Composite Resins in 2013: An Update on Their Progress
Gary M. Radz, DDS
Having steadily evolved and improved over the past several decades, composite resins are providing clinicians with an increased array of options for successfully restoring teeth in a minimally invasive manner. Numerous advances compared to early composite resin systems, such as increased shade availability, reduced polymerization shrinkage, and the development of nanoparticles, have enabled composite resins to offer long-term esthetic solutions for patients. This article summarizes the changes that have occurred, discusses popular applications for the use of composite materials, and presents brief case studies demonstrating their capabilities.
In 2000, Fortin and Vargas stated that composite resins might eventually replace amalgam for direct restorations.1 Although dentistry in 2013 is not there yet, the industry is moving closer to that prediction. Each year the use of amalgam continues to steadily decline while the use of composite resins rises.
Since Buonocore2 and Bowen3 published their industry-changing findings more than 50 years ago, composite resins have slowly, gradually become a common and accepted restorative material. The quick acceptance of that research brought about a sudden end to the use of silicate cements as an esthetic restorative material.
Early composite systems were not without their problems. Initially, only self-curing systems were available and in a very limited number of shades. This restricted the ability of the material to be manipulated and also limited the esthetic results. Additionally, early composites demonstrated excessive shrinkage characteristics, leading to sensitivity and recurrent decay. Lastly, these initial composite systems were loaded with large filler particles, which led to excessive wear rates.4
Despite these issues, the demand from clinicians and their patients for composite resins placed constant pressure on researchers and dental material manufacturers to improve them so that a predictable, long-lasting, esthetic restorative material could be used for direct applications. The composite resins that are available today only remotely resemble the early systems. Numerous changes have been made to create what is coming increasingly closer to an ideal direct restorative material.
Areas of Advancement
Esthetics/Shades
Initially, composite resins were available in only four shades.4 Today’s composite systems may have up to 32 shades available for the clinician to use to create a desired effect.5 Presently, the marketplace demonstrates considerable variability in the number of shades offered. Some “universal” and anterior esthetic systems have 20 to 30 different shades available, as well as variable levels of translucency and opacity, giving clinicians a wide artistic palate with which to work in order to create the final restoration. Conversely, some of the bulk-filled posterior systems have only one to four shades available.
Low-Shrinking Composites
All composite resins will shrink. In early systems, this shrinkage was extreme and would lead to marginal leakage, which would, in turn, lead to sensitivity and/or recurrent decay. Today, manufacturers have developed dental composites that demonstrate lower polymerization shrinkage.6 Some products utilize modified formulations of Bis-GMA/TEGDMA (bisphenol A glycidyl methacrylate [Bis-GMA]/triethylene glycol dimethacrylate [TEGDMA]) to decrease shrinkage, while others employ entirely new formulations to lower the amount of shrinkage and/or the shrinkage stress.4
Using any of these various formulation methods, it is commonplace for today’s composite resins to demonstrate polymerization shrinkage numbers < 2.5%, and several products on the market are approaching 1%. The inherent physical properties of composite resin will probably make it impossible to ever reach a 0% shrinkage factor; however, recent independent developments from several different manufacturers show that shrinkage at < 2% is well within reach. Shrinkage at this level, along with proper technique, should dramatically reduce the negative issues associated with polymerization shrinkage.
Filler Size
Early filler particles were 10 µm in size.4 These filler particles were prone to plucking and led to excessive wear of the resin material.
In the 1980s, microfilled composites were introduced to the marketplace.7 Using extremely small filler particles (0.02 µm to 0.04 µm), microfilled composites were very translucent and highly polishable, demonstrated low wear characteristics, and exhibited excellent handling characteristics. However, the small particle size translated to low strength, and these materials were prone to bulk fractures. Today, microfilled composites still exist and are used by clinicians in anterior applications where esthetics are in high demand and the functional stresses are low.
In an effort to combine the best of both worlds—strength and esthetics—hybrid composites were developed. This methodology combined the larger particle size of the early composites, which provided strength, with the smaller particles of the microfilled composites, which assisted with esthetics and wear. The early hybrids were successful in improving strength and, to an extent, wear, but fell short on the esthetic side.
The next development in the search for the ideal material was the creation of microhybrid composites. These composites were still a “hybrid” by definition, yet the largest particle size in the microhybrid systems was now < 1 µm. Practitioners found that it was possible to maintain the strength of the hybrid materials while significantly improving esthetics.5
The most recently introduced generation of composite resins are new nanofilled composites. These systems feature nanomers (5-nm to 75-nm particles) and “nanocluster” agglomerates as fillers. Nanoclusters are agglomerates (0.6 µm to 1.4 µm) of primary zirconia/silica nanoparticles (5 nm to 20 nm) fused together at points of contact, and the resulting porous structure is infiltrated with silane.4
Popular Uses of Composite Resins
For many years the “holy grail” of composite resins was to create a “universal” composite that could be applied to all clinical situations. The microhybrid and nanofilled composites appeared to have come closest to earning the “universal” label of any of today’s composites. However, in recent years there has been a gradual shift away from this “universal” panacea that the industry has worked so hard to find.
Bulk-Fill Systems
The prime example of this shift is the extreme popularity of posterior “bulk-fill” composite systems. Current bulk-fill systems are designed to have a deep depth of cure—4 mm is typically the recommended depth of cure value associated with these materials. They also have been developed to feature a low percentage of polymerization shrinkage (or shrinkage stress in the case of one particular product). However, a sacrifice has been in the esthetic capabilities of these materials. Typically, only a minimum selection of shades is available, as esthetics seem to be only a secondary goal for these bulk-filled materials. Despite this, based on sales related to these materials, North American dentists have voted with their pocketbooks and have stated to the industry that bulk-filled composite resins are in high demand.
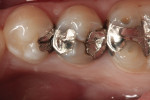
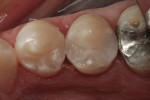
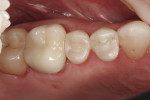
In the following case study (Figure 1 and Figure 2), the ability of one of the more popular bulk-fill composite resins is demonstrated. Figure 1 shows the preoperative view of failing amalgam restorations on teeth Nos. 20 and 21. Using a bulk-fill system (SonicFill™, Kerr Corporation, www.kerrdental.com) it is possible to create the final results demonstrated in Figure 2, which is an immediate postoperative photograph showing that clinically acceptable anatomic form, contour, and contact was achieved. Figure 2 also demonstrates the lack of ability of bulk-fill materials to create a highly esthetic result. In order to be able to have at least a 4-mm depth of cure, these materials must be more translucent in nature; Figure 2 depicts that inherent translucency. However, it is important to note that many, if not most, patients would view this as a dramatic positive esthetic improvement.
Another important factor contributing to the clinical success of bulk-filled posterior composites is the recent development of dramatically improved matrix systems. The introduction of such systems as the Composi-Tight 3D™ System (Garrison Dental Solutions, www.garrisondental.com) and the Triodent V3 System (Ultradent Products, Inc., www.ultradent.com) has enabled clinicians to use bulk-fill systems and create excellent proximal contacts.
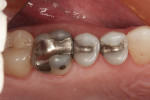
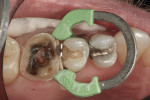
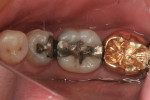
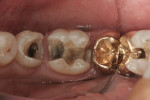
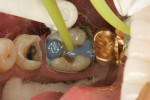
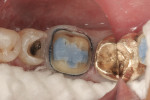
A case in point is depicted in Figure 3 through Figure 5. Figure 3 shows a preoperative photograph of a patient who required the replacement of failing amalgams on teeth Nos. 4 and 5. Using the new Triodent V3 sectional matrix system (Figure 4) it was possible to create predictable anatomy, contacts, and contour with Class II restorations. The postoperative view is shown in Figure 5. Of interest in this case is that the author/dentist completed the restoration on tooth No. 4, and the author’s expanded-duty dental assistant completed the restoration on tooth No. 5. This is important to note because the use of these new matrix systems along with current bulk-fill materials demonstrates that it is possible for a properly trained dental professional to create clinically acceptable Class II restorations. The other item of interest in this case is that the restoration on tooth No. 4 was completed with one bulk-fill material (Venus® Bulk Fill, Heraeus Kulzer, www.heraeus-dental-us.com) while the other on tooth No. 5 was completed with a different bulk-fill material (SureFil® SDR™, DENTSPLY Caulk, www.caulk.com), with both showing excellent clinical results.
Flowable Materials
Another key example of the industry moving away from the concept of a “universal” composite material is the popularity and evolution of flowable composite restorations. Since their introduction almost 20 years ago, flowable composites have been widely accepted and used by clinicians. Over the years, these materials have been utilized in a wide variety of clinical applications, ranging from Class I, III, and V restorations, to sealants and preventive resin restorations (PRRs), to base/liners, to repair of temporary restorations.
In recent years, manufacturers have begun to provide a wider array of shades as well as opacities and translucencies within the material. Most recently, different viscosities have been offered as well. Thus, dentists can now select the flow characteristics of the material to match the clinical need.
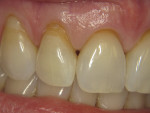
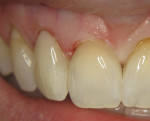
A case demonstrating the use of flowable composite is shown in Figure 6 and Figure 7. Areas of abfraction were present on teeth Nos. 7 and 8 (Figure 6). Using a thin layer of shade A2O of a “no-flow” flowable composite (Beautifil® Flow Plus F00, Shofu, www.shofu.com), the darker cervical shades were opaqued out, then a layer of A2 “low-flow” composite (Beautifil® Flow Plus F03, Shofu) was used for the superficial layer to create the optimum esthetic result (Figure 7).
Core Build-Up Materials
Composite resins have now become the norm for use as core build-up materials. The ability to be used quickly combined with having dual-cure capabilities has allowed clinicians to efficiently provide excellent build-ups.
As this material has been developed, manufacturers have been able to shift the focus away from esthetic requirements and now concentrate on ease-of-use and strength characteristics. A majority of today’s core build-up materials are offered in shades of “natural” (typically A2), opaque or white, and blue. These materials are currently available in dual-cure form with an automix type of delivery. Because these materials are being used as a dentin replacement in teeth being prepared for crowns, the primary concerns in the material development have been related to creating flexural strength and compressive strength in the composites that simulates dentin.
In a case (Figure 8 through Figure 11) showing composite resin used as a build-up material, Figure 8 shows tooth No. 19 requiring a full-coverage restoration. The old amalgam and decay were removed (Figure 9). Using a disposable Tofflemire-type matrix (Omni-Matrix™, Ultradent Products, Inc.), the prepared tooth was isolated, then etched using a total-etch bonding system (OptiBond FL®, Kerr Corporation), and the “flowable” dual-cure composite build-up material (LuxaCore® Z, DMG America, www.dmg-america.com) was injected into the preparation (Figure 10). A 20-second light-cure (Demi Plus, Kerr Corporation) was applied with the matrix on, then repeated with the matrix removed. The material was thus cured so that the final crown preparation could be started immediately. Figure 11 shows the final crown preparation.
Conclusion
Composite resins continue to evolve and improve, providing clinicians with more and better options for successfully restoring teeth in a minimally invasive manner and providing long-term esthetic solutions for patients. The search for “all-in-one universal” composite resins will continue; however, currently, the market is seeing clinicians looking for specific composites that provide the best combination of physical and esthetic characteristics for each different restorative situation. Therefore, in the near future dentistry will continue to see subspecialization of composite resins as manufacturers strive to provide the best material for the varied restorative needs that patients present.
Disclosure
Dr. Radz developed LuxaCore®, LuxaCore® Dual, and LuxaCore® Z with DMG America and has an ongoing financial interest in this product.
References
1. Fortin D, Vargas MA. The spectrum of composites: new techniques and materials. J Am Dent Assoc. 2000;131(suppl):26S-30S.
2. Buonocore MG. A simple method of increasing the adhesion of acrylic filling materials to enamel surfaces. J Dent Res. 1955;34(6):849-853.
3. Bowen RL. Development of a silica-resin direct filling material. Report 6333. Washington, DC: National Bureau of Standards; 1958.
4. Hervás-García AH, Martínez-Lorenzo MA, Cabanes-Vila JC, et al. Composite resins: A review of materials and clinical indications. Med Oral Patol Oral Cir Bucal. 2006;11(2):E215-E220.
5. Sensi LG, Strassler HE, Webly W. Direct composite resins. Inside Dentistry. 2007;3(7):76-79.
6. Duarte S Jr, Botta AC, Phark JH, Sadan A. Selected mechanical and physical properties and clinical application of a new low-shrinkage composite restoration. Quintessence Int. 2009;40(8):631-638.
7. Mitra SB, Wu D, Holmes BN. An application of nanotechnology in advanced dental materials. J Am Dent Assoc. 2003:134(10):1382-1390.
About the Author
Gary M. Radz, DDS
Associate Clinical Professor
University of Colorado School of Dentistry
Denver, Colorado
Private Practice
Denver, Colorado