Thermal Effects on Pulp Due to Laser and Handpiece Usage
Christina Penn; Christopher Beninati; Alissa Mariano; Daniel Dooley; Masly Harsono, DMD; Ronald Perry, DMD, MS; and Gerard Kugel, DMD, MS, PhD
ABSTRACT
OBJECTIVE: The study was designed to compare changes in pulpal temperature during ablation of dental hard tissue while using two established erbium dental laser systems, a new CO2 laser system, and a conventional high-speed handpiece. METHODS: Eighty non-carious human extracted molars were separated into four sample groups of 20 teeth each. Three laser systems were used, respectively, to ablate the occlusal surface of the teeth in three of the groups for 60 seconds each. The high-speed handpiece was used to drill the occlusal surface of the fourth group for 60 seconds. Pulpal temperatures were measured using thermocouples inserted into each tooth’s pulpal chamber prior to ablation. RESULTS: None of the average temperature increases approached the threshold of 5.5°C at which pulpal damage begins. On average, the pulpal temperature of teeth ablated with the Waterlase MD system increased the most (3.56°C). The traditional handpiece caused the lowest average temperature increase (1.57°C), followed by the LightWalker DT system (3.20°C) and the Solea CO2 system (3.30°C).
Despite a remarkable decline over the past 40 years, dental decay still affects 60% to 90% of the world’s schoolchildren and almost 100% of adults, according to the World Health Organization Global Oral Health Data Bank and Oral Health/Area Profile Programme.1 Unfortunately, traditional methods of preparing hard tissue have not significantly changed since the late 1950s, when the first high-speed air-turbine drills began replacing belt-driven handpieces.2 Dental drills, which create vibration and make a distinctive noise, often are a prominent factor in many adults’ fear of visiting a dental office. In contrast, lasers can remove dental hard tissue with minimal vibration and noise. Because of the ability to tightly focus the ablation holes, lasers also have the potential to substantially reduce the amount of tissue removed during cavity preparations, facilitating the preservation of healthy tissue.3
A number of Er:YAG, Er,Cr:YSGG, and Nd:YAG solid-state lasers have been cleared by the US Food and Drug Administration (FDA) for use in dentistry over the past decade. However, the wavelengths of these lasers are not absorbed efficiently by hydroxyapatite, resulting in slow and inefficient ablation. The wavelengths of these lasers are primarily absorbed by the water content of the tooth.4 This makes these wavelengths inherently inefficient, because the composition of tooth enamel by volume is 12% water and 85% hydroxyapatite.5 In contrast, carbon dioxide (CO2) laser wavelengths, especially at 9.3 μm and 9.6 μm, are highly absorbed by the apatite mineral. Their absorption coefficients are 5,500 cm–1 and 8,000 cm–1 respectively, compared to a range of 480 cm–1 to 800 cm–1 for the erbium lasers.6-10
The wavelengths that produce commercially viable cutting speeds range between 9.2 µm and 9.8 µm.6 Recent research has shown that a 9.3-μm CO2 laser can be efficiently absorbed by dental hard tissue and can ablate tooth structure without generating excessive peripheral thermal or mechanical damage or harming the pulp.11,12
Although lasers at the 9.3-μm CO2 wavelength up to now have not been commercially available, a new CO2 dental laser system (Solea™, Convergent Dental, www.convergentdental.com) of this type has been developed. The objective of the present study is to compare changes in pulpal temperature during ablation of dental hard tissue while using two established erbium dental laser systems (Er,Cr:YSGG 2.78 μm, Waterlase MD™, Biolase, Inc., www.biolase.com; and Er:YAG 2.94 μm, LightWalker® DT, Fotona, www.fotona.com), the new CO2 system, and a traditional high-speed handpiece (Midwest® High Speed Handpiece, DENTSPLY, www.dentsply.com). These temperature changes will also be compared to the commonly accepted threshold of a 5.5°C rise. A temperature rise of 5.5°C is considered excessive and likely to lead to a loss of pulpal vitality, according to the seminal work of Zach and Cohen.13
Materials and Methods
Following IRB approval 80 non-carious human extracted molars with no major decay or defects were cleaned of adherent patient material by scrubbing with detergent and water. They were then immersed in a fresh solution of formalin and stored in containers with a distilled water solution containing thymol (0.1%). The teeth were separated into four sample groups of 20 teeth each. Within each group, each sample tooth was labeled with a number and color-coded to correspond to one of the four systems.
In order to compare the four systems at similar power levels and fluence, the manufacturers’ recommended hard-tissue ablation settings were selected:
· Solea system:1.6 kHz repetition rate with 5.94 mJ of pulse energy
· Waterlase MD system with Turbo handpiece (2009 model): 30 Hz repetition rate with 233mJ of pulse energy
· LightWalker DT system (current model): 50 Hz repetition rate with 160 mJ of pulse energy
· Midwest High Speed Handpiece: a size 330 carbide bur
(Editor’s Note: The Waterlase MD system used in this study was from 2009. A newer model, the Waterlase iPlus™, was released in 2011.)
For each system, the standard (recommended) air/water spray mixture was used. The laser system settings and measured power output for each of the system configurations tested are shown in Table 1.
A digital radiograph (Schick CDR Elite Size 2, Sirona Dental, www.schickbysirona.com or Gendex GSX-700™, Gendex Dental Systems, www.gendex.com) was taken of each sample tooth to identify the pulp-chamber location. A single hole was drilled to allow access to the top of each pulp chamber. A thermocouple (model 5TC-TT-K-36-36, Omega Engineering Inc., www.omega.com) was placed in the top of each pulp chamber and bonded to the tooth using thermally conductive epoxy (Hysol® ES1001™, Henkel Electronic Materials, www.henkel.com). After curing of the epoxy, a second radiograph was taken to verify that no air pockets had formed around the thermocouple and that it was properly positioned.
For the laser ablation systems, each sample tooth was placed in a vice holder to ensure a consistent distance (4 mm to 7 mm) away from the laser tip. (The 4 mm to 7 mm range was recommended by the laser manufacturers, who stated there would be minimal fluence changes in this range.) Power readings with a calibrated Ophir 30A-SH laser power meter (Ophir Optronics, www.ophiropt.com) were taken for all systems prior to any tests being run. The occlusal surface of each sample tooth was ablated for 60 seconds using the predetermined laser settings. There were differences in depth among the three systems and the high-speed handpiece. Some units penetrated deeper than others based on such factors as angle of ablation, geometry of the tooth, hardness of lesion, and strength of hydroxyapatite.
For the traditional handpiece, each sample tooth was placed in a holder, and the tip of the bur was placed against the occlusal surface of the tooth. Cutting was initiated by stepping on the rheostat foot pedal, and continued for 60 seconds.
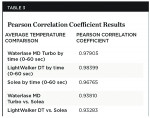
Pulpal temperatures were measured by attaching the thermocouples to the Apollo IV DT304 Digital Temperature Logger (UEi Test Instruments, www.ueitest.com), which was attached via USB connection to a laptop computer running ApolloDigital software. This enabled recording of real-time data for each sample tooth. The results were sent to the Indiana University School of Medicine, Department of Biostatistics (IndeviaData) for analysis. Pearson coefficient calculations also were performed to analyze the correlation of temperature response over time for each system configuration. The correlation of the temperature measurements of the Solea system with the temperature measurements of the other three systems also was analyzed.
Results
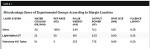
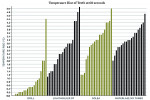
All of the systems appeared to effectively ablate all sample teeth, and minimal char was noted. On average, the pulpal temperature of teeth ablated with the Waterlase MD system increased the most (3.56°C). The Midwest High Speed Handpiece caused the lowest average temperature increase (1.57°C), followed by the LightWalker DT system (3.20°C) and the Solea system (3.30°C). The average temperature findings are summarized in Table 2. None of the average temperature increases approached the 5.5°C at which pulpal damage is understood to begin. Figure 1 displays the individual data sets that were compiled to form the average results in Table 2.
The Pearson coefficients for the three laser test groups are shown in Table 3. All have a correlation of 0.95 or greater, with respect to time and temperature rise. Table 3 also shows that each of the predicates had a Pearson correlation coefficient of 0.93 or greater when compared to the Solea system. Each individual performance data set significantly correlates to each other, confirming the substantial equivalence of the laser systems with respect to temperature over time.
Discussion
The first researchers to investigate the use of lasers for cavity prevention and caries removal concluded that the technology was unworkable, due to the large amount of heat generated locally and the resulting cracking and distortion of the enamel.13 Since then, however, a deeper understanding of the mechanics of hard-tissue ablation has led to the development of lasers that work effectively on the absorbing components of the tissue.12,14
The three laser systems compared in the present study differ significantly, with different pulse characteristics and different frequencies. Erbium lasers typically operate most efficiently at very low repetition rates. In order to achieve higher cutting rates, they therefore must deliver a larger amount of energy per pulse (100 mJ to 500 mJ). CO2 lasers have the flexibility to operate efficiently at high repetition rates, allowing them to deliver lower energy per pulse. CO2 laser beams can be scanned to minimize heat accumulation in a given area.12
In the present study, variables in cutting included differing occlusal geometries and dehydration levels (molars were extracted at different times). The differences in occlusal geometry to some extent affected the size and/or shapes of the holes drilled to access the roof of the pulp chamber. Enamel thickness averages from 1.28 mm on the mesial surface of the first molar to 1.40 mm on the distal surface of the first molar, and from 1.29 mm on the mesial surface of the second molar to 1.48 mm on the distal surface of the second molar.15 Variations in storage time of extracted molars in thymol solution may affect the temperature changes during ablation.16 However, it was implausible to collect all extracted molars used in the study concurrently to avoid differences in storage time. By averaging the pulpal temperature changes, the authors aimed to standardize data to account for variations in occlusal geometries and dehydration levels.
Conclusions
When used to ablate healthy extracted molars, the Solea 9.3-µm CO2 laser operated at standard power settings caused pulpal temperature increases that were substantially equivalent to those caused by the LightWalker DT Er:YAG laser system and slightly less than the pulpal temperature rise caused by the Waterlase MD Turbo Er,Cr:YSGG laser system. Although each of the three laser systems caused pulpal temperatures to increase more than the traditional handpiece, none of the average temperature increases produced by any of the systems approached a rise of 5.5°C, the degree of temperature change known to cause pulpal damage. Despite the differences in beam characteristics, the thermal effects of the three different laser systems on pulpal tissue were equivalent in the sense that they did not harm the pulpal tissue through temperature increases during ablation.
Disclosure
Ms. Penn received a research grant for this study from Convergent Dental. The authors report no other affiliations with any of the companies mentioned in this article.
References
1. Petersen PE. World Health Organization. The World Oral Health Report 2003: continuous improvement of oral health in the 21st century–the approach of the WHO Global Oral Health Programme. Community Dent Oral Epidemiol. 2003;31(suppl 1):3-23.
3. Fried D. IR laser ablation of dental enamel. In: Featherstone JDB, Rechmann P, Fried D, eds. Proceedings of SPIE. 2000;3910:136. doi:10.1117/12.380820.
4. Meister J, Franzen R, Forner K, et al. Influence of the water content in dental enamel and dentin on ablation with erbium YAG and erbium YSGG lasers. J Biomed Opt. 2006;11(3):34030.
5. Featherstone JDB, Fried D. Fundamental interactions of lasers with dental hard tissues. Med Laser Appl. 2001;16(3):181-194.
6. Fried D, Glena RE, Featherstone JDB, Seka W. Nature of light scattering in dental enamel and dentin at visible and near-infrared wavelengths. Appl Opt. 1995;34(7):1278-1285.
7. Fried D, Ragadio J, Akrivou M, et al. Dental hard tissue modification and removal using sealed transverse excited atmospheric-pressure lasers operating at lambda=9.6 and 10.6 microm. J Biomed Opt. 2001;6(2):231-238.
8. Fried D, Zuerlein M, Featherstone JDB, et al. IR laser ablation of dental enamel: mechanistic dependence on the primary absorber. Applied Surface Science. 1998;127-129:852-856.
9. Zuerlein MJ, Fried D, Featherstone JDB. Modeling the modification depth of carbon dioxide laser-treated dental enamel. Lasers Surg Med. 1999;25(4):335-347.
10. Zuerlein MJ, Fried D, Featherstone JDB, Seka W. Optical properties of dental enamel in the mid-IR determined by pulsed photothermal radiometry. IEEE Journal of Selected Topics in Quantum Electronics. 1999;5(4):1083-1089.
11. Staninec M, Darling C, Goodis H, et al. Pulpal effects of enamel ablation with a microsecond pulsed λ=9.3-μm CO2 laser. Lasers Surg Med. 2009;41(4):256-263.
12. Nguyen D, Chang K, Hedayatollahnajafi S, et al. High-speed scanning ablation of dental hard tissues with a λ = 9.3 μm CO2 laser: adhesion, mechanical strength, heat accumulation, and peripheral thermal damage. J Biomed Opt. 2011;16(7):071410. doi:10.1117/1.3603996.
13. Zach L, Cohen G. Pulp response to externally applied heat. Oral Surg Oral Med Oral Pathol. 1965;19:515-530.
14. Seka W, Featherstone JDB, Fried D, et al. Laser ablation of dental hard tissue: from explosive ablation to plasma-mediated ablation. In: Wigdor HA, Featherstone JDB, White JM, Neev J, eds. Lasers in Dentistry II. Proceedings of SPIE. 1996;2672:144-158. doi: 10.1117/12.238763.
15. Stroud JL, English J, Buschang, PH. Enamel thickness of the posterior dentition: its implications for nonextraction treatment. Angle Orthod. 1998;68(2):141-146.
16. Goodis HE, Marshall GW Jr, White JM. The effects of storage after extraction of the teeth on human dentine permeability in vitro. Arch Oral Biol. 1991;36(8):561-566.
About the Authors
Christina Penn
Tufts University School of Dental Medicine
Boston, Massachusetts
Christopher Beninati
Tufts University School of Dental Medicine
Boston, Massachusetts
Alissa Mariano
Tufts University School of Dental Medicine
Boston, Massachusetts
Daniel Dooley
Tufts University School of Dental Medicine
Boston, Massachusetts
Masly Harsono, DMD
Assistant Professor
Department of Research Administration
Tufts University School of Dental Medicine,
Boston, Massachusetts
Ronald Perry, DMD, MS
Director of the Gavel Center for Restorative Research
Associate Clinical Professor
Tufts University School of Dental Medicine,
Boston, Massachusetts
Gerard Kugel, DMD, MS, PhD
Professor, Associate Dean for Research
Tufts University School of Dental Medicine
Boston, Massachusetts