A Review of the Positive Influence of Crown Contours on Soft-Tissue Esthetics
Abstract:
Successful crown restorations duplicate the natural tooth in hue, chroma, value, maverick colors, and surface texture. Equally important is the visual harmony of the facial and proximal soft-tissue contours, which requires the collaborative skills of the restorative dentist, periodontist, and dental technician. The treatment team must understand the biologic structures adjacent to natural dentition and dental implants. This report describes the potential for specifically designed restorative contours to dictate the optimal gingival profile for tooth-supported and implant-supported crowns. Showing several cases, the article explains how esthetic soft-tissue contours enhance the definitive crown restoration, highlights the importance of clinical evaluation of adjacent biologic structures, and discusses keys to predicting when the proximal papilla has the potential to return to a favorable height and shape.
Esthetic crown restorations require precise control of multiple variables during crown fabrication in biologic synergy with the surrounding soft-tissue profile. This commendable goal frequently challenges the treatment team.
The free gingival margin has been described as knife-edged and parabolic, following the buccal and palatal extent of the alveolar bone and cementoenamel junction (CEJ) of the tooth.1,2 The facial contour of the soft tissue is greatly influenced by the concavity of the root interface relative to the convexity of the coronal enamel.3
Simulation of a natural tooth also depends on the location of the facial gingival zenith, defined as the most apical position of the free gingival margin. In healthy normal dentition, this is generally 1 mm distal to the midpoint of the tooth. This is most pronounced in maxillary central incisors and reduced in lateral incisors and cuspids.4
The proximal surface contours of the CEJ are parabolic in shape and slightly concave. The interdental papilla occupies the proximal area apical from the contact point.5 The restorative management of proximal soft tissue relies on many factors, including the embrasure volume, location of the crestal bone from the restorative contact point, and periodontal/peri-implant health of the adjacent tooth or implant.6-9
The following cases review how to manage the facial and proximal gingival profiles solely using restorative contours. Understanding of the biology of soft tissues adjacent to natural dentition and the innate potential for spatial manipulation is of utmost importance. These concepts are directly applicable to implant-supported crowns.
Coronal Migration of the Free Gingival Margin
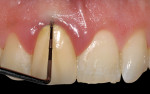
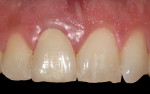
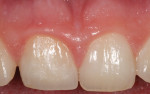
Iatrogenic gingival recession, as in the first patient case shown, can be caused by restorative gingival margins that have impinged upon biologic width.10,11 The typical clinical appearance of the soft tissue when a crown margin has impinged upon connective tissue attachment is shown in Figure 1. The clinical appearance was confirmed by bone sounding using a periodontal probe,12 also shown in Figure 1. There was, thus, a general expectation that the facial gingiva margin would migrate coronally. Diagnostic casts were made for the fabrication of the provisional crown.
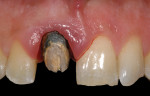
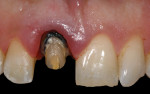
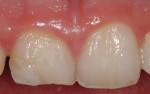
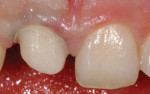
After removal of the metal-ceramic crown, the underlying tooth preparation demonstrated excessive apical placement of the gingival margin and inadequate axial reduction (Figure 2). Initial corrective treatment involved smoothing the previously prepared cementum using a 16-fluted carbide finishing bur. Proper axial-gingival reduction was completed, and the gingival margin was placed coronal to the CEJ of the adjacent central incisor (Figure 3).
The provisional restoration was designed with an under-contoured facial margin that facilitated coronal migration of the facial gingiva over the root surface by a process known as creeping attachment.13-15 This has been reported to result in a stable, long junctional epithelial adhesion or attachment, which is resistant to bacterial infection.16,17
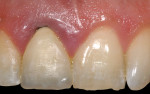
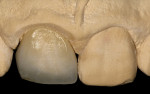
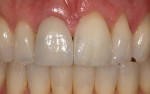
After 6 weeks, the optimal apical location and shape of the definitive facial margin was achieved (Figure 4). Impressions were taken and the metal-ceramic crown delivered. The 1-year clinical appearance demonstrated the stability and clinical health of the facial and proximal gingival profile (Figure 5).
Influence of Crown Contours on the Gingival Profile
The free gingival margin can be moved apically using only the crown convexity without surgical crown lengthening. This requires that the osseous crest be located at an apical position that is > 2 mm.18,19 This permits displacement of the free gingival margin while preserving natural biologic width dimension. In this case, bone sounding was required to precisely determine the location of the alveolar housing.
The patient seen in Figure 6 had a facial gingival asymmetry of the right central incisor tooth caused by altered passive eruption.20,21 A ceramic crown restoration was required due to inadequate remaining coronal tooth support. Bone sounding using a periodontal probe indicated that the intracrevicular sulcus was 1 mm for the left central incisor and 2.5 mm for the right central incisor (altered passive eruption). Therefore, the free gingival margin could be positioned apically 1.5 mm without impinging upon the junctional epithelial attachment.
Prior to placement of the gingival margin, a non-impregnated retraction cord was placed into the sulcus (Figure 7) to move the free gingival margin apically to the same level as the adjacent central incisor. The position of the facial free gingival margin was determined by selective removal of stone from the master cast, developing symmetry with the adjacent central incisor (Figure 8). The convex CEJ contour of the definitive crown moved the free gingival margin into an esthetic and biologically acceptable position. The 1-year appearance of the gingival profile confirmed clinical health and positional stability (Figure 9).
Restoration of Interproximal Papilla
Clinicians have attempted to surgically regenerate interproximal papilla, generally with less-than-stellar results. A systematic review of the literature by Blatz and Hürzeler attests to the unpredictability of these techniques.22 Fortunately, the potential for incisal migration of papilla is robust when underlying proximal bone support is favorable.23 A recent clinical report demonstrated that papillary enhancement with surgical augmentation was not possible without additive alteration of the proximal contours of the central incisor teeth.24
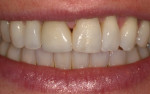
The patient shown in Figure 10 had a papillary height deficiency between the maxillary central incisors that was visible upon normal smile. Replacement of the defective right central incisor metal-ceramic crown provided an opportunity to enhance the height of the proximal papilla, solely with the restorative contours.
The diagnostic wax-up determined that the mesio-distal size discrepancies could be addressed with a feldspathic porcelain resin-bonded restoration on the mesial of the left central incisor. Favorable underlying osseous support afforded the potential for incisal migration of the proximal papilla.
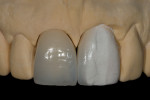
The dental technician fabricated the ceramic crown and resin-bonded restoration. The preparation outline followed facial undulations of the natural tooth surface to camouflage the facial margin (Figure 11). The proximal restorative contour determined the form of the interdental papilla (Figure 12). The patient’s smile seen at the 1-year follow-up (Figure 13) reflected the improved papilla height and form and demonstrated the long-term stability of the proximal papilla.
Implant-Supported Crown Contours
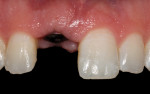
Although an implant-supported central incisor crown may closely duplicate a natural tooth, differences of the free gingival margin may lead to visual disharmony, as seen in Figure 14. Developing optimal surrounding hard and soft tissues is challenging due to the flat restorative platform of dental implants in contrast to the parabolic form of the CEJ found in natural teeth.25,26
When implant-supported crowns are adjacent to natural teeth, the presence or absence of a papilla is dependent on the vertical position of the periodontal attachment on the adjacent tooth (Figure 15). When the adjacent tooth lacks proximal attachment loss, a vertical distance from the contact point to the osseous crest of less than 5 mm possesses the highest potential for complete papilla fill.27 This is assisted by the intact crestal bone and dentogingival and dentoperiosteal fiber groups of the adjacent tooth.28
In this case, the master cast was altered to duplicate the CEJ profile of the right maxillary central incisor tooth. The outline of the CEJ in the definitive metal-ceramic crown determined the gingival facial and proximal profile; this sometimes requires several months. The favorable soft-tissue contours seen 1 year after placement of the definitive zirconia abutment and ceramic crown (Figure 16) confirmed this papillary regenerative potential.
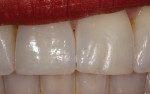
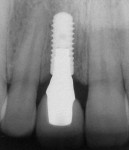
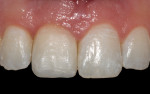
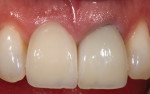
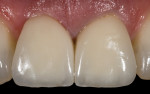
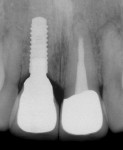
Another case dealing with implant-supported crown contours demonstrated a discrepancy of the free gingival margins associated with the maxillary right implant-supported central incisor and the left tooth-supported complete ceramic crown (Figure 17). The linear slope of the original implant-supported ceramic crown (Figure 18, left) caused apical migration of the free gingival margin. The final crown contours, with the concavity of the root form and the convexity of the crown form, determined the soft-tissue profile (Figure 18, right). The definitive porcelain crown restorations enhanced the natural tooth contour, chroma, hue, surface texture, and gingival frame, as is apparent in the clinical photograph taken at the time of final restoration placement (Figure 19), as well as in the radiograph (Figure 20).
Discussion and Conclusion
Crown restorations placed in the esthetic zone are inherently complex. The collaborative knowledge and skills of an experienced treatment team are frequently required. Often, a nonsurgical, restorative solution can result in the desired gingival esthetics. However, a thorough understanding of the soft and hard tissues adjacent to the restoration is required to avoid an iatrogenic inflammatory response caused by excessive apical placement of the crown margins.29-32
Evaluation of the osseous support with periodontal probe sounding provides the restorative dentist valuable information regarding the feasibility of a restorative solution to a gingival defect. Facial gingiva of maxillary anterior teeth without periodontal disease are highly variable and range from 2 mm to 5 mm.33 The cervical convexity has been shown to form the gingival contour following facial root coverage procedures.34 The CEJ contour of an implant-supported crown determines the facial and proximal soft-tissue contours.35
About the Authors
Richard P. Kinsel, DDS
Health Sciences Associate Clinical Professor
Department of Preventive and Restorative Dental Sciences
University of California San Francisco
San Francisco, California
Private Practice
Foster City, California
Bryan I. Pope, DMD, MSD
Private Practice
Peninsula Periodontal Associates
San Mateo, California
Daniele Capoferri
Owner, Swiss Dental Design
Foster City, California
References
1. Prichard J. Gingivoplasty, gingivectomy and osseous surgery. J Periodontol. 1961;32:275-282.
2. Bensimon GC. Surgical crown-lengthening procedure to enhance esthetics. Int J Periodontics Restorative Dent. 1999;19(4):332-341.
3. Grant DA, Stern IB, Listgarten MA. Periodontics In the Tradition of Gottlieb and Orban. 6th ed. St. Louis, MO: CV Mosby; 1988.
4. Mattos CM, Santana RB. A quantitative evaluation of the spatial displacement of the gingival zenith in the maxillary anterior dentition. J Periodontol. 2008;79(10):1880-1885.
5. Newman MG, Takei HH, Klokkevold PR, Carranza FA. Carranza’s Clinical Periodontology. 10th ed. Philadelphia, PA: Saunders Elsevier; 2006.
6. Tarnow DP, Magner AW, Fletcher P. The effect of the distance from the contact point to the crest of bone on the presence or absence of the interproximal dental papilla. J Periodontol. 1992;63(12):995-996.
7. Tarnow D, Elian N, Fletcher P, et al. Vertical distance from the crest of bone to the height of the interproximal papilla between adjacent implants. J Periodontol. 2003;74(12):1785-1788.
8. Choquet V, Hermans M, Adriaenssens P, et al. Clinical and radiographic evaluation of the papilla level adjacent to single-tooth dental implants. A retrospective study in the maxillary anterior region. J Periodontol. 2001;72(10):1364-1371.
9. Kurth JR, Kokich VG. Open gingival embrasure after orthodontic treatment in adults: Prevalence and etiology. Am J Orthod Dentofacial Orthop. 2001;120(2):116-123.
10. Donaldson D. Gingival recession associated with temporary crowns. J Periodontol. 1973;44(11):691-696.
11. Turner CH. A retrospective study of the fit of jacket crowns placed around gold posts and cores, and the associated gingival health. J Oral Rehabil. 1982;9(5):427-434.
12. Kois JC. The restorative-periodontal interface: biological parameters. Periodontol 2000. 1996;11:29-38.
13. Matter J. Cimasoni G. Creeping attachment after free gingival grafts. J Periodontol. 1976;47(10):574-579.
14. Bell LA, Valluzzo TA, Garnick JJ, Pennel BM. The presence of “creeping attachment” in human gingiva. J Periodontol. 1978;49(10):513-517.
15. Matter J. Creeping attachment after free gingival grafts. A five-year follow-up study. J Periodontol. 1980;51(12):681-685.
16. Magnusson I, Runstad L, Nyman S, Lindhe J. A long junctional epithelium–a locus minoris resistentiae in plaque infections? J Clin Periodontol. 1983;10(3):333-340.
17. Beaumont RH, O’Leary TJ, Kafrawy H. Relative resistance of long junctional epithelial adhesions and connective tissue attachments to plaque-induced inflammation. J Periodontol. 1984;55(4):213-223.
18. Gargiulo AW, Wentz FM, Orban B. Dimensions and relations of the dentogingival junction in humans. J Periodontol. 1961;32(3):261-267.
19. Vacek JS, Gehr ME, Assad DA, et al. The dimensions of the human dentogingival junction. Int J Periodontics Restorative Dent. 1994;14(2):154-165.
20. Dolt AH 3rd, Robbins JW. Altered passive eruption: an etiology of short clinical crowns. Quintessence Int. 1997;28(6):363-372.
21. Gillen RJ, Schwartz RS, Hilton TJ, Evans DB. An analysis of selected normative tooth proportions. Int J Prosthodont. 1994;7(5):410-417.
22. Blatz MB, Hürzeler MB, Strub JR. Reconstruction of the lost interproximal papilla-presentation of surgical and nonsurgical approaches. Int J Periodontics Restorative Dent. 1999;19(4):395-406.
23. van der Veldon U. Regeneration of the interdental soft tissue following denudation procedures. J Clin Periodontol. 1982;9(6):455-459.
24. Geurs NC, Romanos AH, Vassilopoulos PJ, Reddy MS. Efficacy of micronized acellular dermal graft for use in interproximal papillae regeneration. Int J Periodontics Restorative Dent. 2012;32(1):49-58.
25. Holt RL, Rosenberg MM, Zinser PJ, Ganeles J. A concept for a biologically derived, parabolic implant design. Int J Periodontics Restorative Dent. 2002;22(5):473-481.
26. Gallucci GO, Belser UC, Bernard JP, Magne P. Modeling and characterization of the CEJ for optimization of esthetic implant design. Int J Periodontics Restorative Dent. 2004;24(1):19-29.
27. Choquet V, Hermans M, Adriaenssens P, et al. Clinical and radiographic evaluation of the papilla level adjacent to single-tooth dental implants. A retrospective study in the maxillary anterior region. J Periodontal. 2001;72(10):1364-1371.
28. Ten Cate AR. Ten Cate’s Oral Histology: Development, Structure, and Function. 5th ed. St. Louis, MO: Mosby-Year Book Inc.; 1998.
29. Nevins M, Skurow HM. The intracrevicular restorative margin, the biologic width, and the maintenance of the gingival margin. Int J Periodontics Restorative Dent. 1984;4(3):31-49.
30. Dragoo MR, Williams GB. Periodontal tissue reactions to restorative procedures. Int J Periodontics Restorative Dent. 1981;1(1):8-23.
31. Wilson RD, Maynard JG. The relationship of restorative dentistry to periodontics. In: Prichard JF. The Diagnosis And Treatment of Periodontal Disease in General Dental Practice. Philadelphia, PA: W.B. Saunders Co.; 1979.
32. Wilson RD, Maynard G. Intracrevicular restorative dentistry. Int J Periodontics Restorative Dent. 1981;1(4):34-49.
33. Perez JR, Smukler H, Nunn ME. Clinical dimensions of the supraosseous gingivae in healthy periodontium. J Periodontol. 2008;79(12):2267-2272.
34. Cario F, Pini-Prato GP. A technique to identify and reconstruct the cementoenamel junction level using combined periodontal and restorative treatment of gingival recession. A prospective clinical study. Int J Periodontics Restorative Dent. 2010;30(6):573-581.
35. Kinsel RP, Capoferri D. A simplified method to develop optimal gingival contours for the single implant-supported, metal-ceramic crown in the aesthetic zone. Pract Proced Aesthet Dent. 2008;20(4):231-236.