Relevance of the Water Flosser: 50 Years of Data
Abstract
A review of the literature answers many questions related to the use of water flossers, the first of which was introduced in 1962. Numerous studies suggest that water flossers remove biofilm from tooth surfaces and bacteria from periodontal pockets better than string flossing and manual toothbrushing—together or alone. Clinicians should review these findings and consider recommending water flossers for appropriate patients to improve their oral health. As different irrigation or water-flossing devices now on the market offer different features, designs, and combinations of pulsation and pressure, clinicians must consider the needs of individual patients and supporting research in selecting a model that the patient will like and use, and that will provide improved oral health.
The first oral irrigator was introduced to the dental profession in 1962. It was developed by a Colorado dentist who, in an effort to improve his patients’ oral hygiene, enlisted the help of a patient, a hydraulic engineer. The oral irrigator—also called a dental water jet—is known today as a water flosser. While it is one of the most studied self-care devices on the market, questions remain regarding its efficacy, safety, and outcomes. This literature review will provide answers to many of these questions based on clinical research findings.
Does a Water Flosser Remove Plaque (Biofilm)?
A 1971 study by Hoover and Robinson1 reported a significant reduction in the accumulation of plaque and formation of calculus in the group that used the oral irrigator. Likewise, Lobene2 reported a 50% reduction in calculus in the water flosser group, and Phelps-Sandall3 reported a significant reduction in plaque for individuals in intermaxillary fixation. Reductions in plaque have been demonstrated in studies with patients who had gingivitis,4 periodontitis,5 orthodontic appliances,6 and diabetes.7
In 2009, Costerton and his team evaluated the removal of biofilm from the tooth surface using a water flosser.8 In this ex-vivo study, periodontally involved teeth were extracted and new biofilm was grown over the existing deposits. The teeth were then treated with a water flosser for 3 seconds on medium pressure. The results were viewed under scanning electron microscopy (SEM) and showed the removal of 99.9% of the biofilm from the treated area.
A recent study measured the plaque removal of a water flosser after a single use and then evaluated the results after 4 weeks.4 When used with a manual toothbrush, the water flosser removed 75% of whole-mouth plaque after a one-time use. When isolating specific areas, the results were: 84% for facial surfaces, 66% for lingual surfaces, 59% for marginal area, and 92% for approximal area. Four-week results showed 51% whole-mouth reduction in plaque, with specific areas showing 53% for facial, 49% for lingual, 25% for marginal, and 77% for approximal.
Does a Water Flosser Push Bacteria into the Pocket?
Research shows that the water flosser does not push bacteria into the periodontal pocket; in fact, the reverse is true. The water flosser removes bacteria from the pocket. Several studies have shown the reduction of bacteria from the periodontal pocket following irrigation with a water flosser. An early study to measure the ability of a water flosser to reduce bacteria was conducted on subjects with fixed orthodontic appliances. At the end of the 63-day study, results from the group of patients who used a manual toothbrush and water flosser device showed that this method was 80% more effective than toothbrushing and rinsing in reducing total aerobic flora and 60% more effective in reducing the lactobacillus count.9
Cobb and colleagues10 examined 32 teeth with 6-mm pockets that were scheduled for extraction. Half the teeth were treated with water irrigation using a pulsating water flosser device set on medium pressure, and the other half (control group) received no treatment. The experimental teeth were treated for 8 seconds prior to extraction. All teeth were extracted, keeping the epithelial tissue intact. SEM and transmission electron microscopy (TEM) were used to evaluate epithelial cavitation or ulceration. The investigators found that the water flosser group had reduced the numbers of microorganisms by up to 6 mm compared to the untreated areas, which had thick mattes of microbes. Importantly, they reported no differences in the epithelial lining of the pocket or evidence of penetration into the tissue.
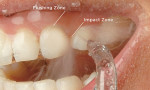
The removal of bacteria is accomplished by the pulsating action of the device. This results in an impact and flushing zone, which produces a compression and decompression phase (Figure 1) and allows for clearing of the bacteria and debris from the pocket. Drisko et al11 demonstrated a reduction in the number of spirochetes from pretreatment levels in 3-mm and 6-mm pockets. Chaves and colleagues12 compared water irrigation, chlorhexidine (CHX) irrigation, CHX rinsing, and brushing alone, and found only the irrigation groups showed a reduction in subgingival bacteria.
Is a Water Flosser as Effective as String Flossing?
To date, only one device, the Waterpik® Water Flosser (Water Pik, Inc., www.waterpik.com), has been compared to dental floss in three different studies.13-15 The first study, published in 2005, compared a water flosser plus either a power toothbrush or a manual toothbrush to a manual toothbrush and string floss.13 The 4-week study showed that regardless of the toothbrush used, the water flosser was significantly better at reducing bleeding and gingivitis than a manual toothbrush and string floss.
In 2008, a study was conducted with adolescents in fixed orthodontic appliances.14 In this study, there were three groups: Group 1 used a water flosser plus a manual toothbrush; Group 2 used string floss with a floss threader plus a manual toothbrush; and Group 3 used only a manual toothbrush (control). The water flosser group was shown to be more effective than the methods used by the other groups, with a 26% greater reduction in bleeding compared to string floss and 53% greater reduction in bleeding compared to toothbrushing alone. The differences for plaque removal were also significant, with the water flosser group showing three times greater reduction than the string floss group and five times greater reduction than the group that used brushing alone.
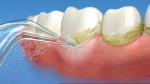
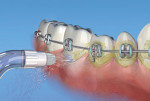
The most recent study was published in 2011.15 Over a 4-week period, subjects used either a water flosser with a traditional jet tip (Figure 2), a water flosser plus a jet tip with three tufts of bristles (Figure 3), or string floss. All subjects brushed using a manual toothbrush twice a day. In both water flosser groups, bleeding was significantly reduced compared with the string floss group. At 2 weeks, the traditional tip was shown to be twice as effective as string floss. At the end of the study, the differences were even greater.
How Can a Water Flosser Perform Better Than String Floss?
The recommendation of dental floss may be more academic than research-based. This was brought to light when a systematic review reported on the results of comparing brushing alone to brushing and flossing. A meta-analysis was performed for the plaque and gingival indices and showed no differences between the groups.16 The authors concluded that the regular recommendation of flossing is not supported by research. Add this to poor compliance,17,18 patient preference for alternatives,19 and poor technique,20 and the need for alternatives is evident. Regarding the question of whether string floss prevents interdental caries, this was addressed by Hujoel et al,21 who found that string flossing was only effective in reducing interproximal caries risk when it was performed by dental professionals on children with a low exposure to fluoride. Self-flossing by adolescents failed to show a benefit, and there were no studies found either for adults or under unsupervised conditions.
How Does a Water Flosser Work?
There are two basic types of irrigation or water-flossing devices. The first is a mechanized device powered by an electrical outlet or batteries. It typically delivers a pulsating stream of water, although not all mechanized units pulsate. Its pressure can be changed, and the pulsations are controlled by the motor. The other is a non-mechanized device that is attached to a water source such as a faucet or shower and delivers a constant stream of water. Devices on the market have different features, designs, and, most importantly, different combinations of pulsation and pressure.
Early studies evaluated the safety and mechanism of action—specifically the combination of pulsation and pressure. It was reported that the combination of 1,200 to 1,400 pulsations per minute is a key component to effectiveness, as this produces a compression and decompression phase.22,23 This hydrokinetic activity creates an impact and flushing zone (Figure 1) that allows for debris and bacteria to be expelled from the sulcus or pocket and is reported to be three times more effective than a continuous-stream device.24 Likewise, a medium-to-high pressure setting—in the range of 50 to 90 pounds per square inch (psi)—was shown to be safe and more effective than lower settings.22-24
Who Should Use a Water Flosser?
Recommendation of self-care devices by dental professionals is based on individual needs, values, preferences, and desired outcomes. Studies have shown that a water flosser can benefit many patient types and oral conditions.
Orthodontics
Orthodontic appliances present oral hygiene challenges regardless of age. A study of 105 adolescents between the ages of 11 and 17 who used a water flosser with an orthodontic tip (Figure 4) showed significant reductions in plaque and bleeding over 4 weeks.6 These results are similar to a previous study that paired a water flosser with either a manual or power toothbrush and compared it to toothbrushing alone in adult orthodontic patients. Regardless of the toothbrush used, the water flosser groups showed significantly greater reduction in bleeding and inflammation compared to subjects who only brushed.25
Periodontal Maintenance
Patients undergoing periodontal maintenance therapy have an increased risk of future loss of attachment, requiring excellent oral hygiene. Patients may have to clean the concavity of the proximal surfaces of the teeth and may be left with 4-mm to 6-mm pockets to maintain. Interdental devices such as floss, wood sticks, and interdental brushes cannot clean into these pockets and may not reach the concavity or furcation.
Several studies have evaluated the subgingival penetration of an oral irrigator. Eakle et al26 tested a standard or classic jet tip placed at 90-degree and 45-degree angles to the long axis of the tooth at the gingival margin (Figure 2). With both angles, depth of penetration varied with pocket depth, with an average of 50%. When placing the tip at a 90-degree angle, a mean percentage of 71% for shallow pockets (0 mm to 3 mm), 44% for moderate pockets (4 mm to 7 mm), and 67% for deep pockets (> 7 mm) was obtained. Placing the tip at a 45-degree angle did not increase penetration, and in some cases penetration was less than when using a 90-degree angle. Notably, 75% or more penetration was seen in 60% of pockets > 7 mm. Larner et al27 reported 42% penetration in 4-mm to 6-mm pockets and 39% for 7-mm to 10-mm pockets. A specialized subgingivally placed tip with reduced flow and pressure (Figure 5) was reported to reach 90% of a 6-mm pocket and 67% in pockets ≥ 7 mm.28
Implants
Implants require daily care similar to natural teeth. A water flosser was tested on implants by comparing rinsing with 0.12% CHX to irrigating using a specialized subgingival tip with 0.06% CHX. The researchers found that using a dilute of CHX with a water flosser was more effective than rinsing with CHX—29% versus 9% for plaque, and 45% versus 10% for gingivitis. The difference in bleeding between groups was 62% for irrigation and 33% for rinsing, but this did not reach significance.29
Diabetic Patients
People living with diabetes have an increased risk for periodontal disease that can present earlier and be more severe. Finding ways to keep the inflammation in check is important and may require a more focused or rigorous homecare program. In a 3-month clinical trial, the water flosser was shown to be beneficial to this population. Fifty-two type 1 and type 2 diabetics were randomly assigned to one of two groups. Group 1 used a water flosser plus subgingival tip twice a day with manual brushing. Those in the control group continued with their current oral hygiene routine. At the end of 3 months, the irrigation group had significantly better improvements in gingivitis, plaque, and bleeding on probing compared to controls.30
Multiple studies show a benefit for patients with varying degrees of gingivitis.2,4,6,13-15 Others who may benefit are those with an increased risk of infection or inflammation, and even those who have relatively good homecare.12 It is important to monitor risk, as situations and medical histories may change.
Conclusion
The research supports the recommendation and use of a water flosser for patients who present with different needs and concerns. There are multiple studies to help practitioners make informed decisions, and they should discuss these with their patients to help them improve their oral health. Clinicians should remind patients that it is never too early or too late to begin a good oral hygiene regimen. Rather than wait for a problem to arise, practitioners should prescribe devices and methods that their patients will like and use. It is especially helpful to instruct patients when they are young.
When evaluating an oral irrigator, dental water jet, or water flosser, clinicians should be aware that research on one device is not transferable to other devices. Each product should be reviewed based on the body of evidence specific to that particular product.
References
1. Hoover DR, Robinson HB. The comparative effectiveness of a pulsating oral irrigator as an adjunct in maintaining oral health. J Periodontol. 1971;42(1):37-39.
2. Lobene RR. The effect of a pulsed water pressure device on oral health. J Periodontol. 1969;40(11):667-670.
3. Phelps-Sandall BA, Oxford SJ. Effectiveness of oral hygiene techniques on plaque and gingivitis in patients placed in intermaxillary fixation. Oral Surg Oral Med Oral Pathol. 1983;56(5):487-490.
4. Sharma NC, Lyle DM, Qaqish JG, Schuller R. Comparison of two interdental cleaning devices on plaque removal. J Clin Dent. 2012;23(1):17-21.
5. Cutler CW, Stanford TW, Abraham C, et al. Clinical benefits of oral irrigation for periodontitis are related to reduction of pro-inflammatory cytokine levels and plaque. J Clin Periodontol. 2000;27(2):134-143.
6. Sharma NC, Lyle DM, Qaqish JG, et al. Effect of a dental water jet with orthodontic tip on plaque and bleeding in adolescent patients with fixed orthodontic appliances. Am J Ortho Dentofacial Orthop. 2008;133(4):565-571.
7. Al-Mubarak S, Ciancio S, Aljada A, et al. Comparative evaluation of adjunctive oral irrigation in diabetics. J Clin Periodontol. 2002;29(4):295-300.
8. Gorur A, Lyle DM, Schaudinn C, Costerton JW. Biofilm removal with a dental water jet. Compend Contin Educ Dent. 2009;30 Spec No 1:1-6.
9. Hurst JE, Madonia JV. The effect of an oral irrigating device on the oral hygiene of orthodontic patients. J Am Dent Assoc. 1970;81(3):678-682.
10. Cobb CM, Rodgers RL, Killoy WJ. Ultrastructural examination of human periodontal pockets following the use of an oral irrigation device in vivo. J Periodontol. 1988;59(3):155-163.
11. Drisko CL, White CL, Killoy WJ, Mayberry WE. Comparison of dark-field microscopy and a flagella stain for monitoring the effect of a Water Pik on bacterial motility. J Periodontol. 1987;58(6):381-386.
12. Chaves ES, Kornman KS, Manwell MA, et al. Mechanism of irrigation effects on gingivitis. J Periodontol. 1994;65(11):1016-1021.
13. Barnes CM, Russell CM, Reinhardt RA, et al. Comparison of irrigation to floss as an adjunct to tooth brushing: effect on bleeding, gingivitis, and supragingival plaque. J Clin Dent. 2005;16(3):71-77.
14. Sharma NC, Lyle DM, Qaqish JG, et al. Effect of a dental water jet with orthodontic tip on plaque and bleeding in adolescent patients with fixed orthodontic appliances. Am J Orthod Dentofacial Orthop. 2008;133(4):565-571.
15. Rosema NA, Hennequin-Hoenderdos NL, Berchier CE, et al. The effect of different interdental cleaning devices on gingival bleeding. J Int Acad Periodontol. 2011;13(1):2-10.
16. Berchier CE, Slot DE, Haps S, van der Weijden GA. The efficacy of dental floss in addition to a toothbrush on plaque and parameters of gingival inflammation: a systematic review. Int J Dent Hyg. 2008;6(4):265-279.
17. Claydon NC. Current concepts in toothbrushing and interdental cleaning. Periodontol 2000. 2008;48:10-22.
18. Kleber CJ, Putt MS. Formation of flossing habit using a floss-holding device. J Dent Hyg. 1990;64(3):140-143.
19. Christou V, Timmerman MF, van der Velden U, van der Weijden FA. Comparison of different approaches of interdental oral hygiene: interdental brushes versus dental floss. J Periodontol. 1998;69(7):759-764.
20. Lang WP, Farghaly MM, Ronis DL. The relation of preventive dental behaviors to periodontal health status. J Clin Periodontol. 1994;21(3):194-198.
21. Hujoel PP, Cunha-Cruz J, Banting DW, Loesche WJ. Dental flossing and interproximal caries: a systematic review. J Dent Res. 2006;85(4):298-305.
22. Bashkar S, Cutright DE, Gross A, et al. Water jet devices in dental practice. J Periodontol. 1971;42(10):658-664.
23. Selting WJ, Bhaskar SN, Mueller RP. Water jet direction and periodontal pocket debridement. J Periodontol. 1972;43(9):569-572.
24. Bhaskar SN, Cutright DE, Frisch J. Effect of high pressure water jet on oral mucosa of varied density. J Periodontol. 1969;40(10):593-598.
25. Burch JG, Lanese R, Ngan P. A two-month study of the effects of oral irrigation and automatic toothbrush use in an adult orthodontic population with fixed appliances. Am J Orthod Dentofacial Orthop. 1994;106(2):121-126.
26. Eakle WS, Ford C, Boyd RL. Depth of penetration in periodontal pockets with oral irrigation. J Clin Periodontol. 1986;13(1):39-44.
27. Larner JR, Greenstein G. Effect of calculus and irrigation tip design on depth of subgingival irrigation. Int J Periodontics Restorative Dent. 1993;13(3):289-297.
28. Braun RD, Ciancio SG. Subgingival delivery by an oral irrigation device. J Periodontol. 1992;63(5):469-472.
29. Felo A, Shibly O, Ciancio SG, et al. Effects of subgingival chlorhexidine irrigation on peri-implant maintenance. Am J Dent. 1997;10(2):107-110.
30. Al-Mubarak S, Ciancio S, Aljada A, et al. Comparative evaluation of adjunctive oral irrigation in diabetics. J Clin Periodontol. 2002;29(4):295-300.
About the Author
Deborah M. Lyle, RDH, BS, MS
Director of Professional and Clinical Affairs
Water Pik, Inc.
Fort Collins, Colorado