To Graft or Not to Graft Anterior Extraction Sockets
Dennis Tarnow, DDS; Brian L. Mealey, DDS, MS; and Barry P. Levin, DMD
Should clinicians graft anterior extraction sockets?
Dennis Tarnow, DDS
Director of Dental Implant Education, Clinical Professor, Department of Periodontology, College of Dental Medicine, Columbia University, New York, New York; Private Practice, Surgical Implantology and Prosthodontics, New York, New York
Whether to use a graft in anterior extraction sockets is certainly a great question that clinicians must address each day. If the clinician wants to make sure the overall dimension of the ridge has minimal change, then a graft placement would certainly be advisable. This and the flapless removal of the tooth are key to minimizing the shrinkage of the ridge after an extraction. In our research, placing a graft into the gap along with palatal placement of the implant toward the cingulum and placing a provisional restoration to support the free gingiva is the best combination to preserve the shape of the ridge. This is certainly the case when the labial plate of bone is intact. We must remember that placing a graft will not stop some resorption of the labial plate of bone; however, placing the graft along with an implant and a provisional at the time of extraction can minimize the decrease in the shape of the ridge. This palatal placement will allow for bone to grow into the gap and create new, thicker bone on the labial of the implant after healing.
If the labial plate of bone is missing, the clinician can start rebuilding the buccal plate by placing a membrane against the buccal tissues while placing a graft into the socket. It has also been shown that one can just do nothing at the time of extraction if the buccal plate is missing and let the socket fill in with bone and tissue for about 6 to 8 weeks. At that time, the clinician can do all the grafting along with placement of the implant. Waiting the 8 weeks will let the soft tissue close over the socket and allow for an easier graft procedure. It will also enable any inflammation or infection, if present in the socket, to resolve before implant placement.
One must remember that the amount of calcified bone that fills into a socket is mostly based on the density of the bone surrounding the socket. In other words, if 2 teeth are removed in the same patient on the same day, and one is a lower cuspid and another is a maxillary molar, then the amount of calcified bone filling that socket at 6 months will be very different. The cuspid socket will be genetically pre-coded to fill with dense bone (type 1 or 2) and the molar will be pre-coded to fill with softer bone (type 3 or 4). This is why most socket studies looking at the density of bone, unless they are bilateral paired lesions in the same person, are highly open to variability.
Research findings are now pointing to placing an implant and a mineralized graft into the gap between the implant and the labial plate of bone. If the buccal plate is missing after extraction, then grafting the socket with a membrane in the facial part of the socket along with a graft can be beneficial or allowing the socket heal for about 8 weeks and then do grafting of the facial place of bone along with the implant placement at the same time.
Brian L. Mealey, DDS, MS
Professor and Graduate Program Director, Department of Periodontics, University of Texas Health Science Center at San Antonio Dental School, San Antonio, Texas
After tooth extraction, bundle bone lining the socket is resorbed and eventually remodeled with woven bone.1 This remodeling results in marked dimensional changes of the alveolus, with reduction in ridge height and width occurring rapidly following extraction.2-4 In a classic study of postextraction clinical healing events, the loss of ridge width reached 50%, with reduction of ridge width from 12 mm before extraction to 5.9 mm 1 year after extraction; most of this change occurs within the first 3 months of healing.3 This loss of alveolar ridge dimension occurs regardless of factors such as buccal plate thickness or tooth type, although thinner buccal plates are associated with a greater loss of ridge width.5
Systematic reviews have examined human clinical studies on alveolar ridge changes after tooth extraction when ridge preservation bone grafting was not performed. One systematic review reported an average reduction of approximately 3.9 mm in ridge width after extraction.4 Another reported a hard-tissue horizontal reduction of 3.8 mm (loss of 29% to 63% of original pre-extraction ridge width) and vertical reduction of 1.24 mm (loss of 11% to 22% of ridge height).6 Most of the reduction in ridge width and height occurred during the first 3 to 6 months after extraction.
The use of alveolar ridge preservation is aimed at preventing or minimizing dimensional changes following tooth extraction to provide an adequate volume and quality of bone for dental implant placement. Extraction sites treated with alveolar ridge preservation have been shown repeatedly to have significantly less dimensional change both vertically and horizontally when compared with controls not treated with ridge-preservation procedures.6-9 In addition, the need for additional bone grafting at the time of dental implant placement, such as grafting to cover exposed implant surfaces, is markedly lower when ridge-preservation grafting has been performed at the time of tooth extraction.10 Alveolar ridge preservation can be accomplished successfully using a variety of materials, such as allografts, xenografts, autografts, and alloplasts.8,9 Our research group at the University of Texas School of Dentistry in San Antonio has published 8 studies in the last 5 years examining histologic and clinical results following ridge preservation with a variety of allograft, xenograft, and alloplast materials. While vital bone formation varies considerably with the type of material used for grafting, we have repeatedly seen that ridge preservation results in much smaller vertical and horizontal alveolar ridge dimensional changes than those seen in studies of extraction without ridge preservation.
A large body of high-level scientific evidence supports the use of ridge preservation in non-molar tooth sites to minimize loss of alveolar bone dimension following tooth extraction. The body of evidence supporting ridge preservation is much larger when considering non-molar tooth sites rather than molar tooth sites simply because non-molar sites have been studied more. I cannot think of a reason not to perform ridge preservation in non-molar sites. Reduction in bone volume is problematic when dental implant therapy is anticipated, as the remaining alveolus may not be suitable for placement of a dental implant in an appropriate restoratively driven position and may require bone augmentation to reconstruct the ridge. If a dental implant is not the chosen treatment option and a fixed or removable tooth-borne dental prosthesis is used instead, it is often desirable to prevent loss of bone volume at the extraction site for esthetics and functionality. Patients who decline the dental implant option today may change their minds at a later date. Without ridge preservation at the time of tooth extraction, a much larger and costlier ridge-augmentation procedure may be needed.
Barry P. Levin, DMD
Diplomate, American Board of Periodontology, Clinical Associate Professor, Department of Periodontology, University of Pennsylvania, Philadelphia, Pennsylvania; Private Practice Limited to Periodontics and Implant Surgery; Elkins Park, Pennsylvania
When teeth are extracted, the initial void or socket eventually heals with new bone formation. After stating the obvious, the future of the anterior region of the dentition is the focus for this discussion. Though extraction sites heal,11 with the exception of those in patients with negative systemic and/or local factors, dentists must anticipate how these teeth will be replaced. Will the patient receive a fixed bridge or removable partial denture, or are dental implants planned?
For the purpose of answering the question (graft or don’t graft), immediate placement will not be discussed here. This discussion will focus on those sites contraindicated for immediate placement.
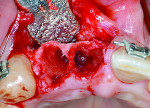
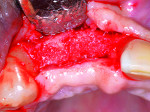
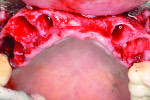
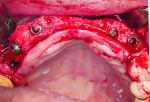
Ridge resorption will predictably occur following tooth loss.3 Although sites with thicker buccal and palatal bone walls undergo less resorption, it is unavoidable to some extent in most cases. In the anterior maxilla, for instance, a thin facial plate is present in the most situations.12 It is rare that this will not, in some manner, negatively affect dental rehabilitation. In the case of a fixed partial denture (FPD), the pontic space often becomes a concave defect, leading to food and plaque accumulation, which can cause caries of the abutment teeth and esthetic compromise. Removable prostheses are partially tissue-borne. As the alveolar ridge resorbs, adjustments, relines, and remakes are common. When implants are planned, esthetic and occlusal success is dependent on the implant’s position being optimal in three dimensions. All three scenarios lend themselves to additive or augmentative steps being performed after tooth extraction. Figure 1 through Figure 4 demonstrate the beneficial effect of socket grafting to facilitate implant placement 4 to 6 months after augmentation.
The case for grafting extraction sites is well supported in the literature.12 If dental implants are planned, the goal of grafting is ridge-dimension stability and osseointegration. Therefore, a graft capable of substitution with vital bone is necessary. The author’s preference for these sites is a mineralized bone allograft: freeze-dried bone allograft (FDBA). This material’s mineralized property serves well as an osteoconductive, but replaceable, bone graft.
In sites where a pontic is anticipated or a removable prosthesis is planned, a mineralized xenograft, which is osteoconductive but slowly resorbing, is preferred.
The overlying soft tissue also plays a critical role in these sites. A case with a naturally occurring thick periodontal phenotype typically can be treated with a cross-linked collagen membrane, because the only desired property of the membrane is to exclude soft tissue during the early bone formation period. For a case with thinner soft tissues, it may be more practical to use a dermal allograft, capable of barrier function, but also tissue thickening. This can be important in esthetic areas of the dentition and when ovate pontics are utilized in FPDs. Autogenous connective tissue grafts can also be used in the most critical esthetic areas.
The primary disadvantages of routinely augmenting extraction sockets are the additional costs and longer treatment times associated with these procedures. Especially when a non-implant solution is chosen, it can be challenging to justify to patients why these auxiliary steps are required. The use of visual aids, such as photographs and diagrams, providing examples of the differences between the two options is often effective in pointing out the benefits to these measures.
References
1. Araujo MG, Lindhe J. Dimensional ridge alterations following tooth extraction: an experimental study in the dog. J Clin Periodontol. 2005;32(2):212-218.
2. Tan WL, Wong TL, Wong MC, Lang NP. A systematic review of post-extractional alveolar hard and soft tissue dimensional changes in humans. Clin Oral Implants Res. 2012;23 Suppl 5:1-21.
3. Schropp L, Wenzel A, Kostopoulos L, Karring T. Bone healing and soft tissue contour changes following single-tooth extraction: a clinical and radiographic 12-month prospective study. Int J Periodontics Restorative Dent. 2003;23(4):313-323.
4. Van der Weijden F, Dell’Acqua F, Slot DE. Alveolar bone dimensional changes of post-extraction sockets in humans: a systematic review. J Clin Periodontol. 2009;36(12):1048-1058.
5. Cardaropoli D, Tamagnone L, Roffredo A, Gaveglio L. Relationship between the buccal bone plate thickness and the healing of postextraction sockets with/without ridge preservation. Int J Periodontics Restorative Dent. 2014;34(2):211-217.
6. Frost N, Banjar A, Galloway P, et al. The decision-making process for ridge preservation procedures after tooth extraction. Clin Adv Periodontics. 2014;4(1):56-63.
7. Iasella J, Greenwell H, Miller R, et al. Ridge preservation with freeze-dried bone allograft and a collagen membrane compared to extraction alone for implant site development: a clinical and histologic study in humans. J Periodontol. 2003;74(7):990-999.
8. Chan HL, Lin GH, Fu JH, Wang HL. Alterations in bone quality after socket preservation with grafting materials: a systematic review. Int J Oral Maxillofac Implants. 2013;28(3):710-720.
9. Avila-Ortiz G, Elangovan S, Kramer KW, et al. Effect of alveolar ridge preservation after tooth extraction: a systematic review and meta-analysis. J Dent Res. 2014;93(10):950-958.
10. Cardaropoli D, Tamagnone L, Roffredo A, Gaveglio L. Evaluation of dental implants placed in preserved and nonpreserved postextraction ridges: a 12-month postloading study. Int J Periodontics Restorative Dent. 2015;35(5):677-685.
11. Boyne PJ. Osseous repair of the postextraction alveolus in man. Oral Surg Oral Med Oral Pathol. 1966;21(6):805-813.
12. Younes F, Eghbali A, Raes M, et al. Relationship between buccal bone and gingival thickness revisited using non-invasive methods. Clin Oral Implants Res. 2016;27(5):523-528.