Adapting to Treatment Complications: Stronger is Not Always Better!
Re-evaluation and further analysis ensure long-term success
By Leon Hermanides, CDT, NHD Dent Tech
Despite high levels of training and experience, a functional diagnosis may not always be clear cut nor fit neatly into one category. The following case demonstrates the principles of risk-based treatment planning and the difficulty in identifying and evaluating all of the evidence in an effort to ensure success in our restorative treatment plans. However, it also offers a strategy for addressing an unexpected treatment complication without increasing the patient’s risk for future problems. Often a change in restorative materials or a change in restorative options requiring increased tooth reduction will follow any failure in an indirect restoration. This will, however, increase a patient’s risk of catastrophic failure to the tooth without refining the diagnosis and finding better ways to manage the patient’s inherent risk profile.
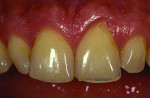
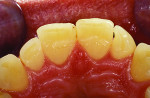
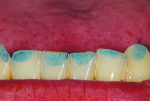
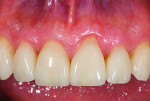
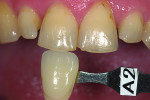
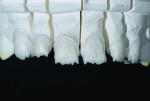
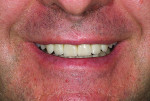
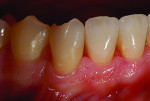
The patient, a 35-year-old male, was concerned about the chipping and thinning of his maxillary incisal edges and unhappy with the appearance of his teeth (Figure 1 and Figure 2). His medical history was noncontributory. His dental history raised concerns, possibly indicating symptoms related to a functional diagnosis of Constricted Envelope.1 He reported that an equilibration had been initiated about 10 years prior but was never completed because during the process, the patient experienced increasing discomfort, tension headaches, sore teeth, and jaw problems. He reported that he clenches his teeth and stated, “When I bite my teeth together I do not feel them all touch.”
Over the last five years, the patient noticed his front teeth becoming thinner and chipping (Figure 1 through Figure 3) and he experienced discomfort when chewing foods such as bagels, hard breads, and chewing gum. He noted that he would sometimes awaken with an awareness of his teeth and when his nightguard came out in the morning, his front teeth were the only teeth contacting in the MIP (maximal intercuspal position).
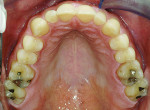
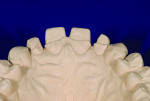
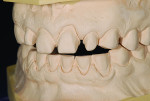
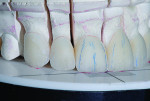
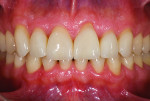
The patient’s periodontal risk was low with no significant bone loss, and the biomechanical risk was low with no caries or structurally compromised teeth present (Figure 4 and Figure 5).
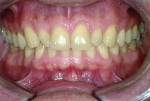
Wear facets were present on the facial aspects of the mandibular anterior teeth with distinct ledges on the palatal surfaces of the maxillary anterior teeth, and minor (less than 1 mm) posterior wear was noted (Figure 3 and Figure 6). The areas of moderate attrition from normal forces were consistent with a diagnosis of a constricted chewing pattern.
The destructive wear on the front teeth (thinning) was not associated with the lateral excursive movements of parafunction. Although a parafunctional habit could not be completely eliminated in the diagnosis, the active destruction of the incisors resulted from the adaptation typically seen with a constricted chewing pattern.
Medium lip dynamics were noted on both the upper and lower arches. The patient wanted to modify the color of his teeth, and some rotations and diastemas were present (Figure 1 through Figure 6).
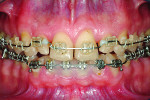
Considering the patient’s diagnosis and risk profile in these four major areas, the various treatment options were carefully evaluated and selected. Initial treatment consisted of orthodontic therapy to correct the anterior rotations, tip the maxillary incisors out facially, and intrude the mandibular anterior teeth. Sufficient inter-arch space was created for both post-orthodontic occlusal equilibration and restoration of the anterior teeth with minimal tooth preparation (Figure 7).
A six-month stabilization period was advised after orthodontic therapy and before equilibration or restorative procedures were initiated. After stabilization, the patient wore a Kois deprogrammer for 3 weeks and an occlusal equilibration was performed utilizing the deprogramming appliance.2
Ultimately, restoration of the anterior teeth and the worn-away tooth structure was accomplished with enamel-bonded feldspathic veneers. With a view to management of any potential parafunction, flattening the guidance on the anterior restorations was recommended to minimize the risk of porcelain failure.
The preparation design for restorations on the palatal of the maxillary incisors was determined by the existing wear facets, which minimized any further tooth reduction (Figure 8 and Figure 9). The cingulum of the incisors remained intact, and the facial and proximal preparations were maintained mostly in enamel. The slight spacing created between the maxillary anterior teeth, when they were flared labially in the orthodontic phase, required proximal preparation of the maxillary incisors. This design reduced the biomechanical compromises to the teeth.3 Spaces distal to the cuspids were not closed as the patient agreed they were not an esthetic compromise.
The cervical margins were prepared to remain slightly supra-gingival and entirely in enamel, (Figure 9) a preparation design that significantly favors a transparent restorative material such as feldspathic ceramic, layered on refractory dies. With the creation of the “contact lens” effect in the final restorations, the margins were not visible after bonding (Figure 10).
When the prepared tooth is not substantially discolored, a translucent all ceramic restoration can be prescribed, such as the refractory veneers used to restore this case. It is, however, vital that the color of the prepared teeth be communicated to the ceramist to help develop a ceramic layering strategy. The ceramist will be able to mask most underlying discolorations or use translucent materials to blend margins prepared supra-gingival as appropriate (Figure 11).
This communication is easily managed by taking a digital photograph of the prepared teeth with a matching shade tab clearly visible. As the tooth preparation procedure will typically dehydrate the abutment teeth, allowing a few minutes for rehydration will help to clearly communicate the extent of any discoloration.
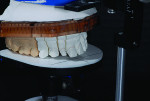
The sequence of articulation and occlusal registration accuracy is critical as the study cast of the provisional restorations and maxillary working model need to be mounted on the articulator in the same reference position. This provides vital tooth position references to be duplicated in the final restorations from the provisional restorations (Figure 12 through Figure 14).
The sequence always begins with articulating the study cast of the provisional, in this case using the record made with the Kois facial plane analyzer and the mounting/reference platform on a Panadent articulator (panadent.com). Once the study cast is articulated, the lower opposing cast (or lower provisional cast) is mounted , followed by the working model of the prepared teeth. If this sequence is completed accurately with all the occlusion records taken at the same vertical dimension of occlusion, the technician will have an accurate three-dimensional plan for creating the final restorations (Figure 14).
As the layers of ceramic were built and fired it was possible to return the articulated casts to the articulator to verify the position of the internal materials such as the dentin layer against the reference platform. The first application of ceramic lays the translucency at the cervical and incisal margins and begins to develop the internal structure. Using fluorescing, somewhat opaque materials at the lingual incisal edge of the preparation will blend the end of the prepared tooth and restoration and helps control the value of the final restoration (Figure 15).
After the dentin layer was built to the desired contours and checked against the reference platform on the articulator, the restoration was fired. This helped to control the ceramic shrinkage as the crown was brought to full contour with up to three thinner layers of ceramic. This also allowed adjustments to be made in color and transparency before the veneers were glazed and the refractory material removed. Firing the dentin layer additionally provided a more stable platform to complete the incisal layering, as the buildup can break off or move when working on the articulator or removing the dies to place in the furnace (Figure 16).
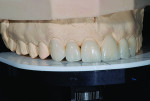
The first step in contouring the veneers was to establish the midline. To do this, either of the maxillary central incisors can be used and once the veneer is placed on the model on the articulator, the pin is used as a sight line. The reference platform on the articulator was then used to determine first the length and then the facial position of the maxillary centrals. The remaining teeth were then added after fitting their proximal contacts and adjusted for length on the reference platform. Using a custom incisal guide table, the lingual contours were formed to determine the appropriate functional parameters (Figure 17 and Figure 18).
After contouring, the veneers were glazed and the refractory material was removed using air abrasion with glass beads. The veneers were then fitted to a stone die and polished to follow the desired emergence profile. The proximal contacts were verified on a solid stone model, after which the length and facial position were checked on the articulator against the reference platform. The veneers were then etched using hydrofluoric acid, cleaned in distilled water in an ultrasonic bath and silanated (Figure 19).
All restorations were bonded using total etch adhesive bonding protocols. After bonding was completed, the occlusion was refined to create bilateral simultaneous contact in centric relation with the cuspids and posterior teeth holding shim stock while the incisors allowed the shim stock to pull through. While sitting up with 200-micron horseshoe paper between his teeth, the patient chewed on the paper to reveal any heavy streaks, indicating anterior interferences. This served to refine the function on the lingual surfaces of the maxillary anterior teeth and establish a smooth pathway into MIP (Figure 20).
Within three months of treatment completion, the patient returned with a fractured veneer at the disto-incisal of the lower right cuspid (Figure 21). He reported that the fracture had occurred while sleeping. The veneer was remade (again in feldspathic ceramic) and bonded. A similar fracture occurred again within the next three months, also during sleep, and was once again replaced with a feldspathic veneer. In addition, a flat-plane nightguard was also delivered.
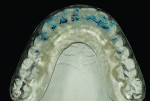
Since the preparation removed very little enamel, the veneer restoration, not the tooth, was at increased risk of fracture. The anterior restorations and dentition ultimately required protection with a flat night guard (Figure 22 and Figure 23). Since placement, lateral grooves appeared on the night guard, confirming the diagnosis of sleep bruxism. In the 9 years since the completion of this treatment and delivery of the night guard there have been no further failures in the restorations.
This case demonstrates that when faced with failure in our restorations despite a thorough risk-based treatment design, a stronger material was not required. A reevaluation of the diagnosis and further analysis proved critical to ensure long-term success. Rather than change the design of the restorations and increase biomechanical (structural integrity of the teeth) risk when faced with restorative fractures, consideration of episodic parafunctional forces and management with a night guard is a good approach.
Acknowledgements
The author would like to thank John Kois, DMD, MSD, for his clinical expertise in completing this treatment, and Brett Fidler, DDS, MSD, for completing the orthodontic treatment. The author also would like to recognize Steve McGowan, CDT, for demonstrating the refractory die techniques used in this case many years ago.
Disclosure
The author had no disclosures to report.
Editor’s Note
A clinical perspective for this case can be found in the April issue of Compendium of Continuing Education in Dentistry. Go to compendiumlive.com.
References
1. Kois JC. New challenges in treatment planning: shifting the paradigm toward risk assessment and perceived value—part 1. Journal of Cosmetic Dentistry. 2011;26(4):62-69.
2. Jayne D. A deprogrammer for occlusal analysis and simplified accurate case mounting. Journal of Cosmetic Dentistry. 2006;21(4):96-102.
3. Magne P, Versluis A, Douglas WH. Rationalization of incisor shape: experimental-numerical analysis. J Prosthet Dent. 1999;81(3):345-355.
About the Author
Leon Hermanides, CDT, NHD Dent Tech
Owner
Protea Dental Studio
Redmond, WA