Is Centric Relation Always the Position of Choice for Temporomandibular Disorders? A Case Report of How TMD and Airway Dimension May Be Associated
William E. Harrell, Jr., DMD, C.DSM; Tim Tatum, DMD; and Mike Koslin, DMD
Abstract
Centric occlusion (CO) and centric relation (CR) have been controversial topics in dentistry for nearly a century. The concept of CR emerged as a result of the search for a reproducible mandibular position that would enable the prosthodontic rehabilitation of patients needing denture treatment. The case study presented is uncommon because of the following two questions: Which mandibular treatment splint position—CR or CO—was appropriate for the initial and eventual final treatment of this patient for her temporomandibular disorder/myofascial pain and dysfunction? Also, how might the mandibular position of CR and CO affect the size and shape of the airway? The airway’s size and shape is important because it relates to sleep-disordered breathing and potential obstructive sleep apnea later in life. The authors believe this is the first case report describing how mandibular position of CR and CO may affect not only TMJ position but also the airway shape and size in three dimensions.
Centric relation (CR) has been a controversial topic in dentistry for almost 100 years.1-6 The concept of CR emerged due to the search for a reproducible mandibular position that would enable prosthodontic rehabilitation, especially in patients needing dentures.7-10 More than 26 definitions of CR have been devised since the term was first developed in 1929 as a starting point for making dentures.8-10 It evolved into orthodontics, restorative dentistry, full-mouth reconstruction, and orthognathic surgery as a diagnostic and treatment position for natural teeth as a part of the gnathological concept of McCollum and Stallard and others.11-13
This case study involved a question of which initial mandibular treatment splint position—CR or CO—was appropriate for the beginning and, ultimately, the final treatment for this patient. It also entailed the problem of the patient’s temporomandibular disorders/myofascial pain and dysfunction and how the maxillary and mandibular position may affect the size and shape of the airway, which may relate to sleep-disordered breathing (SDB) and obstructive sleep apnea (OSA). The article describes an interdisciplinary approach to diagnosing and treating a case that initially presented with pain in the temporomandibular joints (TMJs) along with myofascial pain and dysfunction.
Case Report
A 17-year-old white female student, originally from Tennessee, was examined in Alabama by one of the authors (TT) with the chief complaint of bilateral headaches, TMJ pain, clicking, popping, and locking of the right TMJ. Her chief complaints were: “My bite feels off” and “I have excessive daytime sleepiness.” She had previous orthodontic treatment for an impacted maxillary right canine 2 years prior to seeing the present dentist. She also had a history of clicking and locking 4 years prior to her original orthodontic treatment.
Clinical Examination
Findings from the clinical examination by her dentist (TT) revealed all muscles of mastication had severe pain on palpation and during function. Palpation of the lateral pole and posterior aspect of the TMJs was painful. She had difficulty relaxing her jaw for the dentist to evaluate for any CO-CR discrepancy due to muscle splinting. Cold spray and stretch was used to help relax the muscles and allow the dentist to manipulate the patient’s jaw into CR. The dentist realized a large discrepancy between CO and CR. The mandible dropped back to the right side and created a significant shift of the midline and cross-bite relationship in a manipulated CR position. A maxillary CR splint was considered, but the dentist was concerned about what would happen to the patient’s bite and the consequences that might arise from placing her on a “standard” maxillary CR splint. The dentist then referred her for an orthodontic consultation (WH) and for anatomically accurate imaging with 3D cone-beam computed tomography (CBCT) (i-CAT®, Imaging Sciences International, i-cat.com) and 3D facial imaging (3dMD, 3dmd.com) for diagnosis and treatment planning.
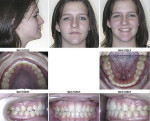
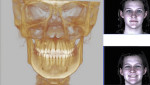
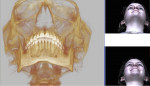
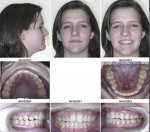
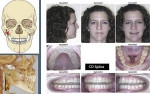
The patient presented clinically with a Class 1 occlusion, which looked normal in CO (Figure 1), and her face, skeletal, and dental structures were symmetric in her initial CO position (Figure 2 and Figure 3). She complained that her bite “feels off,” that her jaw and head hurt badly, and that she was not sleeping well and was tired throughout the day. The clinical examination revealed pain, especially in the left temporal and left masseter muscles, clicking, popping, and intermediate locking of the right TMJ. She had limited maximum opening of 32 mm (normal: 42 mm to 45 mm); limited lateral excursions with pain: right lateral = 0 mm, left lateral = 5 mm (normal: 10 mm to 12 mm); and limited protrusive movement of 4 mm (normal: 8 mm to 10 mm). She deviated to the right 4 mm on opening. Her pain-level score was 7 (visual analog scale [VAS]: 0-10). Because of her complaint of excessive daytime sleepiness, she completed an Epworth Sleepiness Scale (ESS)14 and received a score of 10. A score of 10 or more is considered sleepy and further evaluation should be done for possible SDB or OSA.
(The authors note that they would have liked to have done a polysomnography (PSG) on the patient but were unable to schedule it in time (there was 5-month wait), as the patient was on an accelerated timeframe due to her enlistment in the US Air Force. Their initial goal was to place the maxillary CO splint to support the TMJs and the airway day and night until they could obtain a sleep MD and PSG for evaluation, but they had to move forward due to the patient’s firm time constraint. Their focus was on the minimal cross-sectional area (MCSA) rather than volume changes. Since volume depends on how accurately the superior and inferior limits on sequential scans can be defined, which the authors believe is not highly accurate, MCSA was used, even though the MCSA position may change with jaw position and head posture. They did not perform any pulse oximetry. The patient’s Malampati index was 3 at her normal opening (not deviated to the right) and tongue position. The deviated opening to the right might have shown a different Malampati index.
3D Diagnostic Records
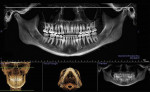
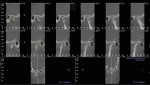
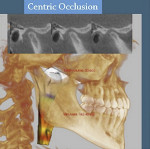
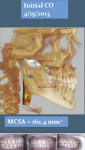
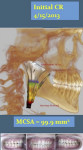
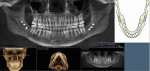
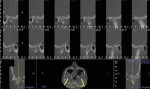
The patient’s initial centric occlusion 3D records included: 1) 2D facial and intraoral photographs in CO (Figure 1); 2) 3D CBCT in CO (Figure 2 and Figure 3) (15-μSv dose [compared to standard panoramic x-ray of 24+ μSv])15; and 3) 3D facial surface imaging in CO (Figure 2 and Figure 3). The CBCT scan was then reconstructed into a panoramic x-ray using a defined focal trough (Figure 4), a reconstructed TMJ series in CO (Figure 5), and a reconstructed airway volume and MCSA in CO (Figure 6), all from one CO CBCT scan. The MCSA of the patient’s airway, while she was in an upright and awake position in CO, was 162.4 mm2 (normal adult16: 155 mm2 to 160 mm2).
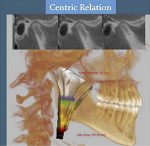
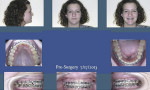
The patient’s initial CR 3D records with right condyle seated into fossa to first-tooth contact included: 1) initial 2D facial and intraoral photographs in CR (Figure 7); and 2) comparison of 3D CBCT of the TMJs and the airway in CO and CR (Figure 6 and Figure 8). The MCSA in CR was 99.9 mm2 (normal adult16: 155 mm to 160 mm2). The buccal cross-bite and midline shift to the right along with facial asymmetry can be observed in the CR records (Figure 7 and Figure 8).
Diagnosis
A diagnosis of osteochondritis (OC), ie, ideopathic condylar resorption (ICR), sometimes referred to as cheerleaders’ syndrome,17,18 was made. Typically occurring in females between 14 to 17 years of age, this condition is characterized by: an acute osteonecrosis of the condylar surface; a possible positive latex fixation or RA factor (Rheumatoid Factor of >25%) but does not recur; an inflammatory necrosis phase lasting 6 to 8 weeks with posterior capsulitis; a healing phase of 10 to 12 weeks; and a shortening of the joint to 2 mm to 3 mm in height but retaining its shape. It is believed that hormonal changes may be involved with ICR. Strain on the TMJs and genetics may also be factors.
After healing, the difference observed between OC and degenerative joint disease (DJD) is the joint space. In OC, the joint space looks normal but is reduced in height. In DJD, the joint space is reduced or even absent, and the condyles show regressive and progressive remodeling and sclerotic changes.17,18
Problems List
Clinically, the patient presented with a “normal” Class 1 bite relationship and a reasonably symmetric face in CO. This is the occlusal position in which the patient functioned and occluded during the day. Her left temporalis and left masseter muscles were painful and created a headache most of the day. At night her jaw would “fall over to the right” and not only create pain but she felt a choking sensation and did not sleep well. The CBCT evaluation revealed a distracted right condyle and a superiorly displaced left condyle in CO. Evaluation of the MCSA of the airway was normal at 162.4 mm2 in her CO position. Her CBCT scan in CR with the right condyle “seated” created a facial asymmetry and altered bite relationship, resulting in a significant malocclusion. Also, the MCSA of her CR airway collapsed to 99.9 mm2, which is a 38.5% difference.
The authors (WH and TT) reviewed her case via teleconference. They determined it was not appropriate to place a CR splint because this would encroach on the airway and physically reduce the airway’s size and shape. Taking a CBCT scan while the patient was in an upright and awake position is not the same as taking one while she is prone and asleep; however, the former position was this patient’s optimal airway. This meant that the airway would most likely be more constricted during sleep. The authors decided to place a maxillary CO splint (Figure 9) to stabilize the bite and TMJ joints into her more normal CO relationship and, more importantly, to support the airway by full-time wear, even when eating, as the patient had to alter her muscle function day and night to try to support her bite in CO. During sleep, her right condyle would seat and not only create a malocclusion but reduce the airway space, thus reducing airflow and possibly contributing to her SDB.
Orthognathic Surgical Plan
The patient was then referred to an oral surgeon (MK) for evaluation of how best to correct her TMJ issue and the bite relationship while also protecting the airway. The orthognathic surgical plan was to perform a 3-mm maxillary advancement and a bilateral sagittal split osteotomy (BSSO) to seat the right condyle onto the articular disc and reduce the torque from the left condyle. Her occlusion was set to her Class 1 position, and the face was kept in its initial symmetric position while protecting the airway.
Treatment Timeline
The authors were on an accelerated timeframe because the patient had enlisted in the US Air Force, and treatment needed to be completed before her service began. The patient had enlisted just after starting splint therapy and prior to orthodontic treatment, and the Air Force required a hard completion date of treatment before her basic training could be scheduled.
She was first seen by her dentist (TT) for initial TMJ examination on April 2, 2013. Two weeks later, she was seen by the orthodontist (WH) for an examination and 3D records. Based on a VAS (0-10), her TMJ pain level was 7, and her ESS score was 10 (considered sleepy). Two days after the orthodontist consultation, a maxillary CO splint was placed for full-time wear to support the right condyle and prevent the collapse of the airway. Approximately 2 weeks later, on April 29, a follow-up was done and the patient reported her TMJ pain level to be 0 and her ESS was 0.
After 6 weeks, full orthodontic appliances were indirectly bonded. Upper and lower nitinol arch wires measuring 0.017 mm x 0.025 mm were placed from first bicuspid to first bicuspid so that anterior alignment could occur. The maxillary splint was adjusted to initially accommodate only anterior tooth movement and for full-time use. Initially, the anterior lip of the upper splint was trimmed to allow alignment of maxillary cuspid to cuspid. The lower teeth were aligned, and the splint was adjusted weekly to maintain stability. Due to the initial alignment, minor tooth movement was needed. The splint was trimmed from the buccal of the posterior brackets, keeping the interproximal areas and lingual intact for retention. The lingual surfaces of the posterior teeth were relined as needed for stability. The clinicians also monitored her sleepiness scores during the treatment.
Two weeks later, upper and lower nitinol arch wires (0.017 mm x 0.025 mm) were placed molar to molar. The anterior section was relined to cap the incisors and cuspids for stability and to ensure no further movement. The inside of the splint (occlusal, buccal, and lingual) was trimmed from cuspid through first molar to accommodate posterior tooth movement. The late Dr. Bill Farrar (Normandie Study Group for TMJ Dysfunction) called this a Sved appliance,19 which could provide TMJ support while allowing rearranging of posterior and anterior teeth. The anterior segment and the upper second molar area were used to “tripod” the mandibular position. The splint was adjusted weekly.
Four weeks later (July 17), upper and lower stainless-steel arch wires measuring 0.017 mm x 0.025 mm were placed along with surgical hooks (Figure 10). The complete inside of the splint was relined for stability until surgery was completed. The orthognathic surgical plan was to perform a 3-mm maxillary advancement and a BSSO to seat the right condyle onto the articular disc and take the torque from the left condyle. The patient’s occlusion was set to her Class 1 position, and her face was kept in its initial symmetric position while protecting the airway.
The next day, orthognathic surgery was performed with an intermediate surgical splint to position the maxilla 3 mm anteriorly. Then a second surgical splint was used to orientate the mandible and condylar segments. Rigid fixation was used to stabilize the surgical segments.
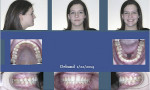
Because the patient was starting basic training in February, the orthodontist (WH) removed her braces in mid-January, 6 months after surgery, as opposed to the typical timeframe of 9 months (Figure 11). Fixed upper and lower 3-3 retainers were placed along with upper and lower clear Essix retainers (Dentsply Raintree Essix, essix.com). As of press time, the patient was functioning well with no pain or dysfunction. Her bite relationship was stable, and she reported no nighttime sleep issues or daytime sleepiness. Her ESS score was 0, and her TMJ VAS pain-level score was 0. Total treatment time was 9 months and 19 days.
Postoperative Follow-up and 3D Records
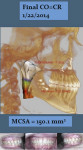
Figure 12, Figure 13, and Figure 14 show a comparison of initial CBCT scan in CO, initial CBCT scan in CR, and deband records. The airway changes can be visualized in three dimensions. The final CBCT scan (Figure 14) was taken the day of debanding, so some postsurgical edema was still present. Figure 15 is the final reconstructed panoramic x-ray, and Figure 16 is the final reconstructed TMJ series.
Conclusion
Though the concept of treating to CR is considered by many to be a stable position with the articular disc interposed in restorative dentistry and in orthodontics, some cases may seem minor based on a clinical examination and with only 2D imaging as the diagnostic modality. However, 2D imaging and a clinical examination do not always represent the “anatomic truth” and do not always reveal accurate diagnostic information.20
This case report demonstrated how a Class 1 bite and normal-looking face may not show the significance of the TMJ disorder and how this might relate to the size and shape of the airway, which could lead to SDB issues. Diagnosis and use of 3D imaging with CBCT scans of the airway dictated the initial treatment plan to stabilize the airway and also to stabilize the TMJs with a CO splint. The final treatment plan of orthodontics and orthognathic surgery to correct this skeletal, dental, TMJ, and airway problem was based not only on the clinical presentation but also on appropriate 3D findings. The case demonstrates the adage, “you cannot diagnose what you cannot see.”
Airway dimensional changes may occur from an altered position of the TMJs. If a patient who presents with a TMJ disorder has a CO-CR discrepancy, the clinician may be wise to also analyze the airway, not only in CO but in CR. This case report could have been more complete by having a pre- and post-sleep study (ie, PSG) for documentation of the patient’s sleep disturbance. A PSG by a sleep professional was recommended but was refused by the patient and her parents due to her school schedule and enlistment in the military.
About the Authors
William E. Harrell, Jr., DMD, CDSM
Board-Certified Orthodontist
Private Practice
Alexander City, Alabama
Tim Tatum, DMD
Restorative and Implant Dentistry
Private Practice
Opelika, Alabama (retired)
Mike Koslin, DMD
Oral and Maxillofacial Surgeon
Private Practice
Birmingham, Alabama
References
1. Rinchuse DJ, Kandasamy S. Centric relation: a historical and contemporary orthodontic perspective. J Am Dent Assoc. 2006;137(4):494-501.
2. Keshvad A, Winstanley RB. An appraisal of the literature on centric relation. Part I. J Oral Rehabil. 2000;27(10):823-833.
3. Keshvad A, Winstanley RB. An appraisal of the literature on centric relation. Part II. J Oral Rehabil. 2000;27(12):1013-1023.
4. Keshvad A, Winstanley RB. An appraisal of the literature on centric relation. Part III. J Oral Rehabil. 2001;28(1):55-63.
5. Palaskar JN, Murali R, Bansal S. Centric relation definition: a historical and contemporary prosthodontic perspective. J Indian Prosthodont Soc. 2013;13(3):149-154.
6. Lucia VO. Centric relation theory and practice. J Prosthet Dent. 1960;10(5):849-856.
7. Hickey JA. Centric relation, a must for complete dentures. Dent Clin North Am. 1964;8:587-600.
8. Academy of Denture Prosthetics. Glossary of prosthodontic terms. The Academy of Prosthodontics. J Prosthet Dent. 1956;692:5-34.
9. Academy of Denture Prosthetics. Glossary of prosthodontic terms. J Prosthet Dent. 1960;10:1200
10. Academy of Denture Prosthetics. Glossary of prosthodontic terms. J Prosthet Dent. 1977;38:66-109
11. Dawson PE. Centric relation. Its effect on occluso-muscle harmony. Dent Clin North Am. 1979;23(2):169-180.
12. Williamson EH. Laminagraphic study of mandibular condyle position when recording centric relation. J Prosthet Dent. 1978;39(5):561-564.
13. Stallard H. Dental articulation as an orthodontic aim. Journal American Dental Association and the Dental Cosmos. 1937;24(3): 347-376.
14. Johns MW. A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep. 1991;14(6):540-545.
15. Ludlow JB, Walker C. Assessment of phantom dosimetry and image quality of i-CAT FLX cone-beam computed tomography. Am J Orthodon Dentofacial Orthop. 2013;144(6):802-817.
16. Schendel SA, Hatcher D. Automated 3-dimensional airway analysis from cone-beam computed tomography data. J Oral Maxillofac Surg. 2010;68(3):696-701.
17. Farrar, WB, McCarty WL. A clinical outline of TMJ diagnosis and treatment. 7th ed, Montgomery, AL: Normandie Study Group for TMJ Dysfunction; 1982.
18. Wolford LM. Idiopathic condylar resorption of the temporomandibular joint in teenage girls (cheerleaders syndrome). Proc (Baylor University Medical Center). 2001;14(3):246-252.
19. Farha KF. Sved appliance. Cranio Clin Int. 1991;1(2):123-141.
20. Harrell WE, Hatcher DC, Bolt RL. In search of anatomic truth: 3-dimensional digital modeling and the future of orthodontics. Am J Orthod Dentofacial Orthop. 2002;122 (3):325-330.