Effects of a Vibratory Device on Pain from Anesthetic Injections
Michael G. DiFelice, DMD, MS; Kraig S. Vandewalle, DDS, MS; Steven C. Maller, DDS, MS; and Raymond H. Hancock, DDS, MS
Abstract:
BACKGROUND: A randomized block, split-mouth design was used to determine the effectiveness of a vibratory device with topical anesthetic compared to topical anesthetic only in reducing the pain experienced during an inferior alveolar nerve block. METHODS: Twenty participants each received two inferior alveolar injections with a 5-minute interval between injections, one with topical anesthetic and one with topical anesthetic and a vibratory device. Each injection included a 2-minute application of topical anesthetic gel at the injection site. Local anesthetic was administered bilaterally using a 27-gauge needle with or without the vibratory device. Participants rated the pain they experienced after each injection by using a visual analog scale (VAS). A mean VAS score and standard deviation was determined per group. Data was analyzed with a paired t test (α = 0.05). RESULTS: The group receiving the vibratory device with topical anesthetic had a mean VAS score of 21.2 mm ± 18.6 mm, and the group receiving the topical anesthetic alone had a VAS score of 38.7 mm ± 23.3 mm. CONCLUSION: The use of the vibratory device and topical anesthetic significantly reduced the pain experienced during the administration of a local anesthetic injection compared with the use of topical anesthetic alone (P = 0.006).
Pain associated with dental injections can create fear and anxiety for patients and become a major obstacle in dental care. The minimization or removal of pain opens the doorway for less stressful dental encounters.1-3 Dentistry has developed a myriad of different theories, techniques, devices, and drugs to help reduce and/or eliminate this chief concern in patient care. Whether it is through vibrating the tissue, application of topical anesthesia, using cold spray, applying pressure, or the use of a mechanical delivery system, the potential for reducing a patient’s pain and fear of dental injections certainly exists.1,2
Clinical research has shown that the application of a topical anesthetic for at least 2 minutes to dry oral mucosa is effective in the reduction of injection pain.1,4,5 However, the effectiveness of the application of topical anesthesia may be related to the site of the injection. At the pterygotemporal depression, ie, the entrance site for the needle in an inferior alveolar nerve block injection, there appears to be a slight, but not substantially relevant, reduction of pain when applying topical anesthesia.4,6 Friedman and Hochman reported that a steady, controlled, computerized injection with topical anesthesia combined with a patient’s influenced expectations can effectively decrease the initial pain during dental injections of the maxillary arch.7
The gate-control theory proposes that the activation of A-beta non-nociceptive fibers by tactile stimulation, touch, or vibration has the potential to override pain signals at the secondary neuronal cell bodies in the dorsal horn from A-delta and C nociceptive fibers. Specifically, within the substantia gelatinosa of the dorsal horn, the non-nociceptive A-beta fibers inhibit transmission of pain signals by increasing the firing of inhibitory interneurons, thereby “closing the gate” and blocking the further projection of pain signals. Following this line of thinking, a painless dental injection may be achieved by using a vibrating device to provide a tactile distraction.8-10
The largest cranial nerve, the trigeminal, is involved with the sensation of pain from an inferior alveolar block injection. Sensory input travels along the three branches of this nerve—the ophthalmic, maxillary, and mandibular—converging at the trigeminal ganglion, where the signal continues to the brainstem via the pons.11 The trigeminal ganglion is considered analogous to the dorsal root ganglia of the spinal cord, acting in the same manner and with similar structural composition.12
Saijo et al conducted a clinical study and found no statistically significant pain reduction when using a device called VibraJect® (VibraJect, LLC, www.dental-syringe.net), which vibrates the syringe and the attached needle.10 Yoshikawa et al also found no significant pain reduction with the use of the VibraJect device versus a typical dental syringe.13 However, two International Association of Dental Research abstracts reported a decrease in pain during intraoral injections with the use of the VibraJect device.14,15 Hutchins et al conducted similar research with topical anesthesia and a vibrating reconfigured electric shaver, creating non-nociceptive tactile tissue stimulation.1 A statistically significant decrease in pain was reported by patients undergoing maxillary premolar injections with topical anesthetic and vibration; however, the authors reported that the amount of decrease in pain was of questionable clinical significance. It was also discovered that there was no effect with vibration 1 minute before injection. Still, it may be theoretically possible that using a device that causes vibration of the surrounding tissue but is not connected to a syringe and needle may create the distraction needed to block the pain signal.10
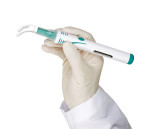
A new vibrating dental device was recently introduced (DentalVibe® GEN II, BING Innovations, www.dentalvibe.com) that the company claims can be used along with any dental anesthetic injection syringe to deliver comfortable injections in all areas of the mouth (Figure 1 and Figure 2). The handheld device provides illumination, retraction, and vibration with VibraPulse™ technology (BING Innovations) through a disposable Comfort Tip®. The company asserts that the “VibraPulse delivers a pulsed, percussive vibration with enhanced amplitude, which gently taps the mucosa in a synchronized, changing pattern.” Simply stated, the device vibrates against the tissue with a variable force and pattern of oscillations that reportedly creates a changing stimulus that sends a signal which distracts the brain and blocks the sensation of pain from the injection.16 A potential contraindication to the use of the device would be the inability of a patient to adequately open their jaw sufficiently to allow full access. (The cost of the DentalVibe GEN II is $695.00 for the handpiece and charging base. The Comfort Tips® cost $69.50 per box of 50.)
The purpose of this study was to evaluate the use of the DentalVibe GEN II vibrating dental device in the potential reduction or elimination of pain with inferior alveolar injections. The injection pain experienced by the patients was evaluated through the use of a visual analogue scale (VAS). The VAS is a reliable, self-reporting device used to measure subjective phenomena in an experimental setting, specifically in this study, a patient’s level of pain.17-19 The null hypothesis tested was that there would be no significant difference in pain with an inferior alveolar injection based on VAS scores with or without the use of the vibratory device.
Materials and Methods
The patient sample for this study consisted of 20 adults undergoing treatment requiring bilateral inferior alveolar blocks. The participants were selected from a pool of patients available for treatment at Dunn Dental Clinic, Joint Base, San Antonio-Lackland, Texas. All of the selected patients were in good general health and classified as ASA PS1 or ASA PS2, according to the American Society of Anesthesiologists Physical Status Classification System. The Institutional Review Board at Wilford Hall Ambulatory Surgical Center, Joint Base, San Antonio-Lackland, Texas approved the protocol and the informed consent document. All subjects signed an informed consent document before any study-related procedures were conducted. Extractions or scaling and root planing with local anesthesia in bilateral posterior areas of the mandible were the specific treatments selected for the study. Patients receiving treatment for chronic pain conditions were excluded from the study. Also, pregnant women and patients with an allergy to ester products or who were diagnosed with a history of methemoglobinemia as a result of the use of topical benzocaine were excluded from the study. The sample size of 20 subjects provided 80% power to detect a 0.75 standard deviation when using a paired t test and an α level of 0.05 to compare the VAS scores for the two treatments.
A randomized block, split-mouth design was conducted with an anesthetic injection on the mandibular left and right ramus area (inferior alveolar nerve block). The same operator performed the injections to standardize the flow rate and delivery style and the preparation of the tissue sites. Each patient received a total of two inferior alveolar injections with a 5-minute interval between injections. Both the treatment (with or without the vibratory device) and side of treatment (left or right) were randomized using a block design. The subjects evaluated the efficacy of the vibratory device with topical anesthesia in reducing pain with injection compared to topical anesthetic alone when both were applied to the inferior alveolar nerve block injection sites on each side of the mouth. Patients reported their perceived pain from the overall experience of the anesthetic injection immediately after each injection.
Topical benzocaine 20% gel (Topex®, Sultan Healthcare, www.sultanhc.com) was used to prepare the sites receiving the inferior alveolar nerve block injection with and without the vibratory device at the pterygotemporal depression. The method of application of the topical gel was as follows: 1) The gel was placed in a syringe, and 0.1 mL was inserted onto a cotton-tip applicator; 2) The mucosa at the pterygotemporal depression was dried with a 2” x 2” gauze; and 3) The gel on the cotton-tip applicator was then applied to the mucosa for 2 minutes.
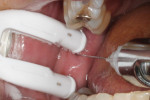
For the side receiving the vibratory device, the anterior border of the ramus was palpated with a finger in a typical manner and the pterygotemporal depression was visualized. The finger was removed and the retracting component of the device, which also provides illumination and vibration, was placed at the injection site. The needle was inserted as close to the prong of the Comfort Tip as possible without contacting it, per the manufacturer’s instructions (Figure 3). The area was stimulated for 5 seconds before inserting the needle. The vibration continued while the 27-gauge (0.406 mm x 32 mm) needle was inserted. The local anesthetic (1.7 mL of 2% lidocaine with 1:100,000 epinephrine) was deposited over a 30-second interval. Vibration of the injection site continued for 5 seconds after the needle was removed, per the manufacturer’s instructions.
The patients’ report of injection pain was evaluated based on the VAS. The VAS is a 100-mm horizontal line with descriptive anchors at each end. The left end was labeled “no pain/no hurting” and the right side and opposite end was labeled “worst possible pain/hurting a whole lot.” Each patient was instructed to mark a vertical line within the 100-mm scale to indicate his or her discomfort level after the injection. The VAS pain score was calculated by measuring the millimeter distance from the left end of the scale using a digital caliper. A larger score translated to a higher pain intensity experienced by the patient. A mean and standard deviation of the VAS values were determined for each of the two groups of injection types. Data was analyzed with a paired t test (α = 0.05).
Results
The participant pool was made up of 12 men and 8 women whose ages ranged from 27 to 78 years (average age, 52.5 years). The group receiving the vibratory device with topical anesthetic had a mean VAS score of 21.2 mm ± 18.6 mm, and the group receiving the topical anesthetic alone had a VAS score of 38.7 mm ± 23.3 mm. The combination of the vibratory device and topical anesthetic significantly reduced the pain experienced during the administration of a local anesthetic injection compared to the use of topical anesthetic alone (P = 0.006).
Discussion
The null hypothesis was rejected. A significant difference was found between VAS scores based on the use of a vibratory device during an inferior alveolar local anesthetic injection. Overall, 15 of the 20 patients (75%) reported a decrease in pain with the device, as they rated the entire injection experience. Many patients stated that the initial pain on insertion of the needle into the tissue was of the same intensity with or without the vibratory device. However, the movement of the needle and delivery of anesthetic during the injection was reportedly not detectable with the use of the vibratory device, therefore providing a more pleasant experience for the patient. Two of the 20 patients (10%) stated that the injections with or without the vibratory device were similar. Three of the 20 patients (15%) stated that they simply did not like the device and felt that the injections were actually more uncomfortable. The number of patients who reported less pain with the vibratory device was significantly greater than those who reported discomfort (sign test, P = 0.008). Anecdotally, 50% of the patients reported that the onset of anesthesia was faster with the DentalVibe GEN II, which supports the manufacturer’s claim that leaving the device on the injection site after the injection facilitates the dispersion of the solution to create a more rapid onset of anesthesia. There was no difference noted in achieving anesthetic success or the need for supplemental injections between the two injection types.
The use of the vibratory device proved to be a significant adjunct to anesthesia delivery. Previous research evaluating the effect of a commercial vibratory device, VibraJect, on the reduction of pain with dental injections was equivocal, with some studies showing a reduction in pain14,15 and others demonstrating no significant difference.10,13 However, VibraJect is a device that attaches to the syringe and vibrates the attached needle, while DentalVibe GEN II is marketed as a separate handpiece that allows tissue retraction, illumination, and oscillation independent from the dental syringe.
Limitations of this study include the inability to control confounding variables such as rate of injection administration and the possible placebo effect from the use of the vibratory device. Regardless of the placebo effects, the use of the DentalVibe GEN II resulted in a more pleasant experience as reported by most of the patients. While similar in use to a handheld soft-tissue retractor, such as a dental mirror or tongue depressor, tactile sensation of intraoral landmarks is reduced with this device, making it paramount that anatomical landmarks be located before placing the device. Also, if the patient’s anterior border of the ramus is not easily palpable because of excessive tissue coverage or anatomic variance, ideal location for placement of the Comfort Tip may be a challenge.
In this study, the manufacturer’s recommendation of the application of topical anesthetic for 2 minutes before the use of the vibratory device was followed. Future studies should evaluate the use of a vibratory device with and without topical anesthetic, and also evaluate its effectiveness at other intraoral sites.
Conclusion
The combination of a vibratory device and topical anesthetic during local anesthetic injections was more effective compared with the use of topical anesthetic alone in reducing the pain experienced by participants who received inferior alveolar nerve block injections.
DISCLOSURE
The views expressed in this study are those of the authors and do not reflect the official policy of the United States Air Force, the Department of Defense, or the United States Government. The authors do not have any financial interest in the companies whose materials are discussed in this article.
References
1. Hutchins HS Jr, Young FA, Lackland DT, Fishburne CP. The effectiveness of topical anesthesia and vibration in alleviating the pain of oral injections. Anesth Prog. 1997;44(3):87-89.
2. Kosaraju A, Vandewalle KS. A comparison of a refrigerant and a topical anesthetic gel as preinjection anesthetics: a clinical evaluation. J Am Dent Assoc. 2009;140(1):68-72.
3. Milgrom P, Coldwell SE, Getz T, et al. Four dimensions of fear of dental injections. J Am Dent Assoc. 1997;128(6):756-766.
4. Evers H, Haegerstam G. Introduction to Dental Local Anesthesia. 2nd ed. Fribourg Switzerland: Mediglobe SA Publishing; 1990;29-30,59-87.
5. Kincheloe JE, Mealiea WL Jr, Mattison GD, Seib K. Psychophysical measurement on pain perception after administration of a topical anesthetic. Quintessence Int. 1991;22(4):311-315.
6. Nakanishi O, Haas D, Ishikawa T, et al. Efficacy of mandibular topical anesthesia varies with the site of administration. Anesth Prog. 1996;43(1):14-19.
7. Friedman MJ, Hochman MN. The AMSA injection: a new concept for local anesthesia of maxillary teeth using a computer-controlled injection system. Quintessence Int. 1998;29(5):297-303.
8. Melzack R. Recent concepts of pain. J Med. 1982;13(3):147-160.
9. Melzack R, Wall PD. Pain mechanisms: a new theory. Science. 1965;150(3699):971-979.
10. Saijo M, Ito E, Ichinohe T, Kaneko Y. Lack of pain reduction by a vibrating local anesthetic attachment: a pilot study. Anesth Prog. 2005;52(2):62-64.
11. de Leeuw R. Orofacial Pain: Guidelines for Assessment, Diagnosis, and Management. 4th ed. Chicago, IL: Quintessence Publishing; 2008:3-10.
12. Sessle BJ, Hu JW, Amano N, Zhong G. Convergence of cutaneous, tooth pulp, visceral, neck and muscle afferents onto nociceptive and non-nociceptive neurones in trigeminal subnucleus caudalis (medullary dorsal horn) and its implications for referred pain. Pain. 1986;27(2):219-235.
13. Yoshikawa F, Ushito D, Ohe D, et al. Vibrating dental local anesthesia attachment reduce injection pain. J Jpn Dent Soc Anesthesiol. 2003;31:194-195.
14. Murray P, Terrett K, Lynch E, Hussey DL. Efficacy of a vibrating dental syringe attachment on pain levels [abstract]. J Dent Res. 2003;81. Abstract 1177.
15. Terrett K, Murray P, Hussey D, Lynch E. Study assessing the effectiveness of a vibrating dental syringe attachment [abstract]. J Dent Res. 2004;82. Abstract 3538.
16. DentalVibe 3-in-1 Injection Comfort System. https://www.dentalvibe.com. Accessed February 17, 2014.
17. Miller MD, Ferris DG. Measurement of subjective phenomena in primary clinical care research: the Visual Analogue Scale. Fam Pract Res J. 1993;13(1):15-24.
18. Price DD, Bush FM, Long S, Harkins SW. A comparison of pain measurement characteristics of mechanical visual analogue and simple numerical rating scales. Pain. 1994;56(2):217-226.
19. Price DD, McGrath PA, Rafii A, Buckingham B. The validation of visual analogue scales as ratio scale measures for chronic and experimental pain. Pain. 1983;17(1):45-56.
About the Authors
Michael G. DiFelice, DMD, MS
Major, United States Air Force, DC, General Dentistry, Aviano Air Force Base, Aviano, Italy
Kraig S. Vandewalle, DDS, MS
Colonel, United States Air Force, DC, Director, Dental Research, Advanced Education in General Dentistry Residency Program, Dunn Dental Clinic, Joint Base, San Antonio-Lackland, Texas; Air Force Postgraduate Dental School, Uniformed Services University of the Health Sciences, Bethesda, Maryland
Steven C. Maller, DDS, MS
Colonel (Ret), United States Air Force, DC. Formerly: Director of Periodontics, Advanced Education in General Dentistry Residency Program, Dunn Dental Clinic, Joint Base, San Antonio-Lackland, Texas; Air Force Postgraduate Dental School, Uniformed Services University of the Health Sciences, Bethesda, Maryland. Currently: Private Practice, San Antonio, Texas
Raymond H. Hancock, DDS, MS
Colonel (Ret), United States Air Force, DC, Clinical Instructor, Periodontics, Advanced Education in General Dentistry Residency Program, Dunn Dental Clinic, Joint Base, San Antonio-Lackland, Texas; Air Force Postgraduate Dental School, Uniformed Services University of the Health Sciences, Bethesda, Maryland