Removal of Invisalign Retention Attachments: A New Minimally Invasive Method
Jose Luis Ruiz, DDS; Werner J. Finger, Dr. med. dent., PhD; Hiromi Sasazaki, DDS, PhD; and Masahi Komatsu, DDS, PhD
Abstract
Removal of Invisalign® resin retention buttons without damaging underlying enamel is a major challenge. To date, the use of tungsten carbide burs is the most common and fastest—yet a risky—ablation method. Stainbuster®, a fiber-reinforced resin bur, has been introduced for removal of surface stains and resin remnants from tooth surfaces. This comparative in vitro and in vivo study proved that a combined technique, using multifluted tungsten carbide burs for fast removal of the bulk of resin followed by Stainbuster grinding for gentle removal of the final resin layer, is a safe and minimally invasive procedure for removing composite buttons from enamel.
Invisalign®, a method for straightening permanent teeth, was introduced to the market in 1997 (Align Technology, Inc, www.aligntech.com).1 According to the manufacturer, the system is based on the use of removable, clear polyurethane aligners that fit over the buccal, lingual/palatal, and occlusal surfaces of fully erupted permanent teeth. These computer-designed aligners are changed sequentially every 2 weeks and worn at least 20 hours a day. The aligners contain hemispheric depressions located over the teeth that must be filled with resin composite retention attachments. After cleaning and acid etching of the respective teeth, the depressions are filled with light-curing resin composite and placed in situ for light activation and polymerization. The manufacturer recommends the use of a highly filled composite, such as a hybrid or posterior composite. Bracket adhesives and flowable composites are discouraged by the manufacturer because of their hardness and wear properties.
At the end of the aligner treatment sequences, the retention attachments must be removed from the teeth. Often, tungsten carbide burs are used for this task. The procedure is similar to the removal of residual adhesive after bracket debonding, albeit occasionally more time-consuming, because a larger volume of resin must be removed. The most common methods to remove orthodontic resin are the use of orthodontic adhesive removal pliers for removing the bulk and then the use of the finishing burs/polishing burs to clean up any residue. With the pliers, dentists can remove the bulk of each attachment in approximately 2 secs—squeeze and it pops off. In many situations, even the residual composite can be removed with the pliers. When using pliers to remove the bulk of the retention attachments (eg, a bracket), the residual is often no greater than with brackets.
The primary requirement for removal of resin from teeth is to leave the enamel in its natural state, avoiding any iatrogenic trauma.2 Grooves and scratches do not disappear within a year, and adverse consequences may include increased plaque retention, staining, gingivitis, and demineralization.3-5 The most common methods for removing resin are low- or high-speed tungsten carbide burs, ultrasonic scalers, Nd:YAG laser ablation, and sandblasting.6-11 However, none of these methods proved fully satisfactory, with the most common failures being grooving, scratching, gouging, and remaining resin.12-17
Considering chairside time spent during resin removal, high-speed resin removal is a quicker yet probably riskier method with regard to enamel damage. With the large volume of resin composite attachments used after Invisalign treatment, the amount of allocation is important.
Recently, a new resin bur reinforced by zircon-rich glass fibers (Stainbuster, Abrasive Technology, Inc, www.abrasive-tech.com) was introduced with the claim that it gently and efficiently removes resin remnants. According to the manufacturer, the abrasive mechanism of these burs is explained by the presence of glass fiber ends covering the entire working surface. The fibers are split into small fragments as they act on a hard surface. At the same time, the resin matrix is used up, continuously exposing new fiber ends. These burs are said to be self-sharpening while maintaining their abrasive power.
The aim of this in vitro and in vivo study was to evaluate the suitability of these new fiber-resin burs for removal of Invisalign attachments when compared with conventional resin remnant removal techniques with high-speed tungsten-carbide burs, with regard to enamel surface alterations, and time spent to remove the attachments.
Methods and Materials
In Vitro Testing
Extracted human upper central incisor teeth, stored for a maximum of 3 months in 1% chloramine solution, were selected. The roots were removed close to the cementoenamel junction with diamond burs under copious water spray. The crowns then were placed in 20-mm wide and 10-mm high cylindrical rubber molds with the labial aspect facing the bottom of the mold and embedded in slow-curing epoxy resin (Lekutherm X-20, Bayer AG, www.bayer.com). After overnight curing at 37°C, the specimens were removed from the molds and wet-grinded on SiC paper (grits 180 to 600) until a sufficiently wide area of peripheral enamel was exposed for mounting of an Invisalign retention attachment. The attachment dimensions were determined from measurements of the manufacturer-made depressions on Invisalign aligners. The mean diameter was 3.5 mm and the mean depth 1 mm. A 12-mm wide and 2-mm deep cylindrical hole was lathe-cut in the end surface of a 16-mm wide and 15-mm high steel cylinder with a 2-mm wide central bore hole for insertion of a steel cylinder with a spherical top segment, 3.5-mm wide and 1-mm high (radius: 2.03 mm), equivalent to the dimension of a regular Invisalign attachment. At the other end, the steel pin with a screw thread was provided for fixing in the cylindrical hole of the main steel block with a screw nut. A 1.5-mm thick and 5-mm high steel ring fitting into the upper 12-mm wide bore hole was coated on the internal surface with adhesive and served as an “impression tray” for the transparent vinyl polysiloxane registration material (Memosil®; LOT 275323, Exp. 05-2009, Heraeus Kulzer, www.heraeus-kulzer-us.com).
Memosil was dispensed from a double-chamber cartridge through a static mixing tip into the seated steel ring, covered with a transparent strip, and pressed flush under a parallel hand press for 5 mins, where it set at ambient laboratory temperature. After removal of the impression, the semispheric hole was filled with light-curing resin composite and pressed on the 30-secs acid-etched (Gluma® Etch 35 Gel, LOT 275055, Exp. 04-2010, Heraeus Kulzer) rinsed-and-dried enamel until reaching the flat specimen surface. Then, it was light-activated through the silicone material for 60 secs (Translux® Energy, Heraeus Kulzer). Next, the excess composite around the attachment was removed with a sharp knife before final light-curing for another 60 secs. Ten specimens each were produced from resin composite materials: Venus™ (A2, hybrid type, LOT 010136, Exp. 09-2010, Heraeus Kulzer), Venus™ Flow (A2, hybrid-type, LOT 010116, Exp. 09-2010, Heraeaus Kulzer), Durafill® VS (A2, microfilled, LOT 010209, Exp. 05-2009, Heraeus Kulzer), and Filtek™ Supreme (A2, hybrid-type, LOT 4AP, Exp. 04-2007, 3M ESPE, www.3MESPE.com). All specimens were immersed in water (23°C) for at least 1 week before further processing.
The 10 specimens from each composite were subdivided randomly into two groups for attachment removal with carbide burs only (Midwest® bur No. FG7104, DENTSPLY Professional, www.dentsply.com) or for gross removal with these carbide burs followed by Stainbuster bur grinding (bur type: STB4002). The carbide burs were used with a turbine and effective water spray; the Stainbuster burs were applied with a contra-angle handpiece at low speed (approximately 10,000 revolutions per minute [rpm]) first under fine water spray and then when dry. All resin composite attachments were removed by the same operator. The total time needed for resin ablation until no resin remnants were detected was registered.
Each specimen was evaluated further under a stereomicroscope at 20-fold magnification according to the following criteria: adhesive remnant index (1 = none, 2 = little, 3 = gross remnants left); enamel appearance (1 = glossy, 2 = moderately shiny, 3 = dull); and enamel damage (1 = none, 2 = moderate, 3 = severe).
Additionally, scanning electron microscopy (SEM) and light microscopy photographs of one characteristic specimen of each group were taken. The treated enamel surfaces were analyzed morphologically with a noncontacting 3-dimensional (3D) roughness and topography measuring device (MicroProf® with FRT Mark III, Version 3.8 software, Fries Research and Technology GmbH, www.frt-gmbh.com). Areas of 1 mm by 1 mm were analyzed at 2-µm point distance in x-axis and y-axis directions and at 20-nm z-axis resolution. Roughness parameters (roughness average [Ra] and mean roughness depth [Rz]) were determined from the 3D profiles according to DIN EN ISO 4287.
In Vivo Testing
Seven patients were selected after finalized orthodontic treatment with Invisalign. Each patient was informed thoroughly about the trial and signed an informed consent form. Opposite quadrant teeth were allocated randomly for attachment removal with carbide burs (n = 21) or for gross removal with carbides and final grinding with Stainbuster burs (n = 22).
Carbide burs (Midwest bur No. FG7104) were used on a turbine under copious water spray; the Stainbuster burs were used on a microengine handpiece (Bien-Air Dental SA, www.bienair.com) at 10,000 rpm under slight water spray. After carbide-bur treatment, the enamel surfaces were polished for 30 secs with a fine-grit aluminum-oxide powder suspended in glycerine (Prisma® Gloss™, extra fine, DENTSPLY Caulk, www.caulk.com) applied in a rotating rubber cup. One operator performed all treatments under a 4.5-fold magnifying loupe. The total time for removal of each attachment was determined from the first bur contact until clinically no resin remnants were detected.
Photographs were taken of each treated tooth at 2:1 magnification (EOS 10D with macrolens EF 100 mm, Canon, Inc, www.canon.com). Additionally, full-arch double-phase impressions were taken in plastic stock trays with vinyl polysiloxane material (Flexitime® Correct Flow and Flexitime® Heavy Tray, Heraeus Kulzer) and cast in epoxy resin (Lekutherm X-20). The replicas of the treated teeth were removed with a diamond blade, seated on aluminum stubs, and Pt-sputtered for SEM investigation. The SEM photographs were evaluated in regard to the resin remnants left on the surface (resin removal index: 1 = none, 2 = little, 3 = gross resin remnants) and enamel damage (1 = none, 2 = moderate, 3 = severe).
Results
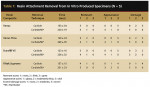
Table 1 summarizes the results of the in vitro resin attachment removal. As shown in the table and illustrated in Figure 1, attachment removal with carbide burs was a significantly faster procedure than gross removal with carbides followed by Stainbuster grinding (one-way analysis of variance [ANOVA]: P < .001). There was no significant difference in treatment time within each of the two experimental groups, irrespective of the resin composite material used (P > .05). From the 40 specimens treated, 34 showed no resin remnants and six specimens displayed small resin areas. In contrast, when enamel appearance was evaluated, none of the 20 specimens treated with carbides had a glossy surface, whereas after carbide plus Stainbuster treatment, 15 of the 20 specimens were highly glossy and five moderately shiny. A total of 19 carbide-treated samples had a dull appearance. Severe enamel damage was found in 12 of the 20 carbide-treated specimens and none in the carbide plus Stainbuster treatment group in which 18 samples showed no enamel damage.
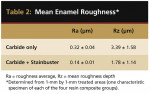
Figure 2 shows topographical characteristics for the two treatment regimens. The carbide-treated surfaces displayed grooves produced by inadvertent touching of the underlying enamel during attachment removal, whereas the enamel after carbide plus Stainbuster treatment displayed uniform and smooth surfaces. These findings were confirmed when the surface roughness parameters of the eight samples were evaluated, one for each of the four resin composite attachments with each of the two removal procedures (Table 2). Both Ra and Rz figures for the carbide-treated samples were approximately twice the roughness parameters for the carbide plus Stainbuster-treated specimens.
Table 3 summarizes the total clinical treatment time for the two removal procedures. The times given for the carbide bur removal procedure include the 30-second polishing sequence. Thus, on an average, the combined carbide and Stainbuster procedure is 30 secs longer than the carbide-only removal technique. The scores given for resin remnants and enamel damage were allocated from inspection of the replica SEMs at 20-fold magnification. Small resin areas were left on most of the teeth with both removal methods; only eight teeth were entirely free of resin. When carbides were used in combination with Stainbuster, resin areas covering approximately half of the target surface were seen on two teeth. Moderate and severe enamel scarring occurred in 12 and eight of the 21 teeth, respectively, when resin was removed with the carbide bur at high speed. In contrast, with the carbide plus Stainbuster technique, 11 teeth showed no enamel scarring; however, seven and four teeth showed evidence of scratching, grooving, and gouging and were classified as moderate and severe, respectively (Figure 3).
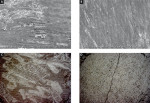
The SEMs in Figure 4 show characteristic enamel surface patterns found on the replicas made from the patients’ impressions. With carbide bur removal of the resin attachments, multiple enamel grooves are visible, whereas the carbide plus Stainbuster-treated enamel looks uniform, resembling a slightly sanded surface.
Discussion
Although it is incumbent on the clinician to select a resin ablation method that returns the enamel to as-near-as-possible the original condition without enamel scarring, the literature offers no clear advice on how to proceed. Various opinions exist concerning removal of resin after bracket debonding including multistep techniques.6,8,18,19 One of the often-applied methods is using a multifluted carbide bur for easy and fast resin ablation. In accordance with other authors, the results of the present study confirm this method is fast but also damaging to the enamel surface unless an additional polishing regimen is used.7,15,18 The clinical time required for resin attachment removal with tungsten carbide burs was between 2 and 2.5 mins for the in vitro treated samples and 1 to 1.5 mins when the attachments were removed in vivo. Another 30 secs, however, had to be added to the total in vivo cleaning time because final polishing according to the protocol and the clinical operator’s experience was requested. Presumably, the in vitro and in vivo time difference is related to the experience, force exerted, and vigor of the operator.8 The average time for in vitro resin removal with carbides followed by Stainbuster grinding was nearly 4 mins, in vivo 2 to 2.5 mins only. Therefore, the tungsten carbide burs are the most time-saving instruments. The type of resin used and the ablation method applied had no significant effect on the required time, although it could be hypothesized that at least the Stainbuster grinding effect would be different for the low-modulus and low-strength microfilled resin compared with the highly filled hybrid resins.
The results of this study demonstrate clearly that resin removal with carbide burs only is a considerably more hazardous procedure than gross removal with carbide burs followed by Stainbuster grinding. With both the in vitro and in vivo tests, moderate-to-severe scarring of the enamel was found in almost all cases. Similar enamel damage with the carbide-bur technique was reported in previous studies.3,16,18 Enamel grooving resembling a washboard pattern, as shown in Figure 3 and Figure 4, was the most frequent finding. Campbell2 and Howell and Weekes13 concluded enamel scarring following removal of bonded brackets is inevitable and therefore, the enamel always should be treated with a suitable polishing sequence. Another study reported high-speed tungsten carbide burs gave the least enamel surface roughness, however, resin remnants remained in more than 30% of all cases.4
The authors of this study hypothesize that the water spray had masked the operator’s ability to contrast between composite and enamel structure. In 27 of the 43 clinically treated teeth, resin remnants were detected, indicating that the contrast between resin composite and enamel was probably too little to detect remaining resin. Another explanation might be that the glossy surfaces, resulting from cutting and grinding, may hide remnants, in spite of careful inspection with magnifying lenses. The in vitro results prove, however, careful visual inspection of the specimens during bur cutting and/or grinding of the attached resin resulted in 34 of the 40 treated teeth exhibiting remnant-free enamel surfaces. Cutting after polishing with the extra-fine aluminum-oxide paste, as practiced during the clinical attachment removal, produces a high luster that makes it difficult to identify both grooves and resin remnants.
Kim et al5 evaluated the enamel surface texture after resin removal with a Talysurf roughness analyzer and found that the use of carbides at low speed and sandblasting gave similar results. In the trial presented, the mean surface roughness produced by bur cutting produced almost three times higher Ra and two times higher Rz than final grinding with Stainbuster burs. Howell and Weekes13 evaluated enamel surfaces subsequent to various debonding procedures by SEM using semiquantitative grading. They found that neither the bonding material nor the type of carbide bur selected had a significant effect on the quality of the finished enamel surface. Sof-Lex™ (3M ESPE) disc grinding followed by pumice slurry produced the roughest surface; pumice alone the smoothest surface. Figure 2 and Figure 3 demonstrate the surface texture of bur plus Stainbuster-treated enamel compared with bur cutting only. These observations indicate that the resin-fiber burs have a very gentle grinding or sanding effect on enamel. The SEM in Figure 4D reveals that the Stainbuster bur has evened minor scars produced on enamel by inadvertent bur scarring.
Conclusion
Removal of Invisalign resin attachments from enamel is time-consuming when the present method is used. The time of removal may, however, be significantly reduced when orthodontic adhesive removal pliers are used first to remove the bulk. This might be possible in many cases. When using pliers to remove the bulk of the retention attachments (eg, bracket), the residual is often no greater than with brackets. Use of high-speed tungsten carbide burs for fast resin ablation is hazardous and often results in enamel scarring. The newly introduced Stainbuster resin-fiber burs are valuable tools in the orthodontist’s armamentarium; they grind resin slowly and act minimal invasively on enamel. Therefore, a combined technique for removal of Invisalign resin attachments is suggested—preferably removal of the bulk of the retention attachment with adhesive removal pliers or cautious removal of the bulk resin part with a multifluted tungsten carbide bur, followed by Stainbuster grinding for removal of the final resin layer. The resin burs offer the advantage of visual control when used without water spray in the final stage because enamel appears immediately shiny on removal of resin remnants. The slightly longer treatment time is considered acceptable as a smooth enamel surface without resin remnants prevents staining, plaque accumulation, and thus demineralization through microbial activity.
Disclosure
The Stainbuster burs used in this study were donated by Abrasive Technology, Inc.
Acknowledgment
The authors would like to thank Thomas Molé for designing and constructing the device for production and seating of the Invisalign resin attachments.
References
1. Meier B, Wiemer KB, Miethke RR. Invisalign—patient profiling. Analysis of a prospective survey. J Orofac Orthop. 2003;64(5): 352-358.
2. Campbell PM. Enamel surfaces after bracket debonding. Angle Orthod. 1995;65(2): 103-110.
3. Schuler FS, von Waes H. SEM-evaluation of enamel surfaces after removal of fixed orthodontic appliances. Am J Dent. 2003;16(6):390-394.
4. Hong YH, Lew KK. Quantitative and qualitative assessment of enamel surface following five composite removal methods after bracket debonding. Eur J Orthod. 1995;17(2):121-128.
5. Kim SS, Park WK, Son WS, et al. Enamel surface evaluation after removal of orthodontic composite remnants by intraoral sandblasting: a 3-dimensional surface profilometry study. Am J Orthod Dentofacial Orthop. 2007;132(1): 71-76.
6. Krell KV, Courey JM, Bishara SE, et al. Orthodontic bracket removal using conventional and ultrasonic debonding techniques, enamel loss, and time requirements. Am J Orthod Dentofacial Orthop. 1993;103(3):258-266.
7. Retief DH, Denys FR. Finishing of enamel surfaces after debonding of orthodontic attachments. Am J Orthod. 1979;49(1):1-10.
8. Oliver RG, Griffiths J. Different techniques of residual composite removal following debonding—time taken and surface enamel appearance. Br J Orthod. 1992;19(2):131-137.
9. Thomas BW, Hook CR, Draughn RA. Laser-aided degradation of composite resin. Angle Orthod. 1996;66(4):281-286.
10. Alexander R, Xie J, Fried D. Selective removal of residual composite from dental enamel surfaces using the third harmonic of a Q-switched Nd:YAG laser. Lasers Surg Med. 2002;30(3):240-245.
11. Reisner KR, Levitt HL, Mante F. Enamel preparation for orthodontic bonding: a comparison between the use of a sandblaster and current techniques. Am J Orthod Dentofacial Orthop. 1997;111(4):366-373.
12. Fitzpatrick DA, Way DC. The effect of wear, acid etching, and bond removal on human enamel. Am J Orthod. 1977;72(6):671-681.
13. Howell S, Weekes WT. An electron microscopic evaluation of the enamel surface subsequent to various debonding procedures. Aust Dent J. 1990;35(3): 245-252.
14. Zachrisson BU, Årthun J. Enamel surface appearance after various debonding techniques. Am J Orthod. 1979;75(2):121-137.
15. Gwinnett AJ, Gorelick L. Microscopic evaluation of enamel after debonding: clinical application. Am J Orthod. 1977;71(6):651-665.
16. Zarrinnia K, Eid NM, Kehoe MJ. The effect of different debonding techniques on the enamel surface: an in vitro qualitative study. Am J Orthod Dentofacial Orthop. 1995;108(3):284-293.
17. Osorio R, Toledano M, García-Godoy F. Enamel surface morphology after bracket debonding. ASDC J Dent Child. 1998;65(5):313-317.
18. Eminkahyagi N, Arman A, Cetinsahin A, et al. Effect of resin removal methods on enamel and shear bond strength of rebonded brackets. Angle Orthod. 2006;76(2):314-321.
About the Authors
Jose Luis Ruiz, DDS
Director
Los Angeles Institute of Esthetic Dentistry
Los Angeles, California
Private Practice
Los Angeles, California
Werner J. Finger, Dr. med. dent., PhD
Professor
Department of Preclinical Dentistry
School of Dental Medicine
University of Cologne
Cologne, Germany
Visiting Professor
Tohoku University
Sendai, Japan
Hiromi Sasazaki, DDS, PhD
Lecturer
Graduate School of Dentistry
Department of Restorative Dentistry
Division of Operative Dentistry
Tohoku University
Sendai, Japan
Masahi Komatsu, DDS, PhD
Professor
Graduate School of Dentistry
Department of Restorative Dentistry
Division of Operative Dentistry
Tohoku University
Sendai, Japan