Materials for Chairside CAD/CAM Restorations
Dennis J. Fasbinder, DDS
Abstract
Chairside computer-aided design/computer-aided manufacturing (CAD/CAM) systems have become considerably more accurate, efficient, and prevalent as the technology has evolved in the past 25 years. The initial restorative material option for chairside CAD/CAM restorations was limited to ceramic blocks. Restorative material options have multiplied and now include esthetic ceramics, high-strength ceramics, and composite materials for both definitive and temporary restoration applications. This article will review current materials available for chairside CAD/CAM restorations.
The delivery of ceramic restorations in a single appointment became a treatment option in 1985 with the introduction of the first chairside computer-aided design/computer-aided manufacturing (CAD/CAM) system.1 In today's dental marketplace, two chairside CAD/CAM systems are available. The CEREC® acquisition center (AC) (Sirona, https://www.sirona.com) and the E4D™ Dentist System (D4D Technologies, https://www.e4dsky.com) were both introduced as CAD/CAM systems capable of imaging, designing, and fabricating ceramic restorations chairside.1,2
Restorative materials for chairside CAD/CAM systems have several unique features. Manufacturers fabricate the material in a solid block form ready for the milling process. Both commercial systems employ a wet grinding process for shaping or milling the restoration from the preformed blocks. The material must be capable of being milled efficiently, generally in less than 20 minutes. This enables the final restoration to be delivered at the same appointment the tooth is prepared. To avoid early failure, the restoration must be capable of being milled without damage to the material. Optimally, the final restoration should require minimal time for the post-milling processing to complement the chairside delivery. A lengthy post-milling processing would be expected to detract from the usefulness of the material chairside. For this reason, zirconia restorations are not considered chairside restorations even though they can be milled in a CAD/CAM system. The required post-milling processing time of 6 to 8 hours is unreasonable for a single appointment procedure.
In the past 25 years, materials have been introduced as chairside CAD/CAM systems have evolved. This article reviews current materials available for chairside CAD/CAM restorations.
CAD/CAM Restorative Materials
Several categories of restorative materials are available for chairside CAD/CAM restorations (Table 1). Esthetic ceramics contain a glass phase that allows the restoration to be etched and adhesively bonded for retention to the tooth. High-strength ceramics offer a substantial increase in flexural strength compared with esthetic ceramics but not at the level of polycrystalline ceramics, such as zirconia. Two types of composite resin blocks are available. One brand is used for final restorations, and the other marketed composite resin blocks are recommended for long-term temporization. Although composite resin materials have desirable properties for chairside applications, ceramic blocks are the primary material used for chairside CAD/CAM restorations.
Esthetic Ceramics
The principle features of esthetic ceramics are that they contain a glass phase and have excellent translucency and moderate strength. The glass component allows them to be etched and adhesively bonded to the tooth, which is critical to the restoration's long-term retention and durability. The two feldspathic glass-ceramic materials are Vitablocs® Mark II (Vident, https://www.vident.com) and CEREC® Blocs (Sirona). Both materials are fine-grained, homogeneous feldspathic porcelain with an average particle size of 4 μm.3 Introduced in 1991, Vitablocs Mark II are available in the 10 most common Vita 3D-Master shades. CEREC Blocs entered the marketplace in 2007 and are manufactured by Vita Zahnfabrik (https://www.vita-zahnfabrik.com).4 The blocks are available in six shades and three degrees of color saturation (chroma): translucent (T), medium (M), and opaque (O).4
Vitablocs Mark II is also offered in several types of multicolored blocks. TriLuxe blocks (Vident) contain three different shade layers to re-create the shade and translucency of the tooth from cervical to incisal. TriLuxe forte blocks (Vident) feature a gradient of color and translucency from cervical to incisal with increased fluorescence and chroma in the cervical area. The newly introduced RealLife block (Vident) has an innovative 3-D radial gradient of color and translucency from the internal to external of the block to simulate the natural transition from dentin core to enamel veneer. CEREC Blocs are also produced in a multicolored block form. The CEREC Bloc PC has a three-layered structure with the bottom (cervical) layer having the highest pigmentation and lowest translucency and the top (incisal) layer possessing the highest translucency and lowest color intensity. It is available in three gradient shades. Multicolor blocks offer an enhanced esthetic result compared with conventional monochromatic blocks. Further customization of either type can be accomplished by shade characterization and glazing using the Vita Shading Paste Assortment Kit. The kit is compatible with both Vitablocs Mark II and CEREC Blocs.
Vitablocs Mark II restorations have the most clinical studies published relative to chairside CAD/CAM materials as this product is the oldest-marketed chairside CAD/CAM material.5 A clinical study conducted on 2328 inlays and onlays for 794 patients in a private practice reported 35 failures over 9 years.6 The Kaplan-Meier survival probability was 97.4% at 5 years and 95.5% at 9 years. Another study reported a Kaplan-Meier survival probability of 90.4% after 10 years for 200 Vitabloc Mark I restorations placed in 108 patients in private practice.7 In a follow-up report for that study, the authors reported an 88.7% success rate at 17 years.8 From 1991 to 2006, a series of papers reported the clinical status of 1011 CEREC restorations for up to 18 years.9-11 After 5 years, the survival probability was 95%, and after 7 years, it was 91.6%. At 10 years, the survival probability was 90% and declined to 84.9% at 16.7 years. A systematic review of 29 clinical studies, which included 2862 inlays, reported a survival rate of 97.4% after 4.2 years.12 The primary mode of failure was fracture of the ceramic restoration. Less common failures included tooth fracture, wear of the cement, and postoperative sensitivity.
The two leucite-reinforced glass-ceramic materials are IPS Empress® CAD (Ivoclar, https://www.ivoclarvivadent.us) and Paradigm™ C (3M ESPE, https://www.3mespe.com). Introduced in 1998, the first leucite-reinforced glass-ceramic CAD/CAM block was ProCAD (Ivoclar). It evolved to the current IPS Empress CAD and is a 35% to 45% leucite-reinforced glass- ceramic similar to IPS Empress I but with a finer particle size of 1 μm to 5 μm. The blocks are available in nine popular shades in either a high translucency (HT) or low translucency (LT) version. The HT version has an increased translucency while the LT type has a brighter value and is available in four bleach shades. IPS Empress CAD is offered in a multicolor block form. Offered in five colors, the block has a color gradient and translucency from cervical to incisal to simulate the transition of color and translucency in the natural dentition. Individual shade customization of either the monochromatic or multicolor blocks can be accomplished with the use of IPS Empress Universal Stains.13
Introduced in 2006, Paradigm C (3M ESPE) is a 30% leucite-reinforced glass-ceramic. Available in six shades, Paradigm C is a radiopaque ceramic that exhibits a chameleon effect once seated in the tooth due to its enhanced translucency and fluorescence14 (Figure 1, Figure 2 and Figure 3). This product is not available in a polychromatic block at this time. The shade of Paradigm C restorations can be customized using the Lava™ Ceram (3M ESPE) stains and glaze.
Studies involving IPS Empress CAD are limited; however, this product is similar to Empress I in physical structure, so a similar clinical performance may be anticipated. A literature review of longevity and clinical performance of IPS Empress restorations was reported in 2002.15 Six clinical trials on the performance of IPS Empress inlays and onlays and three clinical trials on the performance of IPS Empress crowns were identified in the literature. Survival rates for IPS Empress inlays and onlays ranged from 96% at 4.5 years to 91% at 7 years with most failures due to bulk fracture of the restorations. IPS Empress crowns had survival rates from 92% to 99% at 3 to 3.5 years, with failure also mainly due to crown fracture.
High-Strength Ceramics
IPS e.max® CAD (Ivoclar) was introduced in 2006 as a lithium-disilicate CAD/CAM material with a flexural strength of 360 MPa to 400 MPa, which is two to three times the flexural strength of the esthetic ceramics.16,17 The increased strength affords the opportunity to either etch and adhesively bond the material to the tooth or use a conventional cementation technique.18 Lithium disilicate was initially developed as a substructure material that offered greater translucency compared with other high-strength ceramic core materials. However, it has gained popularity for use as a monolithic restoration in chairside CAD/CAM systems due to the enhanced strength. The CAD/CAM block form is available in nine A-D shades, two translucencies, and four bleach shades.
IPS e.max CAD blocks consist of 0.2-μm to 1-μm lithium meta-silicate crystals with approximately 40% crystals by volume. The block is blue violet, accounting for the commonly used "Blue Block" description. This partially crystallized "soft" state allows the block to be easily milled without excessive diamond bur wear or damage to the material. After milling, the restoration must undergo a two-stage firing process in a porcelain oven under vacuum (20 to 25 minutes) to complete the crystallization of the lithium disilicate. This also converts the blue shade of the precrystallized block to the selected tooth color and results in a glass-ceramic with a fine grain size of approximately 1.5 μm and a 70% crystal volume incorporated in a glass matrix.19
Few clinical studies involve IPS e.max CAD or its press-fit counterpart IPS e.max Press due to its limited time in the marketplace. A prospective clinical study on molar onlay restorations used a split-mouth design in 25 patients to compare the clinical longevity of IPS e.max Press onlays with ProCAD onlays.20 One ProCAD onlay fractured at 9 months and was considered a failure. The Kaplan-Meier survivability at 3 years was 97% for the ProCAD onlays and 100% for the IPS e.max Press onlays. An ongoing longitudinal clinical study is evaluating the clinical performance of 62 IPS e.max CAD crowns in 43 patients. Each crown was placed in a single treatment appointment with the CEREC AC system (Figure 4, Figure 5 and Figure 6). At the end of 2 years, there were no reported crown failures and no clinically visible chipping or cracking of the crowns.21
Composite Resin— Permanent Restorations
Paradigm MZ100 (3M ESPE) was introduced in 2000. It is a polymer composite block based on the Z100 composite chemistry using a processing technique to maximize the degree of cross-linking.22,23 Paradigm MZ100 has zirconia-silica filler particles and is 85% filled by weight with an average particle size of 0.6 μm. It is radiopaque and available in six shades, as well as a more translucent enamel color.
Paradigm MZ100 represents a departure from the more popular ceramic materials. Composite can be more easily adjusted and polished intraorally compared to ceramic materials. This is an important feature of the chairside clinical technique because there is generally no working die and occlusal refinement occurs intraorally. Repair of porcelain restorations intraorally has not proven to be more than a moderately effective temporary technique.24,25 With Paradigm, the restoration surface is air-abraded with 50-μm silicon dioxide, and a hybrid composite can be bonded to the abraded surface. Although untested for clinical longevity, this affords an easy and efficient intraoral repair procedure for Paradigm MZ100 restorations.
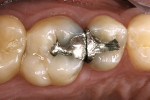
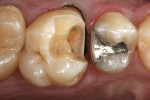
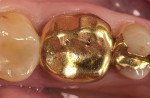
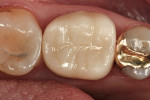
An ongoing clinical study reported the 3-year and 6-year results of a randomized clinical trial of 40 Paradigm MZ100 inlays and 40 Vitabloc Mark II inlays26,27 (Figure 7, Figure 8 and Figure 9). All restorations were evaluated at baseline, 6 months, and annually for 6 years using modified USPHS criteria. One Vitabloc Mark II inlay had postoperative sensitivity that resolved in 2 weeks. Throughout the 6-year recall, all other restorations had no sensitivity. The CAD/CAM composite inlays performed similarly to the CAD/CAM ceramic inlays at the 6-year recall with greater than 90% alpha ratings for all categories evaluated.
Composite Resin— Temporary Materials
The most recent material addition for CAD/CAM chairside restorations is acrylic temporary materials. With the continued development of laboratory CAD/CAM systems and digital impression systems, CAD/CAM temporary crowns and fixed partial dentures (FPDs) are available, as well. The CAD/CAM process avoids an air-inhibited surface layer on conventional self-cure or VLC acrylics, as well as polymerization shrinkage.
Vita CAD-Temp® (Vident) is a highly crosslinked microfilled polymer that is available in extended block sizes, including lengths of 40 mm and 55 mm, to accommodate multiple-unit FPDs.28 It is offered as a monocolor block that comes in four shades or a multicolor form with four shade layers for more esthetic cases. Telio® CAD (Ivoclar) was recently introduced as a millable cross-linked polymethyl methacrylate block for temporary crowns and FPDs. The block is part of the Telio system, which includes a self-curing composite, desensitizer, and cement. It is available in five shades.29
Both temporary materials are recommended by the manufacturers for up to 1 year of clinical service.
Conclusion
The term chairside CAD/CAM restoration is more descriptive of the fabrication technique than the actual final restoration as demonstrated by the various types of materials available for restorative treatment. All of the available ceramic and composite materials demonstrate the desirable qualities of machinable materials. They can be milled efficiently for chairside use without damage to the restoration. The materials are esthetically acceptable as milled yet provide the ability to customize the final shade of the restoration if desired. All are recommended for use with an adhesive cementation technique. To date, clinical studies have documented the predictability and longevity of chairside CAD/CAM restorations.
References
1. Mörmann, WH. The evolution of the CEREC system. J Am Dent Assoc. 2006;137(suppl):7S-13S.
2. Levine N. To the sky and beyond. Dental Products Report. October 2009:116.
3. Vitablocs Mark II. Materials Science and Clinical Studies. Brea, California: Vident. September 2003.
4. CEREC Blocs—for CEREC/InLab. Operating Instructions. Charlotte, NC: Sirona Dental.
5. Fasbinder DJ. Clinical performance of chairside CAD/CAM restorations. J Am Dent Assoc. 2006;137(suppl):22S-31S.
6. Posselt A, Kerschbaum T. Longevity of 2328 chairside CEREC inlays and onlays. Int J Comput Dent. 2003;6(3):231-248.
7. Otto T, De Nisco S. Computer-aided direct ceramic restorations: a 10-year prospective clinical study of CEREC CAD/CAM inlays and onlays. Int J Prosthodont. 2002;15(2):122-128.
8. Otto T, Schneider D. Long-term clinical results of chairside Cerec CAD/CAM inlays and onlays: a case series. Int J Prosthodont. 2008;21(1):53-59.
9. Reiss B, Walther W. Survival analysis and clinical evaluation of CEREC restorations in a private practice. In: WH Mormann, ed. International Symposium on Computer Restorations 1991: State of the Art of the CEREC-Method. Berlin, Germany: Quintessence Publishing; 1991:215.
10. Reiss B, Walther W. Clinical long-term results and 10-year Kaplan-Meier analysis of CEREC restorations. Int J Comput Dent. 2000;3(1):9-23.
11. Reiss B. Clinical results of Cerec inlays in a dental practice over a period of 18 years. Int J Comput Dent. 2006;9(1):11-22.
12. Martin N, Jedynakiewicz NM. Clinical performance of CEREC ceramic inlays: a systematic review. Dent Mater. 1999;15(1):54-61.
13. IPS Empress® CAD Instructions for Clinical Use Chairside. Ivoclar Vivadent Technical. Amherst, NY: Ivoclar Vivadent; September 2006.
14. Paradigm™ C. Technical Product Profile. St. Paul, MN: 3M ESPE. March 2006.
15. El-Mowafy O, Brochu J. Longevity and clinical performance of IPS Empress ceramic restorations—a literature review. J Can Dent Assoc. 2002;68(4):233-237.
16. Vichi A, DelSiena F, Sedda M, et al. Flexural resistance of CAD/CAM blocks for CEREC [Abstract 129]. J Dent Res. 2010.
17. Charlton DG, Robert HW, Tiba A. Measurement of select physical and mechanical properties of 3 machinable ceramic materials. Quintessence Int. 2008;39(7):573-579.
18. Tysowsky G. Science behind lithium disilicate. Oral Health. March 2009:93-97.
19. IPS e.max lithium disilicate: the future of all-ceramic dentistry. Material science, practical applications, keys to success. Ivoclar publication 627329. March 2009:1-15.
20. Guess PC, Strub JR, Steinhart N, et al. All-ceramic partial coverage restorations—midterm results of a 5-year prospective clinical splitmouth study. J Dent. 2009;37(8):627-637.
21. Fasbinder DJ, Dennison JB, Heys D, et al. A clinical evaluation of chairside lithium disilicate CAD/CAM crowns: a two-year report. J Am Dent Assoc. 2010;141(suppl):10S-14S.
22. Rusin RP. Properties and applications of a new composite block for CAD/CAM. Compend Contin Educ Dent. 2001;22(6 suppl):35-41.
23. Paradigm™ MZ100 Block: Technical Product Profile. St. Paul, MN: 3M ESPE; 2000.
24. Leibrock A, Degenhart M, Behr M, et al. In vitro study of the effect of thermo- and load-cycling on the bond strength of porcelain repair systems. J Oral Rehabil. 1999;26(2):13-17.
25. Appeldoorn RE, Wilwerding TM, Barkmeier WW. Bond strength of composite resin to porcelain with newer generation porcelain repair systems. J Prosthet Dent. 1993;70(1):6-11.
26. Fasbinder DJ, Dennison JB, Heys DR, et al. The clinical performance of CAD/CAM-generated composite inlays. J Am Dent Assoc. 2005;136(12):1714-1723.
27. Fasbinder DJ, Dennison JB, Heys DR, et al. The clinical evaluation of CAD/CAM-generated composite inlays: six-year report [Abstract 0543]. J Dent Res. 2006.
28. Vita machinable polymers: product information. Vita Zahnfabrik. 2010.
29. Telio CS and Telio-CAD. Instructions for Use. Ivoclar Vivadent Technical. December 2009.
About the Author
Dennis J. Fasbinder, DDS
Clinical Professor of Dentistry and Director
Advanced Education in General Dentistry Program
Department of Cariology, Restorative Sciences, and Endodontics
The University of Michigan School of Dentistry
Ann Arbor, Michigan