Challenges in Treating Edge-to-Edge Incisal Position for Esthetics
Bozidar “Bole” Kuljic, DDS, FAGD
Abstract: Taking into consideration initial risk assessment, the clinician establishes criteria that are important for risk reduction. All too often, we see perfectly executed, and sometimes elaborate treatments that, in their essence, did not reduce but merely replaced one risk for the another. Careful analysis of the risks and benefits of the potential treatment can help the clinician avoid this. This case presents an adult opting for an acceptable alternative to costly, comprehensive, and time-consuming treatment by using a well-planned orthodontic and restorative plan, leading to satisfactory, stable results.
Restoring the edge-to-edge incisal position for esthetics is often challenging. The presenting skeletal and dental anatomy, etiology, risk factors, and patient preferences must be carefully considered as they affect the prognosis of dental restorations, dentition, and the esthetic result. Treating this kind of dental problem often requires utilization of two or more dental modalities to reach an acceptable outcome.1 In this case, minor oral surgery, limited orthodontic treatment, and restorative care were used to facilitate a desired esthetic improvement while decreasing the patient’s risk for further dental breakdown.
Clinical Case Overview
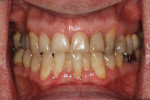
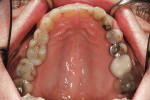
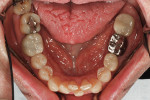
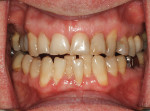
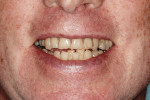
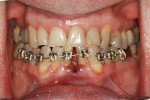
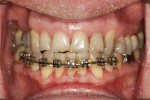
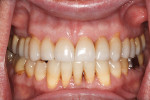
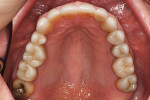
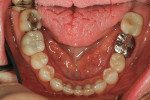
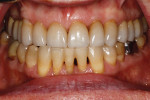
A healthy, 63-year-old male presented for dental care with a primary request to improve his smile. Specifically, he was concerned with lower anterior crowding, “jagged edges” of his upper anterior teeth, and the color and shape of his teeth (Figure 1 and Figure 2). The medical history was unremarkable, except for a successful total right hip replacement performed 9 months prior. His orthopedic surgeon recommended antibiotic prophylaxis for dental treatment. A review of the dental history revealed a moderate amount of restorative dental treatment throughout the patient’s lifetime, and he reported few significant issues in many years. He did note various teeth that had chipped or been broken in the past (Figure 3 and Figure 4). The upper right premolars had been removed many years ago; however, he was unable to recall the cause. He reported no problems with mastication, and he was not aware of any other dental issues.
Diagnosis, Risk Assessment, and Prognosis
Periodontal: Periodontal examination revealed localized probing depths of 2 mm to 4 mm with numerous bleeding points. Radiographically, horizontal bone loss of approximately 2 mm to 3 mm was observed throughout the dentition. Teeth Nos. 3, 6, and 11 each had 2 mm of recession with moderate cervical abrasion on teeth Nos. 3 and 6. The periodontal diagnosis was determined to be AAP type II (early periodontitis).
Risk: Low
Prognosis: Good
Biomechanical: Teeth Nos. 2, 3, 11, 13, and 31 were found to have questionable restorations. Overextended intracoronal restorations were noted on teeth Nos. 2, 3, 10, 12, 13, and 15. Active caries was not found; however, the posterior teeth with extensive, questionable restorations presented significant risk to their structural integrity. Upper and lower anterior teeth exhibited mild and moderate loss of incisal tooth structure.
Risk: High
Prognosis: Fair to poor
Functional: The patient had no reported problems with mastication and no signs or symptoms of temporomandibular dysfunction. Occluding surfaces exhibited moderate wear and chipping on the upper anterior teeth and mild wear on the lower anterior teeth. The patient denied any chipping or breakage had occurred in the last 5 years. As there were no signs of active occlusal disease or temporomandibular dysfunction, a reasonable inference was made that the current damage to the teeth was from previous occlusal dysfunction or a constricted chewing pattern (Figure 5).
Risk: Low (acceptable function)
Prognosis: Good
Dentofacial: Moderate anterior tooth presentation was noted as the patient smiled (Figure 6).
Due to the wear of the upper incisors, a reverse smile line presented, which negatively influenced the patient’s smile characteristics. The maxillary midline was approximately 2 mm to 3 mm to the right due to the early loss of teeth Nos. 4 and 5; however, the midline asymmetry did not concern the patient. Upper-arch gingival architecture was acceptable, except for teeth Nos. 6 and 11 with 1-mm and 2-mm recession, respectively. While smiling, low lip dynamics and moderate tooth display never revealed the cervical regions of tooth structure, so this was not considered a problem to the patient or clinician.
Risk: Moderate
Prognosis: Fair to good
Treatment Goals
The treatment goals were created by scale of importance to the patient and by objective risk assessment of all pertinent dental conditions.2
Treatment goals were to: 1) treat, stabilize, and maintain the periodontium by providing conservative periodontal therapy, systemic antibiotics,3 and re-care maintenance; 2) improve smile characteristics by increasing maxillary tooth length and increasing vertical dimension of occlusion (VDO) with ceramic restorations while correcting the lower anterior crowding orthodontically; and 3) minimize biomechanical risk by restoring questionable restorations and enhancing the occlusion with equal-intensity, bilateral, and simultaneous posterior contacts.4
Treatment Plan
For this patient, current dental technology presented several options for ideal correction, including orthognathic surgery. Risk-to-benefit ratios, patient tolerance, and the clinician’s judgment were necessary to render an acceptable plan. The treatment would be divided into four phases and was expected to take 10 to 12 months. The patient was comfortable with the goals and phases.
Scaling and root planing, along with the use of systemic antibiotics (amoxicillin 500 mg, tid for 8 days; metronidazole 500 mg, tid for 8 days), would be needed. Then, extraction of tooth No. 24 would be completed. Because of the extreme labial position of tooth No. 24 and the lingual and supererupted positions of teeth Nos. 23 and 25, any attempt to improve the esthetic outcome solely by restorative means would require unnecessary removal of the tooth structure. Doing so would elevate the biomechanical risk.
Limited orthodontic therapy would be required to align all lower anterior teeth. The extreme crowding in lower incisors area did not allow for porcelain veneers to be considered for two reasons: first, teeth Nos. 23 and 25 were overerupted and would need to be incisally reduced to the point of endodontic consideration before being used for porcelain veneers. Secondly, tooth No. 24 was displaced out of the lower dental arch and, to prepare this tooth for a porcelain veneer, one would need to perform maximum buccal reduction. That would, without a doubt, cause a major shift in the biomechanical risk, requiring intentional endodontic treatment as a mandatory step before creating optimal space for restoration.
For restoration of the maxillary arch, most of the maxillary posterior teeth would benefit from cohesively retained full-coverage restorations.5 Improved proportions for the maxillary anterior teeth could reasonably be gained by increasing the VDO and adding to the incisal length with ceramic restorations.
Treatment Phases
Phase 1:
Periodontal Therapy
Scaling and root planing was accompanied with the use of systemic antibiotics. Metronidazole and amoxicillin have been shown to enhance the results of scaling and root planing.
Phase 2:
Extraction and Orthodontic Treatment
Tooth No. 24 was removed and limited orthodontic treatment was initiated to align the lower anterior teeth (Figure 7). The patient, while being open to various treatment modalities to achieve his goals, was not willing to commit to either extended treatment times for an ideal orthodontic result or orthognathic surgery. To correct lower anterior crowding, several options were considered: removal of teeth Nos. 23 to 26 and placement of a canine-supported bridge, removal of teeth Nos. 23 to 26 and an implant-supported bridge with implants at the Nos. 23 and 26 sites, and removal of tooth No. 24 with alignment of the remaining incisors utilizing limited orthodontics. With reasonable periodontal and biomechanical prognoses for the remaining lower incisors, the latter plan was acceptable. While being an already acceptable compromise, limited orthodontic treatment presented another challenge; during orthodontic treatment, teeth move in many directions and may have the tendency to tip labially. In this case, labial tipping of the lower incisors might create an unwanted anterior cross bite. Removal of tooth No. 24 allowed for the reduction of the perimeter of the lower arch, and with interproximal stripping between teeth Nos. 22 to 27,6 lingual tipping of the remaining incisors was achieved. Thus, a satisfactory interincisal relationship was maintained (Figure 8).
Phase 3:
Diagnostic Wax-Up of the Upper Arch
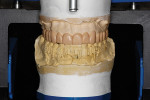
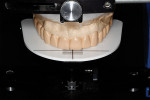
The patient’s maxillary cast was mounted using the Kois Dentofacial Analyzer on a Panadent articulator (Panadent, panadent.com) (Figure 9). The diagnostic wax-up of the upper arch was made using the wax-up platform of the analyzer, and the precise smile line of the future restorations was achieved7 (Figure 10).
Phase 4:
Restorative-Maxillary Restorations
After waiting 6 months for retention following orthodontic treatment the upper arch, except tooth No. 1, was restored at the new VDO, allowing for the planned length-to-width proportion changes and a slight overbite and overjet relationship. The right-side cross-bite was restoratively corrected by the shape of the new restorations (Figure 11). The anterior teeth were conservatively prepared, preserving as much enamel as possible to provide ideal cementation for adhesively retained porcelain restorations. Incisal-edge 2-mm reduction allowed for better esthetics and control of the anterior-posterior position.
Biomechanical risk for the questionable posterior restorations was reduced by the fabrication of full-coverage cohesively retained restorations (Figure 12 and Figure 13). All posterior teeth that had questionable restorations were prepared for full-coverage e.max® crowns (Ivoclar Vivadent, ivoclarvivadent.com). On the other hand, the anterior teeth were prepared to receive partial-coverage restorations and adhesively retained by using dual-cured resin cement. The anterior teeth were restored utilizing e.max. The maxillary restorations were delivered in a single appointment, utilizing an intraorally fabricated maxillary deprogrammer. The deprogrammer allowed for precise final adjustments of the maxillary restorations into occlusion. The treatment was finished in a timely manner respecting all of the patient’s desires (Figure 14). The active orthodontic treatment time was 5 months, followed by a 6-month retention period before the final restorative phase.
Discussion
Taking into consideration the initial risk assessment, the clinician establishes criteria that are important for risk reduction. All too often, we see perfectly executed, and sometimes elaborate treatments that, in their essence, did not reduce but merely replaced one risk for the another (eg, esthetic risk for biomechanical risk). That can be avoided, but only through thorough analysis of risks and benefits of the potential treatment. Understanding and predicting most, if not all, limitations of contemplated modalities and having a coherent and well-thought process that follows a series of sequential steps allow the dentist to easily navigate through the restorative challenges that would otherwise lead to undesirable results.
Conclusion
The edge-to-edge position of the front teeth is often a restorative challenge. If patients are fervently opposed to optimal comprehensive orthodontic treatment or surgery, both upper and lower teeth need to be considered and included in the final restorative planning. This article attempted to present an acceptable alternative to comprehensive orthodontics by utilizing limited orthodontic treatment in the lower arch, thus reducing the length of treatment and total cost while maintaining a predictable and desirable result. The patient has been followed for more than 2 years. The restorations, alignment, function, and periodontal condition are all stable, and he remains pleased with the outcome (Figure 15).
About the Author
Bozidar “Bole” Kuljic, DDS, FAGD
Private Practice
Beverly, MA, and Newburyport, MA
References
1. Roblee RD. Interdisciplinary Dentofacial Therapy: A Comprehensive Approach to Optimal Patient Care. Hanover Park, IL: Quintessence Publishing Co, Inc; 1994.
2. Kois DE, Kois JC. Comprehensive risk-based diagnostically driven treatment planning: developing sequentially generated treatment. Dent Clin North Am. 2015;59(3):593-608.
3. Slots J. Periodontology: past, present, perspectives. Periodontol 2000. 2013;62(1):7-19.
4. Kois JC, Phillips KM. Occlusal vertical dimension: alternation concerns. Compend Contin Educ Dent. 1997;18(12):1169-1174, 1176-1177; quiz 1180.
5. Janus CE, Unger JW, Best AM. Survival analysis of complete veneer crowns vs. multisurface restorations: a dental school patient population. J Dent Educ. 2006;70(10):1098-1104.
6. Kois DE, Kois JC. Comprehensive risk-based diagnostically driven treatment planning: developing sequentially generated treatment. Dent Clin North Am. 2015;59(3):593-608.
7. Tjan AH, Miller GD, The JG. Some esthetic factors in a smile. J Prosthet Dent. 1984;51(1):24-28.