Oral Rehabilitation and Psychosocial Evaluation of a Patient with Bulimia Nervosa Following Teeth in a Day® Immediate Loading Protocol
Thomas J. Balshi, DDS, PhD, FACP; Glenn J. Wolfinger, DMD, FACP; Stephen G. Alfano, DDS, MS, FACP; J. Neil Della Croce, DMD, MS; and Stephen F. Balshi, MBE
Abstract
PURPOSE: The purpose of this patient report is to accurately portray the clinical experience of treating an active bulimic patient by employing an immediately loaded dental implant protocol to provide the patient with an expedited esthetic and functional result. Implementation of a psychometric component statistically quantifies the psychological effects of the oral rehabilitation.
MATERIALS AND METHODS: A 34-year-old woman presented with severe dental perimolysis (erosion) resulting from a 28-year history of bulimic behaviors. Clinical and radiographic evaluation of the existing dentition indicated advanced dental erosion and previous restoration attempts in a state of failure. The patient’s existing teeth were extracted and treated with full maxillary and mandibular implant-supported prostheses, following the Teeth in a Day® (TIAD) immediate functional loading protocol. Psychometric assessment was conducted through administration of a 20-item questionnaire, as seen in previous literature.
RESULTS: Radiographic and clinical analysis suggested all implant fixtures to be viable and accompanied by normal levels of alveolar bone 7 months into treatment. Questionnaire results at the new-patient presentation (T1) resulted in a composite score of 4.0 (SD = 2.9; P = 0.004), indicating severe body-image dysphoria. At 3 months postoperative (T2), the questionnaire score was 0.4 (SD = -1.7; P = 0.09). The final psychometric questionnaire at 7 months (T3) resulted in a score of 0.5 (SD = -1.5; P = 0.12). The patient was followed for a total of 7 years following implant placement. CONCLUSION: In this patient report, oral rehabilitation using the TIAD protocol provided an expedited and predictable alternative method for restoring functional abilities, esthetics, and self-esteem to a severely depressed bulimic patient. Psychometrically, at the postoperative (T2) and final testing period (T3), the patient’s body image profile was no longer considered to be significantly different from established normative values.
Current estimates suggest more than 70 million individuals are affected by eating disorders worldwide.1 In the United States, 20 million women and 10 million men suffer from a clinically significant eating disorder at some time in their life, including anorexia nervosa, bulimia nervosa, binge eating disorder, or an eating disorder not otherwise specified (EDNOS).2 Unfortunately, due to the secretive nature of these disorders, it is likely that these figures are much higher. Despite a steady increase in the frequency of both anorexia nervosa and bulimia nervosa in the last 2 decades, the etiology of eating disorders is considered mainly multifactorial in nature; no one single causative factor can be identified. It has been theorized that a combination of factors, both biological and psychological, combine to produce the disorder’s characteristic starvation, overeating, and purging.
Bulimia Nervosa
Bulimia nervosa, an eating disorder rooted in severe psychological neuroses, affects an estimated 7.5 million Americans.3 Typically, a person diagnosed with bulimia is female, Caucasian, 16 to 35 years old, single, college educated, and from an upper middle class family. However, eating disorder cases have been documented and reported in individuals as young as 6 years of age in some premenarcheal females.4 In fact, 81% of 10-year-old girls have reported being “afraid” of being fat, and 42% of girls in first through third grade described a desire to be thinner. Therefore, concerns about young children’s irregular eating behaviors must be thoroughly investigated before the behavior is considered transitory. It should be noted that girls with eating disorders at an early age present with very different manifestations (short stature, inadequate weight gain, growth retardation, delayed pubertal development) than their elder counterparts who acquire the disease at a later stage in life and are considered to develop a more “typical” symptomology.4
Manifestations of neuroses associated with bulimia may include an obsessive concern with body shape, fear of obesity, guilt, depression, and/or low self-esteem.3,5-8 Additionally, while demonstrating a voracious “binge” appetite for large quantities of food, bulimic patients typically express an exaggerated anxiety about increased body weight.5-7 As a result, some resort to evacuating ingested food through excessive use of laxatives. Individuals using laxatives find the need for laxatives increases as the body adapts to laxative use. Individuals may reach the need for over 60 laxatives in a day in order to get the same effect as when they started on just a few per day. Prolonged laxative abuse leads to a lethargic colon and the resulting problems with defecation.
Others resort to self-induced vomiting, referred to as “purging” episodes.7,9 The patient can be regurgitating as many as five or six times in a day. The frequency of binging and purging episodes varies greatly among known bulimic patients. Mitchell et al estimate the average number of purging episodes related to bulimia nervosa as being 11.7 times per week, with a striking peak report of 140 episodes.10 The clinical implications on enamel from such practices, resulting in an increased frequency of exposure to acidic vomitus, cannot be discounted or considered transient to the dentate state of a bulimic patient. These excessive regurgitation events frequently expose the hydrochloric acid from the stomach to the esophagus, pharynx, and oral cavity, creating an unhealthy oral condition and increased possibility of rupture of the esophagus, which can cause bleeding and risk of mortality.
The purging episodes are usually accompanied by prior “binge” episodes. A bulimic can binge anywhere between 1,000 to 60,000 calories at a single time over a 1- to 2-hour span.11 Feelings of panic, disgust, guilt, or depression typically set in after the behaviors are realized as being abnormal (characteristic of bulimic patients), and the individual soon recognizes the need to purge, often minutes after the binge.
It must be acknowledged that an eating disorder is a chronic syndrome that is complex, multi-symptom, and does not always fit stereotypical persons or behaviors. There are plenty of individuals who have characteristics of disordered eating in the United States and beyond with a broad range of symptoms and dysfunctional behaviors.
According to American Psychiatric Association (APA), clinical features of eating disorders indeed vary, but criteria from the Diagnostic and Statistical Manual of Mental Disorders, 5th edition (DSM 5) serve as a guide to establish a diagnosis in a majority of cases.8,12 Although each individual with an eating disorder displays unique qualities, the pervasive characteristics of these individuals includes an unhealthy weight, refusal to eat, and a disturbance in how they view their body. However, variants of disordered eating that do not meet the diagnostic criteria of anorexia or bulimia nervosa have been reported and studied.9 These are referred to as eating disorders not otherwise specified (EDNOS), which also require treatment and should not be dismissed.9 Individuals with bulimia, as is the focus of this discussion, range in size from small to morbidly obese, and they can gain or lose many pounds in short periods of time. In addition, behaviors may stem from issues such as low self-esteem and a need to use eating as a coping mechanism for emotional issues such as depression, anger, and pain.9
Accordingly, besides self-esteem, individuals who participate in these behaviors usually experience shame and an overall depreciation in their quality of life.11 Self-perception is greatly influenced by their “distorted” body shape and weight. Individuals with bulimia may feel out of control and abnormal and conjure up feelings of shame and depression. Clearly, a decrepit and failing dentition can exacerbate these innately intense emotional responses.
Along with physicians, psychiatrists, nurses, dietitians, psychologists, social workers, parents, teachers, and coaches, there is a pressing need for oral healthcare professionals to be a part of the patient’s eating disorder healthcare team. The dental professional or surgical provider is central to the success of any collaborative care program that seeks to address the bulimic patient’s psychosocial issues. Like other healthcare professionals, dental team members are concerned about their patients’ overall health as well as their oral health. However, dentists have the ability to transform bulimic patients’ failing dentition to a renewed dentate state, which not only improves function but also offers many of the psychosocial benefits associated with an attractive smile.
The Smile and Psychological Consequences
The oral presentation of bulimic patients resembles that of patients with severe dentition wear, gastroesophageal reflux disease, frequent use of acidic drinks (eg, cola), and chemotherapy exposure.5,13 It is imperative that the treating clinician(s) eliminate all other etiologies before embarking upon a treatment plan oriented towards the restoration of a bulimic patient’s oral condition.
Dental lesions typical of bulimic patients include erosion of enamel on the lingual surfaces of the maxillary/mandibular arch and the palatal surfaces of maxillary posterior teeth.5 Usually, the mandibular anterior dentition is less affected due to some protection by the tongue. Raised margins of occlusal restorations may appear due to the frequency of exposure to gastric acids and result in fracture and/or further occlusal changes. Medications prescribed for psychological concerns should also be considered and may affect the gingival status of the patient through generalized erythema, xerostomia, and enlarged papillae.5,7,14 Varying degrees of periodontitis may further hinder the status of the patient’s oral health.5,7
Currently, clinicians are in disagreement about what constitutes the proper timing and modality of treatment for rehabilitating a bulimic patient’s oral condition. Ambard et al depict the treatment of an active bulimic patient with the traditional two-stage method of implant placement, uncovering and subsequent loading.3 Kavoura et al describe the full-mouth rehabilitation of an active bulimic patient using a combination of complete-coverage galvano and metal-ceramic restorations.5 Additionally, Hazleton et al suggest limiting all dental care in an active bulimic patient unless the condition is acknowledged, active caries is not present, and medical/counseling services are explored.14
Analysis of statistical data allows clinicians to better perceive the treatment hurdles that might be encountered when treating a bulimic patient. It is logical and prudent to formulate a treatment option that considers the statistical elucidations. Despite the successful treatment of most of the bulimic patients in the aforementioned reports, the various modalities leave crucial items unaddressed and psychosocial claims statistically unverified.
It is apparent that an immediately loaded dental implant protocol would provide a bulimic patient with a durable, restorative technique minimizing the corrosive effects of acidic vomitus, thereby addressing the immediate esthetic, psychological, and functional demands specific to the bulimic dental patient.
Surgical Protocol
With the advent of immediate loading and protocols such as Teeth in a Day® (TIAD), which guide practitioners through the surgical steps, it is logical and prudent for clinicians to utilize such a modality for expeditious, yet predictable, treatment of bulimic patients.15-18 Balshi and Wolfinger introduced the TIAD protocol as an efficient and predictable means of oral rehabilitation through the use of immediately loaded dental implants.15,18 Since 1997, clinicians have experienced a high success rate for patients’ mandibular arches.19-21 Maxillary full-arch implant rehabilitation cases followed a similar trend, but not until 2000.16,22-24 The durability and low maintenance of an immediately loaded, implant-supported, screw-retained prosthesis offers many advantages, including: improved esthetics, greater hygiene accessibility, osseous retention/preservation, immediate function, condensed chairtime, and reduced long-term maintenance.15-18 Although the TIAD treatment is applicable to most patients, it appears that those who fall into the bulimic patient population may uniquely benefit from such a protocol, which at least enables clinicians to offer an alternative modality of treatment compared to endodontic, periodontal, orthodontic, or crown and bridge prosthodontic treatment that, using this patient example, may require more than 40 treatment visits over 1-½ years. Galindo and Butura published a patient report with similar treatment concepts and discussed the need for immediate function in these types of patients.25
The following treatment report serves to illustrate the full-mouth rehabilitation of a patient with bulimia nervosa following the TIAD immediate functional loading protocol. The psychometric component of this report served as a statistical instrument designed specifically for illustrating and validating the patient’s psychosocial response to the treatment.
Treatment Review
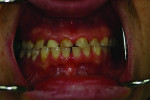
A 34-year-old, Caucasian woman (Figure 1) presented with severe dental perimolysis (erosion) resulting from a 28-year history of varying exposure to acidic vomitus during self-induced purging episodes. Previously, the patient had sought treatment at numerous local/foreign dental specialists and university dental programs; all denied treatment due to the “active” status of her eating disorder. During this 2-½-year time period, the patient’s dental, bulimic, and psychological condition deteriorated to self-reported “all-time lows.” The patient was then referred to the PI Dental Center at the Institute for Facial Esthetics, in Fort Washington, Pennsylvania, where she was considered clinically and psychologically to be a potential candidate for oral rehabilitation utilizing immediately loaded dental implants.
At new patient presentation (T1), a 20-item questionnaire (SIBID-S) was administered to provide the treating clinicians with a psychological profile of the patient while assessing the degree of body-image dysphoria associated with the eating disorder.26 The patient expressed great enthusiasm towards beginning her treatment and the potential to gain control of her eating disorder. This optimistic approach is perceived as a major component to the success of the overall treatment of the patient. A patient who is reticent about treatment or unenthusiastic about the recommended modality greatly hinders the ability of the clinician to adequately treat the patient.
The patient complained of poor function, pain with brushing and clenching, and hot/cold sensitivity—all resulting from frequent exposure to stomach acid during purging episodes. The patient described herself as being equally displeased with both her esthetics and inability to function properly.
Based on the case study, final interview with the patient, and statistical data suggesting the high likelihood of relapses in bulimic binge and purge behaviors, the prognosis of all remaining natural teeth were deemed unfit for restorative techniques using adhesives due to the lack of enamel and residual tooth structure for resistance and retention. While endodontic procedures followed by intracoronal build-ups were acknowledged as being a treatment option, it was decided that the patient’s oral concerns would be more predictably and expeditiously addressed through extraction of the existing dentition and surgical placement of dental implants following the TIAD protocol, despite significant depression and active bulimic behaviors. The continuation of psychometric assessment throughout all stages of treatment was considered appropriate for this patient. Thus, two additional testing points were warranted (T2 = 3 months postoperative [final impressions], T3 = 7 months postoperative [final prostheses delivery]).
Method/Technique
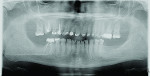
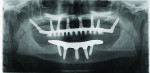
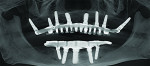
Extraoral examination revealed an Angles Class I jaw relationship/Class I dental relationship and a severely reduced vertical dimension of occlusion (VDO) collapsed bite profile. Intraoral examination of the patient displayed advanced enamel erosion patterns typical of a severely bulimic patient (Figure 2). Teeth Nos. 1, 16, 17 through 19, 31, and 32 were missing. Extensive areas of enamel loss were noted on the occlusal surfaces of the existing upper and lower molars. The palatal and occlusal surfaces of the upper premolars and the palatal surfaces of the upper anterior teeth resulted in severe chipping/wear of the incisal edges and loss of VDO. Severe maxillary and mandibular anterior lingual erosion, flattening of the palatal surfaces of the maxillary molars, and profound erosion of the maxillary palatal cusps were also evident. Mandibular amalgam restorations appeared lifted and compromised due to acidic erosion. Endodontic treatment of teeth Nos. 3, 5, and 30 were in a state of failure, exhibiting signs of recurrent periapical lesions due to coronal leakage from recurrent decay. Radiographic screening (Figure 3) confirmed clinical observations and classified the existing dentition as diseased and failing.
The patient’s existing teeth were extracted. Thirteen Brånemark System implants (Nobel Biocare® USA, www.nobelbiocare.com) were immediately placed following extractions. The 13 implants had transmucosal abutments (Brånemark Standard and Estheticone, Nobel Biocare) installed with the appropriate collar height according the soft-tissue thickness to support maxillary and mandibular screw-retained, all-acrylic resin provisional prostheses (conversion prosthesis)27 during the single surgical visit.
Results
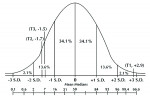
The patient’s questionnaire results at the new patient presentation (T1) resulted in a composite score of 4.0 (SD = 2.9; P = 0.004), indicating severe body-image dysphoria (Figure 4 and Table 1). At this time, the patient was considered to have severe body-image dysphoria and proven to be statistically different from normative values (SD = +/- 0.79) established in previous literature.26
At 3 months postoperative (T2), the patient presented for hygiene check-up, final impressions, and re-administration of the psychometric questionnaire. The questionnaire score at this time was 0.4 (SD = -1.7; P = 0.09) (Figure 4 and Table 1). The new score indicated that the patient was no longer statistically different from normative values. The patient was not only physically responding positively to the clinical treatment, but she was also improving psychologically. The improved score was accompanied by a drastic reduction in body-image dysphoria and agreed with the patient’s noticeable improvement in appearance. The patient left the appointment in good spirits.
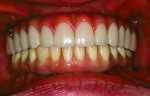
The final prostheses—a maxillary milled titanium framework supporting individual zirconium crowns with a customized acrylic gingival veneer, and a mandibular prosthesis with gold framework—were delivered 7 months (T3) after the initial implant placement (Figure 5). Radiographic (Figure 6) and clinical analysis suggested all implants to be viable, stable, and accompanied by normal levels of alveolar bone. The final psychometric questionnaire was administered at this time. A score of 0.5 (SD = -1.5; P = 0.12) positively indicated yet another improvement in self-esteem and reduction in the patient’s negative body image since the patient’s initial presentation (T1) (Figure 7). It is imperative to note that the patient’s score at this time achieved its closest range to established normative values. The patient was followed for a period of 7 years (Figure 8). All implants remained in function, and hard- and soft-tissue levels appeared normal both clinically and radiographically. Minor prosthetic complications, such as chipping of porcelain and fracturing of acrylic denture teeth, occurred.
Discussion
Patients who suffer from eating disorders present significant challenges to clinicians and respective team members. Concomitant factors, such as continued vomiting episodes and high dropout rates with extended periods of treatment and statistical data indicate the likelihood of complete recovery to be at 37%. Therefore, restorations and provisional phases are all placed at an increased risk of failure for the bulimic patient.3
The appropriate means of restorative management is dependent upon the degree of perimolysis (erosion) found in the bulimic patient.13 Statistical data suggests that one-third of those with eating disorders relapse within 4 years.5 It is apparent that rehabilitative techniques in which the durability of the restoration is derived from existing tooth structure build upon an inherently faulty foundation. Although these treatments may be deemed less invasive and more conservative, the ultimate goals of the clinician and patient are not always best served in this manner, usually resulting in compromised function and esthetics and/or failed restorations.
If the bulimic patient remains untreated, the physiological disturbances caused by these behaviors may progress to a life-threatening situation.5 Viable dentition is not only necessary for providing masticatory function and maintenance of a proper diet, healthy dentition also serves a critical component in the overall perception of one’s self-image, sexual attractiveness, and societal rank. Therefore, a functional, esthetic, long-term, and predictable solution is needed to treat a patient’s oral condition, specifically someone suffering from an eating disorder. Otherwise, unfortunate bulimic patients experiencing a likely relapse may then find themselves not only back in the grips of the disease, but also back to “square one” with their oral rehabilitation. This is hardly a justifiable position for patients to be placed and does not encourage further treatment. Patients must understand that they are “high-risk” and that a universally accepted protocol for treating such patients has not been recognized.
Clinical success experienced in the dental component of treatment is limited by skill level and adherence to the immediate-loading protocol. Additionally, the patient must cooperate throughout the maintenance phase of the treatment. This patient, however, did fracture several teeth on the maxillary all-acrylic resin prosthesis as a result of clenching during the provisional phase of treatment. The patient was provided a new occlusal guard with instructions to wear it as often as possible in order to avoid future damage and extend the use of the prosthesis while the critical healing phase passed.28 Soft-tissue healing did not appear to be abnormal at any stage of treatment.
Oral rehabilitation of this nature utilizing the traditional (two-stage) method, typically requires many clinical visits over a 6- to 9-month period, thus postponing results and further increasing the likelihood of a premature end to treatment. When placing implants, the treating clinician should be aware of the significant role bone quality plays in the primary stability of endosteal implants, especially those that are immediately loaded. In this patient, the bone quality was recognized as being type 3 in both the maxilla and the mandible.29
Bone remodeling around immediately loaded dental implants in this bulimic patient appeared to follow normal healing patterns. Osseointegration was detected at 3 months following implant placement. This was determined clinically by assessing transmucosal abutment screw tightness prior to making the final impressions. Dr. Russell Marx, Chief Scientific Officer of the National Eating Disorder Association (NEDA), indicated in a personal communication that bone remodeling in bulimic patients is generally a function of their body weight as opposed to malnutrition. This is logical and in agreement with Wolff’s Law30 and Brånemark’s reporting of bone architecture and force transmission in his original work.31
Most importantly, intervention through improved esthetics and function using an immediate-loading protocol offers bulimic patients a renewed source of improved self-esteem, while providing hope, professional understanding, and a structured path to recovery in a very timely manner. The ability to treat bulimic patients’ oral condition in a drastically reduced number of clinical visits may encourage even the most timid of patients to seek similar treatment and restore their oral condition.
The administration of a psychometric questionnaire by a dental professional can be used only as a guideline to determining a patient’s body image profile. It is important to note that the dental professional should collaborate with a licensed psychologist to make any psychological interpretation. There is currently no universally accepted body image questionnaire.
Conclusion
In spite of the unprecedented growth of eating disorders in the past two decades, research of eating disorders continues to be underfunded, insurance coverage for treatment is inadequate, and societal pressures to be thin remain rampant. NEDA recognizes that the exact treatment needs of each individual will vary. It is important for individuals struggling with an eating disorder to find a health professional they trust to help coordinate and oversee their specific needs.
The use of prosthodontic treatment to rehabilitate patients in such debilitated conditions, whether from bulimic origin or not, provides an expedient and predictable alternative method for restoring function and esthetics. The durability and low maintenance of an immediately loaded, implant-supported prosthesis offers many advantages such as: immediate function, osseous preservation, greater hygiene accessibility, improved esthetics, less chairtime, and reduced long-term maintenance.
Integral as psychosocial issues are to patient well-being and overall outcomes, they are rarely assessed by practices that focus exclusively on repairing overt physical manifestations of orofacial injury. Addressing associated psychosocial complexities requires a shift to a dental care paradigm that integrates multidisciplinary expertise to address psychosocial antecedents and consequences of orofacial injury.
In this patient report, oral rehabilitation using the TIAD protocol provided an expedited and predictable alternative method for restoring functional abilities and esthetics to a severely depressed bulimic patient. It is hoped that the rehabilitation of clinical and psychosocial factors—all considered integral components to a bulimic patient—encourage acquisition of control over the eating disorder and ultimately increase the likelihood of eliminating all bulimic behaviors.
Acknowledgments
The authors would like to acknowledge the contributions of the following individuals: Bob Winkelman, MDT, of Fort Washington Dental Lab, Fort Washington, Pennsylvania, for laboratory assistance; team members of the PI Dental Center, Fort Washington, Pennsylvania, for their extraordinary patient care and management; Drs. Timothy R. McConnell, PhD, Joseph B. Hazzard, Jr., PhD, and Leon Szmedra, PhD, of the Exercise Physiology Graduate Department at Bloomsburg University of Pennsylvania, Bloomsburg, Pennsylvania, for their respective statistical and psychological specialty analyses; Dr. Mark DiRe, Bellevue, Washington, and fellow prosthodontist, Dr. Walter Warpeha, Minneapolis, Minnesota, for follow-up care and acquisition of the most recent radiographic analysis; fellow prosthodontist Heather Conrad, Director of Advanced Education Program in Prosthodontics at the University of Minnesota, and resident Fouad Badr for assistance with continued care; and Dr. Russell Marx, San Diego, California, for review of this manuscript and insights on the impact of eating disorders.
About the Authors
Thomas J. Balshi, DDS, PhD, FACP
Private Practice
Fort Washington, Pennsylvania
Glenn J. Wolfinger, DMD, FACP
Private Practice
Fort Washington, Pennsylvania
Stephen G. Alfano, DDS, MS, FACP
Private Practice
Fort Washington, Pennsylvania
J. Neil Della Croce, DMD, MS
Private Practice
Kennett Square, Pennsylvania
Stephen F. Balshi, MBE
Director of Research, Pi Dental Center
Institute for Facial Esthetics
Fort Washington, Pennsylvania
President, CM Prosthetics, Inc.
Fort Washington, Pennsylvania
References
1. Eating Disorders 101 Guide: A Summary of Issues, Statistics and Resources. The Renfrew Center Foundation for Eating Disorders. 2003. https://www.renfrew.org.
2. Wade TD, Keski-Rahkonen A, Hudson J. Epidemiology of eating disorders. In: Tsuang MT, Tohen M, Jones P, eds. Textbook of Psychiatric Epidemiology. 3rd ed. New York, NY: Wiley; 2011:343-360.
3. Ambard A, Mueninghoff L. Rehabilitation of a bulimic patient using endosteal implants. J Prosthodont. 2002;11(3):176-180.
4. Swenne I, Thurfjell B. Clinician onset and diagnosis of eating disorders in premenarcheal girls is preceded by inadequate weight gain and growth retardation. Acta Paediatr. 2003;92(10):1133-1137.
5. Kavoura V, Kourtis SG, Zoidis P, et al. Full-mouth rehabilitation of a patient with bulimia nervosa. A case report. Quintessence Int. 2005;36(7-8):501-510.
6. Russell G. Bulimia nervosa: an ominous variant of anorexia nervosa. Psychol Med. 1979;9(3):429-448.
7. Robb ND, Smith BG. Anorexia and bulimia nervosa (the eating disorders): conditions of interest to the dental practitioner. J Dent. 1996;24(1-2):7-16.
8. Kennedy SH, Garfinkle PE. Advances in diagnosis and treatment of anorexia nervosa and bulimia nervosa. Can J Psychiatry. 1991;37(5):309-315.
9. Zachariasen RD. Oral manifestations of bulimia nervosa. Women Health. 1995;22(4):67-76.
10. Mitchell JE, Pyle RL, Eckert ED. Frequency and duration of binge-eating episodes in patients with bulimia. Am J Psychiatry. 1981;138(6):835-836.
11. Bonilla ED, Luna O. Oral rehabilitation of a bulimic patient: a case report. Quintessence Int. 2001;32(6):469-475.
12. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 5th ed. (DSM-5). Arlington, VA: American Psychiatric Publishing; 2013:347.
13. Christensen GJ. Oral care for patients with bulimia. J Am Dent Assoc. 2002;133(12):1689-1691.
14. Hazelton LR, Faine MP. Diagnosis and dental management of eating disorder patients. Int J Prosthodont. 1996;9(1):65-73.
15. Balshi TJ, Wolfinger GJ. Teeth in a day. Implant Dent. 2001;10(4):231-233.
16. Balshi TJ, Wolfinger GJ. Teeth in a day for the maxilla and mandible: case report. Clin Implant Dent Relat Res. 2003;5(1):11-16.
17. Balshi TJ, Wolfinger GJ. Immediate placement and implant loading for expedited patient care: a patient report. Int J Oral Maxillofac Implants. 2002;17(4):587-592.
18. Balshi TJ, Wolfinger GJ. A new protocol for immediate functional loading of dental implants. Dent Today. 2001;20(9):60-65.
19. Balshi TJ, Wolfinger GJ. Immediate loading of Brånemark implants in edentulous mandibles: a preliminary report. Implant Dent. 1997;6(2)83-88.
20. Schnitman PA, Wöhrle PS, Rubenstein JE, et al. Ten-year results for Brånemark implants immediately loaded with fixed prostheses at implant placement. Int J Oral Maxillofac Implants. 1997;12(4):495-503.
21. Tarnow DP, Emtiaz S, Classi A. Immediate loading of threaded implants at stage 1 surgery in edentulous arches: ten consecutive case reports with 1- to 5-year data. Int J Oral Maxillofac Implants. 1997;12(3):319-324.
22. Balshi SF, Wolfinger GJ, Balshi TJ. A prospective study of immediate functional loading, following the Teeth in a Day protocol: a case series of 55 consecutive edentulous maxillas. Clin Implant Dent Relat Res. 2005;7(1):24-31.
23. Horiuchi K, Uchida H, Yamamoto K, Sugimura M. Immediate loading of Brånemark system implants following placement in edentulous patients: a clinical report. Int J Oral Maxillofac Implants. 2000;15(6):824-830.
24. Kinsel RP, Lamb RE, Moneim A. Development of gingival esthetics in the edentulous patient with immediately loaded, single-stage, implant-supported fixed prostheses: a clinical report. Int J Oral Maxillofac Implants. 2000;15(5):711-721.
25. Galindo DF, Butura CC. Immediate loading of dental implants in the esthetic region using computer-guided implant treatment software and stereolithographic models for a patient with eating disorders. J Prosthodont. 2014;23(2):98-103.
26. Cash TF. The situational inventory of body-image dysphoria: psychometric evidence and development of a short form. Int J Eat Disord. 2002;32(3):362-366.
27. Balshi TJ. The Biotes conversion prosthesis: a provisional fixed prosthesis supported by osseointegrated titanium fixtures for restoration of the edentulous jaw. Quintessence Int. 1985;16(10):667-677.
28. Balshi SF, Allen FD, Wolfinger GJ, Balshi TJ. A resonance frequency analysis assessment of maxillary and mandibular immediately loaded implants. Int J Oral Maxillofac Implants. 2005;20(4):584-594.
29. Lekholm U, Zarb GA. Patient selection and preparation. In: Brånemark PI, Zarb GA, Albrektsson T, eds. Tissue-Integrated Prostheses: Osseointegration in Clinical Dentistry. Chicago, IL: Quintessence Publishing Co.; 1985:199-220.
30. Frost HM. Wolff's Law and bone’s structural adaptations to mechanical usage: an overview for clinicians. Angle Orthod. 1994;64(3):175-188.
31. Strid KG. Radiographic results. In: Brånemark PI, Zarb GA, Albrektsson T, eds. Tissue-Integrated Prostheses: Osseointegration in Clinical Dentistry. Chicago, IL: Quintessence Publishing Co.; 1985:187-197.