“Digidontics”: The Computerization of Restorative Dentistry—A Case Report
Abstract
Today’s practitioners of dentistry can be overwhelmed by the need to analyze, understand, prioritize, and implement the extraordinary amounts of knowledge and technical skill required to practice ideal dentistry. Continuing education is not just necessary; an increasingly informed patient population demands it. Among many technological advancements, computers have permeated the mainstream of restorative dentistry. The conventional systems of radiography and impressioning are the latest to face a digital counterpart. This case presentation demonstrates how cone beam computerized tomography (CBCT) and a dedicated digital impressioning system can be used alongside conventional techniques to obtain excellent esthetic and functional results.
In his book The Checklist Manifesto, Dr. Atul Gawande writes that patients expect healthcare professionals to “aim for excellence in [their] knowledge and expertise.”1 Certainly everyone in the dental profession aspires to excellence in the treatment that they provide for their patients. However, with the rapid and voluminous increase in knowledge and technology in the discipline of dentistry, it is a daunting task to remain completely informed and to incorporate these changes into everyday practices. Add to this challenge the evidence that, when faced with such rapid and abundant informational influx many clinicians may make poor decisions or choose to make no decision at all,2 and one can begin to appreciate the challenge that clinicians face in practicing ideal dentistry today. As trusted healthcare providers, dental practitioners must familiarize themselves with these advancements and then incorporate procedures that enable them to provide the best, most up-to-date care for their patients. This case presentation demonstrates how two such technological advancements, cone beam computerized tomography (CBCT) and dedicated digital impressioning, can be implemented alongside traditional techniques to predictably improve treatment planning as well as treatment outcomes.
Case Report
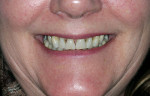
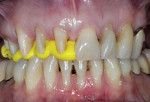
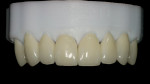
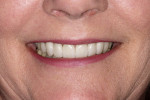
A 55-year-old woman who had been well served by her conventional prosthetics desired to replace her maxillary removable partial denture and improve her esthetic situation (Figure 1). Her periodontal disease had been stabilized for many years, and she had been highly compliant in an alternating maintenance program between the periodontist and restorative dentist.
Conditions existing at initiation of treatment were as follows:
- missing teeth Nos. 1 through 3, 13 through 17, and 32
- tooth No. 4 compromised periodontally and endodontically
- ceramometal crowns Nos. 4 and 12
- Kennedy Class 1 removable partial denture utilizing semiprecision attachments teeth Nos. 4 and 12
- bone and soft-tissue loss in her maxillary anterior teeth resulting in esthetically distracting soft-tissue recession
- displeasing tooth shape secondary to incisal edge wear and interproximal bone and tissue loss
The author’s anticipated plan was as follows:
- all-ceramic crowns Nos. 5 through 12
- implant-supported crowns Nos. 2 through 4, 13, and 14
- mandibular arch restorations in the future
There were no medical contraindications to her proposed treatment plan.
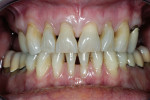
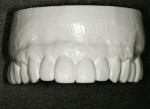
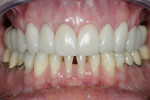
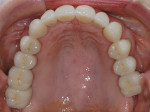
The first objective in planning a complex restorative case is the esthetic diagnosis, which begins with the determination of the incisal edge position.3 Ideally, the anterior teeth fit into the frame of the lips with the incisal edges coincident with the lower lip during full smile.4 The buccal cusps of the posterior teeth continue to follow this curve with no deviations from the occlusal plane. Esthetically, in full smile, this patient’s tooth size and position were favorable, with the maxillary lip generally coincident with the tooth/gingiva interface and the incisal edges generally paralleling her mandibular lip (Figure 2). In addition to a darkened shade, her chief detractors esthetically were the shape of the anterior teeth and the absence of interdental papillae, factors that resulted in unsightly “black triangles,” which were magnified by the triangular contours of the teeth (Figure 3). Having confirmed that the teeth were in good overall position as determined by the above parameters and that the incisogingival length of the central incisors needed a 1-mm increase to achieve the ideal dimension of 75% to 80% height-to-width ratio,5 the author took alginate impressions for fabrication of diagnostic casts. These casts were then mounted on a semi-adjustable articulator using a facebow transfer and a centric occlusion record. Physical measurements and photographs aided in transferring the desired tooth changes to the laboratory where a maxillary full-arch diagnostic waxup was completed. This waxup was then duplicated for use in fabricating direct provisional restorations (Figure 4).
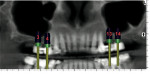
Concurrent with the esthetic diagnosis was the need to plan for posterior restorations. Because implant-supported crowns were the desired final restoration, the use of CBCT was incorporated into the diagnosis and positional planning. Since its introduction to the US dental market in 2001, CBCT is rapidly becoming a vital tool for the diagnosis and planning of dental implant-supported restorations.6 CBCT enables a three-dimensional (3-D) evaluation of the availability, dimension, quantity, and quality of the bone at the proposed implant site(s). Any areas of deficiency can be known before surgery, dramatically reducing errors and unforeseen problems.7 After image capture, the digital data can then be formatted in one of many available software programs and the implant placement accomplished virtually (Figure 5).
In order to be able to visualize the proposed crowns in the digital image, a radiographic template was created using radiopaque teeth in the areas of planned replacement. The CBCT was taken and the resulting data was formatted into implant-planning software. Another benefit of digital imaging is the ability to engage in simultaneous online collaboration with imaging center software specialists, the restorative dentist, and the surgeon. The restorative plan and the surgical plan can be visualized and any adjustments made prior to finalization of the surgical guide and its subsequent fabrication.
This visualization of the proposed restorations and the bone into which the implants were to be placed allowed for a restoratively driven plan8 to place implants in the position of teeth Nos. 2 through 4, 13, and 14. It has been shown that the use of CBCT and software planning programs may result in greater predictability and accuracy in the surgical placement of dental implants.9 From the CBCT data and this digital plan the author ordered a stereolithographic (SLA) surgical guide. SLA is a process whereby digital data is used by lasers to cure photosensitive resin to precise dimensions. SLA surgical guides improve the accuracy of the placement position of implants over freehand placement through precisely placed positioning cylinders.10,11 Because the patient’s available bone from crest to sinus floor was deficient, maxillary sinus augmentation at the time of implant placement was deemed necessary. The use of demineralized freeze-dried bone allograft was planned for this augmentation.12
At the first surgical appointment tooth No. 4 was extracted, the maxillary sinuses were exposed using a lateral window technique, the sinus membrane was gently elevated, and the graft material was placed to augment the bony vertical dimension. With the aid of the surgical guide, implants were placed in the positions of teeth Nos. 2 through 4, 13, and 14 (Figure 6). Cover screws were placed and appropriate postoperative instructions and medications were prescribed to the patient. It was decided to forego placement of a provisional interim partial denture until 3 weeks post-surgery in order to allow for undisturbed initial healing and resolution of swelling and discomfort. At its delivery the transitional appliance was relined with tissue-conditioning material in order to increase retention and minimize pressure to the surgical site. Post-surgical complications were minimal.
Capturing Digital Data
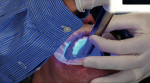
At 10 weeks post-implant placement, the restorative plan was initiated. The second digital technology used in this case, a dedicated digital impressioning system, was chosen for the capture of digital data to be used for creation of the final tooth-supported crowns. These systems were first introduced in 2007 with Cadent, Inc.’s iTero™ (www.cadentinc.com), followed by 3M ESPE’s Lava™ C.O.S. (www.3MESPE.com) in 2008, and CEREC® Bluecam (Sirona Dental Systems, www.sirona.com) in 2009. This case report will demonstrate the use of the Lava C.O.S. system. Dedicated digital impressioning systems capture digital data that is used to replicate the intraoral condition and replace elastomeric impression materials; they are not CAD/CAM systems with a chairside-milling unit. The principal benefit of digital systems is the elimination of numerous steps that can incorporate distortion into the final restoration. Tray selection, material mixing, tray seating, undisturbed set, disinfection, gypsum die stone pouring, die sawing, and ditching are but a few of the steps that computers replace. As in all areas where computerization has been incorporated, efficiency and accuracy are improved compared to “analog” systems, but not without overcoming a learning curve required to establish proficiency in their use.
Another advancement of digital impressioning systems is the ability to preview all aspects of the preparation prior to capture of the digital information (Figure 7). Should any modifications be needed after this initial video view, they can be made pre-scan, enabling ideal preparation design and isolation. In practice, this feature alone has the ability to improve outcomes, as the operator can be certain of accuracy with no need for “remakes.” After the scan is completed, the digital data is transferred to the dental laboratory electronically where virtual articulation, margin marking, die cutting, and ditching are accomplished.13 Once this electronic design is complete the data is again electronically transferred, this time to a model manufacturing facility for fabrication of the master model to be used in the creation of the final restorations. The C.O.S. system uses SLA model manufacturing for production of the master model used for restoration fabrication. The accuracy of the SLA model created from the digital impression is equal to or greater than that of the gypsum cast created from elastomeric impression systems.14
In this case, teeth Nos. 5 through 12 were isolated with a dental dam and prepared for lithium disilicate, all-ceramic crowns. In order to maintain the existing vertical dimension of occlusion, teeth Nos. 5 through 8 were prepared first and the jaw relation for these teeth was recorded (Figure 8). The preparations for the remaining teeth were then completed and a second jaw relation was recorded, having placed the first record back into position, thereby confirming adequate occlusal reduction and maintaining the preoperative vertical dimension. After a first retraction cord was placed circumferentially, the margins of the preparations were finalized and a second retraction cord was placed.
As in conventional impressioning, dryness is essential for accurate replication. Immediately after the removal of the second retraction cord and prior to initiating the scan, a light application of titanium dioxide powder was dusted onto the target scan site in order to provide the computer with points of surface reflectivity. While watching the computer monitor to ensure complete digital data uptake, the author passed the scanning wand over all intraoral surfaces that would be captured in a final conventional impression, both in the operative and the opposing quadrants (Figure 9, Figure 10 and Figure 11). As the data was captured, the monitor displayed a real-time 3-D model of the replicated intraoral condition (Figure 12). While the jaw relation was then captured electronically with the patient closed into one-half of the vinyl polysiloxane (VPS) record mentioned earlier, in actuality the conventional record was used to articulate the models, as a full-arch case could not yet be virtually transferred to an articulator. In cases that do not involve complete loss of the vertical dimension, the C.O.S. will replicate the jaw relation with outstanding accuracy, transferring this interocclusal relationship to the master models.15 Provisional restorations were fabricated using a putty matrix of the diagnostic waxup and a bis-acryl material. The provisional restorations provided an insight into the quality of the esthetic planning and served as a matrix for creation of the final crowns (Figure 13). The fit of the interim partial denture was confirmed and the patient was dismissed. Using the master SLA models (Figure 14) and all records for mounting and articulation, the laboratory fabricated lithium disilicate restorations (Figure 15). At the delivery appointment, the provisional restorations were removed, the prepared teeth were cleaned with a slurry of water and pumice, and the final restorations were tried in. All restorative results were outstanding with little to no adjustment necessary. The restorations were cemented using a self-adhesive resin cement.
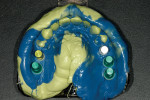
Having had sufficient time for healing, the implants were then exposed, the cover screws were removed, and solid abutments were placed and torqued to 35 Ncm. At the time of this procedure the protocol for scanning implants/abutments required fully exposed abutments. This would have required placement of retraction cords to expose the margins of the abutments, so impressioning baskets and positioning cylinders were placed and a VPS impression was captured (Figure 16) as well as a jaw relation record.
Provisional restorations were again fabricated using a putty matrix of the diagnostic waxup and cemented with provisional cement. Ceramometal crowns were then constructed for the implants in the position of teeth Nos. 2 through 4, 13, and 14. At the delivery appointment, the provisional restorations were removed, the abutments were cleaned with a slurry of water and pumice, the final crowns were tried in, and any necessary adjustments were made. After all results were confirmed as excellent, the crowns were cemented.
Successful Results
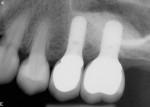
Postoperative radiographs demonstrate the accuracy of the planning and placement achieved utilizing CBCT technology and its associated software. The implants were positioned in the exact positions of the missing teeth, enabling excellent contour, occlusion, and function of the final crowns. The native and grafted bone were well healed, with the implants appearing well integrated. (Figure 17 and Figure 18).
The final postoperative photographs attest to the successful esthetic and functional results achieved in this case, exceeding the goals of both the patient and the operator (Figure 19, Figure 20, Figure 21 and Figure 22). The dedicated digital impressioning technology enabled creation of precisely fitted, highly esthetic restorations.
The efficiency and accuracy of computers have now firmly entrenched them into the world of restorative dentistry. In the case presented, “digidontics” improved treatment planning as well as treatment outcome. The standard of care in dentistry is ever changing. Dental professionals must stay abreast of these changes in order to be worthy of their patients’ trust.
Acknowledgment
The author would like to acknowledge and thank Eric Rindler, DDS, periodontist, San Antonio, Texas, for the skillful and precise placement of the sinus grafts and dental implants for this case, and Summit Dental Laboratory in Waco, Texas for creating the artistic restorations shown herein.
Disclosure
Dr. Schroder has received honoraria from 3M ESPE.
References
1. Gawande A. The Checklist Manifesto, How to Get Things Right. 1st ed. New York, NY: Metropolitan Books, Henry Holt and Co; 2010:182.
2. Begley S. Brain Freeze: how the deluge of information paralyzes our ability to make good choices. Newsweek. March 7, 2011:28-33.
3. Robbins JW. The incisal edge position in complex restorative dentistry. Texas GP. 2000;26(2):12-14.
4. Robbins JW. Differential diagnosis and treatment of excess gingival display. Pract Periodontics Aesthet Dent. 1999;11(2):265-272.
5. Gillen RJ, Schwartz RS, Hilton TJ, Evans DB. An analysis of selected normative tooth proportions. Int J Prosthodont. 1994;7(5):410-417.
6. Curley A, Hatcher DC. Cone beam CT—anatomic assessment and legal issues: the new standards of care. J Calif Dent Assoc. 2009;37(9):653-662.
7. Worthington P, Rubenstein J, Hatcher, DC. The role of cone-beam computed tomography in the planning and placement of implants. J Am Dent Assoc. 2010;141(suppl 3):19S-24S.
8. Rosenfeld AL, Mandelaris GA, Tardieu PB. Prosthetically directed implant placement using computer software to ensure precise placement and predictable prosthetic outcomes. Part 1: diagnostics, imaging, and collaborative accountability. Int J Periodontics Restorative Dent. 2006;26(3):215-221.
9. Orentlicher G, Goldsmith D, Horowitz A. Applications of 3-dimensional virtual computerized tomography technology in oral and maxillofacial surgery: current therapy. J Oral Maxillofac Surg. 2010;68(8):1933-1959.
10. Ozan O, Turkyilmaz I, Ersoy AE, et al. Clinical accuracy of 3 different types of computed tomography-derived stereolithographic surgical guides in implant placement. J Oral Maxillofac Surg. 2009;67(2):394-401.
11. Ersoy AE, Turkyilmaz I, Ozan O, McGlumphy EA. Reliability of implant placement with stereolithographic surgical guides generated from computed tomography: clinical data from 94 implants. J Periodontol. 2008;79(8):1339-1345.
12. Noumbissi SS, Lozada JL, Boyne PJ, et al. Clinical, histologic, and histomorphometric evaluation of mineralized solvent-dehydrated bone allograft (Puros) in human maxillary sinus grafts. J Oral Implantol. 2005;31(4):171-179.
13. Schroder BK, Brown C. Use of selective open architecture in digital restoration fabrication. Compend Contin Educ Dent. 2010;31(spec issue 4):15-22.
14. Ogledzki M, Wenzel K, Doherty E, Kugel G. Accuracy of 3M-Brontes stereolithography models compared to plaster models. J Dent Res. 2010;89(spec issue A): Abstract 1060.
15. Poticny DJ, Fasbinder DJ. Accuracy of digital model articulation. J Dent Res. 2011;90(spec issue A): Abstract 131.
About the Author
Brian K. Schroder, DDS
Private Practice
San Antonio, Texas