Clinical Performance of Scientifically Designed, Hot Isostatic-Pressed (HIP’d) Zirconia Cores in a Bilayered All-Ceramic System
Abstract
PURPOSE: The success of bilayered all-ceramic restorations is dependent upon the combination and contributions of the three principal components of these restorations: core material, core design, and core-veneer interface. The purpose of this paper is to describe the fabrication and clinical survival of optimized ceramic restorations having an explicit, scientifically designed core, machined from HIP’d isotropic zirconia and veneered using a specific protocol with thermally compatible porcelain.
MATERIALS AND METHODS: Using a consistent clinical and laboratory protocol in a multicenter setting, 3,192 bilayered single and 797 bilayered splinted units were fabricated and placed on teeth and implant abutments in 1,007 patients. Approximately 61. 7% (n = 2,462) were posterior restorations and 38. 3% (n = 1,527) were anterior. Of the total, approximately 5. 7% (n = 227) were placed on implant abutments. Survival of the restorations was determined with the Kaplan-Meier (KM) method by tooth number.
RESULTS: For the 3,989 units placed, 9 failures were recorded. The KM survival of most zirconia restorations, when segregated by tooth number, was 100%. Exceptions were the 9 failed units, with a KM survival between 88% and 99% for those restorations. Six restorations failed within the first year of service, including three failed cores. Examination of those restorations revealed failure was related to initial design, quality assessment, or fabrication inconsistencies.
CONCLUSION: The incorporation of a reinforcing ring beam onto an anatomically shaped core made from end-state HIP’d zirconia, in partnership with a thermally compatible veneering porcelain and a specific application protocol, resulted in extremely high survival rates for both anterior and posterior all-ceramic restorations after medium-term clinical use. These results equal or surpass the equivalent-term success rates of porcelain-fused-to-metal restorations.
The transition to all-ceramic restorations from metal-ceramic restorations has disappointed many clinicians due to a high rate of failures. These include catastrophic failure of both monolithic materials and the alumina core material, and fracture and spalling (chipping) of porcelain from alumina as well as from the stronger zirconia cores.1-5 In addition, dimensional changes that occur in the anisotropic partially sintered materials during core production may affect the fit of these restorations, as secondary decay6 and loss of restoration retention7 have also been reported. In an effort to increase the success of bilayered systems, several core materials have been introduced, but core design has largely been ignored. It is accepted that in metal-ceramic systems the veneering porcelain must be supported,8 with the metal frame acting as a stress distributor9; yet many ceramic cores have been designed as nothing more than domed thimbles that fail to provide either occlusal or interproximal porcelain support. The stiff ceramic core must not only bear the forces of occlusion10,11 but also protect its axially layered porcelain. Clinical success and structural reliability of an all-ceramic restoration result primarily from the reliability of its core12,13; however, as in the metal-ceramic system, maintaining the integrity of the interface between core and porcelain is also a significant factor.14,15 Consequently, in construction of bilayered restorations, material composition as well as the design of the core must be carefully considered and then paired with a veneering porcelain having a thermal expansion coefficient (TEC) compatible with that of the core.
To address these problems, a unique design that strengthened the core itself while negating damaging interfacial tensile stresses on a thermally compatible veneering ceramic was conceived and tested in vivo. This design also protected that porcelain from the damage of shearing forces generated during occlusal function and created a more uniform thickness of the occlusal layer of veneering ceramic. In conjunction with the core material itself, the design also allowed for optimal esthetics of the finished restorations. All ceramic materials have porosities and flaws,16 either inherent or generated through processing, and exposure of these defects to tensile forces results in crack propagation and failure. Therefore, because of its dual-phase nature, superior mechanical properties, and distinctive transformative toughening effect that compresses cracks that may form, hot isostatic-pressed (HIP’d) yttrium-stabilized tetragonal zirconia polycrystals (Y-TZP) was chosen for the core material. Unlike the weaker alumina or monolithic materials, this is a 99. 99% porosity-free isotropic material, with physical properties that are identical in all planes. It is an end-state material that undergoes no dimensional changes during the production process of the core, thus providing better fitting accuracy of that core.17 Furthermore, it has high-fracture toughness, which is a quantitative way of expressing a material’s resistance to stress required to propagate a pre-existing flaw and the best indicator of a material’s clinical performance.18,19 Finally, the Food and Drug Administration has approved HIP’d zirconia for medical implantable devices, and the material does not exhibit the cytotoxic effects of the frequently used lithium disilicate materials.20-22
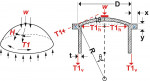
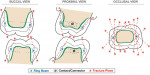
The geometry of dental crown-and-bridge cores generally consists of flat or slightly domed structures supported vertically at the edge by nearly cylindrical walls of undulating and uneven height. Typically, these cores have a 6° to 10° taper extending from the margins to the dome base. Structural theory suggests that in the design of the core, the principal stresses created in the dome, as a result of predominantly vertical forces, are developed along meridional and hoop curves around the dome23-25 as demonstrated in Figure 1. The meridional forces are compressive throughout the dome surface, and the hoop forces are in tension. Shearing forces are not present in either of these two principal directions. Concentrated forces applied to the dome top are transmitted downward, resulting in compression along any dome meridian. The equation for the meridional thrust—or force-per-unit length pushing radially outward, tangent to the dome surface and uniform around the entire circumference—is calculated as:
meridional thrust =

The value W equals the concentrated load on dome [N], D equals the diameter of core [mm], and θ equals the half included angle of dome. The meridional thrust can be broken into components: one in the vertical (y axis) direction and one each in the radial (x and z axes) directions (Figure 2). The equations that resolve the meridional thrust into these components are:
vertical component of meridional thrust =
horizontal component of meridional thrust =
The compressive meridional stress resulting from the meridional thrust is given by the equation:
The value t equals the thickness of core wall [mm].
Meridional stress is also equal to the stress contained in the cylindrical walls supporting the top dome structure. Because of the concentrated force on the dome surface, the circumferential/hoop component thrust, or force-per-unit length, is tensile throughout the core. The magnitude of the hoop thrust force is calculated using the equation:
circumferential or hoop thrust =
The corresponding tensile hoop stress resulting from the hoop thrust is calculated using the formula:
circumferential or hoop stress =
To reinforce the core, a ring beam can be incorporated in the design. This reduces tensile forces on the vertical walls while confining the occlusal forces to compressive forces on the dome surface. The ring beam is primarily subjected to the horizontal component of the meridional thrust (Figure 3). This thrust results in tension in the ring beam, and the hoop tension can be calculated using the equation:
hoop tension =
The hoop tension, when divided by the tensile strength of the ceramic, can be used to calculate the minimal cross-sectional area of the beam required:
ring beam cross-sectional area =
The value equals the tensile strength of the core material [MPa].
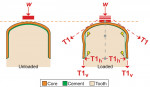
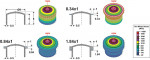
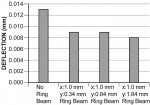
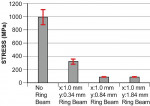
The most commonly reported problems for zirconia core restorations are spalling and fracture in the veneering ceramic.26-28 This has led many to investigate the bond of the layering porcelain to the zirconia core,29-33 yet Al-Dohan et al29 have demonstrated that the mean shear strength of porcelain to HIP’d Y-TZP is not statistically different than that of a metal-ceramic control. Furthermore, Quinn et al34 have shown no differences between veneered zirconia and metal-ceramic specimens in spalling susceptibility. Tensile forces within the core-veneering porcelain interface can, however, adversely affect the stability of that interface, and the problem may not lie with the bond of porcelain to core but with the formation of interfacial tensile stresses between the two materials. Figure 4 demonstrates a finite element analysis (FEA) of the effect of the maximal bite force of 1250N35 on a theoretically designed domed structure and the effect of ring size on the reduction of axial wall tensile stress. A ring of approximately 1 mm by 1-1.5 mm is able to absorb these forces (Figure 5 and Figure 6), maintaining the occlusal portion under compression, while the axial wall, even down to the marginal area, has a significant reduction in deflection and tensile stress.
In addition to compressive and tensile forces, porcelain on a typical ceramic core is also subject to direct shear forces along the axial walls. A ring beam also plays an additional role in that it interrupts these load paths—axial shearing forces that act to cleave the veneering porcelain off of the core sides36 (Figure 7). Guess et al37 have clearly demonstrated that shearing forces resulting from off-axis contact, without core support on the axial walls, result in premature fracture of the veneering porcelain. Coornaert et al38 also demonstrated that nonfunctional lateral excursive contacts on metal-ceramic restorations are the major causes of mechanical failures. These forces are resisted by the extended horizontal support of the core ring beam. The extended surface of the ring eliminates the typical broad convex axial planes subject to shearing, creating an axial concave cradle that protects the veneering porcelain. As a result, the direct shear area is only a small annulus of porcelain that is radially external to the outside diameter of the ring beam.
Vickery and Badinelli39 investigated the bond between metal and porcelain and determined that chemical bonding was responsible for approximately 50%, with mechanical retention and compression bonding equally sharing the remaining 50%. Likewise, Luthardt40 has implicated micromechanical interactions as one mode of bonding at the ceramic core-veneer interface. With a possible lack of chemical bond between zirconia and porcelain, tensile stresses must be reduced while mechanical retention and compression forces generated on the overlaying porcelain must be enhanced. Both anatomic contours and the ring itself increase the core surface area, thereby raising the potential for increased mechanical retention and strength. Although interfacial bonding from compressive forces is partially a function of core design and geometry, the differences in TEC between the core and veneering porcelain also appear to be important. To be effective, it is suggested that the core must have a slightly higher coefficient, approximately 1 x 10-6/°C or less,41,42 so that on cooling, compressive forces are generated uniformly on the veneer layer at the core-veneer interface. These forces are considered to strengthen bilayered systems32,43 and counteract the damaging tensile stresses and cone crack propagation from function that may cause porcelain chipping or failure.44 In addition to these compressive forces, it has also been demonstrated that a faster cooling of the porcelain after firing increases compressive forces on the veneer surface.45 In conjunction with the effect of the TEC mismatch these surface forces may act to significantly reduce chipping of the restoration veneer.46 Although there is ambiguity regarding the effects of cooling rates and the difference in thermal diffusivity between the zirconia core and veneering porcelain on the strength of this bond,15,47 more recent studies have also demonstrated that an increased cooling rate will increase global compressive forces on a restoration.15,32,48
The purpose of this study was to test the hypothesis that the survivability of anterior and posterior all-ceramic restorations could be enhanced through the combination of a new, scientifically designed core made from HIP’d Y-TZP and an appropriate thermally compatible veneering porcelain. A specific protocol for application of the porcelain was also developed, using a rapid cool down and the difference in TEC between zirconia and porcelain to increase the compressive forces on the restorations. The clinical procedures were performed by five dentists: three prosthodontists and two general practitioners. The cores were fabricated in the same core production center (Zircore Dental, www.zircore.net) with final restoration overlay porcelain applied in two in-house dental laboratories.
Materials and Methods
Beginning August 2004 and ending September 30, 2010, 1,007 patients were part of a case series study. The accrual period ended August 30, 2010; thus, the minimum follow-up was 1 month while the maximum follow-up was 74 months. The date of restoration failure was noted and considered to be an event for the time-to-event analysis. Failed restorations were considered complete observations if the date of failure was prior to the study end. Those patients who had been seen 1 year prior to the study end (and no failure) were given an additional 6 months and considered censored. The patients who had been seen less than 6 months prior to the study end (and no failure) or after the study end were also considered censored. Restoration survival was analyzed using the Kaplan-Meier methodology.
A total of 3,989 units were placed in 1,007 patients, restoring both anterior and posterior teeth. These were single-unit and multiple-unit restorations of up to 14 units and were placed on both teeth and dental implant abutments. The restorations were used in lieu of metal-ceramic crowns and fixed partial dentures (FPDs) and were employed in clinical situations in which metal-ceramic restorations would be deemed appropriate. Following a description and history of both metal and zirconia-supported restorations, patients were given the option to indicate their material of choice, with the understanding that any failed restoration would be remade at no cost to the patient. Adequate crown height and interocclusal distance were criteria for patient selection; however, age and gender were not. Patients with obvious parafunctional habits were also not excluded. Teeth with endodontic treatment had to have no signs of periapical pathology and appropriate post/core restoration where indicated. Patients were also required to have adequate oral hygiene and periodontal health, with minimal periodontal inflammation.
Teeth were prepared with 1-mm to 2-mm axial reduction and 1.5-mm to 2-mm occlusal or incisal reduction, leaving an axial wall height of at least 3 mm. In general, a chamfer finish line with marginal reduction of 0.5 mm to 1. 2 mm was used (Figure 8). In situations of excessive gingival recession requiring extended preparations, conservation of tooth structure dictated minimal marginal preparation, which was also similar to the preparation of implant abutments. All preparations were smoothed with sharp angles rounded. Filler material or crown buildups required to achieve classic preparation form were placed at the time of tooth preparation. A composite resin (FluoroCore®, Dentsply International, www.denstply.com) with dentin bonding agents was used. Impressions were taken conventionally using stock trays (Waterpik®, Water Pik, Inc., www.waterpik.com) and poured in a low-expansion Type IV die stone (ResinRock, Whip Mix, www.whipmix.com). In situations in which multiple units were to be splinted, a die system (DVA Precision Model System, Dental Ventures of America, Inc., www.dentalventures.com) was used to further model accuracy.
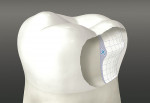
CAD/CAM technology was used in the core fabrication. All dies and, in some instances, opaqued titanium implant abutments were scanned (DCS PreciScan, DCS Dental AG), and the cores were created using design software (DCS DentForm, DCS Dental AG). The cores were then milled (DCS PreciMill, DCS Dental AG) from HIP’d Y-TZP blocks. A spindle speed of 40,000 rpm was used, with feed rates and cutting depths based on the cutting diamond size. The diamond cutting tools were 180 grit. All cores were designed with a minimum of 0.4-mm to 0.5-mm thickness on all surfaces and an organic external form replicating natural dentin geometries, and finished with a feathering of facial margins as indicated to enhance esthetics. A ring beam of 1 mm x 1-1.5 mm was added at the height of the interproximal contact area (Figure 9) to provide direct support for the porcelain overlay as well as strengthen the core. Connectors between units of anterior FPDs were designed with a minimal dimension of 9 mm2, and for posterior FPDs, 12 mm2. All had broadly curved gingival contours to reduce tensile stresses.49 Final finishing was performed using a high-speed handpiece with medium-grit diamonds and water spray or with slow-speed diamond impregnated discs (Bredent Turbo Grinder, Xpdent Corp., www.xpdent.com), using light, intermittent pressure. Minor occlusal or incisal edge adjustments necessary to facilitate core seating were accomplished on die models rather than by grinding on the internal surface of the cores. These changes were then reproduced on the prepared teeth. To enhance the adhesion of porcelain to the uncolored zirconia,33 the cores were lightly micro etched using 50-µm aluminum oxide at 40 psi from a distance of approximately 10 mm, and then steam-cleaned prior to the porcelain application. To replicate enamel thickness (anatomic contours), the cores were veneered with a porcelain (Cerabien ZR, Noritake Dental Supply Co., www.noritake-dental.co.jp) that has a TEC of 9. 1 x 10-6/°C, which is specifically designed for zirconia (TEC of 10 x 10-6/°C). The first coat applied to the cores was a thin wash mix of fine grain opacious dentin porcelain of the appropriate shade. This was used to modify the high value and augment the esthetic qualities of the opalescent core material and to also take advantage of the enhanced bonding capabilities of fine grain ceramics. Opaque or shade base layers were not applied to the cores. All subsequent layers of the fine grain porcelain were applied in thin layers to further minimize tensile stress formation on the veneer surface.50 The porcelain was judiciously condensed, and the crowns were fired 10ºC below the manufacturer’s recommended high temperature, while using the suggested heat rate time. On completion of the firing, the crowns were brought directly from the muffle and allowed to bench cool. This procedure was repeated for all subsequent firing cycles, dropping the high temperature 5ºC with each firing. The final glaze cycle temperature was then raised to that of the first bake, and after firing, the crowns were allowed to bench cool as on previous bakes.
Prior to cementation, the internal surfaces of restorations were again lightly micro etched and cleaned. Prepared tooth surfaces were cleaned of temporary cement residue (TempBond®, Kerr Dental, www.kerrdental.com) by pumice and water. Resin-modified glass ionomer (RMGI) cement (GC Fuji PLUS, GC America Inc., www.gcamerica.com) was used as the final cement following the manufacturer’s recommendations. Restorations on implant abutments were seated either using the RMGI cement or cements that allowed retrievability: TempBond, or petrolatum-modified Durelon® (3M ESPE, www.3MESPE.com). Post-cementation occlusal contacts on all restorations were carefully verified and refined where necessary, with particular attention given to preventing excursive contacts of the posterior restorations. Protrusive excursion contacts were adjusted for optimal force distribution. Areas of final intraoral adjustment were carefully polished using a porcelain polishing system (Ceramisté®, Shofu Dental Corp., www.shofu.com).
After treatment completion, patients were recalled for periodontal and restoration evaluation at least every 12 months and most at 6-month intervals. Restorations were evaluated for core failure and/or fracture or chipping of the veneering porcelain. A restoration was considered a failure if it exhibited a fractured core or porcelain fracture that required either the remake of the restoration or a bonded repair. A porcelain chip, which was defined as less than 1 mm, was polished and the restoration was not considered a failure. Marginal integrity was verified by tactile examinations with a dental explorer and radiographs when indicated.
Results
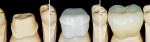
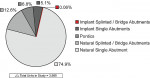
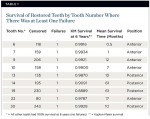
Of 3,989 units placed, three units failed through core fracture, with six units demonstrating fracture of the layering porcelain. Porcelain chips were few, and delamination did not occur with any restoration. This yielded an overall frequency of failure of 2.25 units per 1,000, or a relative success rate of 99.998%. Most failed units resulted within the first year of service. Restorations were placed on natural teeth and dental implants, both as single units or part of multiple-unit restorations (Figure 10). The distribution by location was approximately 61.7% in posterior segments (n = 2,462) and 38. 3% in anterior segments (n = 1,527) (Figure 11). A total of 198 restorations, comprising 797 units, consisted of splinted multiple units, from two to 14 units (Figure 12). Since the total numbers of units were correlated within the patients, the overall Kaplan-Meier survival could not be reported for the total 3,989 units. The Kaplan-Meier was reported and illustrated only for the failed units since all the others had a 100% survival (no failure of the restoration). The results for teeth with a failed restoration were analyzed by tooth number, thereby eliminating the correlation of multiple units per patient (Table 1). Kaplan-Meier survival plots are illustrated for all teeth Nos. 19 (Figure 13) and 22 (Figure 14).
The health of the periodontal tissues remained constant or improved throughout the study, and no instances of secondary decay were noted. There were also no instances of loss of retention of any FPD or the need for endodontic therapy for any of the restored teeth.
Discussion
In this study, the theoretical advantages of ring-beam reinforced HIP’d Y-TZP cores in conjunction with TEC-compatible porcelain were tested in vivo. The survival rates of the all-ceramic restorations at this stage are high, comparing favorably with the results of metal-ceramic restorations over the same period.38 Although core failures are not encountered with metal-ceramic crowns, three cores failed during this study. The primary complication reported for zirconia-based restorations is chipping or fracture of the veneering porcelain; however, secondary caries have also been reported5,6,51 as well as loss of retention of FPDs.7 With regard to these complications, the results of this study are also encouraging. Occlusal parafunction was not a consideration or contraindication to patient selection for these restorations; however, a limitation of this study could be that age and gender of the patients were not collected, and they could be confounders in the Kaplan-Meier survival estimation.
In restorations having veneers with a low modulus of elasticity on cores with a high modulus, load from occlusal forces is transferred to the stiffer core layer, increasing tension in the core and suppressing it in the veneer.10,11,15 Consequently, the design of the core plays an important role in the success of the final restoration. FEA analysis indicates that by placing a reinforcing cross-section ring beam at the intersection of the occlusal surface and the vertical sides, tensile forces are reduced to only an annular area at the height of the ring beam—radially outside the ring—and are in a plane at approximately 90° to the applied bite forces. This beam, which is located at the area of highest tensile stress (ie, hoop) in a dome-shaped ceramic core,52 not only reduces tensile stress within the core walls but also significantly reduces the stresses described by Coelho et al53 at crown margins. These stresses have been implicated in the formation of semi-lunar fractures that have been a significant cause of failure in both monolithic and alumina core crowns.
The geometry of both core and final restoration plays an essential role in fracture initiation and crack propagation in the veneer of all-ceramic restorations.54 Porcelain with uniform thickness is most resistant to spalling and fracture. Organic (anatomic) shaping of the core, which provides for a uniform thickness, also results in superior support of porcelain cusps. Sundh and Sjögren55 have demonstrated that the loads required to fracture crowns built with anatomic support are significantly higher than those needed to fracture crowns with minimally shaped cores and porcelain with significantly uneven thickness. Molin and Karlsson56 also demonstrated no chipping or debonding of veneering porcelain when using anatomically designed HIP’d Y-TZP as the core material.
Spalling or fracture of the porcelain from the core was an insignificant problem in this study. The veneering protocol consisted of the application of thin layers of porcelain and a rapid cooling after firing. This is in contrast to the current practice of a “slow cool” after firing, which is used as an attempt to negate the mismatch of thermal diffusivity between zirconia and porcelain. This process is thought to be necessary to allow the core and veneer to cool from the firing temperature at a more uniform rate. However, the interaction of zirconia and porcelain during veneering requires much more investigation as several principles of thermodynamic behavior are relevant to this system. For example, the temperature of the ceramic crown is determined by convective heat transfer. The equation for this is q = ΔT/(h*A), where q is the heat transfer, ΔT is the change in temperature, h is the convective heat transfer coefficient (which is different for both materials), and A is the surface area. The surface area of the core is also not the same as that of the porcelain. Veneering also involves the transfer of heat from porcelain to zirconia through internal conduction between the layers, which is expressed as q = k(T1-T2) where k is the coefficient of thermal conductivity of the materials and T1-T2 are the temperatures at either boundary. Thus, the assumption that the core and veneer absorb the same amount of energy (heat) while in the furnace is erroneous. The energy absorbed is directly related to the k of the material. For the same temperature of furnace and the same amount of time, the temperature difference is the ratio of the respective k values. The actual net effect of slow cooling is an annealing of the porcelain as it cools. This eliminates the possibility of surface compressive force formation, which has been shown to strengthen the restoration. The slow cool process may in fact be detrimental as it acts to add more heat to the system. The more heat the restoration absorbs, the greater the potential for the induction of thermal strains and possibly even phase changes within the zirconia itself.
An important yet frequently overlooked factor in the success of any all-ceramic restoration is the occlusal design. In bilayered systems vertical forces on the occlusal surface may generate outer and inner cone cracks in the veneer, which can spread to the veneer-core interface57 yet do not cause porcelain failure. During occlusal function and off-axis loading, these cracks may form on cusp inclines and can result in chipping or failure of this porcelain. Anatomically shaped cores that provide lateral support can reduce this problem; however, the presence of off-axis posterior tooth-to-tooth contacts are an occlusion design oversight. An occlusal scheme that is designed to negate or minimize lateral excursive off-axis contact on these teeth and careful occlusal refinement and polishing are most effective in reducing these stresses on the porcelain.58-60 Monolithic lithium disilicate crowns with a recommended minimal thickness of 2 mm and steep cuspal inclines have been suggested as an alternative approach to avoid this problem, yet bulk (radial) fracture still remains a concern with these materials.57 It is also imperative that the manufacturer’s recommended thickness of 2 mm or greater be maintained, as only a 25% reduction of this dimension reduces the material’s resistance to fracture by 50%.26 In addition to steep cuspal anatomy not fitting into the occlusal schemes of many patients, these restorations may exhibit compromised esthetics and imprecise contours, and porcelain added to correct these deficiencies lacks the global compressive forces generated by a full-coverage veneer. Recently introduced monolithic zirconia crowns do not demonstrate the weakness of the earlier lithium disilicate crowns; however, the esthetics of these crowns are only comparable to the porcelain-fused-to-metal (PFM) crowns they have replaced.
The biologic response to the restorations in this study was also encouraging. Secondary decay was not detected using the isotropic end-state material, whereas Sailer et al6 reported a 21.7% incidence of secondary caries after 5 years in restorations using anisotropic intermediate-state material for the cores. This problem, as well as loss of retention, may be attributed to the compromised fit and large cement gap,7 which can result when using the intermediate-state material.17 Zirconia has also demonstrated a favorable response by gingival tissues in an in vitro study by Raffaelli et al,61 and this response was reflected in the present study.
Conclusion
The performance of all-ceramic bilayered restorations is determined by a significant number of complex factors, many involving the interactions of the core material, core design, and core-veneer interface. The porcelain failures encountered in this study were determined to be the result of core design and fabrication errors that occurred during the initial refinement of the dimension and clinical application of the ring beam. As a result of this finding, and the final study results, the hypothesis of this study was accepted. An appropriately designed ring beam on a HIP’d zirconia core improves restoration predictability through enhanced protection of the porcelain veneer from occlusal shear forces while significantly reducing damaging tensile stress at the core-veneer interface. Examination of the fractured cores revealed a failure to maintain the 0.4-mm to 0.5-mm thickness required for strength, thereby resulting in their failure. The reliability and function of the core is most important in these restorations, and adequate material dimension must be maintained. However, in conjunction with a reinforced core that reduces tensile stresses, the veneering porcelain itself and its application protocol also significantly contribute to an enhanced core-veneer interface, a stronger restoration, and improved restoration success.
About the Authors
Bernard E. Keough, DMD
Private Practice
Limited to Prosthetic Dentistry
West Palm Beach, Florida
Howard B. Kay, DDS
Private Practice
Limited to Prosthetic Dentistry
West Palm Beach, Florida
R. David Sager, DMD
Private Practice
Hospital/General Dentistry
Manhattan, Kansas
Eric Keen, PE
Licensed Professional Engineer
Manhattan, Kansas
References
1. Taskonak B, Sertgöz A. Two year clinical evaluation of lithia-disilicate-based all-ceramic crowns and fixed partial dentures. Dent Mater. 2006;22(11):1008-1013.
2. Esquivel-Upshaw JF, Young H, Jones J, et al. Four-year clinical performance of a lithia disilicate-based core ceramic for posterior fixed partial dentures. Int J Prosthodont. 2008;21(2):155-160.
3. McLaren EA, White SN. Survival of In-Ceram crowns in a private practice: a prospective clinical trial. J Prosthet Dent. 2000;83(2):216-222.
4. Bindl A, Mörmann WH. An up to 5-year clinical evaluation of posterior In-Ceram CAD/CAM core crowns. Int J Prosthodont. 2002;15(5):451-456.
5. Raigrodski AJ, Chiche GJ, Potiket N, et al. The efficacy of posterior three-unit zirconium-oxide-based ceramic fixed partial dental prostheses: a prospective clinical pilot study. J Prosthet Dent. 2006;96(4):237-244.
6. Sailer I, Fehér A, Filser F, et al. Five-year clinical results of zirconia frameworks for posterior fixed partial dentures. Int J Prosthodont. 2007;20(4):383-388.
7. Roediger M, Gersdorff N, Huels A, Rinke S. Prospective evaluation of zirconia posterior fixed partial dentures: four-year clinical results. Int J Prosthodont. 2010;23:141-148.
8. Warpeha WS Jr, Goodkind RJ. Design and technique variables affecting fracture resistance of metal-ceramic restorations. J Prosthet Dent. 1976;35(3):291-298.
9. Nally JN, Farah JW, Craig RG. Experimental stress analysis of dental restorations. Part IX. Two-dimensional photoelastic stress analysis of porcelain bonded to gold crowns. J Prosthet Dent. 1971;25(3):307-316.
10. Miranda P, Pajares A, Guiberteau F, et al. Contact fracture of brittle bilayer coatings on soft substrates. J Mater Res. 2001;16(1):115-126.
11. Rudas M, Qasim T, Bush M, Lawn BR. Failure of curved brittle layer systems from radial cracking in concentrated surface loading. J Mater Res. 2005;20(10):2812-2819.
12. Bona AD, Anusavice KJ, DeHoff PH. Weibull analysis and flexural strength of hot-pressed core and veneered ceramic structures. Dent Mater. 2003;19(7):662-669.
13. Lawn BR, Pajares A, Zhang Y, et al. Materials design in the performance of all-ceramic crowns. Biomaterials. 2004;25(14):2885-2892.
14. Sundh A, Sjögren G. Fracture resistance of all-ceramic zirconia bridges with differing phase stabilizers and quality of sintering. Dent Mater. 2006;22(8):778-784.
15. Studart AR, Filser F, Kocher P, et al. Mechanical and fracture behavior of veneer-framework composites for all-ceramic dental bridges. Dent Mater. 2007;23(1):115-123.
16. Kelly JR, Nishimura I, Campbell SD. Ceramics in dentistry: historical roots and current perspectives. J Prosthet Dent. 1996;75(1):18-32.
17. Kohorst P, Brinkmann H, Li J, et al. Marginal accuracy of four-unit zirconia fixed dental prostheses fabricated using different computer-aided design/computer-aided manufacturing systems. Eur J Oral Sci. 2009;117(3):319-325.
18. Evans AG. Perspective on the development of high-toughness ceramics. J Am Ceram Soc. 1990;73(2):187-206.
19. Fischer H, Marx R. Fracture toughness of dental ceramics: comparison of bending and indentation method. Dent Mater. 2002;18(1):12-19.
20. Brackett MG, Lockwood PE, Messer RL, et al. In vitro cytotoxic response to lithium disilicate dental ceramics. Dent Mater. 2008;24(4):450-456.
21. Ozen J, Sipahi C, Çağlar A. The effect of aged dental ceramics on gingival cell viability. Hacettepe Dişhekimliği Fakültesi Dergisi. 2006;30(3):102-107.
22. Messer RL, Lockwood PE, Wataha JC, et al. In vitro cytotoxicity of traditional versus contemporary dental ceramics. J Prosthet Dent. 2003;90(5):452-458.
23. Farshad M. Design and Analysis of Shell Structures. The Netherlands: Kluwer Academic; 1992:168-192.
24. Bangash MYH, Bangash T. Elements of Spatial Structures: Analysis and Design. London, England: Thomas Telford; 2003:243-387.
25. Ventsel E, Krauthammer T. Thin Plates and Shells: Theory, Analysis, and Applications. New York, NY: Marcel Dekker; 2001:373-410.
26. Thompson VP, Rekow ED. Dental ceramics and the molar crown testing ground. J Appl Oral Sci. 2004;12(spe):26-36.
27. Rekow ED, Zhang Y, Thompson V. Can material properties predict survival of all-ceramic posterior crowns? Compend Contin Educ Dent. 2007;28(7):362-369.
28. Aboushelib MN, de Jager N, Kleverlaan CJ, Feilzer AJ. Effect of loading method on the fracture mechanics of two layered all-ceramic restorative systems. Dent Mater. 2007;23(8):952-959.
29. Al-Dohan HM, Yaman P, Dennison JB, et al. Shear strength of core-veneer interface in bi-layered ceramics. J Prosthet Dent. 2004;91(4):349-355.
30. Aboushelib MN, de Jager N, Kleverlaan CJ, Feilzer AJ. Microtensile bond strength of different components of core veneered all-ceramic restorations. Dent Mater. 2005;21(10):984-991.
31. Tholey MJ, Swain MV, Thiel N. SEM observations of porcelain Y-TZP interface. Dent Mater. 2009;25(7):857-862.
32. Taskonak B, Borges GA, Mecholsky JJ, et al. The effects of viscoelastic parameters on residual stress development in a zirconia/glass bilayer dental ceramic. Dent Mater. 2008;24(9):1149-1155.
33. Aboushelib MN, Kleverlaan CJ, Feilzer AJ. Effect of zirconia type on its bond strength with different veneer ceramics. J Prosthodont. 2008;17(5):401-408.
34. Quinn JB, Sundar V, Parry EE, Quinn GD. Comparison of edge chipping resistance of PFM and veneered zirconia specimens. Dent Mater. 2010;26(1):13-20.
35. Gibbs CH, Mahan PE, Lundeen HC, et al. Occlusal forces during chewing and swallowing as measured by sound transmission. J Prosthet Dent. 1981;46(4):443-449.
36. Tinschert J, Schulze KA, Natt G, et al. Clinical behavior of zirconia-based fixed partial dentures made of DC-Zirkon: 3-year results. Int J Prosthodont. 2008;21(3):217-222.
37. Guess PC, Zavanelli RA, Silva N, et al. Monolithic CAD/CAM lithium disilicate versus veneered Y-TZP crowns: comparison of failure modes and reliability after fatigue. Int J Prosthodont. 2010;23(5):434-442.
38. Coornaert J, Adriaens P, de Boever J. Long-term clinical study of porcelain-fused-to-gold restorations. J Prosthet Dent. 1984;51(3):338-343.
39. Vickery RC, Badinelli LA. Nature of attachment forces in porcelain-gold systems. J Dent Res. 1968;47(5):683-689.
40. Luthardt RG, Sandkuhl O, Reitz B. Zirconia-TZP and alumina—advanced technologies for the manufacturing of single crowns. Eur J Prosthodont Restor Dent. 1999;7(4):113-119.
41. Yamamoto M. Metal-Ceramics: Principle and Methods of Makoto Yamamoto. Chicago, IL: Quintessence Publishing; 1985:160-188.
42. DeHoff PH, Anusavice KJ. Viscoelastic finite element stress analysis of the thermal compatibility of dental bilayer ceramic systems. Int J Prosthodont. 2009;22(1):56-61.
43. Tinschert J, Natt G, Mautsch W, et al. Fracture resistance of lithium disilicate-, alumina-, and zirconia-based three-unit fixed partial dentures: a laboratory study. Int J Prosthodont. 2001;14(3):231-238.
44. Kim B, Zhang Y, Pines M, Thompson VP. Fracture of porcelain-veneered structures in fatigue. J Dent Res. 2007;86(2):142-146.
45. DeHoff PH, Anusavice KJ. Analysis of tempering stresses in bilayered porcelain discs. J Dent Res. 1992;71(5):1139-1144.
46. Anusavice KJ, DeHoff PH, Hojjatie B, Gray A. Influence of tempering and contraction mismatch on crack development in ceramic surfaces. J Dent Res. 1989;68(7):1182-1187.
47. Guazzato M, Walton TR, Franklin W, et al. Influence of thickness and cooling rate on development of spontaneous cracks in porcelain/zirconia structures. Aust Dent J. 2010;55(3):306-10.
48. Göstmeyer G, Jandras M, Dittmer MP, et al. Influence of cooling rate on zirconia/veneer interfacial adhesion. Acta Biomater. 2010;6(12):4532-4538.
49. Oh W, Götzen N, Anusavice KJ. Influence of connector design on fracture probability of ceramic fixed-partial dentures. J Dent Res. 2002;81(9):623-627.
50. Swain MV. Unstable cracking (chipping) of veneering porcelain on all-ceramic dental crowns and fixed partial dentures. Acta Biomater. 2009;5:1668-1677.
51. Schmitt J, Holst S, Wichmann M, et al. Zirconia posterior fixed partial dentures: a prospective clinical 3-year follow-up. Int J Prosthodont. 2009;22(6):597-603.
52. Qasim T, Ford C, Bush MB, et al. Margin failures in brittle dome structures: relevance to failure of dental crowns. J Biomed Mater Res Part B Appl Biomater. 2007;80(1):78-85.
53. Coelho PG, Silva NR, Thompson VP, et al. Effect of proximal wall height on all-ceramic crown core stress distribution: a finite element analysis study. Int J Prosthodont. 2009;22(1):78-86.
54. Rekow ED, Zhang G, Thompson V, et al. Effects of geometry on fracture initiation and propagation in all-ceramic crowns. J Biomed Mater Res Part B Appl Biomater. 2009;88(2):436-446.
55. Sundh A, Sjögren G. A comparison of fracture strength of yttrium-oxide-partially-stabilized zirconia ceramic crowns with varying core thickness, shapes and veneer ceramics. J Oral Rehabil. 2004;31(7):682-688.
56. Molin MK, Karlsson SL. Five-year clinical prospective evaluation of zirconia-based Denzir 3-unit FPDs. Int J Prosthodont. 2008;21(3):223-227.
57. Kim JH, Kim JW, Myoung SW, et al. Damage maps for layered ceramics under simulated mastication. J Dent Res. 2008;87(7):671-675.
58. McLean JW. The Science and Art of Dental Ceramics. Volume II: Bridge Design and Laboratory Procedures in Dental Ceramics. Chicago, IL: Quintessence Publishing; 1980:415.
59. Keough BE. Occlusion-based treatment planning for complex dental restorations: part 2. Int J Periodontics Restorative Dent. 2003;23(4):325-335.
60. Rafferty BT, Janal MN, Zavanelli RA, et al. Design features of a three-dimensional molar crown and related maximum principal stress. A finite element model study. Dent Mater. 2010;26(2):156-163.
61. Raffaelli L, Rossi Iommetti P, Piccioni E, et al. Growth, viability, adhesion potential, and fibronectin expression in fibroblasts cultured on zirconia or feldspathic ceramics in vitro. J Biomed Mater Res. 2008;86(4):959-968.