Use of a Resin-Bonded Bridge to Replace a Congenitally Missing Lateral Incisor: Treatment of “Intrusion” of Teeth
Paul S. Rosen, DMD, MS; Oded Bahat, DDS; Stuart J. Froum, DDS; Fereidoun Daftary, DDS; Howard Rosenthal, DDS; and Sylvan Feldman, DDS, MLA
Abstract:
Craniofacial growth is an important factor to consider when providing dental implant treatment for adolescents to replace missing teeth. Ongoing longitudinal observation has demonstrated that such tooth replacements may appear intruded over time, because there may be ongoing downward and anterior movement of both the alveolus and the teeth at a rate exceeding that of the dental implant, which acts like an ankylosed unit. This case reports on a 23.5-year-old female patient who, at age 16, had orthodontics completed and was left with a space where the maxillary right lateral incisor was congenitally missing with the hope of future restoration with a dental implant. A resin-bonded bridge had been placed to fill the space in the interim. After approximately 7.5 years, the bridge loosened and the patient sought an implant option as its replacement. Clinical images revealed that the bridge, which contained two bonded wings, may have limited physiologic growth, causing both the maxillary right central incisor and canine to appear intruded compared with the left central incisor and canine. This case illustrates, at the very least, that growth and development may not be complete in females aged 16 years and that the way in which a missing tooth is replaced must be carefully considered given the impact that ongoing growth and development may have on restorative care. Moreover, further growth and development may also impact adults.
Congenitally missing anterior teeth in adolescents present a challenge for the dental practitioner. A decision must be made whether to orthodontically correct this problem by moving the adjacent canine into the missing lateral incisor position, avoiding the need for a replacement tooth, or to maintain space for a future dental implant. If the latter is chosen, the next decisions are how to provisionalize the site and determining the appropriate time for dental implant placement, because potential ongoing growth and development of the jaws may lead to an unesthetic result in the long term.1-4 In many instances, a resin-bonded restoration can be used. The advantage of this option is its tooth-sparing nature while also allowing for future removal of the bridge and the subsequent placement of a dental implant when growth and development is completed.
Studies have examined the merits of bonding this type of restoration with either 1 or 2 wings.5-8 Much of the discussion centers on which bonding option will offer better adherence without loss of either the bonding or the entire prosthesis itself from the adjacent tooth or teeth. Beyond the issue of retention, no discussion has taken place to date about whether this decision could also impact 3-dimensional tooth positioning in the dentition of an adolescent, in whom growth and development is not complete. This case report highlights the impact that a two-winged resin-bonded bridge had on an adolescent female with a single missing maxillary lateral incisor. The result, similar to those reported with dental implants, led to the bonded central incisor of the 2-winged bridge appearing intruded years later.
Case Report
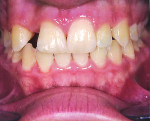
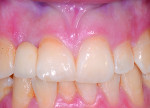
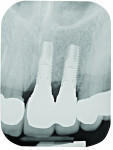
A 23.5-year-old Caucasian woman was referred for evaluation and placement of a dental implant at the site of her congenitally missing maxillary right lateral incisor. She had orthodontic treatment completed 7.5 years prior, and a space had been left to allow for the placement of a dental implant restoration in the location of this tooth (Figure 1). The orthodontics aligned the midline of her teeth with the middle of her nose, and the incisal edges of her two central incisors were level with one another and were also parallel with her eyeline. A resin-bonded bridge was secured to both the adjacent canine and central incisor to provide retention and space maintenance. During the intervening time, the patient had been satisfied with the esthetics and function of the prosthesis. The motivation for her now seeking implant care was that the bridge had recently debonded from her central incisor tooth. It was believed that growth and development would now no longer impact dental implant positioning relative to the natural dentition.
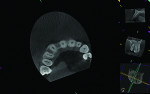
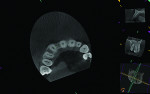
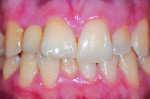
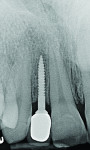
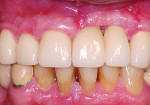
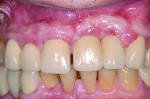
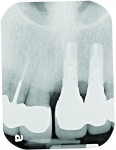
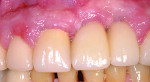
During the examination, two observations were made: First, inadequate space was present for an implant of ≥ 3 mm in diameter to be placed. This was based on measurements made on a cone-beam computed tomography (CBCT) evaluation (Figure 2 and Figure 3). Second, after 7.5 years of the bridge functioning, the incisal edge of the maxillary right central incisor was no longer even with the adjacent left central incisor (Figure 4). Moreover, a comparison of the photographic image (Figure 4) taken at the implant evaluation visit to the one taken at the conclusion of orthodontics (Figure 1) suggested that the canine might have also been limited in its physiologic movement based on its altered relationship to the opposing arch. The conclusion made was that growth and development had not been completed and that in the intervening time, the downward and anterior trajectory of this development was impacted by the fixed prosthesis.
After reviewing with the patient the risks and benefits of each alternative, which included either revising the area with a fixed partial denture bonded with a single wing or placing a narrow-diameter implant (Dentatus USA Ltd., www.dentatususa.com) measuring 1.8 mm in diameter and 10 mm in length (Figure 5 and Figure 6), the patient chose the implant. The reasoning was that this particular implant would not impact the adjacent natural teeth because of its narrow diameter, and it would provide the option to reverse-torque it out in the future should growth and development continue to adversely impact the esthetics of the patient’s dentition and replace it with another option.
Discussion
This case report exhibits some similarities to what has been reported in the literature for implants placed in adolescent and young-adult patients, ie, the appearance of an intruded implant years later.1-4 Hence, practitioners have deferred implant therapy in this age group until a later time, with the belief being that growth and development will have been completed then. The authors’ review of the literature, though not as exhaustive as one that might be performed for either a systematic review or meta-analysis, revealed no case reports of a resin-bonded fixed partial denture impacting tooth position in a growing adolescent patient. A variation of this theme has been reported whereby teeth have intruded from cemented fixed partial dentures when natural teeth were splinted to dental implants.9,10 The relevance of this potential complication is that careful treatment planning for the intervening prosthesis must be performed that will maintain the necessary space in developing individuals. For example, placing a resin-bonded bridge with 1 wing rather than 2 following the completion of orthodontics might be more prudent, provided that the occlusion will allow for this.
The issue of growth and development impacting fixed prostheses may not be just confined to adolescents or young adults. In an article that reported on continued craniofacial growth and development throughout life that affected implants placed in patients well beyond their adolescent years, Daftary et al11 reviewed the historic background on lifelong growth and development and demonstrated in case reports the impact this may have on adult patients. The authors cited a number of studies12-14 that demonstrated growth and development of the craniofacial region continues throughout a patient’s life.
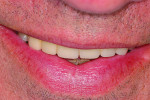
A clinical example of this is seen in Figure 7 through Figure 11 where one of the authors (PSR) treated a case involving a Caucasian man in his late 50s to early 60s. The patient received two dental implants at 59.5 years of age in the maxillary left central and lateral incisor sites where the maxillary ridge had undergone regenerative therapy for deficiencies in both the vertical and horizontal dimensions that prohibited implant placements. In the completed prosthesis, the esthetics were acceptable because the patient had a low smile line and the incisal edges appeared harmonious (Figure 7). Over 6 years, however, a diastema developed between the adjacent central incisors, the implants became more apical relative to the adjacent central and lateral incisors, and compared to when the prosthetics had been completed (Figure 8) the position of the implants now appeared more labial (Figure 10). The gingival hyperplasia had also increased, coinciding with an escalated dosing regimen for the patient’s calcium channel blocker. This, however, did not contribute in any way to the midline diastema that had developed. The patient received treatment for the peri-implant gingival inflammation (Figure 11 versus Figure 9) because no crestal bone loss had occurred in the 6 years; hence, no diagnosis of peri-implantitis was made. Regarding the diminished esthetic result, the fixed partial denture was replaced with a new one (Figure 12). Whether the problem will reoccur is unknown at this time.
Because growth and development can be viewed as a lifelong process, the decision to place a segmental fixed partial denture that is secured to several teeth in an adult may also be subject to the same outcome as with an adolescent. Why this is not reported more frequently in the dental literature may relate to several reasons. In many instances, single-implant placements have been used to replace 3-unit fixed prostheses, making it less likely for this phenomenon to be observed. Also, this may well be relatively rare, or it may happen at a subclinical level of detection. Clinicians may not be aware that this phenomenon exists, or quite possibly, clinicians may be concerned about implicating themselves or a colleague when faced with a suboptimal outcome. Another consideration with integrated/“ankylosed” dental implants is the impact that thinning of the facial bone may have as growth and development progresses. If the labial plate at the dental implant was thin initially, over time labial crestal bone loss can occur, which may be diagnosed as peri-implant disease based on attachment loss.15
In the present case, the decision to place a narrow-diameter implant in the 23.5-year-old woman could clearly come under much negative criticism. Because her growth and development is still ongoing, the possibility of intrusion well exists. Conversely, some patients do not wish to wear bonded or cemented fixed restorations. Bonded restorations carry the risk for coming loose from the adjacent tooth and can make hygiene efforts more difficult for interproximal cleaning, while a cemented full-crown preparation also has the same hygiene issues and introduces the potential need for endodontic treatment at a future time. The use of a narrow-diameter implant provides the benefit of a fixed restoration in an area of limited space. Moreover, Bahat16 has suggested that due to ongoing growth and development, clinicians should possibly consider placing a more retrievable implant that will not cause damage to the area on its potential removal should growth and development adversely affect implant esthetics.
While the original function of narrow-diameter implants was to support a fixed interim prosthesis during the osseointegration of conventional implants, they have also demonstrated the ability to remain stable for an extended period.17 This strategy should be employed only after extensively discussing with the patient the goals and benefits of this approach versus other available options. How well this strategy works will best be determined over time; however, it does appear to offer the flexibility to care that is necessary for a dynamic situation such as the one presented.
Conclusion
The present case report demonstrates the impact that growth and development may have on an adolescent patient who has been restored with a 3-unit resin-bonded fixed partial denture with 2 wings. Considering the advances in adhesive dentistry, consideration should be given to using 1 wing to prohibit the possibility for adverse long-term esthetic outcomes. Moreover, aging of the patient beyond adolescence does not eliminate the potential for this same outcome with either teeth or dental implants. Thus, the use of a narrow-diameter implant may be considered as a treatment option to provide esthetics and function, because it can serve as an easily maintainable restoration while allowing for its removal if needed due to further growth and development. Hence, all treatment planning should consider the possible effects of ongoing anatomic maturation.
Acknowledgements
The authors wish to thank Sheri G. Rosen, OD, for her assistance in the preparation of this article.
About the Authors
Paul S. Rosen, DMD, MS
Clinical Professor of Periodontics
Baltimore College of Dental Surgery
University of Maryland Dental School
Baltimore, Maryland
Private Practice
Yardley, Pennsylvania
Oded Bahat, DDS
Private Practice
Beverly Hills, California
Stuart J. Froum, DDS
Clinical Professor
Department of Periodontology and Implant Dentistry
Kriser Dental Center
New York University Dental School
New York, New York
Private Practice
New York, New York
Fereidoun Daftary, DDS
Private Practice
Beverly Hills, California
Howard Rosenthal, DDS
Private Practice
Newtown, Pennsylvania
Sylvan Feldman, DDS, MLA
Clinical Associate Professor of Periodontics
Baltimore College of Dental Surgery
University of Maryland Dental School
Baltimore, Maryland
Private Practice
Lutherville, Maryland
References
1. Oesterle LJ, Cronin RJ Jr, Ranly DM. Maxillary implants and the growing patient. Int J Oral Maxillofac Implants. 1993;8(4):377-387.
2. Cronin RJ Jr, Oesterle LJ. Implant use in growing patients. Treatment planning concerns. Dent Clin North Am. 1998;42(1):1-34.
3. Brahim JS. Dental implants in children. Oral Maxillofac Surg Clin North Am. 2005;17(4):375-381.
4. Jemt T, Ahlberg G, Henriksson K, Bondevik O. Tooth movements adjacent to single-implant restorations after more than 15 years of follow-up. Int J Prosthodont. 2007;20(6):626-632.
5. Kern M. Clinical long-term survival of two-retainer and single-retainer all-ceramic resin-bonded fixed partial dentures. Quintessence Int. 2005;36(2):141-147.
6. Kern M, Sasse M. Ten-year survival of anterior all-ceramic resin-bonded fixed dental prostheses. J Adhes Dent. 2011;13(5):407-410.
7. Sailer I, Hämmerle CH. Zirconia ceramic single-retainer resin-bonded fixed dental prostheses (RBFDPs) after 4 years of clinical service: a retrospective clinical and volumetric study. Int J Periodontics Restorative Dent. 2014;34(3):333-343.
8. Zitzmann NU. Resin-bonded restorations: a strategy for managing anterior tooth loss in adolescence. J Prosthet Dent. 2015;113(4):270-276.
9. Cho GC, Chee WW. Apparent intrusion of natural teeth under an implant-supported prosthesis: a clinical report. J Prosthet Dent. 1992;68(1):3-5.
10. Rieder CE, Parel SM. A survey of natural tooth abutment intrusion with implant-connected fixed partial dentures. Int J Periodontics Restorative Dent. 1993;13(4):334-347.
11. Daftary F, Mahallati R, Bahat O, Sullivan RM. Lifelong craniofacial growth and the implications for osseointegrated implants. Int J Oral Maxillofac Implants. 2013;28(1):163-169.
12. Bernard JP, Schatz JP, Christou P, et al. Long-term vertical changes of the anterior maxillary teeth adjacent to single implants in young and mature adults. A retrospective study. J Clin Periodontol. 2004;31(11):1024-1028.
13. Bishara SE, Treder JE, Damon P, Olsen M. Changes in the dental arches and dentition between 25 and 45 years of age. Angle Orthod. 1996;66(6):417-422.
14. Tallgren A, Solow B. Age differences in adult dentoalveolar heights. Eur J Orthod. 1991;13(2):149-156.
15. Peri-implant mucositis and peri-implantitis: a current understanding of their diagnoses and clinical implication. J Periodontol. 2013;84(4):436-443.
16. Bahat O. The relationship between craniofacial esthetics, aging and crani ofacial growth of dental implant placements. Lecture presented at: American Academy of Periodontology Annual Meeting; September 19-22, 2014; San Francisco, CA.
17. Klein MO, Schiegnitz E, Al-Nawas B. Systematic review on success of narrow-diameter dental implants. Int J Oral Maxillofac Implants. 2014;29 suppl:43-54.