Creation, Jensen Dental, www.jensendental.com) were planned for teeth Nos. 6 to 11. Completion of the minimally invasive, stacked feldspathic porcelain veneer treatment resulted in enhanced smile esthetics (Figure 13 and Figure 14) and a conservative and pleasing outcome (Figure 15).
Conclusion
Patients today demand much more from their dentists and laboratory ceramists.1 As a result, highly esthetic restorations and minimal-to-no-preparation restorations are no longer mutually exclusive. Therefore, dental professionals must consistently find a way to select treatment options that focus on the patient’s best interest. With this in mind, a recent resurgence in the use of conventional feldspathic porcelain veneers has developed.7
These conventional dental restorations are generally indicated for anterior teeth and occasional bicuspid use; rare molar placement would be acceptable only when all risk parameters are at the least risk level.8 In addition, feldspathic porcelain veneers are ideal when significant enamel remains on the tooth and generally when there is low flexure and stress risk assessment.8 Finally, these restorations absolutely require long-term bond maintenance for success.
With increased patient demands for enhanced esthetics and a need for restorative materials that closely mimic the patient’s natural dentition, feldspathic porcelain represents the premier esthetic material for custom restorations that are conservative and predictable for appropriate indications. Based on its high esthetic value and little-to-no preparation requirements, feldspathic porcelain enables dentists and their ceramists to provide esthetic treatments that are much less invasive, which is precisely what patients expect.
Acknowledgments
The dentistry and laboratory work for Cases 1 and 2 were performed by Dr. McLaren. The dentistry for Case 3 was performed by Dr. LeSage, and the laboratory work was performed by Domenico Cascione, CDT, BS, from Burbank Dental Laboratory.
References
1. Nash R. At the chair: why conservative preparation for elective laminate veneers. Contemporary Esthetics and Restorative Practice. 2002:70-76.
2. Calamia JR. The current status of etched porcelain veneer restorations. J Philipp Dent Assoc. 1996;47(4):35-41.
3. DiMatteo AM. Prep vs. no-prep: the evolution of veneers. Inside Dentistry. 2009;5(6):72-79.
4. Calamia JR. Clinical evaluation of etched porcelain veneers. Am J Dent. 1989;2(1):9-15.
5. Calamia JR. Etched porcelain facial veneers: a new treatment modality based on scientific and clinical evidence. N Y J Dent. 1983;53(6):255-259.
6. Kim J, Chu S, Gürel G, et al. Restorative space management: treatment planning and clinical considerations for insufficient space. Pract Proced Aesthet Dent. 2005;17(1):19-25.
7. Calamia JR, Calamia CS. Porcelain laminate veneers: reasons for 25 years of success. Dent Clin North Am. 2007;51(2):399-417.
8. McLaren EA, Cao PT. Ceramics in dentistry—part 1: classes of materials. Inside Dentistry. 2009;5(9):94-103.
9. Giordano R. A comparison of all-ceramic restorative systems. J Mass Dent Soc. 2002;50(4):16-20.
10. DeLopez TE. Predictable pressed ceramic anterior restorations. Clinical observations. Dent Today. 2002;21(4):68-73.
11. LeSage BP. Minimally invasive dentistry: paradigm shifts in preparation design. Pract Proced Aesthet Dent. 2009;21(2):97-101.
12. Roulet JF, Degrange M. Adhesion: The Silent Revolution in Dentistry. Carol Stream, IL: Quintessence Publishing; 2000.
13. Cattell MJ, Chadwick TC, Knowles JC, et al. Flexural strength optimisation of a leucite reinforced glass ceramic. Dent Mater. 2001;17(1):21-33.
14. Friedman MJ. A 15-year review of porcelain veneer failure—a clinician’s observations. Compend Contin Educ Dent. 1998;19(6):625-630.
15. Castelnuovo J, Tjan AH, Phillips K, et al. Fracture load and mode of failure of ceramic veneers with different preparations. J Prosthet Dent. 2000;83(2):171-180.
16. Magne P, Belser U. Bonded Porcelain Restorations in the Anterior Region: A Biomimetic Approach. Chicago, IL: Quintessence; 2002.
ABOUT THE AUTHORS
Edward A. McLaren, DDS, MDC
Professor, Founder, and Director
UCLA Post Graduate Esthetics
Director, UCLA Center for Esthetic Dentistry
Founder and Director
UCLA Master Dental Ceramist Program
UCLA School of Dentistry
Los Angeles, California
Brian LeSage, DDS, FAACD
Founder and Director
UCLA Esthetic Continuum
Los Angeles, California
Beverly Hills Institute of Dental Esthetics
Private Practice
Beverly Hills, California