A Classification System of Patients for Esthetic Fixed Implant-supported Prostheses in the Edentulous Maxilla
Avinash S. Bidra, BDS, MS, FACP; and John R. Agar, DDS, MA, FACP
Abstract
Edentulous maxillary fixed rehabilitation using dental implants is challenging and requires meticulous planning because of anatomic variations and the importance of facial and dental esthetics. This article reviews the application of facial esthetics, lip support, smile lines, residual ridge position, tooth proportions, and tooth positions for different types of patients. Based on these parameters, a simple new classification system is proposed to classify patients into four categories, which will help facilitate an easier diagnostic and communicative system. It will also enable the clinician to understand when and why gingiva-colored prosthetic material is needed. Using this classification system, a stepwise method of diagnosis and management techniques are described in detail for each of the four classes. The proposed classification system has been based on an analysis of various successfully treated patients with a minimum follow-up period of 2 years.
Edentulous maxillary implant reconstructions are often challenging and complicated.1 Some of the important considerations and challenges include the anatomy of the maxilla, the pattern of bone resorption, quality of available bone for implants, development of pontic form, role of the maxilla in speech, and perception of esthetics.1-3 A few authors have addressed issues regarding treatment-planning the edentulous maxilla for fixed rehabilitation and have advised caution. These researchers have suggested the alternative of using removable overdenture prostheses in complex situations.3-5 However, implant-supported rehabilitation of the edentulous maxilla using a fixed prosthesis has gained considerable popularity in recent years. This article describes a system of esthetically focused treatment planning for the edentulous maxilla when the patient exclusively desires a fixed implant-supported prosthesis.
A classification of patients is needed not only for diagnostic purposes but also to facilitate treatment planning, patient education, and professional communication among different specialists. Misch6 has classified the different types of implant prostheses available for patients while Simon and Raigrodski7 have specifically classified the types of residual ridge deficiencies and addressed the need for use of gingival prosthesis. The classification system described in this article exclusively categorizes patients, based on specific clinical parameters, and suggests management techniques for each class. The classification is focused on evaluation of anatomic and physiologic variables that could lead to esthetic and functional failures, if they are not considered prior to rehabilitation of the edentulous maxilla. It is necessary to treat each patient uniquely and to avoid the use of a generic or similar design of fixed prosthesis for all patients. Therefore, the proposed classification system categorizes patients into four classes, based on the amount of tissue loss, position of anterior teeth in relation to residual ridge location, lip support, smile line, and need for gingiva-colored prosthetic material. Using this system will help prevent completed prostheses with various adverse situations, such as an unsightly restoration to natural tissue interface, disproportionate teeth, and inappropriate lip support.
Clinical Considerations for Classification
For a diagnosis and patient classification in planning a fixed prosthesis for an edentulous maxilla, a thorough esthetic analysis using complete denture principles should be performed, incorporating the following diagnostic elements:
Maxillary Incisal Edge Position
The maxillary incisal edge position is considered the starting point of all full-mouth reconstructions.8 It is critical to determine the ideal location of this edge on the face because it helps determine esthetics, occlusal plane, and occlusal vertical dimension. Its ideal position is determined by esthetics and phonetics. An important assessment also involves observation of how visible the incisors are when the lips are in repose. Normally, this is about 3 mm at 30 years of age, 1 mm at 50 years, and less than 1 mm at 60 years.9,10 Although these are broad guidelines, there are variations involving race, gender, and length of the upper lip. The phonetic determination of the maxillary central incisors includes positioning them such that the incisal edges gently touch the wet-dry junction of the lower lip on pronunciation of F and V sounds.10-12
Maxillary Cervical Edge Position and Esthetic Tooth Proportions
Once the maxillary incisal edge position has been determined, the length of the incisors may be established using standard tooth proportions.12 This can be evaluated based on esthetic tooth proportions, the patient’s previous dental casts, or photographs if esthetically acceptable. The average length of a maxillary central incisor is 10.5 mm in height and 8.5 mm in width.13,14 Average proportions or those similar to these proportions should be used.15,16 The height and width of the prosthetic teeth should be based on esthetic tooth proportions and not based on the location of the patient’s anterior residual ridge. If any additional space exists between the esthetically determined cervical margin of the prosthetic teeth and existing natural tissues, it should be filled with a gingiva-colored prosthetic material.7
Smile Line
Maxillary lip position is one of the most important elements in anterior esthetics. Its analysis in static and dynamic positions will eventually determine the type of fixed prosthesis for the patient. The average length of the maxillary lip is 19 mm to 22 mm.17 Lip length generally increases with age and will decrease the incisal display at rest.18,19 Based on maxillary lip position, smiles have been classified into high, medium, or low, with medium the most commonly seen in about 70% of the population.20,21 A fourth type has been differentiated by some authors as the “gummy smile” with an exposure of 4 mm of maxillary gingival tissues by the lip.10,22 This type may indicate a hard-tissue abnormality called vertical maxillary excess (VME) or a soft-tissue abnormality caused by a short and/or a hyperfunctional maxillary lip.19,22-25 In treatment planning for a maxillary implant-supported fixed prosthesis, it is critical to diagnose the highest or the most apical position of the upper lip when the patient poses a stretched and extensive smile. This position will affect the type of fixed prosthesis and management of the junction between the prosthesis and patient’s natural tissues. It is important to determine this position with the diagnostic teeth in the mouth because the prosthetic teeth height eventually will affect the amount of gingival display. Diagnostic teeth that are shorter than ideal or positioned too incisally may exaggerate the display of the residual ridge when a patient smiles and lead to an incorrect diagnosis of a high or gummy smile.
Gingival Display
Gingival display is directly related to the maxillary incisal edge position, cervical edge position, and smile line. Excess gingival display results from hard- or soft-tissue abnormalities and cannot be fully corrected by prosthodontic means alone. However, if the tooth positions and proportions are accurate, it may be acceptable to display well-fabricated prosthetic gingiva when a patient smiles. However, clinicians must avoid the visibility of the prosthesis tissue junction (PTJ) to prevent esthetic failures.7,26 The PTJ can be defined as the junction of the natural tissues of the edentulous ridge and abutting surface of the prosthesis. The literature has made it clear that a convex shape is favored most for this abutting surface in order to facilitate oral hygiene.27-29
Maxillary Lip Support
One of the most subjective elements related to facial esthetics in prosthodontics is the determination of the ideal maxillary lip support or lip projection for a patient. Lip projection at its apex is related to its thickness, as well as support provided by the maxillary alveolar process and anterior teeth; lip projection at its pedestal is intimately related to the morphology of the cartilaginous part of the lower nose, nasal septum, and anterior nasal spine.30 “Ideal” lip support is a range, and its assessment and perception are affected by various factors described below.
1. Maxillary anterior teeth: For dentate patients, the cervical contours of the maxillary incisors have been directly implicated in providing lip support.12 Thus, the inclination of the maxillary incisors with respect to the frontal plane can affect the perception of lip support. An axial inclination of 28° to the sagittal plane has been recommended in positioning the prosthetic central incisors to provide optimal lip support.12 However, clinical judgment often is necessary to avoid positioning the anterior teeth excessively proclined or excessively retroclined.
2. Alveolar bone loss: Tallgren, Atwood, and others have demonstrated that maxillary bone resorbs in a centripetal fashion moving superiorly and medially.31-33 This leaves the residual ridge crest upward and backward compared to the condition at the time of extraction. Thus, if prosthetic teeth were positioned directly on a severely resorbed ridge, the lip support would be obviously deficient.
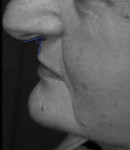
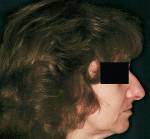
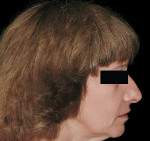
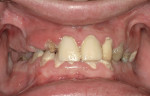
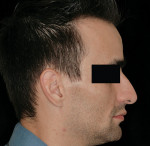
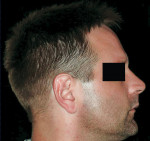
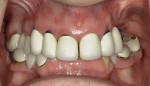
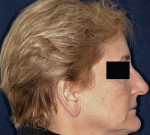
3. Nose length: The length or projection of the nose has often been overlooked; however, it plays a considerable role in the perception of lip projection.30,34 A patient with a longer nose may confound the clinician’s perception of the maxillary lip projection, and there may be a tendency to place the diagnostic teeth further anterior than the ideal position unknowingly. This may change the lip projection and eventually will affect the design of the final prosthesis (Figure 1 and Figure 2).
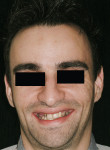
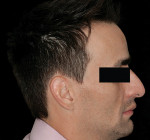
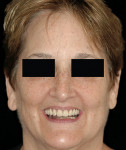
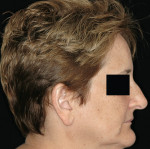
4. Angulation of the nasal tip: The nasolabial angle (NLA) is defined as the angle formed the intersection of the columella and subnasale.35 The average NLA is 90° to 95° for men and 100° to 105° for women.10,17 Most cases fall in this range with minor variations. However, if a patient presents with a nasal tip rotated naturally upward, the NLA is more obtuse, leading to a perception of “lacking” in maxillary lip support. The clinician may unknowingly overcompensate for this by placing the maxillary diagnostic teeth further anterior to the residual ridge, which will change the lip projection and thus change the design of the prosthesis (Figure 3 and Figure 4).
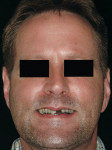
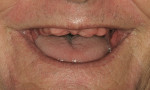
5. Angulation of the chin: Similar to the nose, the chin can play a role in the perception of lip support. A patient with an excessive soft-tissue chin or a skeletal Class III situation presents with a concave profile and may give the illusion of lacking maxillary lip support. Compensation for this to “improve” lip support will necessitate the placement of diagnostic teeth in a position that will change the type of fixed prosthesis planned for the patient (Figure 5 and Figure 6).
The patient should be educated about these factors and allowed to make the final decision of “acceptable” lip support because this will eventually determine the design of the fixed prosthesis indicated.
Patient Classification
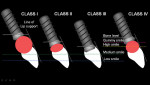
After a thorough analysis of all of the above elements, a diagnosis can be made and patients can be categorized into the following four classes for esthetic fixed implant-supported prostheses in the edentulous maxilla (Table 1 and Table 2). The proposed classification system has been based on an analysis of various patients receiving treatments with a minimum follow-up period of 2 years. The key elements in this system are amount of tissue loss, position of anterior teeth in relation to the residual ridge, smile line, and need for gingiva-colored prosthetic material (Figure 7).
Class I
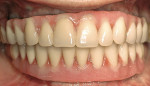
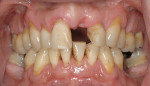
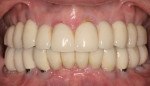
These patients will require gingiva-colored prosthetic material to obtain esthetic tooth proportions and optimal prosthesis contour, as well as lip support (Figures 8, 9, 10, 11, 12, 13).
Class II
These patients will require gingiva-colored prosthetic material only to obtain esthetic or ideal tooth proportions and for prosthesis contour. Lip support is not a consideration in this class because the difference in lip projection with and without any prosthesis is generally insignificant (Figure 14, Figure 15, Figure 16, Figure 17, Figure 18 and Figure 19).
Class III
These patients will not require gingiva-colored prosthetic material (Figure 20, Figure 21, Figure 22, Figure 23, Figure 24 and Figure 25).
Class IV
These patients may or may not require gingiva-colored prosthetic material, based on the outcome of the chosen intervention and class of conversion (Figure 26, Figure 27, Figure 28, Figure 29, Figure 30 and Figure 31).
Discussion
The diagnosis and treatment for Class I, II, and III should be relatively straightforward if the above-mentioned keys are used. Bone grafting may be considered for placement of the implants into appropriate positions. A key distinction between classes is the amount of prosthetic space, which sequentially decreases from Class I to Class IV (Figure 7). The prosthesis design can be correlated to the amount of prosthetic space and the patient classification. A fixed complete denture (FCD) requires more space to sup port the abutments, bar, resin, and teeth; a fixed partial denture (FPD) with gingival prosthesis requires lesser space than an FCD; and an FPD without gingival prosthesis needs the least amount of space. Based on this principle, it is possible to change the classification and accordingly alter the design of the prosthesis. For example, minimal prosthetic space is available for Class III patients who are good candidates for FPDs without any gingival prosthesis. To design an FCD for these patients, alveoloplasty procedures may be performed to reduce the bone and thus create the required prosthetic space, which then converts patients to a Class I or Class II. Conversely, it appears that with the use of complex ridge augmentation surgical procedures, a patient from a Class I or Class II may be converted to a Class III. The authors, however, recommend the lesser invasive alternative of using gingiva-colored prosthetic material.
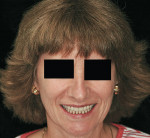
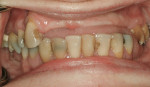
Management of a Class IV patient is complex and always requires conversion to another class for optimal treatment. The Class IV patient is distinct by being the only one that presents with a high smile or a “gummy smile,” exposing a large amount of gingiva, teeth, or residual alveolar ridge on maximum smile (Figure 32 and Figure 33). Depending on the design of the prosthesis, this gingival display has a great potential to compromise esthetics at the PTJ. Hence, if a gingiva-colored prosthetic material is used, it is always desirable to hide the PTJ under the lip, even in an exaggerated smile. Thus, if the tooth proportions are esthetic, it may be preferable to display well-fabricated prosthetic gingiva when a patient smiles rather than the patient displaying the PTJ, which will lead to an esthetic failure.7 Depending on its etiology, the Class IV patient can be managed in various ways.
If the gingival display is severe and a result of a severe skeletal discrepancy such as VME as seen in dolichofacial patients, a Lefort I osseotomy needs to be advocated to vertically impact the maxilla.22,34,36 Patients with VME often have their existing natural maxillary teeth significantly incisal to the ideal position.19,24,36 Preprosthetic surgical planning and an ideal diagnostic wax-up after the surgical intervention will esthetically position the occlusal plane high enough to have the PTJ concealed beneath the lip. Essentially, the patient is now converted from Class IV to II. It is also possible to convert a patient from Class IV to III if there is enough thickness of soft tissue available on the residual ridge to develop good interdental papillae and an esthetic soft-tissue interface with the prosthetic teeth.
If the gingival display is a result of either a short and/or a hyperfunctional upper lip and unrelated to a skeletal discrepancy, plastic surgery procedures may be chosen. These procedures have been reported to lengthen the upper lip and diminish its movement.22,34,36-38 Some authors have advocated the use of Botox® (Allergan, Inc, https://www.allergan.com) and shown successful short-term results.22,25 These procedures could be used in combination with dental procedures to reduce the gingival display. However, the actual results and long-term validity of these cosmetic techniques are not well established, and the authors recommend caution until validated by future research.
If the gingival display is moderate and unrelated to any severe skeletal discrepancy, then a less invasive surgery, such as anterior bone reduction, may satisfy the esthetic requirement.26 The diagnostic wax-up procedure is first accomplished, and the teeth should be set to ideal positions. Based on the prosthetic design chosen, the residual alveolar bone in the anterior maxillary region should be reduced such that the new crestal bone level is apical to the maxillary lip line, recorded at the patient’s maximal smile. The implants should be placed at this new bone level. This will ensure that the PTJ is adequately concealed under the lip26 (Figure 26, Figure 27, Figure 28, Figure 29, Figure 30 and Figure 31). Thus, a Class IV patient may now be converted to Class I, II, or III based on the preplanned prosthetic design.
If the gingival display is minimal, it may be left untreated if the patient chooses. A slight display of gingiva, especially in younger women, has been reported to be esthetically acceptable.24,39 If this option is chosen, the management becomes very challenging as the patient can only be treated as a Class III; gingiva-colored prosthetic material should not be used. This is because the shade of the prosthetic gingiva and the natural mucosal tissues is difficult to match;7 improper shade matching may lead to an esthetic failure at the PTJ, which is left visible in these patients. It is well understood that obtaining interdental papillary fill is difficult when implants are placed adjacently.40,41 Therefore, periodontal surgical procedures probably will be needed to augment the hard and soft tissues to obtain esthetic soft-tissue architecture around implant abutments and pontic sites. The patient should be told about the challenges and realities of these procedures.7,40,41
Conclusion
Patients requiring fixed implant-supported prosthesis in the edentulous maxilla are seen in various forms. This clinical review described a stepwise method to diagnose, treatment plan, and classify patients based on esthetic analyses. The clinician should have a thorough knowledge and understanding of facial esthetics and complete denture principles before treatment-planning these complex procedures. This will help ensure appropriate individualized treatment plans. To the authors’ knowledge, this is the first known classification of patients based on the described cri teria and essential for facilitating a logical method to achieve excellence in the final treatment outcome.
This article was presented October 4th 2007 at the 14th Northeast Implant Symposium, Baltimore, MD, and February 22nd 2008 at the American Prosthodontic Society, Annual Session, Chicago, IL. It received second prize at the Steven J. Gordon Memorial Contest on November 14th 2007, American College American College of Prosthodontists - MA section, Boston, MA.
Acknowledgements
The authors thank the following for sharing their clinical images: Nancy Dubois, DMD, MDS; Adam Geach, DMD, MDS; and Andrew Chapokas, DMD, MDS. The authors also thank Steven J. Sadowsky, DDS, for his input.
References
1. Desjardins RP. Prosthesis design for osseointegrated implants in the edentulous maxilla. Int J Oral Maxillofac Implants. 1992;7(3):311-320.
2. Sadowsky SJ. The implant-supported prosthesis for the edentulous arch: design considerations. J Prosthet Dent. 1997;78(1):28-33.
3. Zitzmann NU, Marinello CP. Fixed or removable implant-supported restorations in the edentulous maxilla: literature review. Pract Periodontics Aesthet Dent. 2000;12(6):599-608.
4. Taylor TD. Fixed implant rehabilitation for the edentulous maxilla. Int J Oral Maxillofac Implants. 1991;6(3):329-337.
5. Bosse LP, Taylor TD. Problems associated with implant rehabilitation of the edentulous maxilla. Dent Clin North Am. 1998;42(1):117-127.
6. Misch CE. Contemporary Implant Dentistry. 2nd ed. St. Louis, MO: Mosby; 1999:68-69.
7. Simon H, Raigrodski AJ. Gingival-colored ceramics for enhanced esthetics. Quintessence Dent Technol. 2002;25:155-172.
8. Spear FM, Kokich VG, Mathews DP. Interdisciplinary management of anterior dental esthetics. J Am Dent Assoc. 2006;37(2):160-169.
9. Vig RG, Brundo GC. The kinetics of anterior tooth display. J Prosthet Dent. 1978;39(5):502-504.
10. Fradeani M. Esthetic Analysis: A Systematic Approach to Prosthetic Treatment. Hanover Park, IL: Quintessence; 2004:52-124.
11. Zarb GA, Bolender CL, Carlsson GE, et al, eds. Boucher’s Prosthodontic Treatment for Edentulous Patients. 11th ed. St. Louis, MO: Mosby; 1997:383.
12. Zitzmann NU, Marinello CP. Treatment plan for restoring the edentulous maxilla with implant-supported restorations: removable overdenture versus fixed partial denture design. J Prosthet Dent. 1999;82(2):188-196.
13. Ash MM Jr, Nelson SJ. Wheeler’s Dental Anatomy, Physiology, and Occlusion. 8th ed. Philadelphia, PA: Saunders; 2002:13.
14. Sterrett JD, Oliver T, Robinson F, et al. Width/length ratios of normal clinical crowns of the maxillary anterior dentition in man. J Clin Periodontol. 1999;26(3):153-157.
15. Magne P, Gallucci GO, Belser UC. Anatomic crown width/length ratios of unworn and worn maxillary teeth in white subjects. J Prosthet Dent. 2003;89(5):453-461.
16. Chu SJ. Range and mean distribution frequency of individual tooth width of the maxillary anterior dentition. Pract Proced Aesthet Dent. 2007;19(4):209-215.
17. Arnett GW, Bergman RT. Facial keys to orthodontic diagnosis and treatment planning. Part 1. Am J Orthod Dentofacial Orthop. 1993;103(4):299-312.
18. Fudalej P. Long-term changes of the upper lip position relative to incisal edge. Am J Orthod Dentofacial Orthop. 2008;133(2):204-209.
19. Peck S, Peck L, Kataja M. The gingival smile line. Angle Orthod. 1992;62(2):91-100.
20. Tjan AH, Miller GD, The JG. Some esthetic factors in a smile. J Prosthet Dent. 1984;51(1):24-28.
21. Dong JK, Jin TH, Cho HW, et al. The esthetics of a smile: a review of some recent studies. Int J Prosthodont. 1999;12(1):9-19.
22. Polo M. Botulinum toxin type A in the treatment of excessive gingival display. Am J Orthod Dentofacial Orthop. 2005;127(2):214-218.
23. Arnett GW, Bergman RT. Facial keys to orthodontic diagnosis and treatment planning—Part II. Am J Orthod Dentofacial Orthop. 1993;103(5):395-411.
24. Peck S, Peck L. Selected aspects of the art and science of facial esthetics. Semin Orthod. 1995;1(2):105-126.
25. Polo M. Botulinum toxin type A (Botox) for the neuromuscular correction of excessive gingival display on smiling (gummy smile). Am J Orthod Dentofacial Orthop. 2008;133(2):195-203.
26. Maló P, Nobre Mde A, Lopes I. A new approach to rehabilitate the severely atrophic maxilla using extramaxillary anchored implants in immediate function: a pilot study. J Prosthet Dent. 2008;100(5):354-366.
27. Johnson GK, Leary JM. Pontic design and localized ridge augmentation in fixed partial denture design. Dent Clin North Am. 1992;36(3):591-605.
28. Abrams L. Augmentation of the deformed residual edentulous ridge for fixed prosthesis. Compend Contin Educ Dent. 1980:1(3):205-213.
29. Pietrokovski, J, Sorin S, Hirschfeld Z. The residual ridge in partially endentulous patients. J Prosthet Dent. 1976:36(2);150-158.
30. Cocconi R. The nasolabial unit: clinical considerations. Paper presented at: Roth Williams International Society of Orthodontists (RWISO) meeting; June 9th 2007; Kyoto, Japan.
31. Tallgren A. The continuing reduction of the residual alveolar ridges in complete denture wearers: a mixed-longitudinal study covering 25 years. J Prosthet Dent. 1972;27(2):120-132.
32. Atwood DA. Bone loss of edentulous alveolar ridges. J Periodontol. 1979;50(4 spec no):11-21.
33. Pietrokovski J, Starinsky R, Arensburg B, et al. Morphologic characteristics of bony edentulous jaws. J Prosthodont. 2007;16(2):141-147.
34. Sarver DM. Esthetic Orthodontics and Orthognathic Surgery. St. Louis, MO: Mosby; 1998:8-27.
35. American Association of Orthodontists (AAO) Glossary 2008. Accessed Nov 20th, 2008.
36. Proffit WR, White RP, Sarver DM. Contemporary Treatment of Dentofacial Deformity. St. Louis, MO: Mosby; 2002:403-500.
37. Sarver DM, Rousso DR. Plastic surgery combined with orthodontic and orthognathic procedures. Am J Orthod Dentofacial Orthop. 2004;126(3):305-307.
38. Rosenblatt A, Simon Z. Lip repositioning for reduction of excessive gingival display: a clinical report. Int J Periodontics Restorative Dent. 2006;26(5):433-437.
39. Geron S, Atalia W. Influence of sex on the perception of oral and smile esthetics with different gingival display and incisal plane inclination. Angle Orthod. 2005;75(5):778-784.
40. Elian N, Jalbout ZN, Cho SC, et al. Realities and limitations in the management of the interdental papilla between implants: three case reports. Pract Proced Aesthet Dent. 2003;15(10):737-744.
41. Tarnow D, Elian N, Fletcher P, et al. Vertical distance from the crest of bone to the height of the interproximal papilla between adjacent implants. J Periodontol. 2003;74(12):1785-1788.
About the Authors
Avinash S. Bidra, BDS, MS, FACP
Assistant Professor and Maxillofacial Prosthodontist
Department of Prosthodontics
School of Dentistry
University of Texas Health Science Center
San Antonio, Texas
John R. Agar, DDS, MA, FACP
Professor and Graduate Prosthodontics Program Director
Department of Reconstructive Sciences
School of Dental Medicine
University of Connecticut Health Center
Farmington, Connecticut