Direct Restorative Treatment of Dental Erosion Caused by Gastroesophageal Reflux Disease Associated with Bruxism: A Case Report
Cristina de Mattos Pimenta Vidal, DDS; Anderson Catelan, DDS; André Luiz Fraga Briso, DDS, MS, PhD; and Paulo Henrique dos Santos, DDS, MS, PhD
Abstract:
Gastroesophageal reflux disease (GERD) is a gastrointestinal disorder in which stomach acids are chronically regurgitated into the esophagus and oral cavity. Continual exposure of the teeth to these acids can cause severe tooth wear. Dentists are often the first healthcare professionals to diagnose dental erosion in patients with GERD. This article presents a case report of a 27-year-old male smoker with tooth wear and dentin sensitivity caused by GERD associated with bruxism. After diagnosis, a multidisciplinary treatment plan was established. The initial treatment approach consisted of medical follow-up with counseling on dietary and smoking habits, as well as management of the gastric disorders with medication. GERD management and the dental treatment performed for the eroded dentition are described, including diagnosis, treatment planning, and restorative therapy.
The loss of dental hard tissues without bacterial action is a multifactorial condition and, depending on the process and cause of wear, can be called attrition, erosion, or abrasion. Attrition is defined as physiologic tooth wear caused by direct contact of tooth against tooth,1 abrasion is the wear caused by a mechanical/rubbing process,2 and erosion is the tooth dissolution caused by a chemical process.3 Frequently, the wear caused by a mechanical process is related to toothpaste abuse and bruxism,2 while the chemical process involves acids that reach the mouth and have extrinsic or intrinsic origin. The extrinsic acid material includes certain medications, coffee, acidic fruit juices, soft drinks, and alcoholic beverages. Exposure to intrinsic acids occurs as a result of bulimia nervosa, anorexia nervosa, vomiting, hiatus hernia, and gastroesophageal reflux.4
Gastroesophageal reflux disease (GERD) is a gastrointestinal disorder caused by a relaxing of the sphincter between the stomach and esophagus, allowing inverse movement of fluid, including gastric juices, into the esophagus. The fluid can reach the cervical portion of the esophagus, pharynx, and oral cavity.5
Risks factors for GERD are obesity, hiatus hernia, and pregnancy. The most common symptoms are vomiting, heartburn or retrosternal burning discomfort, oral regurgitation of bitter gastric contents, laryngitis, asthma, cough, angina, and dental erosion.5,6 However, not all patients experience these systemic symptoms; dental erosion may be the first to appear.
When a substance with a pH below 5.5 (ie, the critical pH of the enamel) reaches the mouth, it can dissolve the hydroxiapatites crystals in enamel.7 Gastric juices have an extremely acidic pH, which indicates their erosive potential and capability in producing severe erosion on dental surfaces.
In the mouth, saliva has an important role in protecting teeth from dissolution because of its diluting and buffering capacity. Some studies have shown lower saliva buffering capacity in patients with GERD than in normal individuals.8 However, dental erosion may be a multifactorial phenomenon in which the saliva's protective buffering capacity is overcome by either reduced salivary secretion or a higher amount of gastric refluxate.6
Although accurately diagnosing noncarious lesions can be difficult, the distribution and clinical appearance of the lesions can help identify the cause. For example, dental erosion on the lingual surfaces of anterior maxillary teeth is related to bulimia or vomiting, whereas dental lesions on posterior teeth involving lingual and occlusal surfaces may suggest GERD.4
The consequences in the oral cavity of the loss of dental structure are sensitivity to thermal, tactile, and sweet stimuli; pain during mastication; loss of vertical dimension; and temporomandibular joint pain in severe cases, which occur when GERD is associated with other factors, such as attrition, bruxism, and consumption of acidic foods and beverages.9,10 Bruxism is the habitual grinding of teeth (tooth to tooth when not eating), which is the major cause for abrasion.2 Its combination with GERD can severely damage dentition.
The erosion lesions on teeth can present in different stages from a loss of surface luster evident on clean, dry enamel (early stages) to typically yellowish areas on the surface of the tooth, caused by exposure of the underlying dentin through the thinned overlying enamel.3
Treatment of these lesions depends on the severity of the tooth wear and can range from placement of composite restorations in the areas of corrosion to full-mouth rehabilitation with indirect materials in cases of devastated dentition.11 This should be conducted after medical treatment has eliminated the acid reflux cause.5
The aim of this study was to report and discuss a case presentation of tooth wear caused by GERD associated with bruxism.
Case Report
A 27-year-old male smoker presented to the restorative dentistry department of Araçatuba Dental School—UNESP in São Paulo, Brazil complaining about the appearance and sensitivity of his teeth. The patient said he had frequent heartburn and had noticed the oral lesions approximately 5 years earlier. At that time, he sought dental treatment and was informed about the tooth wear. The use of an occlusal splint was recommended.
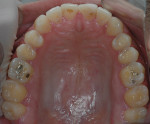
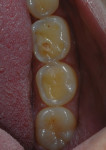
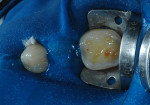
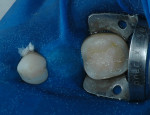
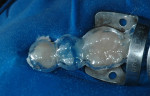
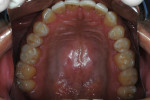
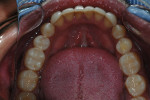
During clinical examination, good oral hygiene was noted. The patient showed corrosion of occlusal and palatal surfaces of the maxillary and mandibular posterior teeth (Figure 1 and Figure 2). He also had dentin tissue areas displayed (Figure 3) and amalgam restorations compromised by a lack of support.
Based on clinical interview and in consideration of the clinical aspect of the lesions, the patient was referred to a gastroenterologist for verification of possible systemic alterations that could be related to the tooth wear. Endoscopy examination showed a hiatus hernia with erosive esophagitis (Grade 2 of Los Angeles Classification) and bulbar erosive duodenitis. The gastroenterologist prescribed pantoprazole sodium 40 mg a day (Protonix®, Pfizer Inc., www.pfizer.com) and recommended weight loss; avoidance of foods and liquids before bedtime; avoidance of fatty and spicy foods; and abstinence from smoking, alcohol, and coffee.
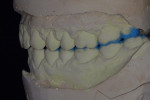
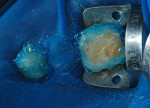
After the treatment of GERD's causes, alginate impressions were taken and the cast models were mounted on a semiadjustable articulator. The areas to be restored were waxed-up on the models for diagnostic analysis of the desired occlusal relation. Then a semirigid acetate tray was created to serve as a guide during the restorative procedure. According to the analysis of the models mounted in the articulator, the minimum height to reestablish the vertical dimension of occlusion was 1.5 mm (Figure 4).
The posterior area of the acetate tray was cut in the region of canine and first premolar and the pieces were used to restore all posterior teeth. Colors A2 for dentin and A2E for enamel were selected. The cavities prepared for corrosion lesions were limited by the removal of preexisting restorations. It was opted to use general field isolation with rubber dam, intercalating teeth to prevent the composite from reaching the proximal faces. After pumice prophylaxis was performed, enamel surfaces were etched with 37% phosphoric acid (Scotchbond™ Etchant, 3M ESPE, www.3MESPE.com) for 30 seconds (Figure 5). After rinsing with an air/water spray for 30 seconds, a self-etching adhesive (Clearfil™ SE Bond, Kuraray America Co., www.kuraraydental.com) was applied to the enamel and dentin and light-cured with a halogen device (Optilight Plus, Gnatus, www.gnatus.com.br) at 500 mW/cm2 for 20 seconds (Figure 6).
The composite resin (Filtek™ Supreme XT A2D, 3M ESPE) was initially inserted in the region of the amalgam restoration and light-cured with a halogen device for 20 seconds (Figure 7). Then, a bigger portion of the composite was distributed on all occlusal surfaces. The guide then was filled with the composite resin Filtek™ Supreme XT A2E (3M ESPE) and led into position. Photoactivation was performed for 40 seconds (Figure 8). After polymerization, the composite excesses had been removed with a 3195F diamond bur (K.G. Sorensen Ind. Com. LTDA, www.kgsorensen.com.br) and Sof-Lex™ Pop-On sandpaper discs (3M ESPE) (Figure 9).
All posterior teeth were rehabilitated with direct resin-based restoration for a hemi-arc similar to what was described previously, reestablishing the vertical dimension (Figure 10 and Figure 11). Occlusal adjustment was realized, and some repairs in the proximal contacts were performed to achieve a better proximal contour.
Anterior guidance was reestablished through the increase of approximately 2 mm of the incisal of mandibular anterior teeth (canine to canine). Restoration of tooth No. 11 was performed because the presenting tooth had an unsatisfactory form. The same materials and colors were used for anterior teeth restoration (Figure 12). The new occlusal splint was created to help ensure good clinical longevity. The patient received oral hygiene instructions.
The patient was asked to attend scheduled in-office visits to check the preservation of the occlusal parameters and to certify that the restorations were in perfect function. After 12-month follow-up, correct function of the stomatognathic system was checked and new polishing was performed. The patient was questioned about the sensitivity and gastric disturbances and reported the pain had almost disappeared. The patient had not stopped smoking.
Discussion
Because the loss of tooth surface is a multifactorial condition, the dental treatment plan should include medical treatment in order to prevent further lesions. This means the involvement of other health professionals for the definitive diagnosis.
In the present case, the clinical appearance of the lesions suggested the diagnosis: the occlusal surface of posterior teeth presented areas of cupping or depressions with spoon-shaped appearance caused by erosion.1,12
When GERD is diagnosed, the treatment must be as minimally invasive as possible and the treatment plan should consider the threat to the tooth's structural integrity; the dentin hypersensitivity; the loss of tooth structure, vertical dimension, and/or function; esthetic damage; and possible pulp exposure.13
The severity of tooth lesions can vary, and the treatment depends on the individual's circumstances. Initial restorative treatments should be conservative, especially in younger patients, and may include adhesive resins to restore appearance and function and the use of composites if the wear is in a low-stress area.14 However, when the wear is more extensive, with loss of vertical dimension, an occlusal reconstruction with adhesive resins or crowns may be necessary.
In this case, although the patient used a nightguard to avoid the wear from bruxism, the tooth with amalgam restorations presented a clean and stain-free surface, which suggested an active erosion process.1 Conservative treatments for dentin sensitivity may be considered; replacing lost dental structure is often necessary. In the present case, the factor that established the necessity of treatment was the loss of tooth structure associated with hypersensitivity.
The material selected should preserve the natural tooth whenever possible.12 In the present case, considering the severity of loss in restricted areas with adequate tooth structure present for bonding, the composite resin was an option for restoration of tooth wear. The advantages of using a composite resin are its lower cost compared to indirect treatments, facility to use by the dental professionals, the longevity even in posterior areas,15 and the possibility of repairs when necessary. In addition, some studies demonstrated composite resin restorations reach longevity and success rates that closely match those of other materials when properly used.16 Research has also shown that in acidic conditions, all dental restorative materials have shown degradation over time and composite materials have shown higher durability.17
The choice of a self-etch adhesive system is based on the absence of rinsing and drying steps to maintain the ideal humidity of the dentine. The adhesive system used is classified as mild self-etch adhesive, which can demineralize the dentin, maintaining residual hydroxyapatite. This is considered an advantage for better bonding and durability of restoration.18 However, it has been proposed that additional etching be performed only in the enamel when using this type of adhesive systems due to its lower demineralization rate compared to the phosphoric acid on this substrate.18
While analyzing the occlusion and models, the lack of space was noted, which was probably caused by a secondary eruption of the teeth to compensate for the wear.1,19 Treatment was impossible without reestablishing the vertical dimension. For this reason, the height was kept as minimum as possible to restore tooth form and function. Considering that the masticatory system is capable of successful adaptation to minimal or moderate adaptation changes in the vertical dimension of occlusal,19 the treatment was performed without using an occlusal splint for some time. After treatment, the patient did not relate pain or discomfort.
Following the occlusal restorative procedure and adjustments, the restitution of a lateral and anterior guidance was necessary in order to achieve a stable occlusion and comfort function for the stomatognathic system.20 Fabrication of a new splint guard helps guarantee the durability of the treatment realized and prevents further wear mainly from bruxism.
Conclusion
Considering the damage in the dentition caused by a systemic illness such as GERD and the fact that sometimes the patient may not show other symptoms, the dentist should be able to identify the oral lesions as a sign of a possible systemic disease and perform the correct dental treatment.
References
1. Bartlett DW. The role of erosion in tooth wear: aetiology, prevention and management. Int Dent J. 2005;55(4 suppl 1):277-284.
2. Abrahamsen TC. The worn dentition–pathognomonic patterns of abrasion and erosion. Int Dent J. 2005;55(4 suppl 1):268-276.
3. Pindborg JJ. Chemical and physical injuries. Pathology of the Dental Hard Tissues. 1st ed. Philadelphia, PA: WB Saunders Co.; 1970:312-325.
4. Bartlett DW, Evans DF, Anggiansah A, et al. A study of the association between gastro-oesophageal reflux and palatal dental erosion. Br Dent J. 1996;181(4):125-131.
5. Van Roekel NB. Gastroesophageal reflux disease, tooth erosion, and prosthodontic rehabilitation: a clinical report. J Prosthodont. 2003;12(4):255-259.
6. Farrokhi F, Vaezi MF. Extra-esophageal manifestations of gastroesophageal reflux. Oral Dis. 2007;13(4):349-359.
7. Gudmundsson K, Kristleifsson G, Theodors A, et al. Tooth erosion, gastroesophageal reflux, and salivary buffer capacity. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1995;79(2):185-189.
8. Moazzez R, Bartlett D, Anggiansah A. Dental erosion, gastro-oesophageal reflux disease and saliva: how are they related? J Dent. 2004;32(6):489-494.
9. Lazarchik DA, Filler SJ. Effects of gastroesophageal reflux on the oral cavity. Am J Med. 1997;103(5A):107S-113S.
10. Machado NAG, Fonseca RB, Branco CA, et al. Dental wear caused by association between bruxism and gastroesophageal reflux disease: a rehabilitation report. J Appl Oral Sci. 2007;15(4):327-333.
11. Gandara BK, Truelove EL. Diagnosis and management of dental erosion. J Contemp Dent Pract. 1999;1(1):16-23.
12. Aziz K, Ziebert AJ, Cobb D. Restoring erosion associated with gastroesophageal reflux using direct resins: case report. Oper Dent. 2005;30(3):395-401.
13. Lambrechts P, Van Meerbeek B, Perdigão J, et al. Restorative therapy for erosive lesions. Eur J Oral Sci. 1996;104:229-240.
14. Yip HK, Smales RJ, Kaidonis JA. Management of tooth tissue loss from erosion. Quintessence Int. 2002;33(7):516-520.
15. el-Mowafy OM, Lewis DW, Benmergui C, et al. Meta-analysis on long-term clinical performance of posterior composite restorations. J Dent. 1994;22(1):33-43.
16. Ritter AV. Direct resin-based composites: current recommendations for optimal clinical results. Compend Contin Educ Dent. 2005;26(7):481-527.
17. Jaeggi T, Grüninger A, Lussi A. Restorative therapy of erosion. Monogr Oral Sci. 2006;20:200-214.
18. Van Landuyt KL, Kanumilli P, De Munck J, Peumans Met al. Bond strength of a mild self-etch adhesive with and without prior acid-etching. J Dent. 2006;34(1):77-85.
19. Rivera-Morales WC, Mohl ND. Relationship of occlusal vertical dimension to the health of masticatory system. J Prosthet Dent. 1991;65(4):547-553.
20. McIntyre F. Restoring esthetics and anterior guidance in worn anterior teeth. A conservative multidisciplinary approach. J Am Dent Assoc. 2000;131(9):1279-1283.
About the Authors
Cristina de Mattos Pimenta Vidal, DDS
Postgraduate student
Department of Restorative Dentistry
Araçatuba School of Dentistry–UNESP
São Paulo, Brazil
Anderson Catelan, DDS
Postgraduate student
Department of Restorative Dentistry
Araçatuba School of Dentistry–UNESP
São Paulo, Brazil
André Luiz Fraga Briso DDS, MS, PhD
Associate Professor
Department of Restorative Dentistry
Araçatuba School of Dentistry–UNESP
São Paulo, Brazil
Paulo Henrique dos Santos DDS, MS, PhD
Assistant Professor
Department of Dental Materials and Prosthodontics
Araçatuba School of Dentistry–UNESP
São Paulo, Brazil