Techniques for Accurate Impressions of the Peri-implant Soft Tissue
Step-by-step guidelines for capturing the ideal gingival position
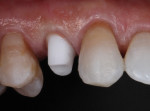
One of the more challenging aspects of successful implant dentistry is the creation of pleasing soft-tissue architecture in the esthetic zone (Figure 1). The implant must be placed in the proper position and the surgeon must protect or create sufficient volume of bone and gingiva. It is the job of the restoring dentist to create an accurate impression and successfully deliver the prosthesis created by the technician.
There are, of course, many difficult steps in this process, but the creation of esthetically pleasing gingiva is the one that requires the most interdisciplinary collaboration. This delicate and intricate procedure requires precision to ensure that it is accurately captured in the definitive impression. A highly accurate impression will significantly enhance the predictability of the final outcome.
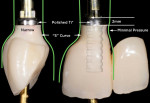
The appropriate gingival architecture must first be created by a provisional restoration that is properly designed to support, shape, and encourage development (Figure 2). After no less than 4 weeks of tissue maturation, the impression can be made. If the clinician does not act quickly during the impression procedure, it is inevitable that the gingiva will flatten before the impression sets (Figure 3). When this impression is poured up and the technician begins to plan the restoration, it will be apparent that the tissue will need to be reshaped on the cast. This process results in an abutment that is different in shape from that of the provisional, and this will result in tissue that will be different than was planned.
Recommended Impression Techniques: Step-by-Step Instructions
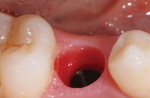
The goal of this discussion is to share a few techniques that will help clinicians make impressions for their technician that accurately capture the ideal gingival position. These procedures take place following maturation of the gingiva at the desired position using a provisional restoration. They are applicable for shaped gingiva, not for cases where the healing abutment has simply been removed for the impression (Figure 4).
Technique No. 1: The Indirect Custom Impression Coping1,2
Remove the provisional restoration from the mouth and attach the appropriate implant analog. Fill a small container with low-viscosity impression material. Insert the analog (with the provisional attached) into the impression material to a depth of approximately one half the crown height, and allow to set. Indicate the facial on the impression material using a marker. Carefully unscrew the provisional and remove. Attach the appropriate impression coping. Either an open or closed tray will work. A straight emergence is preferred.
There will now be empty space surrounding the impression coping, which will be an exact replica of the tissue side of the provisional. Fill the emergence space with a low-shrinkage acrylic (eg, GC Pattern Resin™ LS, GC America, gcamerica.com). Flowable composite or PMMA acrylic would be less accurate options. Using the facial mark on the impression material from earlier, mark the facial aspect of the coping. This will allow proper rotational orientation of the coping.
Place the impression coping into the patient’s mouth, ensuring proper position using the facial marking. There will be some blanching of the gingiva, depending on the amount of time spent making the coping. The blanching should be allowed to dissipate before making the impression. Verify the fit radiographically. Make the definitive impression.
Technique No. 2: The Direct Custom Impression Coping3,4
Ensure that all components and materials are ready. This procedure must be performed quickly. Remove the provisional restoration. Attach the impression coping. Either an open or closed tray will work. A straight emergence is preferred.
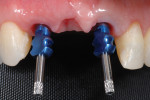
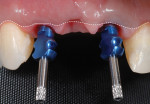
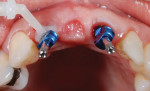
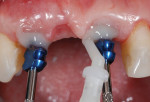
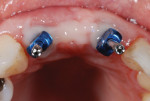
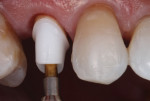
There will be empty space surrounding the impression coping. Fill the space with dual-cure resin material (eg, Bisco Duo-Link™, BISCO, bisco.com), then polymerize. This resin will now fully support the gingiva as though the provisional were still in position. The entire process should take no more than 60 seconds. (Figure 5 through Figure 7). Verify fit radiographically. Make the definitive impression. (Figure 8).
Technique No. 3: Matched Custom Healing Abutment and Impression Coping
The laboratory fabricates a (or purchases a pre-fabricated) healing abutment that is designed to allow the gingiva to mature into an appropriate position supporting the papilla. It should be marked to indicate the proper rotational position, usually by a mark on the facial.
Attach an analog to the healing abutment. Insert the analog/custom healing abutment into unset impression putty and allow to set. Remove the custom healing abutment.
Attach the appropriate impression coping. Either an open or closed tray will work. A straight emergence is preferred. There will now be empty space surrounding the impression coping that is an exact replica of the tissue side of the provisional. Fill the emergence space with a low-shrinkage acrylic (eg, GC Pattern Resin LS). Flowable composite or PMMA acrylic would be less accurate options. Mark the facial orientation.
Both items are delivered to the treating clinicians pre-surgery. The custom healing abutment (from the beginning) is placed at the time of surgery. Following osseointegration (generally 4 to 6 months), the custom impression coping (from earlier) is used to make the impression. Its shape matches that of the healing abutment and thus creates an impression that captures the shape of the tissue.
Conclusion
These techniques will create a highly accurate cast that gives the technician a complete blueprint of the desired soft-tissue architecture, which is developed in the patient’s mouth with its unique biology. The abutment should then be designed to exactly follow the established contours. This will result in an abutment that will go in place with no blanching and no empty space surrounding it (Figure 9 and Figure 10).
The beauty of allowing the gingiva to develop against the provisional is that it allows the patient-specific conditions and biology to form the final contours. It is unreasonable to expect that a cast can be predictably modified to create an abutment that will create an acceptable soft-tissue form. Without using the above techniques, it is likely that the abutment will either be too large or too small, both resulting in undesirable and unpredictable changes to the soft tissue.
In this author’s experience, all three techniques are highly accurate, but the direct custom impression coping technique (No. 2) is most efficient, accurate, and practical.
References
1. Shor A, Schuler R, Goto Y. Indirect implant-supported fixed provisional restoration in the esthetic zone: fabrication technique and treatment workflow. J Esthet Restor Dent. 2008;20(2):82–95.
2. den Hartog L, Raghoebar GM, Stellingsma K, Meijer HJ. Immediate loading and customized restoration of a single implant in the maxillary esthetic zone: a clinical report. J Prosthet Dent. 2009;102(4):211–215.
3. Polack MA. Simple method of fabricating an impression coping to reproduce peri-implant gingiva on the master cast. J Prosthet Dent. 2002;88(2):221–223.
4. Schoenbaum TR, Han TJ. Direct custom implant impression copings for the preservation of the pontic receptor site architecture. J Prosthet Dent. 2012;107(3):203-206.
About the author
Todd R. Schoenbaum, DDS, FACD
Assistant Clinical Professor, Division of Restorative Dentistry, Director of Continuing Education,
UCLA School of Dentistry
Los Angeles, CA