Conservative Preparation Guidelines for CAD/CAM Restorations
Abstract:
The advent of computer-aided design/computer-aided manufacturing (CAD/CAM) technology has enabled clinicians to perform conservative dentistry more predictably. Rapid improvements in technology have spawned several computerized devices that can fabricate ceramic restorations within a matter of minutes. One such system, CEREC® CAD/CAM, is designed to be used chairside, eliminating the need for conventional impression taking, temporary restorations, and multiple appointments. Prior to the arrival of CAD/CAM, the most commonly performed indirect restoration was the full-coverage crown with total axial reduction. Using CAD/CAM to scan and design allows dentists to keep preparations within enamel and, as a result, achieve an ideal bonded restoration that is conservative as well as innovative.
The full-coverage crown has long served as the “go-to” preparation design for indirect restorations. The traditional approach to preparing the tooth leads to unnecessary removal of healthy tooth structure, and, the author contends, the process that follows is time-consuming and inconvenient for both patient and the dental team. The recommended reduction is 1.5 mm to 2 mm of occlusal reduction and 1 mm to 1.5 mm of axial reduction, depending on the type of material being used to fabricate the restoration. A polyvinylsiloxane (PVS) impression is then taken and a temporary is fabricated. During the approximately 2- to 3-week time period typically required for the crown to return from the laboratory, it is not uncommon for the patient to return to the dental office with a broken or lost temporary crown, requiring additional chairtime for remaking the temporary restoration.
Once the crown is received from the laboratory, the patient then needs to return to the office for the final delivery of the crown. This appointment requires the patient to be anesthetized again. In addition, the crown is often sent back to the laboratory for re-fabrication due to an open contact or inadequate margin or occlusion.
CAD/CAM Workflow
As an alternative to the often laborious aforementioned approach, the author uses the CEREC Omnicam (CAD portion of CAD/CAM) (Sirona Dental, www.sirona.com) to digitally scan teeth and design restorations that can be milled and delivered the same day. The Omnicam is a color-streaming intraoral scanning camera that requires no powder or opaquing agent. This simplifies the learning curve for the clinician and makes the scanning process convenient and fast, yet retains the high level of precision needed.
After the tooth has been appropriately prepped, and proper tissue management and isolation have been achieved, images are taken with the Omnicam. It requires approximately 3 to 5 minutes to design the restoration with the help of different design tools available with the CEREC 4.0 software on the Omnicam. Once the restoration has been designed, the computer directs a micro milling devise (the CAM portion of the system), which mills the restoration out of a high-quality ceramic block in a matter of minutes. A wide range of porcelain blocks are available to fabricate these restorations.
In the author’s experience, the key to delivering superior restorations with CAD/CAM lies in the preparation of the tooth, which must be ideal to support conservative, adhesive dentistry. It is very important to master the preparation guidelines as outlined below, because when performed properly, they can be used to maximize the longevity of the restoration.
Preparation Guidelines for CEREC CAD/CAM Restorations
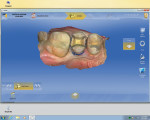
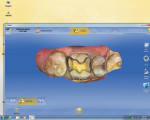
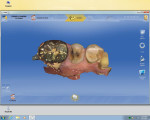
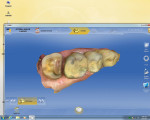
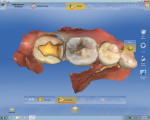
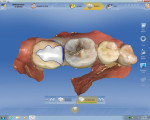
First, a 1.5-mm reduction in the central groove and a 1.5-mm isthmus width are essential. The primary reason for the failure of all-porcelain restorations is inadequate reduction. The manufacturer recommends a 1.5-mm reduction because it provides adequate thickness of porcelain to withstand occlusal forces and avoid fracture of restoration during the milling process. Figure 1 and Figure 2 show inlay preparations on a premolar and molar, respectively.1
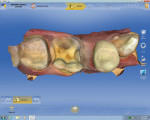
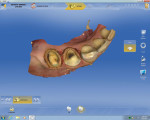
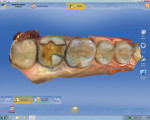
Proximal boxes are prepared identically as those for cast metal inlays. The facial, lingual, and gingival margins of the proximal boxes should be extended to clear at least 0.5 mm to 1 mm, which provides adequate access for imaging as well as finishing and polishing these restorations. This can be seen in the four-surface onlay on a molar (tooth No. 14) in Figure 3, as well as in the premolar and molar shown in Figure 1 and Figure 2, respectively.1
It is very important that there be absolutely no undercuts on these preparations to make them easy to image and to avoid interference with the insertion and removal of the restoration. The gingival to occlusal divergence of the preparation may be increased from 2 to 5 degrees per wall for cast metal restorations and from 6 to 8 degrees for all-ceramic restorations. The divergence can be increased in this way because the tooth-colored restoration will be adhesively bonded at cementation. Over-tapering of walls should be avoided, as that leads to weak porcelain at the cavosurface (Figure 1 and Figure 2).1
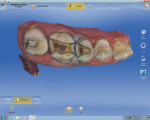
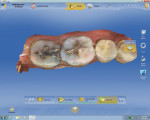
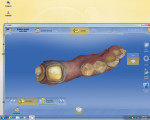
When prepping for inlays and onlays, the exit angles must draw completely with each other and they should exit in graceful curves (Figure 1, Figure 2, and Figure 4). Line and point angles—both internal and external—should be well rounded to avoid stress concentrations in the restoration and tooth, thereby reducing the potential for fractures. This will yield a smooth intaglio of the restoration without any over-milling (Figure 1 through Figure 7).1
The axial walls should be straight without any steps or ledges. It has been the author’s experience that steps on the axial walls lead to steps in the restoration, which results in a weak restoration and premature failure (Figure 1, Figure 2, and Figure 4).
Proximal walls of adjacent teeth should be smooth without undercuts. If there is an old restoration on the adjacent tooth that is over-contoured or rough on the surface, the clinician should smooth out the surface with a fine diamond bur to create a smooth contact. This will allow the scanner to image the margin of the restoration as well as the wall of the adjacent tooth that will help build an ideal contact (Figure 4 and Figure 8 through Figure 10). When prepping onlays that require cuspal reduction, especially centric holding cusps, it may be necessary to provide a “collar” to move the facial or lingual cavosurface margin away from any possible contact with the opposing tooth, either in maximum intercuspation (MIP) or during mandibular movements. Such contacts on margins can lead to premature deterioration of marginal integrity (Figure 3, Figure 5, Figure 6, and Figure 11).1
The author highly recommends that when prepping restorations with complete cuspal reduction and no axial reduction it is important to have a keyway for the restorations to seat during the delivery. This keyway is most commonly achieved in the form of proximal boxes. The keyway or slot becomes necessary for a positive seat as these types of preparation lack retention and easily rotate during cementation (Figure 6 and Figure 7).
In the event that a complete crown with total axial reduction is desired, it is imperative to have 1.5 mm reduction in the central groove, 2 mm reduction at the cusps, and 1 mm reduction on the axial. This amount of occlusal and axial reduction will provide sufficient bulk of material for all-ceramic restorations (Figure 7 and Figure 12).1 Having said that, several manufacturers are coming out with blocks that will push towards lesser reduction due to the improvements in their physical properties.
Before the preparation is ready to be imaged, tissue should be properly managed so it is easy to image all the margins and also have a dry field of operation to avoid any kind of contamination by blood, saliva, or crevicular fluid. Tissue management can be achieved by any one or a combination of the 1- or 2-cord technique (Figure 1, Figure 2, and Figure 4), diode laser and electrosurge (Figure 6 and Figure 7), etc. Isolation devices such as a rubber dam, cotton rolls, or dry angles are useful in achieving a dry field for the final cementation.
Discussion
Conservative preparation design eliminates unnecessary removal of healthy tooth structure, especially enamel, which is the best bonding surface. When proper preparation guidelines and adhesive protocols are met, it is possible to achieve restorations that will stand the test of time. With the ample choices of restorative and bonding materials available today, fit and esthetics that rival laboratory-fabricated restorations can be attained at a fraction of the cost.
CEREC Omnicam can be used to fabricate single-unit restorations such as inlays, onlays, 3/4 crowns, and complete crowns, as well as bridges for posterior teeth. It can also be used to fabricate highly esthetic veneers and complete crowns for anterior teeth. With the advances in the software, it is now possible to make custom zirconia abutments and crowns for implant patients. The use of this technology is not limited to single-unit restorations; it can also be used for full-mouth rehabilitations as well as highly esthetic smile designs.
In the event that a same-day restoration is not desired, CEREC Onmicam enables clinicians to digitally scan preparations and send them to an approved laboratory for fabrication. This eliminates the need for a physical impression, and the turn-around time is much shorter.
Summary
Using CEREC Omnicam allows the modern practitioner to practice minimally invasive, same-day dentistry. This technology has truly brought the entire lab into the dental office and helps serve patients like never before.
ACKNOWLEDGMENT
The author refined the preparation methods described, which are based on those originally featured in Chapter 17 in The Art and Science of Operative Dentistry, 3rd edition, by Clifford M. Sturdevant, et al, as well as the manufacturer.
REFERENCES
1. Heyman HO, Sturdevant JR, Robertson TM, Sockwell CL. Tooth-colored restorations for classes I, II, and IV cavity preparations. In: Sturdevant CM, Robertson TM, Heymann HO, Sturdevant JR, eds. The Art and Science of Operative Dentistry. 3rd ed. Mosby: St. Louis, MO; 1995.
ABOUT THE AUTHOR
Dhaval Patel, DDS
Private Practice, Roseville, California. His dental practice is supported by Pacific Dental Services. Dr. Patel can be reached at pateld@pacden.com.