Peripheral Odontogenic Fibroma Associated with a Dilacerated Maxillary Central Incisor: A Case Report
Srinivas Sulugodu Ramachandra, MDS; Vidya Baliga, MDS; and Umesh Chandra Prasad, MDS
Abstract
The authors report a case of a 16-year-old male with peripheral odontogenic fibroma (POF) in the anterior maxilla associated with dilaceration of a tooth in its vicinity. A solitary, exophytic and sessile growth was present between the maxillary right central and lateral incisors and extended from the labial mucosa to the palatal gingiva. A periapical radiograph of the maxillary right central incisor revealed a shortened and dilacerated root. The growth was excised and sent for histopathologic examination. A diagnosis of POF (World Health Organization type) was rendered. The clinical and microscopic features are discussed.
Peripheral odontogenic fibroma (POF) is a rare lesion regarded in the World Health Organization (WHO) histologic typing of odontogenic tumors as a benign odontogenic neoplasm derived from fibroblasts.1 In 1982 Gardner2 described the nature of the POF, which had been considered the extraosseous counterpart of the central odontogenic fibroma.3 The incidences of POF in biopsied lesions ranged from 1% to 2% in pediatric patient studies4,5 and 9% to 10% in research in adults.6,7
Dilaceration is a deformity caused by a disturbance between the unmineralized and mineralized portions of a developing tooth germ.8 It can occur in the crown or root, resulting in the disruption of the tooth’s normal axial relationship.8 The problem is most frequently observed in the maxillary permanent incisor region.9 Dilacerations occur in approximately 3% of all permanent dentitions, with females being affected six times more frequently than males.9 The authors report a case of POF present for 10 years in a 16-year-old male and associated with dilaceration of the maxillary central incisor. The clinical and microscopic features of POF are discussed.
Case Report
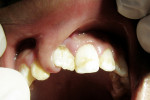
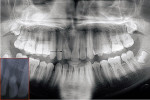
A 16-year-old male presented with a chief complaint of gums covering his upper right front tooth for the past 10 years. On examination, a solitary, exophytic, and firm sessile growth was observed between the maxillary right central and lateral incisors. The growth extended from the labial mucosa through the interdental papilla and onto the hard palate (Figure 1 and Figure 2). Measuring approximately 4 cm x 1 cm, the growth was broader near the attachment to the lip. Overlying mucosa was normal in appearance, with no evidence of discharge. Because the maxillary central incisor was rotated mesially, interdental contact with the adjacent lateral incisor was lost. Mammelons were noticed on the incisal aspect of the maxillary right central incisor, and generalized fluorosis of the dentition was present. Oral hygiene status around the maxillary central incisor was fair due to access difficulty. No history of trauma was present, and the growth had slowly increased throughout the 10 years. Eruption of the permanent maxillary right central incisor was delayed by approximately 2 years. Orthopantomographic and intraoral periapical radiographs revealed a dilacerated and shortened root of the right maxillary central incisor at its cervical one third. Dilaceration was present at the cervical one third of the root (Figure 3). The findings from a complete haemogram and medical history ruled out any systemic abnormalities. Differential diagnoses of fibroma, pyogenic granuloma, POF, peripheral giant cell granuloma, and neurofibroma were considered. Because fibroma is the most common among these lesions, the authors arrived at a provisional diagnosis of fibroma. An excisional biopsy was advised, and an informed consent was obtained from the patient.
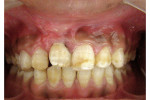
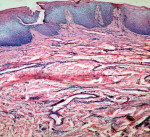
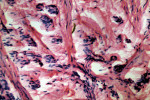
The growth was excised, and sutures were placed to approximate the incised wounds. Excised tissue was submitted for histopathologic examination. In the next appointment, sutures were removed and uneventful healing was noted (Figure 4). The findings from a microscopic examination revealed a lesion consisting of stratified squamous epithelium and underlying cellular connective tissue (Figure 5). Multiple small islands, cords, and strands of odontogenic epithelium resembling remnants of the dental lamina were in the connective tissue (Figure 6). A diagnosis of POF (WHO type) was established. Orthodontic correction of the rotated incisor was advised; however, the patient and his parents did not provide consent. The patient was lost to follow-up.
Discussion
Gingival overgrowths are usually plaque-related; however, nonplaque-related lesions referred to as reactive lesions and exemplified by a fibroma, pyogenic granuloma (or a tumor in pregnant women), peripheral giant cell granuloma, and POF. These fibromas are also reactive because pyogenic granulomas left untreated usually become fibromas and might develop ossifications, which can be categorized as POFs. Many traumatic fibromas are not preceded by pyogenic granuloma; traumatic fibromas do not become POF because POF has granulation tissue and fibromas do not. Benign neoplasms (eg, [not a neoplasm] neurofibroma) can also cause gingival overgrowth.10 Clinical and histopathologic features of these lesions are given in Table 1.11 Treatment of benign neoplasms is excision; if the excision is complete, recurrence is rare. Along with complete excision of the lesion, removal of the trigger factor, such as calculus, defective restorations/overhangs, restorative or impression materials not removed, and foreign bodies (eg, food, prophy paste), should be considered to avoid recurrence.
Clinically, POF appears as a localized, well-circumscribed, slow-growing, asymptomatic, exophytic growth of the gingiva, having a normal color, usually without ulceration.12 These growths are sessile, firm, and painless.12 A POF is mainly seen in the posterior region of the mandible and more prevalent in females in the second decade of life. On radiographic examination, slight erosion of the underlying bone may be seen.13 Microscopically, a key feature is the presence of multiple nests and strands of odontogenic epithelium in a cellular and fibrovascular stroma.13 The present case showed numerous islands and strands of odontogenic epithelium. The treatment of POF consists of surgical removal of the growth.
Odontogenic lesions presenting as enlarged opercula and resulting in the delayed eruption of teeth have been reported.14 Flaitz reported a case of a POF presenting as an overgrown gingiva around a partially erupted mandibular second molar.14 In the present case, the POF had prevented the eruption of the maxillary right central incisor for 2 years, after which the tooth erupted, albeit in a deviated path.
The etiology of dilaceration is not fully understood. It is generally accepted that an acute episode of mechanical trauma to the primary predecessors, whose apices lie close to the developing permanent tooth germ, may result in dilaceration of the permanent successor.15 Dilaceration has been observed in teeth with no predecessors, suggesting that dilaceration may be due to ectopic development of the tooth germ.16 Dilaceration in the authors’ case was seen at the cervical one third of the maxillary right central incisor. History of trauma to the deciduous predecessors was negative. Because the growth was present for 10 years, it is more likely that an episode of trauma was not remembered. The long history of the POF and its location between the maxillary right central and lateral incisors suggested it interrupted the normal path of eruption of the central incisor. However, the central incisor had continued to erupt in a deviated path, along with a shift in the angulation of the mineralized and unmineralized portions, leading to dilaceration at the cervical one third on the distal aspect. Displacement of teeth and interference with eruption of teeth may be an associated finding with POF.14
For 10 years, the patient had opted to not receive treatment. POFs attaining large sizes had been reported in a retrospective analysis performed in a Taiwan Chinese population.17 Lin et alreported a case of a POF in a 30-year-old Chinese woman in the right mandible that was 4.5 cm x 4 cm and had been present for 2 years.17 In the present case, the size of the growth was 4 cm x 1 cm with the growth being much broader near its attachment to the undersurface of the lip. Resorption of the underlying bone was not observed. Similar to the case reported by Lin et al, the authors’ case report also highlights the size that these lesions can attain in a long absence of treatment. A POF can cause spacing and delay the eruption of teeth.17
A WHO-type POF usually shows a cellular fibrous stroma, whereas the non-WHO type shows more collagenous fibrous stroma with plump fibroblasts. However, some investigators no longer categorize these as WHO and non-WHO types.3
Gingival growths commonly manifest as inflammatory or reactive lesions and rarely manifest as peripheral odontogenic neoplasms. If not excised, POFs can cause alteration in the path of eruption and delay in eruption of teeth, as well as grow significantly.
References
1. Daley TD, Wysocki GP. Peripheral odontogenic fibroma. Oral Surg Oral Med Oral Pathol. 1994;78(3):329-336.
2. Gardner DG. The peripheral odontogenic fibroma: an attempt at clarification. Oral Surg Oral Med Oral Pathol. 1982;54(1):40-48.
3. Barnes L, Eveson JW, Reichart P, et al. Pathology and Genetics, Head and Neck Tumors, Classification of Tumors. Geneva, Switzerland: World Health Organization; 2005:317.
4. Skinner RL, Davenport WD Jr, Weir JC, et al. A survey of biopsied oral lesions in pediatric dental patients. Pediatr Dent. 1986;8(3):163-167.
5. Das S, Das AK. A review of pediatric oral biopsies from a surgical pathology service in a dental school. Pediatr Dent. 1993;15(3):208-211.
6. Stablein MJ, Silverglade LB. Comparative analysis of biopsy specimens from gingiva and alveolar mucosa. J Periodontol. 1985;56(11):671-676.
7. Layfield LL, Shopper TP, Weir JC. A diagnostic survey of biopsied gingival lesions. J Dent Hyg. 1995;69(4):175-179.
8. Jafarzadeh H, Abbott PV. Dilaceration: review of an endodontic challenge. J Endod. 2007;33(9):1025-1030.
9. Ezoddini AF, Sheikhha MH, Ahmadi H. Prevalence of dental developmental anomalies: a radiographic study.Community Dent Health. 2007;24(3):140-144.
10. Fatima G, Sandesh N, Ravindra S, et al. Moving beyond clinical appearance: the need for accurate histological diagnosis. Gen Dent. 2009;57(5):472-477.
11. Neville BW, Damm DD, Allen CM, et al. Oral and Maxillofacial Pathology. 3rd ed. St. Louis, MO: Elsevier; 2009:507-552.
12. Sciubba J, Fantasia J, Kahn LB, eds. AFIP Atlas of Tumor and Pathology. Washington DC: Armed Forces Institute of Pathology; 2001:105-126.
13. Bonetti GA, Marini I, Zucchelli G, et al. Obstruction of the eruption pathway by peripheral odontogenic fibroma: report of a patient. Am J Orthod Dentofacial Orthop. 2008;133(2):303-317.
14. Flaitz CM. Gingival enlargement associated with a partially erupted mandibular molar. Pediatr Dent. 2001;23(5):435-437.
15. McNamara T, Woolfe SN, McNamara CM. Orthodontic management of a dilacerated maxillary central incisor with an unusual sequela. J Clin Orthod. 1998;32(5):293-297.
16. Andreasen JO, Sundström B, Ravn JJ. The effect of traumatic injuries to primary teeth on their permanent successors. I. A clinical and histologic study of 117 injured permanent teeth. Scand J Dent Res. 1971;79(4):219-283.
17. Lin CT, Chuang FH, Chen JH, et al. Peripheral odontogenic fibroma in a Taiwan Chinese population: a retrospective analysis. Kaohsiung J Med Sci. 2008;24(8):415-421.
About the Authors
Srinivas Sulugodu Ramachandra; MDS
Senior Lecturer
Department of Periodontics
Kanti Devi Dental College and Hospital
Mathura, India
Vidya Baliga, MDS
Senior Lecturer
Department of Periodontics
Kanti Devi Dental College and Hospital
Mathura, India
Umesh Chandra Prasad, MDS
Professor and Head
Department of Oral Pathology and Microbiology
Kanti Devi Dental College and Hospital
Mathura, India