A Multidisciplinary Approach to the Esthetic and Functional Rehabilitation of a Worn and Spaced Dentition: A Case Report
Anabella Oquendo, DDS; Richard Trushkowsky, DDS; Philip G. Kotick, DDS, FICOI; Steven David, DMD
Esthetic and functional rehabilitation requires proper diagnosis and a sequenced treatment plan. A satisfying smile is dependent on tooth position, size, shape, and color, as well as the amount of gingival display. The display of both teeth and gingiva is controlled by the elevation of the upper lip when smiling. Often, the lip is higher with spontaneous smiles rather than posed smiles.1 The existence of multiple diastemata may create discord.2 The spaced dentition can be due to hypodontia, tooth-size discrepancy, impeded eruption,3 dental alveolar discrepancies, and Bolton discrepancies.4
Dental alveolar discrepancies may be a result of incongruities between the dental arch size and tooth width. In 1958, Bolton suggested these issues may be caused by a lack of harmony between these elements.5 If a proper balance does not exist between the maxilla and mandible, there may be a negative impact on proper interdigitation, overbite, and overjet. The Bolton index relates the mesiodistal tooth-size ratio between maxillary and mandibular teeth. A Bolton analysis is performed by measuring the mesiodistal width of all mandibular and maxillary teeth from first molar to first molar. Then, the summed mesiodistal widths are used to calculate the ratio between the anterior mandibular and maxillary teeth. These numbers are compared with normal values of 0.77 for the anterior ratio and 0.91 for the total arch ratio.
A dentoalveolar discrepancy analysis, or cast discrepancy analysis, can be used to determine the amount of existing space with what is needed for teeth alignment. A comparison of the available space to the required room needed to achieve an ideal esthetic arch form in conjunction with a wax-up will aid in formulation of a treatment plan.6 The tooth-size discrepancy may be result of altered tooth morphology, such as a peg-shaped lateral incisor. The size may also result in gingival margin discrepancies and clinical crowns that are not ideally proportioned.7 Some other causes are enlarged labial frenum, defects in the intermaxillary suture, harmful habits or unbalanced muscular function, and pathologic conditions, such as partial agenesis, supernumerary teeth, odontomas, cysts, and palatal clefts.8-10
The management of a complete oral rehabilitation in a patient with a severely worn dentition can be complex. Often, some vertical dimension and tooth structure has been lost. Uneven tooth wear can result with a multilevel plane of occlusion and parafunctional habits, which may jeopardize any reconstruction efforts. Erosion, attrition, abrasion, and bruxism may be complicating factors. Erosion is the loss of hard tissues due to chemical effects. Attrition is the wear of tooth against tooth, and abrasion is the wear from other surfaces.11 Bruxism is a parafunctional habit during which a person may clench (no lateroprotrusive movement) or grind (small or large mandibular movements) teeth during the day or night. Ramjford and Ash classified bruxism into two types: centric (vertical loading during the day) and eccentric (grinding into lateral excursions during sleep). Usually, patients clench or grind due to psychological or odontogenic causes.12
The clinician should recognize the damage caused by clenching and bruxing, including tooth hypermobility, tooth wear, abfractions, periodontal breakdown, stress fractures, and loss of posterior disclusion.12 These indications have to be used to formulate a treatment plan that will prevent or mitigate further breakdown. Dawson has indicated that the following must be satisfied: the patient can function from centric relation without interferences, the temporomandibular joints (TMJs) can be loaded without tenderness, centric stops are between the maxillary and mandibular anterior teeth, anterior coupling allows disclusion of the posterior teeth, and the teeth are in balance with the tongue and facial muscles.13 Prior to restoration, occlusal vertical dimension (OVD) and interocclusal rest space must be determined. OVD is the distance between two points when teeth are in contact.14 However, the loss of tooth structure does not always mean a loss of OVD has occurred. In order to provide space for new restorations, the vertical dimension may need to be increased.15 Sometimes the restoration of the anterior teeth is hindered due to insufficient interocclusal space. One treatment option would be to increase the OVD with crowns or onlays placed in the posterior. This usually means more hard-tissue destruction and greater cost. Another option would be intrusion of the lower incisors to regain space.16
A comprehensive esthetic and functional analysis is required before initiating treatment. The examination should include the following elements: a dentolabial analysis, determination of the incisal edge position, orientation of the incisal plane, determination of the incisal profile, measurement of the incisal length of the central incisors, measurement of tooth proportions (length-to-width ratio of individual teeth) and tooth-to-tooth ratio, and assessment of gingival contour and tooth color.17,18 The first step should be a maxillary vestibular wax-up. Typically, the laboratory technician does not meet the patient, and a wax-up on a diagnostic cast may appear perfect but is unrealistic.19 An intraoral composite mock-up that includes the anterior teeth only would be deceptive because the teeth would not be harmonious with the untouched posterior dentition. Just the vestibular part should be included and extend to the second premolar or first molar. Once a result that is satisfactory to the restorative dentist and patient is achieved, a series of photographs should be taken and an impression should be obtained and sent to the laboratory.
Incisal Edges
Patients with incisal wear have become accustomed to their appearances and initially balk at any suggestion to have their teeth lengthened. However, given the opportunity to try the modification with a provisional restoration, they agree. Alterations can be made readily to both shape and length, sometimes with a flowable composite resin. Esthetics and phonetics can be evaluated prior to fabrication of the final restoration and serve as a guide for the patient in accepting treatment. Increasing the length of the anterior teeth for a patient with significant wear or abrasion allows the creation of incisal guidance and enables the posterior teeth to disclude.20
Traditionally, treatment planning would begin with caries removal, periodontal treatment, endodontic therapy, oral surgery, implant placement, and possibly orthodontics. However, this sequence may compromise the esthetic outcome. Spear et al21 has suggested starting from esthetics and proceeding to function, structure, and, ultimately, biology. The first step should be the assessment of the position of the maxillary central incisors in relation to the upper lip in repose. The amount of maxillary incisal edge display will depend on the patient’s age and sex. Usually, with age, the patient displays less of the incisal edge. This is due to the decreasing tone and resiliency of the upper lip.
The selection of the type of restoration and the material used for its fabrication are critical in achieving longevity and esthetics. Advances in materials and techniques have resulted in routine use of ceramic restorations. Often, all-ceramic restorations are in two categories: translucent materials and opaque cores that are layered with an esthetic ceramic material. Translucent materials may be feldspathic porcelains or pressable ceramics. Opaque materials may be alumina, lithium disilicate, or zirconium oxide. Usually, the translucent materials are bonded to increase their longevity while high-strength materials can be conventionally cemented. Spear et al21 categorized restorations according to the requirements of the particular tooth: porcelain-laminate veneers that replace enamel, partial-coverage restorations that replace enamel and dentin, complete crowns that cover normal dentin, and complete crowns that mask discolored dentin or metal posts. In addition to esthetic factors, high strength may be required to restore anterior guidance and address the problems associated with parafunctional habits. If high strength is not required, an adhesive restoration could be placed if resistance and retention form is lacking.22,23
Case Report
A 74-year-old woman presented to the Department of International Advanced Esthetic Dentistry Program at New York University College of Dentistry. Her chief complaint was the appearance of her teeth. She believed they were old, thin, dark, small, and spaced (Figure 1). She wanted her teeth to be whiter but natural and “normal” size without spaces. She reported no pain symptoms related to the TMJs, musculature, or other dental structures. Noticeable wear was present on the maxillary and mandibular anterior teeth and the remaining posterior natural teeth (Figure 2 and Figure 3). Vertical dimension was closed slightly, and centric occlusion and centric relation were coincidental. Ideally, all the posterior teeth would be restored and the vertical dimension increased in the posterior about 1 mm. This would result in a 3-mm anterior correction. However, financial constraints prohibited this.
Radiographs, photographs, and diagnostic casts were obtained. The findings from an esthetic analysis revealed a straight profile, upper and lower midline deviation to the right, moderate overjet, and normal occlusion. Gingival papillae were blunted, and the gingival zenith was irregular (Figure 4). The maxillary anterior teeth did not touch the lower lip. Also, the patient had a high smile line with 2 mm to 3 mm of display; the midline was off to the right of the philtrum; no teeth showed in repose; the buccal corridor was normal; a full smile exposed 12 teeth; and she had a reverse smile line. The recent dental history included extractions of teeth Nos. 29 and 31 to treat nonrestorable decay under a fixed bridge, endodontic treatment for tooth No. 13, a sinus lift using Bio-Oss® (Osteohealth, https://www.osteohealth.com) mixed with autogenous bone, and two implant placements in the upper left quadrant for teeth Nos. 14 and 15.
An intraoral mock-up with composite resin was used for dento–labial analysis of the incisal edge position and posterior occlusal plane. The goal was a vertical dimension that would be both esthetic and functional. The mock-up was also used to determine the width-to-length ratio of the maxillary anterior teeth because they are critical elements for formulating a pleasing smile.24 A silicone index was made of the incisal edges to aid in the wax-up. After patient approval of the wax-up (Figure 5), an intraoral mock-up was fabricated using Luxatemp (DMG America, https://www.dmgamerica.com) (Figure 6). The patient could visualize the proposed relationship of the incisal edge parallel to her lower lip, closure of the spaces, lightening of her teeth, and the relationship of the dentition to the surrounding soft tissue after the proposed gingival and osseous recontouring were accomplished. In the following visit, a fiber post (D.T. Light-Post® Illusion™, Bisco, https://www.bisco.com) was placed in tooth No. 13. A post placement kit with One-Step® Plus (Bisco) as the bonding agent and Duo-Link™ (Bisco) as the luting agent was used. A composite core was fabricated (RapidCore® MiniMix™, Centrix Dental, https://www.centrixdental.com) and the provisional was created with Luxatemp.
Then, crown lengthening with an osseous recontouring procedure was performed on teeth Nos. 6 to 12 to correct the gingival height and allow the creation of ideal tooth dimensions. The wax-up and subsequent bis-acryl mock-up demonstrated the need for lengthening the teeth at the incisal edges and gingival margins. The incisal edge position is selected first relative to the upper and lower lips. The height that will correspond to the desired width dictates the position of the gingival margin. The appropriate gingival zenith should be incorporated into the template.25 This is especially important when moving midlines, as illustrated here. The surgeon must have such information to perform the crown lengthening. The designated gingival outlines can be marked on a model, and a clear vacuum-form template can be adapted over the model and cut to follow the gingival outline. This guide can be used for the subsequent surgery to provide accurate position of the margins.26
Measurements of sulcular depth, attached gingiva, and bone sounding prior to the surgery (Figure 7) allows for proper formation of biologic width. Gargiulo et al27 reported the biologic width to be, on average, 2.04 mm, with 0.97 mm occupied by junctional epithelium and 1.07 mm occupied by connective tissue attachment to the root surface. Vacek et al28 found 1.34 mm +/- 0.84 mm for sulcus depth; 1.14 mm +/- 0.49 mm for epithelial attachment; 0.77 mm +/- 0.32 mm for connective tissue attachment, and 2.92 mm +/- 1.69 mm for loss of attachment. This supported the concept that the connective tissue attachment is a variable width. However, this is an average and to obtain a precise measurement for a particular patient, bone sounding must be done. If biologic width is violated in a thin biotype, bone loss and gingival recession will occur. In a thick biotype, bone resorption may result in a vertical osseous defect, pocketing, and chronic inflammation.29 Rosenberg30 believed a 6-month wait prior to the final impression was necessary, while Pontiero and Carnevale indicated changes can occur up to 12 months after surgery.31 Two weeks after the initial crown-lengthening procedure, the gingival zenith positions were refined. Chu et al32 found all central incisors have a distal gingival zenith position from the vertical bisected midline of approximately 1 mm, lateral incisors have a slight deviation distal of 0.4 mm, and canines have the gingival zenith position concurrent with the vertical bisected midline, or 0 mm. The gingival zenith level of the lateral incisors is usually 1 mm below a line connecting the gingival zenith level of the adjacent teeth.
Teeth Nos. 7 to 11 were prepared slightly into the sulcus for zirconium crowns (Lava®, 3M ESPE, https://www.3mespe.com) because of their darkness (Figure 8). Provisionals were fabricated with Luxatemp® Fluorescence (DMG America), using the preparation guide fabricated from the wax-up. Then, teeth Nos. 22 to 26 were prepared for feldspathic porcelain veneers, employing the same preparation guide. Provisionals were created with Luxatemp Fluorescence. Subsequently, teeth Nos. 4, 5, and 12 were prepared for the crowns and provisionals fabricated with Structur® Premium (VOCO America, https://www.voco.com). Then, tooth No. 28 was prepared for a porcelain-fused-to-metal (PFM) crown. A PFM was treatment-planned to permit the use of a crown with a distal ball attachment. The use of an attachment eliminated the need for a clasp near the esthetic zone.
During the maturation period of the maxillary periodontium, the patient was able to assess the esthetics and could function because of the provisional restorations. Impression copings were positioned in the Nos. 14 and 15 molar sites (complete seating verified by radiograph), and a retraction cord (Ultradent, https://www.ultradent.com) was placed (Figure 9). Final impressions of the maxillary and mandibular arches were obtained with Impregum™ (3M ESPE). Shades of the future restorations and stump were chosen (Figure 10). The vertical dimension was maintained by keeping occlusal stops with the implant provisionals and the right and left posterior molars in contact. At the following visit, the fabricated crowns were cemented with FujiCEM (GC America, https://www.gcamerica.com) and the porcelain veneers (Figure 11) were bonded with Choice™2 translucent veneer cement (Bisco, https://www.bisco.com), which is a light-cured luting material without tertiary amines that may cause yellowing over time.33 New maxillary and mandibular pick-up impressions were taken and sent to the laboratory for fabrication of a cast partial denture with the female part of the ball attachment on the right and conventional circumferential clasps on the left in the molar area. This was to reduce visibility of the clasps. The patient was pleased with the restoration of esthetics and function (Figure 12 and Figure 13).
Discussion
The treatment of multiple anterior diastemata in conjunction with a worn dentition requires proper diagnosis of etiologic causes and may necessitate an interdisciplinary treatment plan. Restoration of a worn dentition can be demanding especially when restorative space is lacking. The relatively recent development of more predictable dentin bonding and high-strength ceramic crowns requires a better understanding of the indications for these materials and techniques. Traditional biomechanical principles of preparation for full-coverage and porcelain veneers must be mastered. Cement selection is guided by the restorative material used and the location of the restoration margin relative to the gingival sulcus. Crown preparations with margins past the cementoenamel junction would benefit from the use of a resin-modified glass ionomer. Preparations with inadequate remaining tooth structure would require resin cement.34 The gingival levels of the maxillary anterior teeth also need to be considered. Typically, an adult will demonstrate marginal discrepancies due to wear or abrasion of the incisal edges. Compensatory eruption will contribute to the creation of uneven gingival levels and unequal crown lengths, which need to be addressed. Crown lengthening or orthodontic intrusion or extrusion has to be considered. If orthodontic procedures are used, the tooth positions need to be retained for approximately 6 months.35 A diagnostic wax-up is critical to envision the final esthetic outcome.
Conclusion
This case report illustrates the interaction of the different aspects of dentistry to achieve an esthetic, biologic, and functional result. A combination of sinus lifts and subsequent implant placement, crown lengthening, and fixed and removable prosthetics were required. Anterior guidance, leveling of gingival margins, restoration of edentulous spaces, and a stable occlusion were achieved through vigilant treatment planning.
Acknowledgment
The authors wish to thank Dr. Mehrdad Ijadi for the periodontal surgery and Pat Rector at BonaDent Dental Laboratories Seneca Falls, NY, for the laboratory work.
References
1 Van der Geld P, Oosterveld P, Van Heck G, et al. Smile attractiveness. Self-perception and influence on personality. Angle Orthod. 2007;77(5):759-765.
2. Vailati F, Belser UC. Full-mouth adhesive rehabilitation of a severely eroded dentition: the three-step technique. Part 1. Eur J Esthet Dent. 2008;3(1)30-44.
3. Chay SH, Ho KK. Spaced dentition—open, close or redistribute. Annals of the Royal Australasian College of Dental Surgeons. 2000;15:83-86.
4. Furuse AY, Franco EJ, Mondelli J. Esthetic and functional restoration for an anterior open occlusal relationship with multiple diastemata: a multidisciplinary approach. J Prosthet Dent. 2008;99(2);91-94.
5. Bolton WA. Disharmony in tooth size and its relation to the analysis and treatment of malocclusion. Angle Orthod. 1958;28:113-130.
6. Akylçin S, Doğan S, Dincer B, et al. Bolton tooth size discrepancies I skeletal Class I individuals presenting with different dental angle classifications. Angle Orthod. 2006;76(4):637-643.
7. Waldman AB. Smile design for the adolescent patient—interdisciplinary management of anterior tooth size discrepancies J Calif Dent Assoc. 2008;36(5):365-372.
8. Oesterle LJ, Shellhart WC. Maxillary midline diastemas: a look at the causes. J Am Dent Assoc. 1999;130(1):85-94.
9. Huang WJ, Creath CJ. The midline diastema: a review of the etiology and treatment. Pediatr Dent. 1995;17(3):171-179.
10. Stockton HJ. Abnormal frenum attachment controversial. Oral Health. 1969;59(7):25.
11. Malkoc MA, Sevimay M, Yaprak W. The use of zirconium and feldspathic porcelain in the management of the severely worn dentition: a case report. Eur J Dent. 2009;3:75-80.
12. McIntyre F. Restoring esthetics anterior guidance in worn anterior teeth. A conservative multidisciplinary approach. J Am Dent Assoc.2000;131(9):1279-1283.
13. Dawson PE. Evaluation, Diagnosis and Treatment of Occlusal Problems. 2nd ed. St Louis, Mo; Mosby; 1989.
14. The glossary of prosthodontic terms. J Prosthet Dent. 2005;94(1):10-92.
15. Prasad S, Kuracina J, Monaco EA Jr. Altering occlusal vertical dimension provisionally with base metal onlays: a clinical report. J Prosthet Dent. 2008;100(5):338-342.
16. Bernardo JK, Maia EA, Cardoso AC, et al. Diagnosis and management of maxillary incisors affected by incisal wear: an interdisciplinary case report. J Esthet Restor Dent. 2002;14(6):331-339.
17. Fradeani M. Evaluation of dentolabial parameters as part of a comprehensive esthetic analysis. Eur J Esthet Dent. 2006;1(1):62-69.
18. Steuer S. Esthetic rehabilitation of anterior teeth with consideration of periodontal and functional parameters Part 1: diagnosis and treatment planning. Eur J Esthet Dent. 2009;4(2):152-162.
19. Simon H, Magne P. Clinically based diagnostic wax-up for optimal esthetics: the diagnostic wax-up. J Calif Dent Assoc. 2008;36(5):355-362.
20. Kokich VG, Spear FM. Interdisciplinary management of anterior guidance: a case report. Advanced Esthetics & Interdisciplinary Dentistry. 2007;3(3):17-24.
21. Spear FM, Kokich VG, Mathews DP. Interdisciplinary management of anterior dental esthetics. J Am Dent Assoc. 2006;137(2):160-169.
22. Spear F, Holloway J. Which all-ceramic system is optimal for anterior esthetics? J Am Dent Assoc. 2008;139:(suppl):19S-24S.
23. Donovan TE. Factors essential for successful all-ceramic restorations. J Am Dent Assoc. 2008;139:(suppl):14S-18S.
24. Duarte S Jr, Schnider P, Lorezon AP. The importance of width/length ratios of maxillary anterior permanent teeth in esthetic rehabilitation. Eur J Esthet Dent. 2008;3(3):224-234.
25. Mattos CM, Santana RB. A quantitative evaluation of the spatial displacement of the gingival zenith in the maxillary anterior dentition. J Periodontol. 2008;79(10):1880-1885.
26. Chiche GJ. Aesthetic previews for gingival alterations. International Dentistry SA. 2007;9(5):40-44.
27. Gargiulo AW, Wentz FM, Orban B. Dimensions and relations of the dentogingival junction in humans. J Periodontol.1961;32:261-267.
28. Vacek JS, Gher ME, Assad DA, et al. The dimensions of the human dentogingival junction. Int J Periodontics Restorative Dent. 1994;14(2):154-165.
29. Kois J. The restorative-periodontal interface: biological parameters. Periodontol 2000.1996;11:29-38.
30. Rosenberg ES, Cho SC, Garber DA. Crown lengthening revisited. Compend Contin Educ Dent. 1999;20(6):527-538.
31. Pontoriero R, Carnevale G. Surgical crown lengthening: a 12-month clinical wound healing study. J Periodontol. 2001;72(7):841-848.
32. Chu SJ, Tan JH, Stappert CF, et al. Gingival zenith positions and levels of the maxillary anterior dentition. J Esthet Restor Dent.2009;21(2):113-120.
33. Schneider LF, Pfeifer CS, Consani S, et al. Influence of photoinitiator type on the rate of polymerization, degree of conversion, hardness and yellowing of dental resin composites. Dent Mater. 2008;24(9):1169-1177.
34. Mizrahi B. The anterior all-ceramic crown: a rationale for the choice of ceramic and cement. Br Dent J. 2008;205(5):251-255.
35. Bellamy LJ, Kokich VG, Weissman JA. Using orthodontic intrusion of abraded incisors to facilitate restoration: the technique’s effect on alveolar bone level and root length. J Am Dent Assoc.2008;139(6):725-733.
 Figure 1 Patient exhibited spacing, discolored teeth, and a reverse smile. | 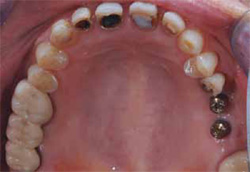 Figure 2 Occlusal view of the maxillary arch demonstrating wear, decay, and implants. | ||||||
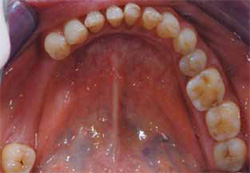 Figure 3 Occlusal view of the mandibular arch demonstrating edentulous area and worn posterior teeth. | 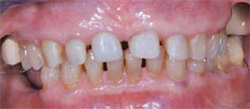 Figure 4 Patient presented with blunted gingival papilla, irregular gingival zenith, reverse smile, and an extruded right posterior segment. | ||||||
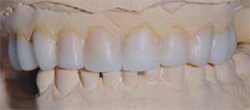 Figure 5 A diagnostic wax-up demonstrated esthetic potential. | 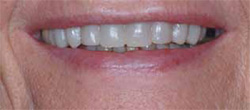 Figure 6 Facial view of intraoral mock-up of the wax-up with bis-acryl resin. | ||||||
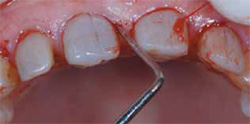 Figure 7 Bone sounding prior to crown lengthening to determine where osseous recontouring was required. | 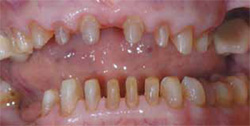 Figure 8 Maxillary and mandibular teeth prepared for zirconium crowns and feldspathic porcelain veneers. | ||||||
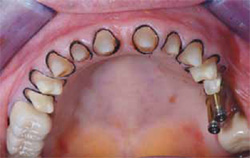 Figure 9 Retraction cord was placed prior to final impression. | 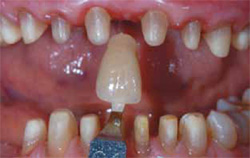 Figure 10 Stump shade was selected. Dark color needed to be masked. | ||||||
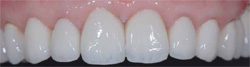 Figure 11 Lava crowns after cementation effectively masked the dark teeth underneath with slight gingival asymmetry present. | 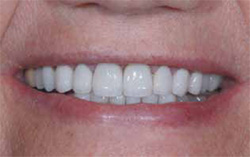 Figure 12 Smile is parallel to lower lip and slight gingival asymmetry is not visible. | ||||||
 Figure 13 Full facial view demonstrates smile parallel to the pupils of the eyes, midline coinciding with the maxillary philtrum, filling of the buccal corridor, dramatic shade change, and proper tooth proportion. | |||||||
| |||||||



