Respecting All Forms of Nature in Implant Dentistry
Science has provided the innovations to achieve excellence
Physicians and dentists should be humble enough to respect nature and biology, since this is the only way to achieve natural outcomes. Humans share an innate sense of esthetics, which, among other things, calls for harmonious integration of teeth with the oral environment. There is a need for dental practitioners to satisfy this requirement. Recent developments in the dental field, notably in implant dentistry, are supportive of this quest. Implants are not better than natural teeth, but they can (must) be nearly as good. In this communication, the authors describe their treatment concept and provide an update on implant dentistry.
As the dental community as a whole and the technological potential at its disposal have advanced rapidly, implant dentistry has arguably benefited more than any other specialty. In a parallel development, the expectations of patients have also increased. Satisfying these demands exceeds the requirement of providing restorations that will “merely” restore function.
Today’s patients expect tooth replacements that are true to nature and esthetic in appearance. Materials science has provided us with opportunities to achieve excellent outcomes. Soft-tissue management, however, remains a critical issue.
Perhaps the most decisive area in naturally appearing restorations is the transition from the prosthetic restoration to the gingiva, also known as the emergence profile of the superstructure. This interface will showcase any surgical and restorative problems that may be present. Subsequent attempts to correct this area will rarely succeed and therefore should be avoided from the outset. The following rule applies: All parties involved (restorative dentist, surgeon, technician, patient) need to develop the treatment plan in a joint effort, and all of them need to be aware of the problems and/or limitations of the strategy adopted. Predictable outcomes can only be expected if this rule is observed. Taking a team approach has often been endorsed and is particularly important in esthetic implant dentistry.
Impressions from Clinical Practice
Teeth form an overall complex whose appearance depends on harmonious interplay with the surrounding gingiva. We should observe nature and learn from nature. Teeth and their associated structures offer countless details that nature has defined for us to be and which can be incorporated into esthetic treatment concepts.
Modules of Implant Profile
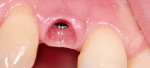
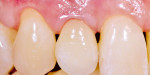
Surgical ability (bone and soft tissue) and laboratory skills (restoration) are required to create an emergence profile that will approach natural beauty as closely as possible (Figure 1 and Figure 2). Both outcomes are then combined by the skills and competence of the restorative dentist. It is essential that clinicians get involved in the laboratory side to understand the potential and struggles of technicians. Conversely, there is a need for technicians to study the biology and behavior of peri-implant soft tissue, since the appearance and sulcus line of the mucosa will greatly influence how the team’s success is ultimately judged. Especially around implant-supported restorations, the mucosal architecture will tip the scale. While deviations in shape, color, structure, and volume are often very real, everything must be done to avoid or compensate for them.
Six Modules for Success in Anterior Implant Treatment
1. Timing of implant placement
Our policy is to use immediate or early placement whenever possible (6 to 8 weeks post-extraction) if anatomical conditions are favorable. The rationale is to counteract resorption as early as possible, as well as to support and preserve the peri-implant tissue. Why should we restore with great effort and compromise what already exists by nature?
2. Augmentation procedures
In our experience, augmentation of bone and soft tissue is absolutely required in almost all cases. The existing defect (or anatomy) will determine which augmentation technique should be used—whether before, during, or after implant placement.
3. Implant positioning
Two-piece implants are positioned 3 mm below the ideal level of the prospective labial sulcus. Our preference is for implant diameters that will offer a distance of at least 2 mm to 3 mm from neighboring structures such as the labial alveolar wall or any adjacent teeth or implants. Ignoring this rule will carry a risk of bone resorption and loss of associated tissue structures (hard and soft tissue, tooth attachment). Implants used to replace multiple anterior teeth must not be positioned too closely to each other. Pontics should instead be used to bridge sites not covered by implants.
4. Soft-tissue management
Upon scrupulous preservation or restoration, the soft tissue needs to be carefully conditioned to its desired shape using a prototype crown or fixed partial denture (FPD). By exerting mild pressure on the soft tissue, this area can be optimally modeled.
Rule of thumb: Use labial relief and proximal pressure! The prototype crowns are fabricated to ideal length between the incisal edge and sulcus on their labial surface. The transition to the sulcus is designed as a small pontic, similar to a bulging cementoenamel junction, and emphasizes the desired eccentric crown segment. The submucosal area is fabricated to a wholly concave (ridge-lap) shape and is gradually developed to the form of a tulip. For retention, we prefer occlusal screws whenever possible in the anterior segment. This will allow for an uninterrupted emergence profile.
5. Prosthetic design
To avoid cement residues on the submucosal surface of cemented restorations (implant is positioned centrally or labially inclined), the restoration margin should never extend more than 0.5 mm to 1 mm into the submucosal space. Also make sure that the abutment follows the scalloped line of the surrounding tissue. On palatally positioned implants, we favor retention via a palatal screw, as this will greatly simplify creating an idealized emergence profile. For anterior restorations, ceramic abutments and all-ceramic crowns should invariably be preferred.
The transitional line angles are a crucial determinant of shape; they should be continuous and reach into the sulcus. Their imaginary line should extend down to the tip of the implant, as this is the only way to obtain a natural shape and corresponding modeling of the sulcus. For cemented restorations, the surface of the eccentric portion needs to be ground somewhat deeper than the less pronounced (usually distal) part, making sure that a natural esthetic result can be obtained.
The same principle is known from conventional prosthetic restorations. The design created for the prototype restoration needs to be transferred to the final restoration, as by custom impression-taking or by obtaining a CAD/CAM copy of the shaped temporary crown.
6. Materials
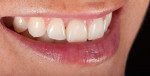
Our preference is to combine CAD/CAM-generated zirconia abutments with pressable ceramic restorations (Figure 3). Our decision to use esthetic zirconia abutments is additionally supported by the fact that ceramic materials (including zirconia) are well known to offer material properties that are benign on gingival tissue.
Case Report 1
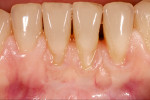
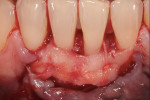
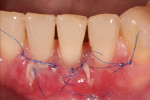
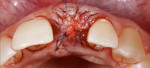
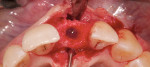
An example is provided in the series depicted in Figure 4 through Figure 7. The baseline situation was compromised by both functional and esthetic problems (Figure 4). Recessions of up to 4 mm were present in the anterior mandibular segment. Mucosal and muscle (or their ligament) structures were observed to insert into the sulcus. Even though the teeth were healthy and exhibiting natural esthetics, the presence of soft-tissue deficits nevertheless created an unpleasant overall appearance. Regenerative therapy was needed to restore an ideal dentogingival complex. It was decided to place a coronal advancement flap in conjunction with a connective-tissue graft (Figure 5 and Figure 6).
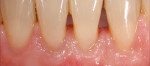
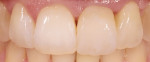
Given the requisite skills and experience, periodontal treatment is capable of bringing about the planned outcome of a healthy and more stable periodontium offering improved harmony between the teeth and gingiva. One year after treatment, the tissue situation was markedly improved in terms of form, volume, and structure (Figure 7). This case illustrates very nicely how emergence profiles can be effectively optimized for esthetics and function.
The same principle can be applied to implant dentistry. We must attempt to proceed carefully from the very outset, either preserving the peri-implant soft tissue or developing it to such an extent that prosthetic contouring will take care of the rest. The prime objective is to create a healthy and stable gingiva that will favorably interact with the superstructure for harmonious integration within the stomatognathic system. Looking at different patients, it is evident that sulcus margins do not always follow a distally eccentric line as they should, but instead will often deviate from this regular pattern.
Case Report 2
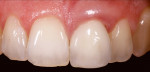
One deviation from this ideal is illustrated by the situation depicted in Figure 8. When this female patient first presented at our office, the gingival line around tooth No. 11 displayed an eccentric architecture mesially. Tooth No. 21 had a poor prognosis due to a transdental fixation that had been altered by inflammation (Figure 8).
Treatment protocol
1. Fabrication of study casts
These are used to fabricate a planning/surgical template and an adequate prosthetic restoration.
2. Delayed immediate placement of an implant
Due to the presence of apical osteolysis, it was decided to refrain from immediate implant placement (Straumann, Bone Level).
3. Extraction and soft-tissue augmentation
Soft tissue from the tuberosity area was used for grafting (Figure 9).
4. Bone augmentation
Eight weeks following extraction of tooth No. 21, no significant bone resorption was noted. An implant was placed in conjunction with grafting in the apical segment of the alveolus on its facial aspect, using autogenous bone harvested from the retromolar area (Figure 10).
5. Implant exposure
Second-stage surgery to expose the implant was performed three months after placement. The crestal soft-tissue architecture was found to be adequately preserved. An impression was taken to insert a “prototype” crown restoration as quickly as possible.
6. Fabrication of the prototype crown
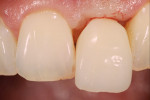
A double-press technique was performed in two steps, including firstly a dentine core in A3/A2, and secondly enamel in A2. Emphasis was placed on the mesially eccentric sulcus line and on obtaining an ideal crown length between the incisal edge and the sulcus. Tooth No. 11 (and its gingival margin) served as reference to be replicated and mirrored for symmetry (Figure 11 through Figure 13). The subgingival portion of the crown was fabricated to a concave, tulip-style shape and was adjusted chairside as needed (Figure 14).
7. Insertion of the prototype crown
The mesially eccentric sulcus line could be optimally imitated. The labial surface of the submucosal crown portion was slightly reduced to provide some relief for the soft tissue. While the soft-tissue volume was well preserved, some upward development of the distal segment of the papilla was still possible. Over the next few weeks, the favorable attachment level of tooth No. 22 would contribute to filling the interproximal space. After 2 weeks, we furthermore added some material to the crown to compress the interproximal tissue toward the incisal (Figure 15 through Figure 18).
8. Fabrication of the final crown
The referring dentist was supplied with a custom impression post (also representing the submucosal portion of the idealized prototype crown) and was able to fabricate the final restoration four months after the prototype had been inserted.
Treatments involving restorations in the anterior segment are always challenging. Particularly exciting are those involving replacement of multiple teeth by implants. Successful outcomes have turned out to be more readily attainable if implants directly adjacent to each other are avoided. Indications of this type should be managed with pontic-style elements whenever possible.
Conclusions
Our treatment concept places a strong focus on each individual patient. Losing sight of the patient will make successful planning impossible. It is therefore imperative that he or she forms part of the team even in the planning stage. After all, it is ultimately the patient who has to carry the psychological and financial burden of extensive dental treatment.
For all the points we have presented and elaborated upon, we must bear in mind that each case is different and complex in itself. Placing implants and inserting superstructures on them will always remain an exciting challenge. We shall always face not black and white but shades of grey. We need to keep reminding ourselves that deviations from original treatment plans may occur. Some decisions need to be made spontaneously and, if necessary, be implemented even amidst treatment steps. Success will greatly depend on the clinician’s experience, sensitivity, and skill. These qualities should be reliably present before any treatment. Finally, and for the benefit of our patients, there is definitely no harm in taking a careful and restrained approach to solving clinical cases, always remaining humble enough to respect biology.
Acknowledgments
Requirements for success include not only experience but also imagination and knowledge of the treatment objective. Memory is an important source of these qualities, as we draw from what we have encountered and assimilated in the past. With this in mind, I wish to express my gratitude to all my mentors from whom I have been privileged to learn. Part of my success I owe to my former colleagues in Freiburg, most notably to Professor Jörg Rudolf Strub. I would also like to thank Joachim Kern (formerly of the Zahnwerkstatt laboratory in Bötzingen, Germany; currently running a laboratory in Los Angeles, Beverly Hills, North Camden Drive). Numerous of his thoughts and concepts have entered the discussions in this article.
Editor’s Note
This article was originally published in EDI Journal, and any techniques or products discussed apply to the international market, not necessarily the U.S. The article is meant to present the reader with a broader perspective of the clinical and technical experiences.