Nonvital Tooth Bleaching: A Case Discussion for the Clinical Practice
Maciej Zarow, DDS, PhD
Discolored root canal–treated anterior teeth can negatively affect a patient’s appearance. Endodontically treated teeth can cause impaired crown stiffness due to structural loss of hard tissue.1 In the past, many root canal–treated teeth were routinely reconstructed with metal posts and crowns. More conservative strategies such as internal bleaching, fiber posts, composite restorations, or minimally invasive porcelain veneers provide alternative contemporary treatment options.1
Due to a relative lack of sound empirical data, today’s clinical concepts regarding the restoration of root canal–treated teeth are not well defined. The wide range of published opinions can be perplexing and may lead to less-than-optimal treatment decisions. There is also debate about whether teeth that have been root canal–treated or discolored should be bleached at all. Through a case report, this article provides dental practitioners with guidance about the available options for bleaching discolored anterior teeth after root canal therapy.
Internal Bleaching
In terms of biomechanics and biomimetics, there is no better material than the natural tooth itself. Thus, the less a tooth is reduced, the better the clinical long-term outcome and potential for re-intervention.2 If using porcelain veneers or crowns to mask the dark color of a tooth, a dental laboratory requires more tooth reduction, which significantly diminishes the mechanical and adhesive properties of restorations. For longevity of porcelain veneers, the presence of enamel is crucial. Reducing the enamel lowers the adhesion value of the porcelain veneer to the tooth structure, making the final restoration less predictable. Therefore, instead of reducing tooth structure, the aim should be to try to change the color as much as possible by bleaching internally.
Internal bleaching is well documented in the literature.2 Sodium perborate remains the primary choice in bleaching materials.3,4 The treatment can be successful even for a tooth that received root canal treatment and became discolored many years previously. However, careful evaluation of the tooth and surrounding tissues is necessary for the success of the bleaching, because the outcome depends on the identification of etiology, correct diagnosis, and proper execution of bleaching technique procedures.3 Bleaching success also requires healthy periodontal tissues, a properly obturated canal, and most of all, a perfectly positioned barrier in order to prevent leakage of the bleaching agent into the periapical tissues.4
Today, the most commonly used method is the walking bleach technique—ie, bleaching treatment that takes place between the patient’s office visits. The term was first used by Nutting and Poe5 in 1963, and the method has been modified by eliminating the use of 30% aqueous solution of hydrogen peroxide (H2O2), making it a very popular and safe technique.2,6Sodium perborate powder mixed with water to a thick consistency of “wet snow” is placed, usually in two treatments. If no significant improvement is observed after three attempts, the tooth should be reassessed to confirm the etiology of discoloration and suitability of the treatment plan.4 Although relapse to discoloration is possible and described in the literature,6 if it occurs at all, the tooth usually is not discolored to the same degree that it had been prior to the treatment.3
Practitioners can also apply some contemporary methods to reduce the probability of discoloration relapse. The first is a home-use custom tray method with a reservoir for a bleaching agent (eg, 10% to 15% carbamide peroxide) placed periodically on the buccal and palatal surfaces of the treated tooth (recommended for overnight use for 1 week every 6 months).3 The second method requires the mandatory suspension of final restoration for 2 weeks7,8 in order to remove the inhibitory effect on the polymerization of resin-based materials. It is believed that more stable results are achieved due to better adhesion and reduced microleakage of the final restoration.
Intracoronal bleaching, in general, is an effective and safe procedure, although it has been associated with a certain level of risk, including cervical root resorption (CRR). Though the mechanism of CRR is not yet fully known, it has been speculated that the bleaching agent diffuses through dentinal tubules, reaching periodontal tissues and causing necrosis of the cementum, inflammation of the periodontal ligament, and CRR.9-11 Clinical observations indicate that previous traumatic injury, the patient’s age, and a high concentration of H2O2 in combination with heating appear to be risk factors that promote cervical resorption.10-14 Therefore, the use of highly concentrated H2O2 and heat for internal bleaching should be avoided. Higher risk for CRR stimulation associated with nonvital bleaching therapy pertains to adolescents, as well as to teeth that after being injured have visible craze lines extending into the subgingival area, and cases where there is a limited amount of tooth structure.3
Case Report
Patient History and Chief Complaint
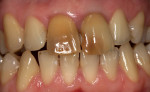
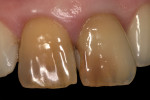
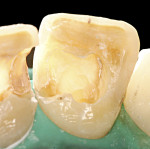
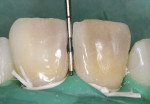
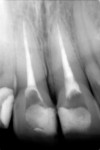
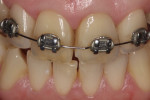
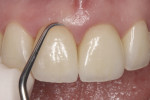
In 2004, a 25-year-old woman with fair oral hygiene was referred to the dental clinic with a stated desire to improve her smile and a request for what she called “esthetic full ceramic crowns.” Her chief concerns included extensive discoloration of teeth Nos. 8 and 9 (Figure 1 and Figure 2). Her medical history was unremarkable, except for a known allergy to penicillin. Her dental history revealed no periodontal, biomechanical, or functional problems. However, because of some minor malocclusal problems, orthodontic treatment was discussed, but the patient chose to postpone such treatment. Based on the patient’s interview, it was determined that she had undergone endodontic treatment about 12 years previously, and gradual discolorations appeared within a few years after this. The following treatment plan was proposed to the patient.
Retreatment
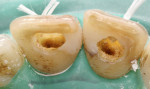
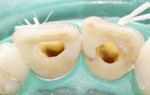
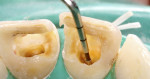
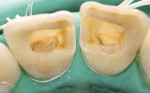
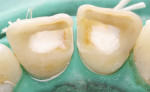
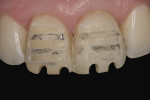
After rubber dam isolation, root canal access was performed. The old paste filling material was removed entirely (Figure 3 and Figure 4), and after shaping and finishing with rotary files (ProTaper®, DENTSPLY, www.dentsply.com) and irrigation with 5.25% sodium hypochlorite (NaOCl) and 18% of ethylenediaminetetraacetic acid (EDTA), the root canals were filled by means of the continuous wave technique using an endodontic heat source (System B™, Kerr Dental, www.kerrdental.com) and Obtura (Obtura Spartan Endodontics, www.obtura.com).
Emphasis was placed on removing all the pulp remnants and the existing cement materials from the pulp chamber, particularly from the pulp horns. The author recommends that this procedure be performed using at least 5 times magnification. In this case, a microscope (OPMI® pico, Zeiss, www.zeiss.com) was used to avoid removing additional hard dental structure (Figure 5).
Proposed Treatment Plan
The plan consisted of two main phases. Phase 1 entailed endodontic retreatment of teeth Nos. 8 and 9, whose root canals were filled with paste, not gutta-percha. This phase would include fiber post placement and replacement of existing composite restorations. Because of the extent of the teeth discolorations, the plan for phase 2—covering the teeth with porcelain veneers or full ceramic crowns—would depend on the result of the nonvital bleaching therapy.
Barrier Placement
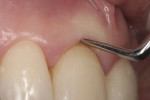
To learn the position of the periodontal ligaments during the barrier placement, a periodontal probe was used to measure the length between the interdental papilla and the incisal edge (Figure 6), and that measurement was applied to the pulp chamber (Figure 7). The barrier was created with glass-ionomer cement in a semilunar shape (Figure 8 and Figure 9) to protect the periodontal ligaments from the diffusion of the bleaching agent while also allowing for diffusion toward the discolored buccal wall of the tooth. A prolonged 10-minute setting time of the glass-ionomer cement was used to achieve a stable barrier. The positioning and appropriate shaping of the barrier are crucial elements to achieve a safe and successful final result of the bleaching. If it is necessary to correct the shape, long shaft drills can be used.
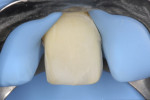
The bleaching agent was prepared in situ from sodium perborate tetrahydrate mixed with 3% hydrogen peroxide, creating a paste with the aforementioned consistency of “wet snow.” The bleaching agent was applied to the pulp chamber with a spatula instrument (LM-Arte Applica, LM-Instruments Oy, www.lm-dental.com) and condensed with a wetted cotton pellet (Figure 10).
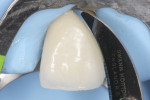
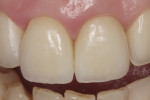
Glass-ionomer cement was used as a temporary material. The patient was also informed about the increased risk for fracture, which can occur between bleaching appointments. She was advised to avoid eating hard foods and chew with caution. The bleaching agent was re-placed at 7 and 14 days after the first appointment. Three rounds of sodium perborate treatment produced satisfactory color improvement (Figure 11).
Reliable bond strength of bleached dental hard tissues can be achieved after 2 weeks.7,8,14 It was during this time that the color of the bleached tooth stabilized and a calcium hydroxide dressing was placed in the pulp chamber in order to buffer the low pH level that can occur on cervical root surfaces after intracoronal application of bleaching agents.
Restorations
Two weeks after the bleaching was completed, the patient returned for a tooth reconstruction appointment. The old restorations and the glass-ionomer cement from the temporary restoration and barrier were removed.
Then the canals were prepared for the placement of fiber posts; this was done without additional hard dental tissue reduction and with removing only gutta-percha, with Gates instruments under microscope magnification.
After the fiber posts were adjusted, the dentin was cleaned with 27-μm aluminum oxide, etched with phosphoric acid, irrigated with distilled water, and delicately dried with paper points. Then the bonding agent (Ena Bond, Micerium S.p.A., www.micerium.com), which was mixed with a chemical catalyzer (Ena Cat, Micerium S.p.A.), was applied to the dentin in two layers and delicately air-blown.
An initial layer of light dentin composite (Enamel Plus, UD1, Micerium S.p.A.) was placed palatally toward the buccal wall of the teeth. Afterward, fiber posts with an opalescent effect (Ena Post, Micerium S.p.A.) were cemented with composite cement (Ena Cem, Micerium S.p.A.) into the canals, thus completing the composite reconstruction.
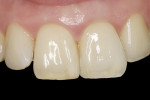
Because of the remarkably good result of the nonvital bleaching (Figure 12), a decision regarding tooth preparation versus indirect restoration fabrication was unnecessary at that time.
Maintenance Protocol
To prolong the good bleaching results and prevent any reoccurrence of discoloration, special bleaching trays with a buccal and lingual reservoir for the bleaching agent can be used. In such a bleaching maintenance protocol, the patient should be instructed to re-bleach the previously discolored teeth for 7 days (at night) once every 6 months.
A comparison between the pre-treatment situation and final result shows that a very good outcome can be achieved in cases of root canal–discolored tooth bleaching, even in those involving old discolorations. Therefore, in this case the patient declined additional treatment for the time being.
Porcelain Veneers
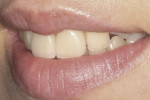
The patient presented to the office 6 years later upon completing the orthodontic treatment that had previously been proposed to her (Figure 13). The upper central incisors, which had been bleached 6 years previously, showed only slight recurrence of discoloration but had not returned to the original dark shade. This time, however, the patient wanted further esthetic improvement, and, therefore, the porcelain veneers discussed 6 years earlier were again proposed.
After a composite additive mock-up was presented to the patient, her phonetics and smile were analyzed precisely. The putty matrix was fabricated in order to control the preparation (silicon index) and produce the temporaries at the following appointment.
At the preparation appointment, shade selection was carried out using the VITA Easyshade® (Vident™, www.vident.com) and 3D Master Shade Guide (Vident). This was done prior to any other procedures to avoid color mistakes that might occur due to dehydration of the teeth. After anesthesia, a bone sounding was performed in order to evaluate the level of the bone crest.15
The preparation was produced starting at the mock-up level (Figure 14) to minimize tooth reduction16; in this way dentin was not exposed so as to avoid increasing biomechanical risk. After placement of a size 00 retraction cord, fine diamonds were used to finalize the preparations. The finishing lines were carried just slightly under the free gingival margin, and the incisal preparation was angled lingually to allow the technician to hide the incisal edge.17 A vinyl polysiloxane impression was taken using a standard two-cord technique, and a bite record and facebow record (ARCUS/ARCUSevo, KaVo ARCUS, www.kavo.com) were taken. The preparation shade was chosen and photographed in order to communicate with the laboratory. The putty matrix was filled with bisphenol A diglycidyl ether methacrylate (bis-GMA) to produce provisionals, and overhangs were removed accordingly.
At the try-in appointment, the provisionals were removed, and porcelain veneers were tried in using glycerin gel before administering anesthesia in order to analyze upper and lower lip positions in relation to the veneers. Once the patient approved them for cementation, the intaglio surfaces were cleaned using 70% alcohol, etched with 10% hydrofluoric acid, and rinsed for 5 minutes in an alcohol ultrasound bath. The veneers were then dried, carefully silanated in several layers (Lute-It® Silane, Pentron, www.pentron.com), and covered by a bonding agent (Ena Bond).18
The patient was anesthetized and rubber dam isolation was obtained (Figure 15). The isolated tooth surfaces were cleaned off using air abrasion with 27-μm aluminum oxide at low pressure (40 psi). The teeth were each etched for 15 seconds using 37% phosphoric etch and rinsed thoroughly. Two coats of bonding agent (Ena Bond) were placed on the prepared teeth, then the veneers were loaded with a light-curing composite (Enamel Plus, UD3) seated on the teeth using apical and inward pressure. Most excess cement was immediately removed using a 6A explorer (Hu-Friedy, www.hu-friedy.com). Then the veneers were “tacked” into place with a preliminary light-cure, and initial cement removal was obtained with waxed floss. Glycerin gel was applied to all margins for oxygen inhibition, and final curing was carried out for 60 seconds from each side of the veneer (buccal-cervically, buccal-middle third, and incisally from the palatal side). Final cement removal was accomplished using a #12B scalpel blade (Figure 16) and, after removal of the rubber dam, a hand scaler (Figure 17 and Figure 18).
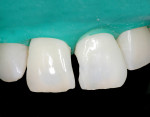
Margins were polished using a brownie point. The veneers were cemented in isolation, one after another. After occlusion was checked, a final polish of the veneers was accomplished using a porcelain polishing paste and a felt disc. The final results can be seen in Figure 19 and Figure 20.
Conclusion
Bleaching of root canal–treated discolored teeth with sodium perborate tetrahydrate should be considered as a first option in an esthetic treatment plan. Effective nonvital tooth beaching demands complete removal of the existing cements, restorations, and pulp remnants, as well as precise barrier placement under microscope magnification. Appropriate patient indication for nonvital bleaching, along with proper calcium hydroxide dressing, in addition to accurate barrier placement, constitute crucial elements to prevent external cervical resorption. Finally, ensuring that adhesive bonding is delayed at least 14 days after bleaching and the use of preventive bleaching trays can play key roles in maintaining the color of bleached teeth.
Acknowledgment
All photos used in this article were printed with permission from Zarow M. Endoprotetyka - przewodnik dla praktyki. Barcelona, Spain: Internationale Quintessence Publishing (2013).
About the Author
Maciej Zarow, DDS, PhD
Private Practice
Krakow, Poland
References
1. Zarow M, Devoto W, Saracinelli M. Reconstruction of endodontically treated posterior teeth—with or without post? Guidelines for the dental practitioner. Eur J Esthet Dent. 2009;4(4):312-327.
2. Meyenberg KH. Nonvital teeth and porcelain laminate veneers— a contradiction? Eur J Esthet Dent. 2006;1(3):192-206.
3. Zarow M, D’Acangelo C, Felippe LA, et al. Endo-Prosthodontics: Guidelines for Clinical Practice. Poland, Warszawa: Quintessence Publishing Co. Inc.; 2013.
4. Baba NZ. Contemporary Restoration of Endodontically Treated Teeth: Evidence-Based Diagnosis and Treatment Planning. Chicago, IL: Quintessence Publishing Co. Inc.; 2013.
5. Nutting EB, Poe GS. A new combination for bleaching teeth. J So Calif Dent Assoc. 1963;31(9):289-291.
6. Dietschi D. Nonvital bleaching: general considerations and report of two failure cases. Eur J Esthet Dent. 2006;1(1):52-61.
7. Garcia-Godoy F, Dodge WW, Donohue M, O’Quinn JA. Composite resin bond strength after enamel bleaching. Oper Dent. 1993;18(4):144-147.
8. Lai SC, Mak YF, Cheung GS, et al. Reversal of compromised bonding to oxidized etched dentin. J Dent Res. 2001;80(10):1919-1924.
9. Madison S, Walton R. Cervical root resorption following bleaching of endodontically treated teeth. J Endod. 1990;16(12):570-574.
10. Rotstein I, Friedman S, Mor C, et al. Histological characterization of bleaching-induced external root resorption in dogs. J Endod. 1991;17(9):436-441.
11. Lado EA, Stanley HR, Weisman MI. Cervical resorption in bleached teeth. Oral Surg Oral Med Oral Pathol. 1983;55(1):78-80.
12. Buchalla W, Attin T. External bleaching therapy with activation by heat, light or laser—a systematic review. Dent Mater. 2007;23(5):586-596.
13. Lin LC, Pitts DL, Burgess LW Jr. An investigation into the feasibility of photobleaching tetracycline-stained teeth. J Endod. 1988;14(6):293-299.
14. Plotino G, Buono L, Grande NM, et al. Nonvital tooth bleaching: a review of the literature and clinical procedures. J Endod. 2008;34(4):394-407.
15. Kois JC. The restorative-periodontal interface: biological parameters. Periodontol 2000. 1996;11:29-38.
16. Magne P, Belser U. Novel porcelain laminate preparation approach driven by a diagnostic mock-up. J Esthet Restor Dent. 2004;16(1):7-16.
17 Kois JC, McGowan S. Diagnostically generated anterior tooth preparation for adhesively retained porcelain restorations: rationale and technique. J Calif Dent Assoc. 2004;32(2):161-166.
18. Magne P, Belser U. Bonded Porcelain Restorations in the Anterior Dentition: A Biomimetic Approach. Chicago, IL: Quintessence Publishing Co. Inc.; 2002.