Orthodontic and Prosthetic Treatment of a Patient with Cystic Fibrosis and Agenesis of Maxillary Lateral Incisors
Harold Slutsky, DMD; and Joseph R. Greenberg, DMD
Abstract
The young dental patient with maxillary lateral incisor agenesis, maxillary canine impaction, and cystic fibrosis presents considerable challenges to the dentist. An interdisciplinary approach is described here for the orthodontist and restorative dentist to plan and work together with the patient’s and parents’ cooperation and consent. Despite some compromises, a successful outcome was achieved, as demonstrated in this case report. The use of conservative yet esthetic and durable fixed replacement prostheses is highlighted. Congenitally absent maxillary lateral incisors, impacted maxillary canines, and cystic fibrosis are clinical conditions that can significantly complicate and compromise dental treatment for any young patient. All three can be present simultaneously, as described in this case report.
Cystic fibrosis is an autosomal recessive disease of the exocrine glands occurring with equal prevalence in males and females.1 It appears in approximately 1 in 3,000 Caucasians and 1 in 17,000 African Americans but rarely in Asians. Seventy years ago, most patients died in infancy or early childhood. Now, the median life expectancy exceeds 37 years.2-4 Changes to the mucus glands of the pulmonary and digestive systems may lead to unusually high sodium levels in perspiration, malabsorption of fat-soluble vitamins A, D, E, and K, and abnormally viscous mucus.4 This mucus can lead to a nonproductive cough, acute respiratory infection, bronchopneumonia, bronchiectasis, and lung abscesses.1 Patients with cystic fibrosis typically display digestive symptoms, as well. An estimated 85% to 90% of infants with the disease develop pancreatic insufficiency, with typical signs of greasy stools, flatulence, abdominal bloating, and inability to gain weight.4 Treatment may involve nutritional and pancreatic enzyme supplementation, antibiotics, inhaled aerosols, steroids, and lung transplantation for end-stage lung disease.5,6
It has been reported in the literature that maxillary canine impaction is twice as common in females as in males, occurs in approximately 2% of the population, and is twice as likely to appear in the maxilla as in the mandible.7-10 Except for third molars, maxillary canines are the most commonly impacted teeth.11,12 Unerupted canines may cause root resorption of lateral incisors and damage adjacent roots.13 Multiple exposure techniques are available, each with distinct benefits and indications. While labial impactions may need gingivectomies, apically positioned flaps, or closed eruption (exposure of a tooth and recovering with soft tissue14), palatal impactions may require closed flaps or open eruptions.10 Preservation of attached gingiva is critical on labial exposures for enhanced long-term canine root health.
The young patient with agenesis of permanent lateral incisor teeth often presents a challenge to the orthodontist and restorative dentist. This is an autosomal dominant trait and occurs in 2% of the population. The problem is twice as common in females, and nearly two-thirds of those individuals have both lateral incisors missing. In half of patients with one lateral missing, the contralateral tooth is deficient or peg shaped.15 The patient and his/her family should have a preliminary tooth replacement discussion prior to beginning orthodontic treatment when tooth replacement is desired and when the existing tooth position does not support the chosen plan. Then, the challenge for the orthodontist is to manipulate the patient’s tooth position and accompanying alveolus to best support the final tooth replacement scheme. The challenge for the restorative dentist is to satisfy the esthetic and functional needs of the patient and deliver a restorative service with reasonable longevity in accordance with expectations. The tooth replacement restoration should contribute to the retention of the final tooth position and offer therapeutic occlusal function and stability. Kinzer and Kokich16 described three options for replacing missing maxillary lateral incisors: canine substitution, a tooth-supported restoration, and single-tooth implants.
Sharma and Vargevik report that for children missing a single permanent tooth with adjacent permanent teeth, the skeletal development is a more important consideration than chronological age. They recommend avoiding implant placement until two annual cephalograms show no change in the position of the adjacent teeth and alveolus. The concern here is the dentoalveolar development adjacent to the edentulous space. With growth, there is downward and forward development of the alveolus in the maxilla and a height increase of the alveolus in the mandible. If an implant is placed before dentoalveolar growth is complete, the implant will become submerged relative to the adjacent teeth.17
Implants placed in growing jaws do not change position over time and do not improve vertical alveolar development.18 Various studies note alveolar development is deficient when teeth are congenitally absent, lateral incisor implant restorations are esthetically challenging, and facial development, continuous eruption, and mesial drift of natural teeth are compromising factors.19,20 Zachrisson21 has reported all implant-supported crowns in the esthetic zone are subject to darkening of the overlying labial gingiva, progressive infraocclusion of the crown (even in mature adults), and gingival retraction.
Fear, financial constraints, and other medical conditions can add complexity to the treatment-planning discussion. Whenever a combination of factors compromises treatment, all issues should be presented to the patient and/or parents before any therapy begins.22 Despite the popularity of dental implants, not every patient is a candidate. At the case presentation, providers must put forth solid treatment alternatives along with the associated complications and compromises.
Case Report
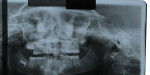
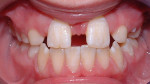
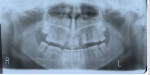
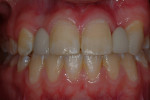
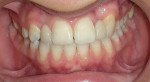
On presentation in December 2002, the patient was an 8.1-year-old female with cystic fibrosis and a midfacial deficiency. She had a Class I malocclusion resembling a Class III. Maxillary central incisors, deciduous maxillary lateral incisors, deciduous maxillary canines, and deciduous maxillary left first and second molars were in the cross-bite position. In addition, the patient had stained teeth with an idiopathic etiology (Figure 1). The authors spoke with the patient’s father, who did not know why her teeth were stained. The authors did not believe the stain was caused by cystic fibrosis and noted this was a surface stain, which was easily polished off. A panoramic x-ray from May 2002 revealed agenesis of the maxillary lateral incisors and mandibular right second premolar, as well as possible impaction of the maxillary canines, most notably the maxillary left canine (Figure 2).
The Phase I treatment plan needed to address the correction of the anterior cross bite. With good compliance, a posterior bite plate with finger springs is highly effective and relatively inexpensive for moving the maxillary incisors out of cross bite. If this is unsuccessful, then fixed appliances could be placed to rectify the anterior cross bite. Therefore, Phase I orthodontic treatment consisted of a posterior bite plate with finger springs engaging the maxillary central incisors to correct the anterior cross bite. The deciduous maxillary lateral incisors were extracted to ensure eruptive clearance for the permanent maxillary central incisors. The maxillary and mandibular right first molars erupted into a posterior cross-bite position, so cross elastics were worn for several months to correct this.
Several treatment plans were available for Phase II. The patient and her parents were seeking the most esthetic, noninvasive tooth replacement alternative that would also provide “reasonable longevity,” in that order. “Reasonable longevity” for them was 8 to 10 years. Possible treatment plans typically include canine substitution (moving maxillary canines into the position of maxillary laterals), dental implants to replace maxillary lateral incisors, Maryland bridges, or porcelain-fused-to-metal (PFM) resin-bonded bridges. Canine substitution was ruled out because it would decrease the breadth of the smile and significantly prolong treatment time—to move all maxillary posterior teeth mesially when erupted would greatly increase treatment time and the risk of potential iatrogenic root blunting. Another reason for eliminating this option was that it would compromise the cosmetics of the canines because the position of the lateral incisors would not provide balanced esthetics. Placement of dental implants was rejected in view of the patient’s age, the proposed need for multiple surgeries (eg, hard- and soft-tissue ridge augmentation), and the impact on biologic and mental stress, as well as increasing total treatment time. Of the various conservative tooth replacement options, the etched PFM resin-bonded prosthesis23 seemed to offer the best option for the following reasons:
- Esthetic superiority: no postinsertion metal shadows
- Conservative approach: little-to-no tooth preparation required
- Proven materials: precious metals, PFM technology
- Bond reliability: etched porcelain to enamel bonding
- Reported longevity: 8 to 16 years24
Phase II Treatment
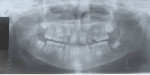
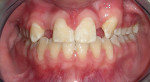
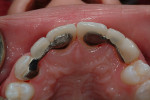
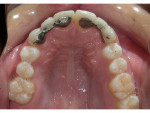
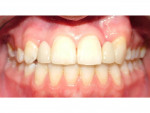
Phase II treatment was intentionally delayed until April 2006 when the patient was 11.5 years old. At this time, she had adequate eruption and root development whereby fixed appliances would not be worn for an extended period. She no longer displayed any anterior or posterior cross bite; however, she had a large maxillary diastema, mostly because she was missing the maxillary lateral incisors (Figure 3). In this stage, the panoramic x-ray showed agenesis of the maxillary lateral incisors and mandibular right second premolar, anatomically foreshortened roots of the maxillary central incisors, impaction of the maxillary left canine, and retarded root development of the mandibular left second premolar (Figure 4). Phase II began with an upper 2x2 braces on maxillary first molars and central incisors to de-rotate the maxillary right first molar. Then, full-arch fixed appliances were employed in order to accommodate further tooth eruption. The maxillary left canine was surgically exposed early in the treatment process and had taken approximately 18 months to be brought to the dental arch (Figure 5). The patient wore Class II elastics on the left side to pull the canine into position; however, this tooth never achieved the desired complete Class I relationship. In April 2009, debanding was performed after 37 months of treatment (Figure 6). For retention, she was given a fixed bonded lingual retainer on the six mandibular anterior teeth and a maxillary Hawley retainer with pontics for the maxillary lateral incisors to hold the spaces and provide temporary cosmetics until the restorative dentist could place the fixed replacement prostheses. In addition, a labial bow was used to help with retention and enable placement of gentle, lingually directed forces if needed.25 Finger springs were distal to the maxillary central incisors and mesial to the maxillary canines to allow gentle mesiodistal movement of teeth if required (Figure 7).
Before debanding, treatment was carefully coordinated with the restorative dentist. There was concern that the patient would have difficulty wearing a long-term removable retainer due to the coughing and breathing problems associated with cystic fibrosis. In addition, because of the agenesis of the maxillary lateral incisors, there was inadequate alveolar development and, thus, insufficient dimensions for dental implants without soft- and hard-tissue ridge augmentation. The patient’s age and related growth and development were also at issue.19 The final panoramic x-ray showed agenesis of the mandibular third molars and maxillary right third molar in addition to agenesis of the maxillary lateral incisors and the mandibular right second premolar. Also, there was root blunting of the maxillary central incisors, which also existed on pretreatment x-rays (Figure 8).
Etched PFM resin-bonded bridges were chosen as long-term restorations. This design features the use of precious metals, PFM technology, and the bonding of etched porcelain to tooth surfaces.26 It is a modification of the Maryland bridge24 and requires only minor conservative tooth preparation within the enamel. Unlike with the Maryland bridge, postcementation dark incisal shadows and frequent debondings have not been observed.23
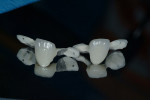
Strength was provided by a cast precious metal framework. Because some interincisal space would be desirable for the metal framework of the bonded bridges, the orthodontist engineered a 1-mm space between the lingual surfaces of the maxillary central incisors and labial incisal edges of the mandibular central incisors (Figure 9). The intaglio surfaces of the abutment wings were porcelain-fused to the underlying metal frame and etched and bonded to the tooth enamel on the lingual aspects of the abutment teeth. Figure 10 shows the two etched PFM resin-bonded bridges prior to cementation. The cementation process included acid-etching and application of an enamel/dentin primer to the tooth surfaces, hydrofluoric acid-etching/cleansing/silane application to the intaglio surfaces of both bridges, and cementation with a self-curing all-resin system. The cemented bridges are shown in Figure 11. The patient was concerned about a “shiny metal display” behind her front teeth when she smiled or threw her head back. So all metal surfaces were sandblasted prior to insertion.
The restorative dentist requested that the maxillary midline be finished to the patient’s facial midline, which was 1 mm right of the mandibular midline.27 The plan also called for the restorative dentist to add direct-bonded composite resin to the left canine and perform enameloplasty to shorten and reshape the right canine to create a visually acceptable match. The patient practiced dentist-supervised customized mouthguard whitening of her natural teeth28 nightly for 3 weeks. A 16% carbamide peroxide gel in a vacuum-formed customized mouthguard was used. The whitening process was initiated after final placement of the bridgework so that the patient would have a fitting appliance for touch-up whitening in later years. This required an estimate of a final shade for the bridge pontics before the whitening process began (Figure 12).
When the patient presented several weeks later, a 0.5-mm diastema had opened between the maxillary central incisors (Figure 13 and Figure 14). The restorative dentist re-equilibrated the lingual aspects of the restorations and adjacent tooth structure, and the orthodontist placed a wrap-around Hawley retainer appliance. The acrylic was relieved lingual to the maxillary central incisors, and the Hawley wire was positively set on the maxillary central incisors to place gentle lingually directed forces (Figure 15). The Hawley appliance successfully closed the diastema, and the restorative dentist placed a conservative intracoronal-bonded retaining splint across adjacent mesial surfaces of the lingual aspects of the maxillary central incisors. A gold pin was set into a bed of acid-etched composite resin with the Hawley appliance in place for consistent stability. Then, all centric, lateral, and protrusive occlusal markings on the maxillary incisors were diminished to light contact. The patient was concerned with the open appearance of the incisal embrasure, so this was partially closed with the labial aspect of the splint (Figure 16 and Figure 17). The patient and parents were pleased with the final result.
Conclusion
Each patient has unique needs and desires. Experts have recently confirmed that the patient’s expectations are primary when formulating an esthetic dental treatment plan.29 Flores-Mir et al30 assert the patient places the most importance on the full-face smiling view. The authors in the present study presented an interdisciplinary dental treatment for a young female with numerous genetic dental challenges and significant health issues. The treatment was rendered in as a conservative, noninvasive manner as possible and yet still met the stated objectives. During treatment, the patient and her parents were informed of the various compromises. They were actively involved in the decision-making process and were pleased with the results.
The author has found the etched PFM resin-bonded bridge to be a reliable restoration with an approximated 10-year longevity. It can be a useful, esthetically pleasing restorative alternative for the patient with congenital absence of incisor teeth or in other incisor tooth loss situations.
References
1. Burden D, Mullally B, Sandler J. Orthodontic treatment of patients with medical disorders. Eur J Orthod. 2001;23(4):363-372.
2. Gershman AJ, Mehta AC, Infeld M, et al. Cystic fibrosis in adults: an overview for the internist. Cleve Clin J Med. 2006;73(12):1065-1074.
3. Couzin-Frankel J. Genetics. The promise of a cure: 20 years and counting. Science. 2009;324(5934):1504-1507.
4. O’Sullivan BP, Freedman SD. Cystic fibrosis. Lancet. 2009;373(9678):1891-1904.
5. Hamer L, Parker HW. Treatment of cystic fibrosis in adults. Am Fam Physician. 1996;54(4):1291-1297.
6. Wagener JS, Headley AA. Cystic fibrosis: current trends in respiratory care. Respir Care. 2003;48(3):234-247.
7. Proffit WR, Fields HW, Sarver DM. Contemporary Orthodontics. 4th ed. St. Louis, MO: Mosby; 2006:234-267.
8. Yavuz MS, Aras MH, Büyükkurt MC, et al. Impacted mandibular canines. J Contemp Dent Pract. 2007;8(7):78-85.
9. Cooke J, Wang HL. Canine impactions: incidence and management. Int J Periodontics Restorative Dent. 2006;26(5):483-491.
10. Bedoya MM, Park JH. A review of the diagnosis and management of impacted maxillary canines. J Am Dent Assoc. 2009;140(12):1485-1493.
11. Ngan P, Hornbook R, Weaver B. Early timely management of ectopically erupting maxillary canines. Semin Orthod. 2005;11(3):152-163.
12. Bishara SE. Impacted maxillary canines: a review. Am J Orthod Dentofacial Orthop. 1992;101(2):159-171.
13. Mitchell L, ed. An Introduction to Orthodontics. 3rd ed. New York, NY: Oxford University Press; 2007:147-156.
14. Burden D, Mullally B, Robinson S. Palatally ectopic canines: closed eruption versus open eruption. Am J Orthod Dentofacial Orthop. 1999;115(6):640-644.
15. Polder BJ, Van’t Hof MA, Van der Linden FP, et al. A meta-analysis of the prevalence of dental agenesis of permanent teeth. Community Dent Oral Epidemiol. 2004;32(3):217-226.
16. Kokich VO Jr, Kinzer GA. Managing congenitally missing lateral incisors. Part 1: canine substitution. J Esthet Restor Dent. 2005;17(1):5-10.
17. Sharma A, Vargevik K. Using implants for the growing child. J Calif Dent Assoc. 2006;34(9):719-724.
18. Odman J, Gröndahl K, Lekholm U, Thilander B. The effect of osseointegrated implants on dentoalveolar development: A clinical and radiographic study in growing pigs. Eur. J. Orthod 1991;13(4):279-286.
19. Kokich V. Maxillary lateral incisor implants: the orthodontic perspective. Advanced Esthetics and Interdisciplinary Dentistry. 2006;2(2):2-7.
20. Heij DG, Opdebeeck H, van Steenberghe D, et al. Facial development, continuous tooth eruption, and mesial drift as compromising factors for implant placement. Int J Oral Maxillofac Implants. 2006;21(6):867-878.
21. Zachrisson BU. Single tooth implant-supported crowns in the anterior maxilla: potential esthetic long-term (> 5 years) problems. World J Orthod. 2006;7(3):306-312.
22. Goldstein RE. Attitudes and problems faced by both patients and dentists in esthetic dentistry today: an AAED membership survey. J Esthet Restor Dent. 2007;19(3):164-170.
23. Greenberg J. The etched porcelain-fused-to-metal resin-bonded prosthesis: an eight year retrospective. Dent Dialogue. 2003;3:388-398.
24. Livaditis GJ, Thompson VP. Etched castings: an improved retentive mechanism fort resin-bonded retainers. J Prosthet Dent. 1982;47(1):52-58.
25. Proffit RW, Fields HW, Sarver DM. Contemporary Orthodontics. 4th ed. St. Louis, MO: Mosby; 2006:623-626.
26. Greenberg JR, Kelly JT Jr, Yoshida A. Etched porcelain-fused-to-metal resin-bonded prosthesis. J Esthet Dent. 1996;8(6):273-278.
27. Greenberg JR, Ho PP. Communicating facial plane information to the dental laboratory: introducing the Facial Plane Relator device. J Prosthet Dent. 2001;86(2):173-176.
28. Haywood VB. Current status of nightguard vital bleaching. Compend Contin Educ Dent. 2000;28(suppl):S10-S17.
29. Patthoff D, Ozar D. Need vs desire: professional judgment in esthetics. AGD Impact. 2007:32-35.
30. Flores-Mir C, Silva E, Barriga MI, et al. Lay person’s perception of smile aesthetics in dental and facial views. J Orthod. 2004;31(3):204-209.
About the Authors
Harold Slutsky, DMD
Clinical Associate Professor (Adjunct) of Orthodontics
The Kornberg School of Dentistry at Temple University
Philadelphia, Pennsylvania
Joseph R. Greenberg, DMD
Clinical Professor of Restorative Dentistry
The Kornberg School of Dentistry at Temple University
Philadelphia, Pennsylvania
Clinical Professor of Periodontics
The University of Pennsylvania School of Dental Medicine
Philadelphia, Pennsylvania