Using Fiber-Optic Transillumination as a Diagnostic Aid in Dental Practice
Howard E. Strassler, DMD; and Mark L. Pitel, DMD
Abstract:
Fiber-optic transillumination (FOTI) is a well-accepted and valuable adjunctive diagnostic tool with a wide range of clinical applications. In dentistry, FOTI has been primarily associated with caries diagnosis and has been corroborated through research studies to be a valid indicator of the histological presence or absence of bacterially infected tooth structure. In this review, techniques for using FOTI for tooth evaluation are presented along with examples of how FOTI can be effectively used as a supplemental diagnostic aid.
In this era of enhanced diagnostic digital technologies, clinicians desiring to provide the most up-to-date digital technology when diagnosing and treating their patients must be careful not to overlook opportunities to use well-proven evidence-based technologies. One such example of an adjunctive diagnostic tool that does not require additional digital support is fiber-optic transillumination (FOTI). Applications for fiber-optic transillumination include: its use as an adjunctive diagnostic aid for anterior and posterior interproximal caries and occlusal caries diagnosis; detection of calculus; evaluation of stained margins of composite resins; evaluation of cusp fractures and cracked teeth; as an exploration tool to illuminate endodontic access and root canal orifices within the pulp chamber of teeth during endodontic treatment; as a tool for improved evaluation of soft-tissue lesions; for evaluation of all-ceramic restorations to rule out any fractures before cementation; for clinical evaluation of fracture and craze lines in all-ceramic restorations and natural teeth; and for evaluation of depth of extrinsic staining to determine appropriate treatment recommendations.1
Fiber optics (optical fiber) refers to flexible, thin cylindrical fibers of high-optical-quality glass or plastic. The theory of fiber optics is based on a single optical fiber that consists of glass or plastic material with an outer cladding of a lower index of refraction material. Since the fiber core has a higher refractive index, light rays are reflected back into the core. This phenomenon is based on Snell’s Law and is called Total Internal Reflection (TIR). Individual fibers are grouped together to form a fiber optic bundle.1,2 These fibers can be as small as 0.01 mm in diameter for glass and 0.1 mm for plastic.2 Fiber optics have been used in dentistry for adjunctive illumination of other devices such as handpieces and ultrasonic scalers, as well as attached to magnifying loupes.
Dental and medical transillumination refers to light transmission through tissues of the body. Many remember experiencing transillumination of light as children during Halloween, when shining a flashlight through the mandible and soft tissues, thus creating an eerie red glowing appearance due to the red blood cells’ absorbing the other wavelengths of light. In fact, physicians use transillumination for diagnosis of hand tumors and for evaluation of sinuses and breasts.3-5 In dentistry, fiber-optic transillumination has been primarily associated with caries diagnosis. A bright light can illuminate the translucent tooth structure to reveal changes in tooth color, the presence of cracks and fractures, as well as other defects. Typically, the majority of carious lesions are visually accessible. Caries on occlusal and buccal/lingual surfaces account for almost 90% of caries in children and adolescents.6 Approximately 60% of caries occur in 20% of the population, and fewer than 5% of adults are caries-free.7 Caries has been identified as the single most common chronic disease of childhood. While caries is decreasing on interproximal surfaces, occlusal pit and fissue caries has shown a continued increase, yet the interproximal surfaces of the tooth are the least accessible to diagnose.
Accurate diagnosis of smooth-surface proximal enamel and dentin carious lesions is highly challenging to the clinician. Interproximal caries is typically diagnosed using an intraoral clinical assessment, including visualization of superficial enamel discolorations combined with using an explorer to feel for surface roughness and cavitation combined with the use of bitewing radiographs.8-11 In most clinical cases, the access to evaluate the posterior proximal site visually and tactilely is very limited. Radiographs are an important diagnostic tool for the detection of interproximal caries,12,13 and bitewing radiographs are the most frequently used aid in assessing the potential for caries on the proximal tooth surface. Yet, the detection of interproximal caries using bitewing radiographs has been demonstrated to have an accuracy estimated at 40% to 65%.14-16 Also, there is significant variation among clinicians regarding how often diagnostic radiographs should be taken.17 As health professionals, dentists are concerned about limiting their patients’ ionizing radiation exposure. It is well accepted and proven that ionizing radiation dosages are cumulative in their effects and their risks.18,19
To address the need to decrease patients’ exposure to ionizing radiation, clinicians can safely evaluate difficult-to-access proximal surfaces using FOTI to supplement the clinical examination.20 FOTI is a no-risk, minimally invasive, pain-free procedure that can be used repeatedly during routine dental examinations. Using a narrow beam of bright white light directed across the facial and interproximal surfaces, the dry tooth can be visualized for changes in color, texture, tooth surface appearance, and the presence or absence of shadows within the tooth.17
FOTI has been corroborated through research studies to be a valid indicator of the histological presence or absence of bacterially infected tooth structure, with a specificity and sensitivity equivalent to or better than radiographs.21-24 The sensitivity of a test—ie, the true positive rate—is the percentage of people identified as having the condition. Specificity measures the proportion of negatives, ie, the percentage of individuals who do not have the condition. A diagnostic test would ideally have 100% sensitivity and 100% specificity; it would not predict that anyone from the healthy group was sick. From the evidence, the research strongly suggests that proximal caries diagnosis should be based on a combination of evaluations, not a single method, and that combining radiographs, clinical examination, and FOTI together provides the most accurate assessment.25-28
Techniques for Using FOTI for Tooth Evaluation
Traditionally, the use of the brightest light has been associated with providing the best diagnostic tool to illuminate the oral cavity and teeth. In some cases dentists use curing lights to transilluminate teeth, which recent research has demonstrated to pose a significant risk associated with “blue light hazard” that can cause retinal injury and macular degeneration.29-31 It is recommended that specialized light sources with small apertures of 3 mm or less be used, as these provide a point source that results in a sharper image for improved visualization. These smaller light guides provide white light that can be used as an indirect light for FOTI. Past FOTI devices were large boxes with light sources that required fans for cooling and tethered electrical sources. With the latest generation of light-emitting diodes (LEDs), FOTI devices are small, compact, and powered by batteries. The technique of moving the light angulation to change the irradiance provides a more accurate portrayal of different tooth conditions.
FOTI works due to differences in normal enamel and dentin light transmission compared with caries, calculus, restorative materials, and external tooth discolorations.1 Caries, which appears shadowed within the tooth, has a lower index of light transmission than sound tooth structure. Calculus shows up as a darkened area on the surface of the tooth. Translucent tooth-colored restorative materials can be easily distinguished from normal tooth structure using FOTI.
Evaluating for Anterior Caries
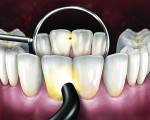
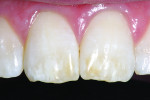
For both maxillary and mandibular anterior teeth, in order to visualize anterior proximal caries the probe should be placed on the labio-cervical region of the tooth, and the surface should be examined from the lingual aspect with a mouth mirror (Figure 1). In some cases, because of the thinness of mandibular incisors, the light guide can be placed on the lingual surface.
Evaluating for Posterior Interproximal Caries
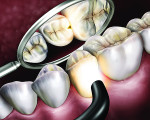
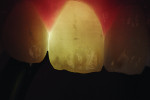
To visualize posterior proximal caries using a conventional light guide, the probe is placed on the cervical area of the tooth, buccally or lingually. Light passes into the cervical tooth structure and then radiates occlusally. Caries can appear as a dark shadow on the occlusal surface (Figure 2).
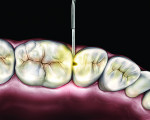
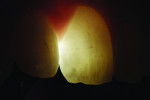
A recent development involves an innovative thin, flexible fiber-optic tip used for evaluating interproximal posterior caries (Microlux Proximal Caries Light Guide, AdDent, Inc., www.addent.com). This 0.75-mm thin light guide is also beneficial for visualizing root canal orifices within pulp chambers. For caries diagnosis, the thin light guide tip is slid into the gingival embrasure below the proximal contact under the marginal ridge. Figure 3 depicts a view from the occlusal. This method often shows caries with a higher definition than a conventional fiber-optic light guide.
Examples of FOTI Usage
FOTI can be used as a supplemental diagnostic aid for anterior and posterior interproximal caries and occlusal caries diagnosis, detection of calculus, evaluation of stained margins of composite resins, and evaluation of cusp fractures and cracked teeth. It can also be used as an exploration tool to illuminate endodontic access and root canal orifices within the pulp chamber of teeth during endodontic treatment, as a tool for improved evaluation of soft-tissue lesions, for evaluation of all-ceramic restorations to rule out any fractures before cementation, for clinical evaluation of fracture and craze lines in all-ceramic restorations and natural teeth, and for evaluation of the depth of extrinsic staining to determine appropriate treatment recommendations.
Case Reports
Supplemental Caries Detection
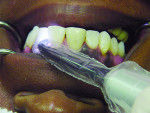
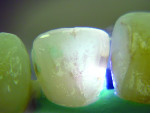
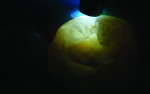
Anterior teeth. For maxillary anterior teeth and mandibular canines, the best view can be achieved by placing the light tip at right angles to the facial surface of the tooth, illuminating the lingual tooth surface (Figure 4). The lingual surface is visualized using a mirror (Figure 5). Placement of the light guide on the lingual surface does not provide the optimal diagnostic image. As seen in Figure 6, initial preparation reveals that caries extension was verified based on its appearance visualized with FOTI.
Caries on the distal surfaces of canines can be more difficult to visualize clinically and radiographically (Figure 7 through Figure 9). Using FOTI combined with clinical and radiographic evidence, an accurate diagnosis can be made (Figure 10). For narrower and thinner mandibular incisors, the light source on the lingual surface can provide an excellent diagnostic view (Figure 11).
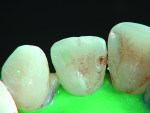
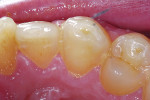
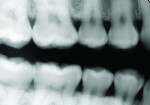
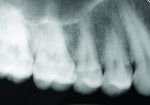
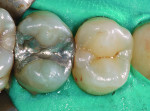
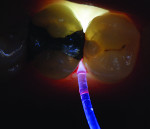
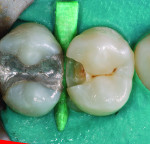
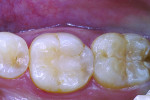
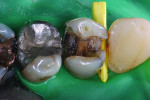
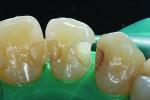
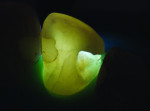
Posterior teeth. Visualization of interproximal caries for posterior teeth requires initial placement of the light guide at right angles on the facial surface just below the contact area. Specialized thin fiber-optic tips that can be threaded between the teeth can offer the best diagnostic view. Interproximal caries for posterior teeth should be diagnosed using a clinical examination (Figure 12), bitewing radiographs, and FOTI (Figure 13). As seen in Figure 14, definitive preparation and caries removal verifies the accuracy of the FOTI portrayal of the caries penetration. Conventional fiber-optic tips are also valuable as an adjunctive aid when diagnosing posterior interproximal caries.
Evaluation of Other Tooth Conditions
Enamel dysplasia. Superficial enamel discoloration can be evaluated using FOTI for depth of the discoloration and degree of opacity of the discoloration. The most commonly seen enamel dysplasia in dental practice is dental fluorosis32 (Figure 15). Using FOTI, the discoloration is revealed for its depth and diffuse opacities on the enamel surface (Figure 16 and Figure 17).
Incomplete tooth fractures. Incomplete tooth fractures typically present as a patient’s self-assessment of pain on biting33 (Figure 18). A comprehensive assessment includes patient questioning and the use of a bite device. A positive response by the patient can be corroborated with visualization of the incomplete fracture of a cusp using FOTI (Figure 19). In some cases, the incomplete fracture might not be a cuspal fracture, but a mesial-distal vertical fracture present on the pulpal wall. The evidence of the fracture can become readily apparent after the restoration is removed and the tooth transilluminated. It is critical to use the fiber-optic tip from a variety of orientations to best visualize incomplete tooth fractures.
Another example is a case of an incomplete fracture noted during preparation, with no symptoms that needed to be evaluated for tooth prognosis over time (Figure 20). FOTI was used to demonstrate to the patient the guarded prognosis for treatment (Figure 21). In this case, the composite restoration was placed and the patient scheduled for a follow-up appointment.
Transillumination of root canal orifices. In some cases that involve preparing an endodontic access or exploring to find the root canal orifices, using a FOTI tip at the cervical of the tooth below the dental dam retainer will illuminate the interior of the tooth to better visualize the root canal (Figure 22).
Existing defective composite resins. During tooth preparations, especially when there are existing defective composite resins, it may be difficult to visualize the complete removal of the defective composite. Using FOTI makes it easier to visualize the difference between tooth structure and composite and to see the borders of the defective restoration being removed (Figure 23 and Figure 24). Also, when composite resins have stained margins, FOTI can demonstrate whether the tooth has only a stained margin or caries penetrating deeper into the tooth.
Conclusion
Conventional clinical examinations and radiographs provide critical information in diagnosing oral conditions. In recent years, a surge in the availability of digital devices for use as supplemental aids for diagnosis of dental pathologies has enabled dentists to add to their diagnostic armamentarium. While excitement is often associated with new technologies, clinicians must remember that there are proven conventional technologies that can also make a difference. Fiber-optic transillumination (FOTI) is a category of supplemental diagnostic tools that do not require additional digital support. By merely shining a bright light through translucent oral tissues using well-accepted techniques, clinicians can expand their ability to achieve an accurate diagnosis. Moreover, FOTI provides an additional tool to be used during treatment. Applications of FOTI include:
- a supplemental diagnostic aid for anterior and posterior interproximal caries and occlusal caries diagnosis
- detection of calculus
- evaluation of stained margins of composite resins and of cusp fractures and cracked teeth
- an exploration tool to illuminate endodontic access and root canal orifices within the pulp chamber of teeth during endodontic treatment
- improved evaluation of soft-tissue lesions
- evaluation of all-ceramic restorations to rule out any fractures before cementation
- clinical evaluation of fracture and craze lines in existing all-ceramic restorations and natural teeth
- evaluation of the depth and quality of extrinsic staining to determine appropriate treatment recommendations.
About the Authors
Howard E. Strassler, DMD
Professor and Director of Operative Dentistry
Department of Endodontics
Prosthodontics, and Operative Dentistry
University of Maryland Dental School
Baltimore, Maryland
Mark L. Pitel, DMD
Associate Clinical Professor of Operative Dentistry
Director of Predoctoral and CDE Esthetic Studies
Columbia University College of Dental Medicine
New York, New York
References
1. Friedman J, Marcus MI. Transillumination of the oral cavity with use of fiber optics. J Am Dent Assoc. 1970;80(4):801-809.
2. DeCusatis C, DeCusatis CJ. Fiber, cables, and connectors. In: DeCusatis C, DeCusatis CJ, eds. Fiber Optic Essentials. San Diego, CA: Elsevier; 2006:1-28.
3. Erne HC, Gardner TR, Strauch RJ. Transillumination of hand tumors: a cadaver study to evaluate accuracy and intraobserver reliability. Hand (N Y). 2011;6(4):390-393.
4. Dixit SS, Kim H, Comstock C, Faris GW. Near infrared transillumination imaging of breast cancer with vasoactive inhalation contrast. Biomed Opt Express. 2010;1(1):295-309.
5. Sharan R, Thankappan K, Iyer S, et al. Intraoperative transillumination to determine the extent of frontal sinus in subcranial approach to anterior skull base. Skull Base. 2011;21(2):71-74.
6. Ripa LW, Leske GS, Sposato A. The surface-specific caries pattern of participants in a school-based fluoride mouthrinsing program with implications for the use of sealants. J Public Health Dent. 1985;45(2):90-94.
7. Diagnosis and Management of Dental Caries Throughout Life. NIH Consensus Statement. Bethesda, MD: National Institutes of Health. 2001;18(1):1-24.
8. Gordan VV, Riley JL 3rd, Carvalho RM, et al. Methods used by Dental Practice-based Research Network (DPBRN) dentists to diagnose dental caries. Oper Dent. 2011;36(1):2-11.
9. Roberson TM. Cariology: the lesion, etiology, prevention and control. In: Roberson TM, Heymann HO, Swift EJ Jr, eds. Sturdevant’s Art and Science of Operative Dentistry. 5th ed. St. Louis, MO: Mosby Elsevier; 2006:67-134.
10. Nielsen LL, Hoernoe M, Wenzel A. Radiographic detection of cavitation in approximal surfaces of primary teeth using a digital storage phosphor system and conventional film, and the relationship between cavitation and radiographic lesion depth: an in vitro study. Int J Paediatr Dent. 1996;6(3):167-172.
11. Davies GM, Worthington HV, Clarkson JE, et al. The use of fibre-optic transillumination in general dental practice. Br Dent J. 2011;191(3):145-147.
12. Kidd EA, Pitts NB. A reappraisal of the value of bitewing radiograph in the diagnosis of posterior approximate caries. Br Dent J. 1990;169(7):195-200.
13. Pitts NB. Advances in radiographic detection methods and caries management rationale. In: Stookey GK, ed. Early Detection of Dental Caries: Proceedings of the First Annual Indiana Conference. Indianapolis, IN: Indiana University School of Dentistry; 1996.
14. Espelid I. Radiographic diagnoses and treatment decisions on approximal caries. Community Dent Oral Epidemol. 1986;14(5):265-270.
15. Espelid I, Tveit AB. Clinical and radiographic assessment of approximal carious lesions. Acta Odontol Scand. 1986;44(1):31-37.
16. Mileman PA, van der Weele LT. Accuracy in radiographic diagnosis: Dutch practitioners and dental caries. J Dent. 1990;18(3):130-136.
17. Dental Treatment. GDS Quarterly Statistics. January-March, 1999. DPB.
18. Brambilla M, De Mauri A, Leva L, et al. Cumulative radiation dose from medical imaging in chronic adult patients. Am J Med. 2013;126(6):480-486.
19. Kleinerman RA. Cancer risks following diagnostic and therapeutic radiation exposure in children. Pediatr Radol. 2006;36(suppl 2):121-125.
20. Pitts NB. Diagnostic tools and measurements—impact on appropriate care. Community Dent Oral Epidemiol. 1997;25(1):24-35.
21. Pine CM. Fibre-optic transillumination (FOTI) in caries diagnosis. In: Stookey GK, ed. Early Detection of Dental Caries: Proceedings of the First Annual Indiana Conference. Indianapolis, IN: Indiana University School of Dentistry; 1996.
22. Peers A, Hill FJ, Mitropoulos CM, Holloway PJ. Validity and reproducibility of clinical examination, fibre-optic transillumination, and bite-wing radiology for the diagnosis of small approximal carious lesion: an in vitro. Caries Res. 1993;27(4):307-311.
23. Reddy VV, Sugandhan S. A comparison of bitewing radiography and fibreoptic illumination as adjuncts to the clinical identification of approximal caries in primary and permanent molars. Indian J Dent Res. 1994;5(2):559-564.
24. Côrtes DF, Ekstrand KR, Elias-Boneta AR, Ellwood RP. An in vitro comparison of the ability of fibre-optic transillumination, visual inspection and radiographs to detect occlusal caries and evaluate lesion depth. Caries Res. 2000;34(6):443-447.
25. Hintze H, Wenzel A, Danielsen B, Nyvad B. Reliability of visual examination, fibre-optic transillumination, and bite-wing radiography, and reproducibility of direct visual examination following tooth separation for the identification of cavitated carious lesions in contacting approximal surfaces. Caries Res. 1998;32(3):204-209.
26. Choksi SK, Brady JM, Dang DH, Rao MS. Detecting approximal dental caries with transillumination: a clinical evaluation. J Am Dent Assoc. 1994;125(8):1098-1102.
27. Mialhe FL, Pereira AC, Pardi V, de Castro Meneghim M. Comparison of three methods for detection of carious lesions in proximal surfaces versus direct visual examination after tooth separation. J Clin Pediatr Dent. 2003;28(1):59-62.
28. Strassler HE, Sensi LG. Technology-enhanced caries detection and diagnosis. Compend Contin Educ Dent. 2008;29(8):464-470.
29. Wielgus AR, Roberts JE. Retinal photodamage by endogenous and xenobiotic agents. Photochem Photobiol. 2012;88(6):1320-1345.
30. Wielgus AR, Collier RJ, Martin E, et al. Blue light induced A2E oxidation in rat eyes—experimental animal model of dry AMD. Photochem Photobiol Sci. 2010;9(11):1505-1512.
31. Shaban H, Richter C. A2E and blue light in the retina: the paradigm of age-related macular degeneration. Biol Chem. 2002;383(3-4):537-545.
32. Strassler HE, Griffin A, Maggio M. Management of fluorosis macro- and microabrasion. Dent Today. 2011;30(10):91-97.
33. Ailor JE Jr. Managing incomplete tooth fractures. J Am Dent Assoc. 2000;
131(8):1168-1174.