Composite Resin: A Versatile, Multi-Purpose Restorative Material
Abstract
Introduced more than some 50 years ago, composite resin technology has simplified the manner in which clinicians practice restorative dentistry, offering greater predictability and improved physical properties. Decades of material science and laboratory development along with clinical trials in human subjects have culminated in composite resin being validated as a reliable, multifunctional restorative material. With a wide range of composite resins available today, clinicians can benefit from knowing the infrastructure of a given material in order to determine which type will work best in a particular clinical situation.
In 1871, Thomas Fletcher introduced a new plastic filling called silicate cement. Its use in dentistry continued into the early 1960s. Although the esthetics were not ideal, it was the material of choice until the development of composite resins.
Composite resin technology was first introduced in 1958, with the development of a high-molecular-weight monomer called bisphenol A-glycidylmethacrylate, or Bis-GMA.1 Along with the development of acid etching in 1955, these two discoveries were the impetus for composite resin techniques used today.2
The first composite resins consisted of a base and catalyst and were only chemical-cured. This made procedures somewhat difficult, yet they were easier than with the silicate cements, and the esthetics were better. With the introduction of light-cured composite resins in the 1970s3 dentistry became more predictable, providing longer working times and better physical properties. These composite resins were more color-stable and had smaller particle sizes than earlier self-cured resins.4
In the late 1970s, microfill resins were introduced with a submicron average particle size, which resulted in high polishability and wear.5 The following decade brought reductions in particle size and increased filler loading, which significantly improved light-cured composite resins for universal use in the anterior and posterior regions.5
Today, after 50 years of material science and laboratory development as well as clinical trials in human subjects, composite resins have been revalidated as an all-purpose restorative material.6,7 There are many different composite resin systems available today. In order to determine which material will work best in a given clinical situation, clinicians must know the infrastructure of composite resins, which is comprised of three phases: the organic phase (matrix), the dispersed phase (filler), and the interfacial phase (coupling agent).3 In essence, composite resins consist of a continuous polymeric or resin matrix into which an inorganic filler is dispersed.8
The addition of fillers in dental composite resins significantly enhances their physical properties by increasing the strength and reinforcement of the matrix9 while reducing the linear coefficient of thermal expansion. There are many fillers for composite resins. These materials can include ground quartz, alumina, zinc, and zirconium, just to name a few. The fillers can vary in size depending on the manufacturing process.
In order for a strong bond to occur between the matrix and the filler, a silane coupling agent is used.10 Altering the filler component remains the most significant development in the evolution of composite resins.11
Classifications of Composite Resins
Today, many manufacturers are working to increase the amount of fillers in their resins to improve such mechanical and physical properties as compression strength, flexural strength, elastic modulus, coefficient of thermal expansion, water sorption, and wear resistance. Several classification systems have been developed based on particle size, distribution, and quantity incorporated.12 Classifications are more commonly referred to as hybrid, microhybrid, microfill, and the newer nanofill. The descriptions of these classifications can vary from system to system.
The hybrid and microhybrid materials generally have a filler content of approximately 75% by weight. Filler particles can range in size from 1 µm to 3 µm and include silica particles, which generally have a size of 0.04 µm. Hybrid materials exhibit superior tensile strength, reduced polymerization shrinkage, low coefficient of thermal expansion, improved abrasion resistance, and better fracture resistance.13 The downside of hybrid materials is their poor polishability and need for maintenance of polish over time.
Microfills consist of submicroscopic silica particles that are approximately 0.04 µm in size. Due to the difficulty in wetting these smaller particles, the filler concentration is usually 35% by weight. The smaller particle size enables excellent polishability and the ability to hold a polish over time. These types of materials are significantly weaker than the hybrids and have a higher water sorption, a lack of radiopacity, and decreased fracture toughness. These materials are best used in conjunction with a hybrid material on the lingual surface for strength and in low-stress areas. They are well suited for Class 3 and Class 5 restorations as well as for direct veneers.
To try and achieve both strength and polishability in one type of composite, manufacturers have introduced smaller particle hybrid composite resins with average particle sizes of approximately 0.02 µm to 1 µm.9 This allows the clinician to implement a single restorative material with all the improved mechanical and physical properties of previous resins. The major drawback of these types of composites is maintenance of polish. The polish is satisfactory initially but tends to lose its luster over time.
Nanocomposites
Nanotechnology, or nanoscience, refers to the research and development of an applied science at the atomic, molecular, or macromolecular levels, which is also known as molecular engineering.14 The prefix “nano” is defined as a unit of measurement in which the characteristic dimension is one-billionth of a unit.15
While many companies use the term “nano” to describe their composite systems, few are actually true nanocomposites. The nanocomposite is composed of two types of nanofiller components: nanomeric particles and nanoclusters.16 The nanomeric particles are monodispersed discrete nonaggragated and nonagglomerated nanosized silica particles, 20 nm and 75 nm in diameter. There are two types of nanoclusters. The first consists of spheroidal agglomerates formed by lightly sintering discrete zirconia and silica particles with a primary size from 2 nm to 20 nm. The second type of nanocluster is synthesized from 75 nm discrete primary particles of silica and has broad secondary particle distribution with an average particle size of 0.6 µm.17 This type of composite was developed for both anterior and posterior use.
Benefits of Composite Resins
Composite resins in everyday practice offer outstanding benefits. They enable clinicians to follow a predictable, conservative, and reliable chairside protocol for enhancing patient smiles and restoring worn and decayed tooth structure. Combined with the best adhesive protocols, these procedures can be used successfully for beautiful results.
Composite resin is one of the most versatile materials in dentistry, and when utilized properly with meticulous care it can perform comparably to porcelain restorations. Proper usage often requires additional training to achieve a master’s level of skill. When used in appropriate situations, these materials should last for many years with long-lasting strength and maintenance of polish.
The ability to be minimally invasive and conserve tooth structure is another significant benefit. Composites are used on a daily basis to restore caries, close spaces, lengthen teeth, cover dark or discolored teeth, and fix fractured teeth. Which type of material to use in a given clinical situation, as previously discussed, is open for debate.
Often times hybrids and microfills are used in combination to achieve a restorative result that offers optimal physical and mechanical properties. The hybrid material provides strength and opacity, and the microfill delivers the definitive luster and durability of the polish. This incremental layering technique with composite resin results in an optimum depth of cure while reducing the effects of shrinkage and stress forces during polymerization.18 In addition, the polychromatic effect can be observed when different restorative components of varying refractive indexes, shades, and opacities are stratified.19 By utilizing an anatomic stratification with successive layers of dentin, enamel, and incisal composite, a more realistic color can be achieved, as can surface and optical characteristics that mimic nature.20
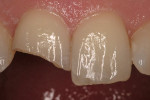
In Figure 1, a clinical situation of a fractured tooth is depicted in which the patient presented to the clinician’s office in an emergency. Figure 2 shows the tooth restored on the same day immediately following a multiple layering technique of composite resins. A dentin-like composite material was used to replace the dentin and produce the opacity to block any shine-through, and an enamel-like composite material was used to provide translucency.
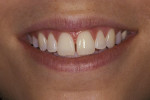
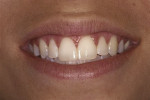
Another clinical situation that commonly arises in dental practices and that is an ideal situation for the use of composite resins is one where patients present with diastemata. The diastema could be due to congenitally small teeth, or it may be a situation where there is simply too much space between teeth. The use of composite resins in this type of instance is minimally invasive and typically is reversible. Usually, no tooth structure needs to be removed, and the procedure is done in one appointment. Orthodontists rely on general dentists to be able to close the unwanted spaces or change the shape of a peg lateral. If the space is small, the material for this type of clinical situation can be either a microfill or nano material, both of which handle well and can provide an excellent final result. Figure 3 shows the smile of a patient who was unhappy with the space between her central incisors. In one appointment the space was closed with composite resin and no preparation of tooth structure was needed (Figure 4).
When a patient presents with fractured porcelain off of a long-span bridge, composite resin can be used to repair the fracture. This type of procedure is not always predictable, but when done correctly and with proper control of occlusion, a successful outcome can be achieved. Numerous composite materials are needed when undertaking a repair with metal exposed. The use of opaquers, tints, hybrids, or nanofills along with a microfill for the final layer can provide a beautiful result by blocking out the underlying metal substructure.
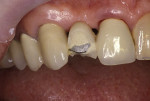
Figure 5 shows a fractured lateral pontic off of a bridge. The patient opted not to expend the finances for a new bridge, thus the bridge was repaired using composite materials in one appointment with an excellent result (Figure 6).
These are just a few examples of the multiple uses of composite resin.
Conclusion
Composite resins offer a conservative and cost-effective solution for many clinical situations. Manufacturers are continually striving to improve the physical properties and ease of use of these materials. It is up to the individual clinician to determine which materials he or she prefers to use for everyday clinical situations. Newer nano-type materials are a welcome addition to the already fine array of composite resins available for clinical use.
References
1. Bowen RL. Dental filling material comprising vinyl siloxane treated fused silica and a binder Bis GMA. US patent 3 066 112. November, 1962.
2. Buonocore MG. A simple method of increasing the adhesion of acrylic materials to enamel surfaces. J Dent Res. 1955;34(6):849-853.
3. Talib R. Dental composites: a review. J Nihon Univ Sch Dent. 1993;35(3):161-170.
4. Leinfelder KF, Sluder TB, Sockwell CL, et al. Clinical evaluation of composite resins as anterior and posterior restorative materials. J Prosth Dent. 1975;33(4):407-416.
5. Jackson RD, Morgan M. The new posterior resins and a simplified placement technique. J Am Dent Assoc. 2000;131(3):375-383.
6. Mazer RB, Leinfelder KF. Evaluating a microfill posterior composite resin: A five-year study. J Am Dent Assoc. 1992;123(4):32-38.
7. Mazer RB, Leinfelder KF. Clinical evaluation of a posterior composite resin containing a new type of filler particle. J Esthet Restor Dent. 1988;1(1):66-70.
8. Roberson TM, Heymann HO, Swift EJ Jr. Sturdevant’s Art and Science of Operative Dentistry. 4th ed. St Louis, MO: Mosby; 2002.
9. Ferracane JL. Current trends in dental composites. Crit Rev Oral Biol Med. 1995;6(4):302-318.
10. Craig RG. Chemistry, composition, and properties of composite resins. Dent Clin North Am. 1981;25(2):219-239.
11. Roulet JF. Degradation of Dental Polymers. 1st ed. Basel, Switzerland: S Karger Pub; 1987.
12. Leinfelder KF. Composite resins. Dent Clin North Am. 1985;29(2):359-371.
13. Jordan RE. Esthetic Composite Bonding. 2nd ed. St Louis, MO: Mosby; 1992.
14. Kirk RE, Othmer DF. Encyclopedia of Chemical Technology. 4th ed. New York, NY: John Wiley and Sons; 1990.
15. Myshko D. Nanotechnology: It’s a small world. PharmaVOICE. February 2004;34-39.
16. Davis N. A nanotechnology composite. Compend Contin Educ Dent. 2003;24(9):662-670.
17. Terry DA, Leinfelder KF, Geller W, et al. Aesthetic & Restorative Dentistry. Everest Publishing Media; 2009.
18. Kovarik RE, Ergle JW. Fracture toughness of posterior composite resins fabricated by incremental layering. J Prosthet Dent. 1993;69(6):557-560.
19. Dietschi D. Free-hand composite resin restorations: a key to anterior aesthetics. Pract Periodontics Aesthet Dent. 1995;7(7):15-25.
20. Jefferies SR. The art and science of abrasive finishing and polishing in restorative dentistry. Dent Clin North Am. 1998;42(4):613-627.
About the Author
Robert Margeas, DDS
Adjunct Professor
Department of Operative Dentistry
University of Iowa College of Dentistry
Iowa City, Iowa
Private Practice
Des Moines, Iowa