Management of Pediatric Mandibular Fracture: A Case Series
Abstract:
A pediatric mandibular fracture can cause a child severe pain and the parent or caregiver extreme worry. While the pattern of fractures and associated injuries in children is similar to adults, the incidence is low. Due to a number of factors, including the anatomical complexity of the developing mandible in a child, management of such fractures differs from that of adults and can greatly challenge the pediatric dentist. Various treatment modalities of managing mandibular fracture are available, such as closed/open cap splint with circummandibular wiring, arch-bar fixation, and cementation of the cap splint. This article reviews 19 cases in the management of pediatric facial fracture using varied treatment methods.
While facial fractures in the pediatric population comprise less than 15% of overall facial fractures in the general population,1 mandibular fractures are among the most common in pediatric patients. The incidence of mandibular fracture in children ranges from 0.6% to 1.2%.2 The most typical causes of fracture in children were fall (64%), traffic incidents (22%), and sports-related accidents (9%).3 Mandibular fractures are most likely to cause dental injuries (39.3%).4 Furthermore, there is widespread acceptance that the patterns of fractures change with advancements in age. McGraw and Cole5 reported that fractures shifted from the upper to the lower region of the face as age increased.
Mandibular fractures can be diagnosed clinically but should be confirmed radiographically. Fractures occurring in children present problems in achieving and maintaining stability that are quite different from those in adults.6,7 As such, the treatment modality differs in children due to the anatomic complexity of the developing mandible, presence of tooth buds, and eruption of primary and permanent teeth. The most common treatment includes cap splints with circummandibular wiring, cap splint cemented onto the arch, and Erich arch-bar fixation.
Through a discussion of a case series, this article presents various treatment modalities in the management of pediatric mandibular fractures.
Cases
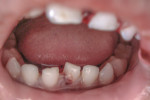
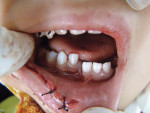
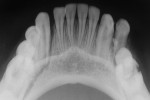
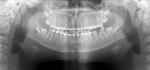
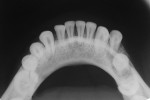
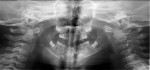
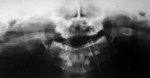
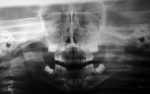
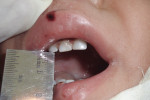
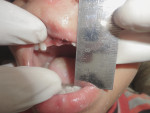
Nineteen patients between the ages 3 and 12 years with maxillofacial injuries (Figure 1 and Figure 2) presented to the Department of Pedodontics and Preventive Dentistry in K D Dental College and Hospital, Mathura, India. Detailed case histories, clinical examinations, and radiographic investigations such as orthopantomography, occlusal radiography, and intraoral periapical radiography were performed (Figure 3 through Figure 8). After careful evaluation, a diagnosis of the type of fracture was made and a treatment plan was formulated for each patient. Informed consent was obtained from the parent, and in some cases, treatment was performed under general anesthesia, with written consent obtained from the parent.
Preparation of Acrylic Splints
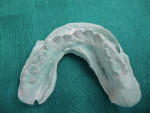
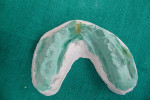
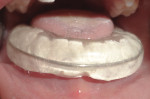
Upper and lower alginate impressions were made for each patient and models prepared. In cases of displaced fracture, mock surgery was performed on dental casts (Figure 9 and Figure 10). After mock surgery, the casts were held in their reduced positions and proper occlusion with the opposing maxillary cast was confirmed. Both the upper and lower casts were stabilized and mounted onto an articulator. An acrylic splint was prepared using self-cure acrylic resin involving labial and buccal flanges (Figure 11).
For Displaced Fractures
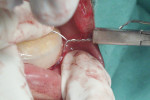
In children with displaced fractures, the mandibular arch was reduced manually under general anesthesia with occlusion in the guidance position, and the acrylic splint was tried in. Stab incisions were placed in the submandibular and submental regions to facilitate the passage of a Kelsey-Fry mandibular bone awl, which was passed lingually along the body of the mandible through a stab incision and piercing the lingual mucosa. A 26-gauge orthodontic wire was fed to the awl. Once the wire was secured to the awl, it was withdrawn until the tip of the awl reached the lower border of the mandible and then the wire was carefully passed on to the buccal sulcus along the body of the mandible, with care taken to prevent soft-tissue injury. One wire was passed on each side, taking precaution to avoid injury to the mental neurovascular bundle (Figure 12).
For Nondisplaced Fractures
In children with nondisplaced fractures, the prepared acrylic splint was placed onto the mandibular arch and occlusion was verified. After achieving proper occlusion, the splint was cemented directly onto the arch using glass-ionomer luting cement (Ketac™ Cem, 3M ESPE, www.3MESPE.com) (Figure 13).
Arch-Bar Fixation
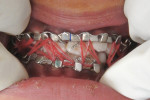
Before inserting the arch bar, occlusion was checked to confirm full interdigitation of the teeth with regular contact. The prefabricated arch bar was adjusted in shape and length, with care taken to avoid damage to gingival tissue. The bar was adapted closely to the dental arch and placed between the dental equator and gingiva. The arch bar was extended to the last tooth on both sides in the oral cavity. The hooks were positioned symmetrically in the upper and lower jaws to achieve calculable tension forces on both the bars for functional training with elastics. To fix the arch bar in place, a ligature in the premolar region was prepared on each side. The arch bar was positioned and fixed using the wire twister. The wire was cut with a cutter, and the ends were turned away from the gingiva to prevent damage. Maxillomandibular fixation was performed with elastics for intraoperative management of the occlusion (Figure 14).
Postoperative instructions for following a soft and liquid diet and using antibiotic prophylaxis were given to each patient.
Results
In all patients, splints and arch bars were removed after 2 to 4 weeks. Postoperative radiographs were obtained to confirm the healing of the fractured site before removal of the splint (Figure 5 and Figure 8), and all the patients were followed-up for 12 months. None of the patients had complications in the postoperative period, and uneventful healing and union of the fracture segment occurred in all patients. In one patient, healing time was prolonged because of continuous dislodgement of the splint, which was re-cemented. A slight discrepancy in the occlusion in a few patients was observed, which was corrected on its own over the course of time.
Discussion
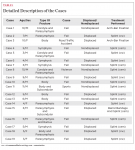
Maxillofacial injuries in children are uncommon. The prevalence of different sites of mandibular fracture, including the condyle, alveolus, body, symphysis, parasymphysis, angle, ramus, and coronoid, is given by Haug and Foss.6 Of 19 cases presented in this article, eight were fracture in the symphysis/parasymphysis region, four were in the body of the mandible, four in the parasymphysis associated with condylar fracture, and there was one case each of body and condyle, body and parasymphysis, and ramus and symphysis (Table 1) In the present case series, the most common etiology was fall, which accounted for 80% of all children. Most children were younger than age 6 years (12 children), with a male-to-female ratio of 4:1.
Management of mandibular fractures in children differs somewhat from that in adults because of several considerations, including anatomic variation, rapidity of healing, degree of patient cooperation, and the potential for changes in mandibular growth. The treatment modality of fractures in the pediatric mandible depends on the patient’s age and stage of tooth development.8 Minimally displaced fractures can be treated by soft diet, analgesic use, and antibiotic prophylaxis. However, in very young children, healing might be prolonged because of insufficient cooperation in following postoperative instructions. In such cases, fabrication of a splint and cementing onto the arch can be used to overcome these hindrances.
In the present case series, six patients reported with nondisplaced symphysis/parasymphysis fracture, which was managed with acrylic splint cemented onto the arch for an average of 2 weeks. All 19 patients showed satisfactory healing in 2 to 3 weeks with no complications. Moreover, reduced mouth opening was one of the common features in the children following fracture of the mandible, which was improved over time (Figure 15 and Figure 16). Rowe2 suggested employing closed reduction as a treatment in cases of displaced fractures probably because of the remodeling potential of the pediatric craniofacial skeleton. Displaced fractures need to be reduced and immobilized. Children demonstrate greater osteogenic potential and faster healing rates than adults.8 Therefore, anatomic reduction in children must be accomplished earlier9 and immobilization time should be shorter (2 weeks).10
In the present case series, seven displaced fractures were reduced manually and immobilized using splints with circummandibular wiring, two cases were treated with arch-bar fixation, and one case involved a splint being cemented onto the arch. The case in which the splint was cemented showed delayed healing due to continuous dislodgement of the splint, which occurred because of dissolution of the cement. Previous research has shown the use of arch-bar fixation restricts normal dietary intake in children, resulting in significant weight and protein loss.11 Here in the present case series, maxillomandibular fixation was performed using light-training elastics so that an active exercise program could be started as soon as the child could cooperate. Extended periods of maxillomandibular fixation can lead to ankylosis in children and should be avoided.12 In cases of condylar fractures, nonoperative management is overwhelmingly popular, because minimal complications occur and the outcomes are good in both adults and children.13 Moreover, in older children, the bone has less capacity to adapt and remodel, and the ramus height may not be regained.14
In this case series, condylar fracture was associated with symphysis/parasymphysis, ramus, or body of the mandible. In such cases, emergency management with a barrel bandage was advised along with a soft and liquid diet until the mandible was immobilized with a splint. The condyle showed remodeling over time. Open reduction with rigid internal fixation is rarely indicated for pediatric condylar and subcondylar fractures unless a displaced fragment produces a mechanical obstruction.3,5 Fractures of the condyle are seen more often in children than in adults (50% of the mandibular fractures versus 30%), because a child’s highly vascularized condyle and thin neck are poorly resistant to impact forces occurring in falls. In children younger than 6 years, condylar fractures are more often intracapsular than extracapsular in location. In children older than 6 years, most condylar fractures typically occur in the neck region.6 Although a conservative approach is preferred in children, sometimes open reduction and internal fixation is necessary in cases of condylar fractures associated with symphysis/parasymphysis fracture to provide stabilization to the symphysis/parasymphysis region and to facilitate healing. The malocclusion seen immediately post-injury in children with condylar fracture is caused by the muscle spasm, which dissipates in 3 or 4 days without the use of maxillomandibular fixation.15
Conclusion
Management of pediatric mandibular fractures is a challenge, considering the age and the anatomic variation of the child. In this case series, symphysis/parasymphysis fractures were the most common (42%) among the different areas of mandibular fracture. The role of a pediatric dentist is vital in managing children with such fractures. If proper principles are followed, satisfactory results with minimum discomfort can be anticipated in children.
About the Authors
Ravi M. Agarwal, BDS
Post-Graduate Student, Department of Pedodontics, K D Dental College and Hospital, Mathura, India
Ramakrishna Yeluri, MDS, FPFA
Professor and Head, Department of Pedodontics and Preventive Dentistry, Teerthanker Mahaveer Dental College and Research Centre, Moradabad, India
Chanchal Singh, MDS
Professor and Head, Department of Pedodontics, K D Dental College and Hospital, Mathura, India
Kalpna Chaudhry, MDS
Reader, Department of Pedodontics, K D Dental College and Hospital, Mathura, India
Autar K. Munshi, MDS
Former Senior Professor and Head, Honorary Consultant, Post-Graduate Training and Dental Research, K D Dental College and Hospital, Mathura, India
References
1. MacLennan WD. Fractures of the mandible in children under the age of six years. Br J Plast Surg. 1956;9(2):125-128.
2. Rowe NL. Fractures of the jaws in children. J Oral Surg. 1969;27(7):497-507.
3. Dodson TB. Mandibular fractures in children. OMS Knowledge Update. 1995:1:95-107.
4. Lida S, Matsuya T. Paediatric maxillofacial fractures: their aetiological characters and fracture patterns. J Craniomaxillofac Surg. 2002;30(4):237-241.
5. McGraw BL, Cole RR. Pediatric maxillofacial trauma. Age-related variations in injury. Arch Otolaryngol Head Neck Surg. 1990;116(1):41–45.
6. Haug RH, Foss J. Maxillofacial injuries in the pediatric patient. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2000;90(2):126-134.
7. Eggensperger Wymann NM, Hölzle A, Zachariou Z, Iizuka T. Pediatric craniofacial trauma. J Oral Maxillofac Surg. 2008;66(1):58-64.
8. Kaban LB. Facial trauma I: midface fractures. In: Kaban LB, ed. Pediatric Oral and Maxillofacial Surgery. Philadelphia, PA: W.B. Saunders; 1990:209-232.
9. Messinger A, Radkowski MA, Greenwald MJ, Pensler JM. Orbital roof fractures in the pediatric population. Plast Reconstr Surg. 1989;84(2):213-216.
10. Oji C. Fractures of the facial skeleton in children: a survey of patients under the age of 11 years. J Craniomaxillofac Surg. 1998;26(5):322-325.
11. Kaban LB. Diagnosis and treatment of fractures of the facial bones in children 1943-1993. J Oral Maxillofac Surg. 1993;51(7):722-729.
12. Kale TP, Urologin SB, Kapoor A, et al. Open cap splint with circummandibular wiring for management of pediatric mandibular parasymphysis/symphysis fracture as a definitive treatment modality; a case series. Dent Traumatol. 2013;29(5):410-415.
13. Kaban LB. Facial trauma II: dentoalveolar injuries and mandibular fractures. In: Kaban LB, ed. Pediatric Oral and Maxillofacial Surgery. Philadelphia, PA: W.B. Saunders; 1990:441-524.
14. Jones KM, Bauer BS, Pensler JM. Treatment of mandibular fractures in children. Ann Plast Surg. 1989;23(4):280-286.
15. Myall RWT. Management of mandibular fractures in children. Oral Maxillofac Surg Clin. 2009;21(2):197-20.