Part 2: The Single Central Dilemma
Overcoming variables that challenge successful single central restorations
Joshua Polansky, MDC
In the April issue of Inside Dental Technology, the author presented a series of challenges and solutions technicians may face when attempting to restore a patient’s maxillary single central. For many in dentistry, the restoration maxillary single central is probably the most dreaded procedure and poses a challenge for the restorative team. The loss of or damage to a central incisor is most often attributed to trauma, and with the trauma come many variables that may need to be taken into consideration when restoring the patient’s smile. The damage associated with the incurred trauma can range from complete loss of the tooth or a large fracture, to tissue loss and extreme discoloration of the underlying abutment.
Trying to meticulously color match a single central crown is difficult enough in a perfect, non-traumatized intraoral environment; however, when trauma is the culprit, the job of restoring team becomes even more challenging and every detail must be taken into consideration prior to treatment.
The goal of discussing the following cases in this two-part series is to show a continuation of different scenarios associated with damage to a single central incisor and the solutions the restorative team devised to mimic nature.
Stump Color Challenge
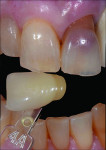
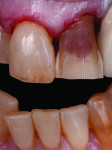
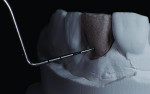
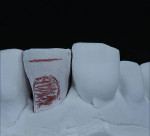
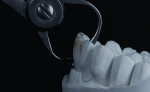
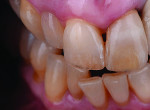
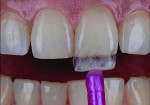
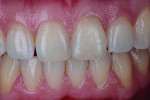
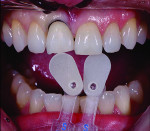
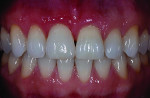
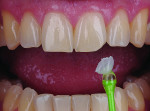
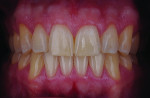
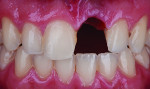
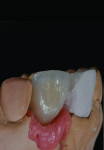
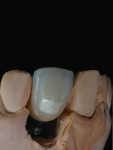
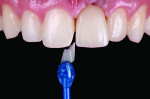
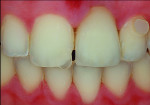
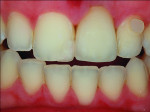
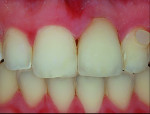
A patient who presents with a dark underlying stump color can challenge the team’s ability to block out the discoloration and achieve an optimal shade match with surrounding natural dentition. Figure 1 and Figure 2 show a veneer preparation with an undesirable abutment color due to previous trauma to the tooth. To ensure the underlying stump color would not affect the shade of the final restoration, the author fabricated an alveolar model and measured the facial space with a periodontal probe (Figure 3). A refractory pencil can be used to highly discolor the refractory die and layer ceramic of different opacities onto the die (GC InitialTM MC, GC America, gcamerica.com) until the pencil marks disappear (Figure 4). The technician can then drill a round hole in the back of the refractory die and check the thickness of the ceramic with a caliper once the pencil marks disappear. This measurement is subtracted from the original measurement with the periodontal probe to determine the needed thickness for the layered ceramic for masking the dark stump coloration (Figure 5). Once the technician knows the underlying color can be blocked, the restoration can be layered to the desired color with the confidence that the dark underlying abutment will not show through and affect the final shade (Figure 6).
Chipped Tooth Challenge
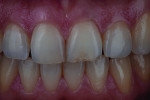
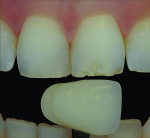
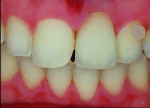
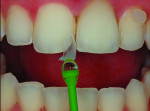
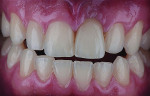
In many instances the trauma incurred does not threaten the loss or vitality of the central incisor but rather the esthetic appearance of the tooth. In these cases patients are looking for a cosmetic fix to restore their smiles. Figure 7 shows a patient with a chip to the incisal edge of tooth No. 9 with a slight but distracting discoloration. In this case no preparation is needed. The fabrication of an additive feldspathic chip can block out the discoloration and restore length to the tooth. As a standard protocol, a polarized shade image was taken for shade selection (Figure 8). A thin, clear feldspathic chip was then layered with a small amount of opacity to block out the discoloration (Figure 9). Once bonded, the feldspathic chip solved the patient’s problem with no preparation required (Figure 10).
In cases such as this one, no margin is required. The technician can use a clear window ceramic to extend the veneer chip over the natural tooth. Once the restoration is bonded, the dentist can then burnish the clear ceramic to blend into the natural tooth, yielding a very natural-looking outcome. Figure 11 through Figure 13 show a patient who presented with a chipped incisal edge. In this case, a ceramic chip was finished intraorally to solve the problem (GC Initial MC). Additive feldspathic chips can be bonded wherever tooth structure is lost to regain esthetics without any tooth preparation. Figure 14 and Figure 15 show a distal fracture on tooth No. 9 that was also repaired with an additive feldspathic chip.
Complex Case Challenge
In many cases, an accident leads to trauma to both maxillary anterior centrals. Figure 16 shows a patient who lost tooth No. 9 from trauma. The same trauma damaged the mesial incisal edge of tooth No. 8. An implant was surgically placed to restore the edentulous space of tooth No. 9, and a feldspathic chip was prescribed to restore the fractured mesial incisal edge of tooth No. 8. The author fabricated a screw-retained restoration for the implant-restored site and a ceramic chip to be added to the mesial incisal fracture (Figure 17 and Figure 18). Figure 19 shows the screw-retained restoration in situ and the additive chip being seated to restore the mesial fracture. It is extremely important with additive chips that the proper color is used to bond the veneer. Figure 20 through Figure 24 show the veneer being tried in with different colored try-in pastes to see what would work best for final cementation. One can see in the image that the clear paste would show the demarcation line if it were to be used at final cementation. A1-colored paste successfully blocked out the demarcation line for seamless integration of the veneer with the natural tooth. Figure 25 shows the final restorations in situ.
Conclusion
Maxillary single central restorations are among the most challenging cases. The dental team must approach the single central case by taking all criteria into consideration in order for the restoration to have a better chance for success. When trauma to the site is involved in the case, new and more complex variables associated with trauma such as tissue management, surrounding dentition, and underlying tooth structure should all be taken into account for achieving a successful outcome.
Acknowledgments
Dentistry was performed by Dr. Barry Polansky, Dr. Mike Monokian, Dr. Devon Conklin, and Dr. Ben Ross.
About the author
Joshua Polansky, MDC
Owner
Niche Dental Studio
Cherry Hill, NJ