Current Clinical Strategies with Lithium-Disilicate Restorations
Abstract
Ceramics have a rich history in dentistry, playing an integral role in providing high-quality, natural-appearing restorations. From the early days of porcelain jacket crowns to the leucite-reinforced glass ceramics of the 1990s, to new 3rd generation monolithic lithium-disilicate glass-ceramic material, ceramic technologies have evolved and will continue to revolutionize modern-day esthetic dentistry. In this overview article, two cases are presented that illustrate both partial- and full-coverage restorations using lithium-disilicate glass ceramics.
Ceramics have enjoyed a rich history in dentistry, from the porcelain jacket crown and shrink-free alumina crown (Cerestore® , Johnson & Johnson, www.jnj.com), to the castable glass-ceramic crown (Dicor® , Corning Glass Co., www.corning.com; DENTSPLY International, www.dentsply.com).1-4 In the early 1990s, leucite-reinforced glass ceramics (LRGC) were developed, which employed leucite crystals in an amorphous glass matrix (IPS Empress 1, Ivoclar Vivadent Inc., www.ivoclarvivadent.com). The leucite particles increased the strength of the material through the limitation of crack propagation. These restorations employed the lost-wax technique and thermal pressing technology.5 In addition, the ability to acid-etch the surface and adhesively bond to tooth structure greatly improved the predictability and survival of these restorations where prior efforts failed.6 LRGC restorations have stood the test of time and revolutionized modern-day esthetic dentistry.
Further development continued in 2000 with the introduction of a lithium-disilicate glass-ceramic (LDGC) material (IPS Empress 2, Ivoclar Vivadent), which improved the strength of single- and multiple-unit restorations. Early problems encountered were related to the de-veneering of the layered ceramic to the framework due to inadequate removal of the investment “skin” layer. The 2nd generation LDGC (Eris, Ivoclar Vivadent) addressed the concerns of cracking and de-veneering of the layering ceramic.
Recently, a 3rd generation monolithic lithium-disilicate glass-ceramic material (IPS e.max® CAD, Ivoclar Vivadent) was developed with flexural strength values between 360 MPa and 400 MPa for CAD and pressed restorations, respectively. In vitro laboratory studies of single-unit restorations using mouth-motion fatigue testing showed impressive results, where no failures were reported after 180,000 cycles at a load value of 900 N.7 The use of such material for fixed dental prostheses (FDPs) still remains a question due to the strength of the connector areas, with the understanding that connector strength is a function of mouth location, ie, anterior versus posterior FDP, and size. Data on 2- to 8-year survival rates of lithium-disilicate FDPs range from 50% to 93% and suggest that further work in this arena requires additional research and development.8-12
Clinical Applications
Partial Coverage
Partial-coverage restorations, ie, inlays and onlays, are excellent indications for lithium-disilicate glass ceramics due to their superior fatigue resistance strength.
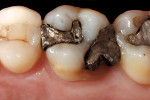
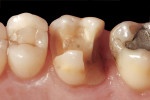
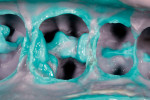
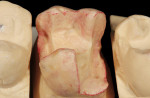
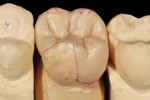
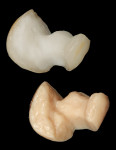
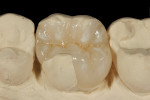
A patient presented with a fractured distal-palatal cusp of tooth No. 14 (Figure 1). The existing amalgam restoration was removed and the distal-palatal cusp was onlayed in the tooth preparation design (Figure 2). A polyvinyl siloxane (PVS) impression was made (Flexitime® , Heraeus Kulzer, www.heraeus-dental-us.com) (Figure 3), and a gypsum stone die was fabricated (ResinRock, Whip Mix Corp., www.whipmix.com) (Figure 4). The onlay restoration was created with medium hardness inlay wax (Modern Materials® , Heraeus Kulzer), invested, pressed, devested, fitted onto the stone die, and glazed, respectively (Figure 5 through Figure 7). The definitive restoration was evaluated in the cavity preparation for fit and marginal adaptation, and then luted with a dual-cure resin-based cement (Maxcem Elite™, Kerr Corporation, www.kerrdental.com) (Figure 8).
Full Coverage
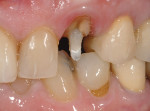
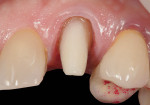
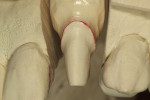
Full-coverage single-unit restorations are also excellent indications for LDGCs. In a separate case, a patient presented with a decemented core and crown restoration on tooth No. 11 (Figure 9). The fiber post (D.T. Light-Post® , Bisco, Inc., www.bisco.com) was intact, so a new core buildup (FluoroCore® , DENTSPLY Caulk,www.caulk.com) was fabricated (Figure 10). A chamfer preparation was created, a final impression made, and an acrylic provisional restoration fabricated. The impression was poured in gypsum stone, and dies were fabricated and trimmed (Figure 11).
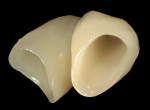
The lithium-disilicate full-coverage restoration was pressed to the correct shade/translucency ingot and characterized to the proper shade through two-set stain and one glaze cycle. The key to shade control is not to achieve the final shade in one stain/glaze cycle; through a stain-layering technique a more uniform shade can be achieved with depth of color (Figure 12).
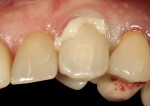
A dentin adhesive (ClearFil™ SE Bond, Kuraray Dental, www.kuraraydental.com) was applied and light-cured prior to definitive cementation with an autopolymerizing resin-based cement (Figure 13). The occlusion of the definitive restoration was reevaluated after cement removal (Figure 14), and a final radiograph was taken.
Summary
Ceramic technologies will continue to evolve and revolutionize modern-day esthetic dentistry as the demand—by patients and clinicians alike—for high-quality natural-appearing restorations continues to grow and drive the industry into the coming decades. The quest for the use of lithium disilicate for FDPs will continue through ongoing research and development.
References
1. McLean JW, Hughes TH. The reinforcement of dental porcelain with ceramic oxides. Br Dent J. 1965;119(6):251-267.
2. Adair PJ, Grossman DG. The castable ceramic crown. Int J Periodontics Restorative Dent. 1984;4(2):32-46.
3. Malament KA, Grossman DG. The cast glass-ceramic restoration. J Prosthet Dent. 1987;57(6):674-683.
4. Malament KA, Socransky SS. Survival of Dicor glass-ceramic dental restorations over 20 years: Part IV. The effects of combinations of variables. Int J Prosthodont. 2010;23(2):134-140.
5. Dong JK, Luthy H, Wohlwend A, Schärer P. Heat-pressed ceramics: technology and strength. Int J Prosthodont. 1992;5(1):9-16.
6. Oh SC, Dong JK, Lüthy H, Schärer P. Strength and microstructure of IPS Empress 2 glass-ceramic after different treatments. Int J Prosthodont. 2000;13(6):468-472.
7. Guess PC, Zavanelli RA, Silva NR, et al. Monolithic CAD/CAM lithium disilicate versus veneered Y-TZP crowns: comparison of failure modes and reliability after fatigue. Int J Prosthodont. 2010;23(5):434-442.
8. Esquivel-Upshaw JF, Young H, Jones J, et al. Four-year clinical performance of a lithia disilicate-based core ceramic for posterior fixed partial dentures. Int J Prosthodont. 2008;21(2):155-160.
9. Wolfart S, Eschbach S, Scherrer S, Kern M. Clinical outcome of three-unit lithium-disilicate glass-ceramic fixed dental prostheses: up to 8 years results. Dent Mater. 2009;25(9):e63-e71.
10. Marquardt P, Strub JR. Survival rates of IPS empress 2 all-ceramic crowns and fixed partial dentures: results of a 5-year prospective clinical study. Quintessence Int. 2006;37(4):253-259.
11. Taskonak B, Sertgöz A. Two-year clinical evaluation of lithia-disilicate-based all-ceramic crowns and fixed partial dentures. Dent Mater. 2006;22(11):1008-1013.
12. Makarouna M, Ullmann K, Lazarek K, Boening KW. Six-year clinical performance of lithium disilicate fixed partial dentures. Int J Prosthodont. 2011;24(3):204-206.
About the Author
Stephen J. Chu, DMD, MSD, CDT
Clinical Associate Professor and Director of Esthetic Education
Columbia University College of Dental Medicine
New York, New York