Clinical Case Report: Treatment of Mild-to-Moderate Fluorosis With a Minimally Invasive Treatment Plan
Howard E. Strassler, DMD
Background
Age at Initial Presentation: 24
Initial Presentation: June 2006
Active Treatment Completed: September 2006
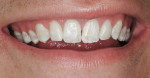
The patient’s chief concern was the appearance of his maxillary teeth, which had a mottled, brown-white enamel dysmineralization indicative of mild-to-moderate fluorosis. The patient was a second-year dental student and was concerned that the appearance of his teeth would negatively impact interactions with his patients. He believed the tooth discolorations of his maxillary anterior teeth would detract from his treatment plan presentations to patients for esthetic dental procedures.
Medical History
The patient presented with an unremarkable medical history except for a penicillin allergy and had no contraindications for treatment.
Dental History
As a young child in rural Vermont, the patient lived in an area that relied on well water. Because it was assumed that well water did not have fluoridation, the patient took multivitamins with fluoride and used a fluoride-containing toothpaste as an infant and young child, respectively. The patient reported the use of a bubble gum-flavored toothpaste and using larger amounts of toothpaste because he liked the taste. Therefore, he would swallow after brushing, rather than spitting. The patient also recalled drinking juices from cartons and some soft drinks that were probably reconstituted from concentrates at a bottling plant from the closest major metropolitan area (Burlington, Vermont). In all likelihood, the water used to reconstitute the juices and soft drinks was fluoridated. The patient had received regular dental care with recall appointments approximately every 6 months.
Diagnostic Findings
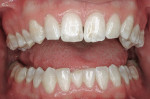
Intraoral: Maxillary and mandibular teeth were in acceptable alignment. The findings from the cancer screening were negative and hard and soft tissues within normal limits (WNL). Maxillary and mandibular incisors presented with mild-to-moderate brownish-white mottled enamel hypomineralization and discoloration. Transillumination of the maxillary incisors and canines revealed superficial enamel discoloration. Maxillary and mandibular third molars were malpositioned, creating difficulty for the patient to adequately clean teeth Nos. 1, 16, 17, and 32. No evidence of fremitus or occlusal dysfunction was present.
Temporomandibular Joints: WNL; no history of clicking or pain. Normal range of movement; no deviation on opening.
Diagnosis
Periodontal: AAP Type 1
Biomechanical: No caries; no restorations.
Functional: Slight wear of the mandibular incisors with chipping of tooth No. 25 from biting forks. Malpositioned teeth Nos. 1, 16, 17, and 32.
Dentofacial: Tooth proportions, shapes, and location acceptable. Tooth discoloration of mild-to-moderate brownish-white mottled enamel hypomineralization most likely due to fluorosis. Superficial enamel malformation on the facial surface of tooth No. 8 (Figure 1a and Figure 1b).
Risk Assessment
Periodontal: Low
Biomechanical: Low
Functional: Low
Esthetics: Medium
Radiographic Assessment
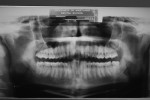
Bone levels as well as shape and size of pulp chambers appeared normal. No evidence of caries. Maxillary and mandibular third molars bilaterally malpositioned (Figure 2).
Concerns
- How could the appearance of the maxillary teeth be changed to provide a more even color?
- How could the appearance of the maxillary teeth be altered in a minimally invasive treatment so as to preserve the shape, size, and overall appearance of the smile? The patient expressed he did not want the teeth prepared and, if possible, did not want significant restorative intervention that would require future restoration replacement throughout life.
Treatment Goals
- Change the appearance of the maxillary teeth that were seen on smiling to an esthetically acceptable level for the patient.
- Maintain the enamel, shape, size, occlusion, and alignment of the maxillary teeth.
- Remove the malpositioned maxillary and mandibular third molars.
Treatment Plan
Diagnosis, treatment options, and goals were discussed with the patient. The patient’s primary objective was to modify the appearance of his maxillary teeth discolorations and the appearance of his smile minimally invasively to maintain as much enamel as possible and the shape, size, and position of his teeth in relationship to lips and smile line. The use of microabrasion and macroabrasion of the facial surfaces of the maxillary teeth was discussed as well as the use of adhesive directly placed composite resin veneers and minimally invasive porcelain veneers. Because minimal future maintenance and durability were the patient’s chief desires, the options of adhesive veneers were deferred until after treatment with microabrasion and macroabrasion. The patient was informed that the final shade and color of the teeth might require tooth bleaching in order to meet his expectations. As part of the treatment plan and because the maxillary and mandibular third molars had no acute issues, removal of the third molars was deferred until completion of the esthetic treatment.
Phase I: Enamel Abrasion
After routine oral prophylaxis, the maxillary teeth in the esthetic zone (teeth Nos. 5 to 13) were isolated with a dental dam. A combined enamel macroabrasion/microabrasion technique was chosen for treatment of the hypomineralized defects of the maxillary first premolars, canines, and lateral and central incisors. Enamel macroabrasion refers to the use of either medium or fine grit diamond abrasives or multifluted finishing burs with a high-speed handpiece with air and water spray to remove the superficial layer of the enamel.1 Enamel microabrasion refers to the use of a low-concentration acid combined with an abrasive agent as a water soluble gel or paste that would be applied to the enamel surface with an extremely low-speed rotary handpiece pressure applicator for precise compression of the compound on the tooth surface. This is to eliminate or minimize splattering of the compound. Use of the ultra-low-speed rotary application would make the procedure safer, easier, and quicker.2 The current formulation for microabrasion pastes is a low-concentration hydrochloric acid (6.6%), silicon carbide abrasive, and silica gel as a binding agent. This paste, in fact, etches the enamel surface more aggressively than the use of phosphoric acid employed in adhesive restorative dentistry.3
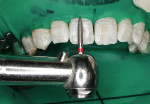
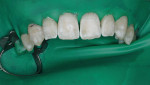
The facial surfaces of the teeth to be treated were lightly abraded with a fine grit (50 µm) diamond using a high-speed handpiece with air and water spray (Figure 3) to remove the superficial enamel dysmineralization layer to a depth of approximately 0.2 mm to 3 mm. After the completion of the rotary macroabrasion, the microabrasion paste (Opalustre™, Ultradent Products, Inc, https://www.ultradent.com) was applied to the facial surfaces of the maxillary teeth to be treated. Using a right-angle latch-type slow-speed handpiece running at 1000 revolutions per minute, a hybrid bristle brush cup was used to apply the microabrasion paste in three separate applications of 30 secs to 40 secs each (Figure 4). Between applications, the microabrasion paste was rinsed and dried from the tooth surfaces (Figure 5). Then, the etched enamel surfaces were polished with a series of silicone and rubber abrasives for smoothing and polishing the enamel surface. To remineralize the acid-etched enamel surface, the teeth were treated with a sodium fluoride (NUPRO®, Dentsply International, https://www.dentsply.com) and an amorphous calcium phosphate paste (MI Paste, GC America, Inc, https://www.gcamerica.com). Evaluation of the final color and appearance of the teeth was to be performed 1 week after treatment. Isolation with the dental dam and use of acid etching left the teeth demineralized, making final color evaluation impossible. The patient returned for color evaluation 3 days posttreatment. In case postoperative tooth bleaching was needed, an impression was made of the maxillary arch to create a cast for bleaching tray fabrication.
Phase II: Tray Bleaching
The patient returned 3 days posttreatment for evaluation of the color of the maxillary teeth treated (Figure 6). In the author’s experience, the removal of brownish-white enamel dysmineralization usually leaves the tooth slightly yellower than the original appearance. This, in fact, was seen in this patient. The decision to treat the maxillary arch with tray bleaching to further whiten the teeth was made. A bleaching tray was fabricated for the maxillary arch, and the patient was given a 15% carbamide peroxide with potassium nitrate and fluoride bleaching gel (Opalescence 15% PF, Ultradent Products, Inc, https://www.ultradent.com) to be used with overnight tray application for 3 weeks. The final result was esthetically acceptable for the patient (Figure 7). At 2 years, the tooth color was stable (Figure 8).
Commentary
Treatment with macroabrasion and microabrasion followed by tooth whitening using tray bleaching is a conservative, minimally invasive approach for discolored dentition when the diagnosis of the discoloration is enamel hypomineralization due to fluorosis, enamel dysmineralization due to trauma, or bacterial-mediated decalcification–remineralization staining. During childhood, the patient consumed multivitamins with fluoride and used a fluoride-containing toothpaste because his water supply lacked fluoride.
Most anticaries toothpastes for children are sweet, and the recommendation is to spit out the toothpaste but not rinse after brushing. Most young children swallow the toothpaste. Children who begin using fluoride-containing toothpaste before age 2 are at greater risk for enamel fluorosis; it has been accepted as a reasonable and minor consequence balanced against the substantial protection from dental caries. (For this patient, no restorations or caries were present.4) The recommendation for children is a pea-sized increment of fluoride toothpaste to be applied to a brush.4 Yet most toothpaste dispensing for children is probably unsupervised.
Dental professionals and pediatricians must have a better understanding of the avenues of fluoride ingestion for their patients. Commonly, before a dentist sees a young infant or child for a first dental visit, the pediatrician has been prescribing fluoride supplements and may be overlooking the amount that child already ingests. For this reason, dentists and dental hygienists should have dialogues with local pediatricians and primary care physicians to be certain they understand the optimal fluoride dose for young patients based on the real circumstances and beverages that may contain fluoride.
This patient described ingesting a higher-than-recommended amount of fluoride. This caused enamel hypomineralilzation due to retention of amelogenin proteins by fluoride, leading to fluorosis.5 Reconstituted juices and soft drinks from concentrates in bottling plants in metropolitan areas that contain fluoridated water can result in adequate fluoride intake. Prescription-strength fluoride drops may not be needed in infants and young children. For this patient, the closest major city was Burlington, Vermont, which began providing fluoridated water in 1952.
The minimally invasive treatment fulfilled the patient’s desire to have minimal maintenance of the treatment throughout his life. If the shade changes, the patient has the option to use tray bleaching for tooth whitening again. If adhesive resins or bonded porcelain had been used to change the appearance of the maxillary teeth, these restorations would likely need to be replaced at least several times in the patient’s life with additional removal of enamel during each treatment cycle. Various treatment options for minor color corrections are important. Dentists are urged to listen to patients’ desires for the final treatment outcome and then craft plans to fulfill the treatment goals.
Acknowledgments
The author would like to thank Alice K. Pazmino, DDS, and Cedric Pecor, DDS, who were instrumental in this patient’s care throughout all treatment phases.
Disclosure
The author has received grant/research support from Dentsply International, GC America, Inc, and Ultradent Products, Inc.
References
1. Coll JA, Jackson P, Strassler HE. Comparison of enamel microabrasion techniques: Prema Compound versus a 12-fluted finishing bur. J Esthet Dent. 1991;3(5):180-186.
2. Croll TP. Enamel microabrasion: concept development. In: Enamel Microabrasion. Chicago, IL: Quintessence Books; 1991:37-41.
3. Allen K, Agosta C, Estafan D. Using microabrasive material to remove fluorosis stains. J Am Dent Assoc. 2004;135(3):319-323.
4. Recommendations for using fluoride to prevent and control dental caries in the United States. CDC-MMWR Recommendations and Reports. https://www.cdc.gov/mmwr/preview/mmwrhtml/rr5014a1.htm. Accessed October 29, 2009.
5. Rozier RG. The prevalence and severity of enamel fluorosis in North American children. J Public Health Dent. 1999;59(4):239-246.
About the Author
Howard E. Strassler, DMD
Professor
Division of Operative Dentistry
University of Maryland Dental School
Baltimore, Maryland
Private Practice
Pikesville, Maryland