A Conservative Alternative to Implant Therapy
A telescopic prosthesis provides stability and retentiveness
By Arian Deutsch, CDT
In a world where implants are becoming the standard of treatment, many times implant therapies are over-prescribed, and perfectly good teeth are overlooked as a viable option to utilize in treatment plans. The overwhelming trend has been to remove all partial dentition, with full-arch replacement as the goal. What are some issues with this method and what is truly best for the patient?
It has been well documented that implant bar treatments with acrylic fixed hybrids are not very hygienic, and can present the clinician with a number of problems and issues requiring a significant amount of chair time in the long term.1,2 Additionally, in fully edentulous patients, proprioception is lost and the periodontal ligament is gone.
As technicians, it is not our responsibility to decide how to proceed with treatment. But isn’t it true that most of the time technicians are called upon to give opinions and offer solutions? Therefore, education in a variety of solutions is imperative, including some conservative alternatives to implant therapies.
In addition, in many cases implant therapies may not be an option due to a variety of reasons including inadequate available bone, financial limitations, etc. A technician does well to ask: When I offer a solution, what is the driving force behind the advice I give? Is it what is best for the patient? Is it based on longevity of the prosthesis? Is it money? Or is it a combination of all the above? Every situation should be treated as unique.
As an integral part of the dental team, the technician should address the need to speak and listen to patients in order to know how to proceed and meet their expectations. It may require more time in the beginning, but it will always reduce problems in the end. It has been noted that when a patient senses the camaraderie of the team working on his or her behalf, that patient is more willing to accept suggestions and recommendations based on the expertise of the professional dental team. Again, it is not the responsibility of the technician to prescribe treatment, but it is necessary to be included in the consultation and planning phases for the success of the case.
What is the technician’s time worth? Everyone needs to determine that on an individual basis. In the author’s experience, it is best to figure out what one’s time is worth on an hourly basis and charge accordingly when in the consulting phase. This should be a separate charge from the actual laboratory fees, because it may require significant time and research.
Example Case
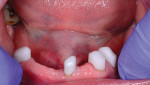
A client called for consultation on a case. The patient presented with a fully edentulous maxilla and partial mandibular dentition. Because the dentition on the mandible was healthy and stable, and implants were not an option due to cost and possible complications, it was decided that a tooth-borne telescopic restoration would best suit the patient’s needs and desires. The patient was presented with multiple options, and she decided that a telescopic prosthesis was right for her situation. The patient had good hygiene habits and good dexterity, which are ideal for this solution.
Telescopic Solutions
Telescopic solutions have a long history of success in Europe and to this day are often the standard of treatment. The treatment dates as far back as the 1940s and 1950s, when Professor Arnold Gaerny documented it in his book Closure of the Interdental Space With a Removable Device. Over the span of decades the concept has remained the same but now utilizes more modern materials. Currently, one protocol utilizing zirconia and galvano gold is yielding very favorable results.
In the case presented here, the maxillary denture was planned with an ideal occlusal plane in mind, and fabricated in staged timing with the mandibular telescopic prosthesis. For the purposes of this article, the focus will be on the mandibular telescopic prosthesis.
Mandibular Telescopic Prosthetic
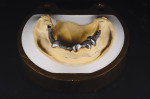
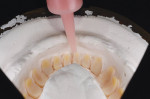
The dentist prepared the remaining mandibular teeth for the primary telescopic crowns, which would be fabricated in zirconia. A mandibular impression was made with a custom tray. Once a preliminary model had been poured in Type IV resin reinforced gypsum (GC Fujirock IMP, GC America Inc., gcamerica.com), a digital scan was performed and the primary telescopic crowns were digitally designed (Figure 1 and Figure 2).
The crowns were milled, sintered, and placed back onto the initial cast. A custom tray was made with the telescopic crowns in place. A pickup impression of the telescopic crowns was taken with the custom tray. It is sometimes best to provide a seating jig for clinical use as well. The telescopic crowns were now in the master impression. To provide a stable and usable foundation cast, GC Pattern Resin LS (GC America Inc.) was used to fill the inside of the telescopic crowns, and retention was added.
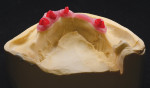
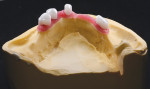
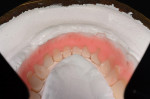
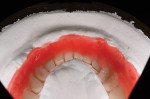
The impression was boxed and poured using GC Fujirock IMP. Soft tissue material can be used if desired and was in this case (Figure 3 and Figure 4).
The primary telescopic crowns were then hand milled at 2° using a Schick Dental S3-Master Milling Unit with the S3-Ceramic Milling Set Upgrade (Vacalon, vacalon.com). The hand milling was carried out with the high-speed water turbine with a series of five diamond milling burs down to 4 μm (Meisinger, meisinger.de) and subsequently dry-polished on the hand mill with a series of three diamond-impregnated polishers to obtain a very highly polished surface. This highly polished surface is similar to glass in that very little wear results on the secondary galvano gold telescopes (Figure 5 and Figure 6).
Galvano Gold
When the primary zirconia telescopic crowns were polished and finished, preparations were made for the galvano or electroforming of the secondary gold telescopic component. This step is very important and can be created either directly or indirectly with very predictable results. The electroforming process facilitates an extremely intimate fit of between 4-5 μm of the secondary telescope to the primary telescope.
This fit, coupled with the passive intraoral pickup technique, easily surpasses any CAD/CAM milled interface in terms of both fit and passivity. In addition, because the periodontal ligament and proprioception were still intact, it is not necessary to think so much in terms of AP spread, etc, although some basic engineering principles must be kept in mind.
In this case, the secondary telescopes were made indirectly on dies. The primary zirconia telescopes were poured in duplicating silicone (GC Polypour™, GC America Inc.) and, once completely set, were poured in vacuum-mixed Type IV resin reinforced die stone (GC Fujirock IMP). The dies were prepared by coating with a conductive silver lacquer, and connected to an electroforming unit (GAMMAT® Easy, Gramm Technik, grammusa.com).
Once the galvano process was complete (after approximately 6 hours), the dies were removed, rinsed, and placed into stone-and-plaster remover in an ultrasonic unit in order to remove the gypsum dies from the gold telescopes. At this point, any remaining conductive silver lacquer needed to be removed. The most efficient method, in the author’s opinion, is to submerse them in a nitric acid solution and place them into an ultrasonic unit for approximately 15-20 minutes. In this case a 40% nitric acid solution was used (American Dental Supply Inc., americandentalinc.com). The nitric acid was then neutralized and the gold telescopes were rinsed (Figure 7).
The secondary gold telescopes were fit to the primary zirconia telescopes and could be removed using telescopic pliers.
Tertiary Structure
On the master cast with both primary and secondary telescopes in place, another digital scan was performed and a tertiary structure was designed. The secondary gold telescopes would be cemented into this non-precious tertiary structure intraorally to ensure complete passivity.
Once approved by the clinician, the digital design was transmitted to the SLM facility (Bego USA, begousa.com), and the selective laser melting process began. The process provides a very accurate tertiary structure with a precise cementation gap.
Both the secondary galvano telescopes and SLM tertiary structure were prepared for cementation by air abrasion with aluminum oxide at 2-bar pressure. They were then steam cleaned and additionally cleaned with denatured alcohol. A metal primer was applied (GC Metal Primer, GC America Inc.), and it was light cured. The tertiary structure was sent with both primary and secondary telescopes to the clinician. At this appointment the clinician temporarily seated all telescopic primary crowns and secondary telescopes, being sure to keep a dry field. The tertiary structure was checked over the secondary telescopes to ensure passivity and adjusted as necessary. The SLM tertiary structure could now be cemented to the secondary galvano gold telescopes intraorally using an adhesive resin cement (GC G-CEM™, GC America Inc.).
Final Wax Check with Hardware
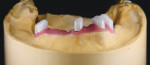
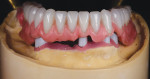
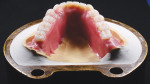
Using the intraoral pickup, the master cast could be altered to reflect the corrected, passive position of the primary telescopes. The tooth positioning was now transferred to the corrected master cast using a silicone putty matrix (Matrix Form 70, anaxdent North America, anaxdentusa.com), and a complete wax try-in with hardware could be performed (Figure 8 through Figure 10).
Processing and Finishing
A duplicate processing cast was poured using duplicating silicone (GC Polypour) and vacuum mixed Type IV resin reinforced gypsum (GC Fujirock IMP). The wax-up was seated and the secondary telescopes were protected with a VPS/Polyether hybrid impression material (GC EXA’lence™ Light Body, GC America Inc.). The wax-up was sealed and refined and finally invested in the flask (Figure 11 and Figure 12).
Once the wax had been eliminated, a separator (GC Coe-Sep™, GC America Inc.) was applied to the surfaces of the investment and cast, and the SLM tertiary structure was cleaned and prepared (Figure 13 and Figure 14). In some cases the SLM tertiary structure is opaqued if metallic show-through is likely.
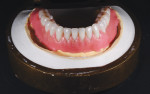
The gingival characterization was now created using a variety of heat-cured acrylic powders that had been sifted (GC Nature-Cryl® Super Hi Impact, GC America Inc.), using a syringe technique to place the colors where desired, and a Kolinsky brush to manipulate the colors and blend them together. Blue and red modifiers were swirled into the more vascular colors to add some randomness to the color scheme (Figure 15 through Figure 17). The case was trial packed, and then final pressure was applied and cured using a base acrylic (GC Nature-Cryl Super Hi Impact Original shade, GC America Inc.) according to the manufacturer’s instructions. The case was carefully deflasked, trimmed, and finished with a variety of burs, and then brushed and final polished to achieve a high shine (Figure 18 and Figure 19).
Delivery
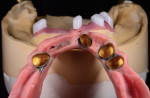
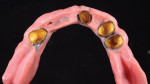
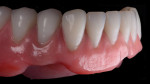
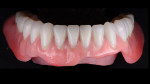
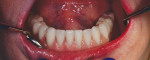
On the day of delivery, the process went very smoothly due to good planning; the focus, as it should be, was on the patient. The primary telescopic zirconia crowns were final cemented over the preparations (Figure 20), and any excess cement was removed. The prosthesis was seated during the cementation to ensure passivity (Figure 21).
A check of occlusion and excursive and protrusive movements was made. The patient was instructed on how to insert and remove the telescopic prosthesis, and was observed inserting and removing the prosthesis several times. The patient was also instructed regarding care of the primary cemented telescopic crowns, and a follow-up appointment and hygiene regimen were scheduled.
Conclusion
The patient’s desires and expectations were met, and the patient had been treated using a conservative option that was very stable and retentive. The final outcome replaced the missing dentition and gave the patient back her security and confidence. However, this did not occur haphazardly. It required good communication among all dental team members, from the patient consultation, to the treatment planning with the clinician, and through careful treatment to achieve the final outcome.
References
1. Kwon T, Bain PA, Levin L. Systematic review of short- (5-10 years) and long-term (10 years or more) survival and success of full-arch fixed dental hybrid prostheses and supporting implants. J Dent. 2014;42(10):1228-41.
2. Bozini T, Petridis H, Garefis K. A meta-analysis of prosthodontics complication rates of implant-supported fixed dental prostheses in edentulous patients after an observation period of at least 5 years. Int J Oral Maxillofac Implants. 2011;26(2):304-18.
3. Gaerny A. Removable Closure of the Interdental Space (CIS). Hassell TM, trasn-ed. Berlin, Germany: Buch und Zeitschriften-Verlag; 1972.
About the Author
Arian Deutsch, CDT
Owner
Deutsch Dental Arts
Surprise, Arizona