Simplified Posterior Restorations with Monolithic Pressed Ingot
Achieve production efficiency and esthetics
The traditional cut-back and layering techniques necessary to create esthetic and lifelike pressed restorations can be time-consuming for ceramists. Yet, creating strong, esthetic, and durable restorations is the standard of care that is demanded by both dentists and patients. Regardless of whether the restoration is placed in the anterior or posterior, harmonious shade blending and translucency similar to natural teeth is expected.
To realize enhanced and simplified esthetics, an alternative to using cut-back and layered pressed restorations is fabricating a full-contour monolithic restoration. For several years, this has been possible with CAD/CAM restorations milled from ceramic blocks that have multidimensional shades within them.1-3
However, what has been necessary is a pressable material that is inherently progressive in its chroma and opacity from the cervical to dentin regions, and suitably translucent in the incisal areas. Fortunately, a new lithium disilicate ingot (IPS e.max® Press Multi, Ivoclar Vivadent, ivoclarvivadent.us) now can be used to predictably press highly esthetic and natural-looking full-contour monolithic restorations that not only require minimal staining and glazing for customization, but also demonstrate the strength required for posterior cases.4
These ingots eliminate the need for ceramists to cut back and layer pressed restorations in order to achieve the desired esthetics. This not only contributes to greater fabrication efficiency but also ensures functional durability, because these restorations have been shown to demonstrate greater fracture resistance than other posterior options (eg, bilayered zirconia/ceramic).4 In fact, the heat-pressed monolithic lithium disilicate material exhibits a strength of 400 MPa.
The following case outlines the simplified fabrication, staining, and glazing of an esthetic full-contour monolithic pressed restoration using this new ingot.
Fabrication Technique
An 81-year-old female presented with a fractured mesial lingual cusp to the gingival line on tooth No. 14, which had a large amalgam restoration and would need a full crown. Tooth No. 14 was prepared, and an impression was taken. The patient’s shade was determined to be Ivoclar 430 gingival and VITA D2 incisal. The laboratory ceramist received the records needed for fabricating the posterior full-coverage crown restoration for tooth No. 14, which included preoperative and preparation photographs, study models, and shade requirements. Because the restoration would function in the posterior and, therefore, require appropriate strength to withstand mastication forces, a monolithic lithium disilicate material (eg, IPS e.max Press Multi, Ivoclar Vivadent) was chosen. The ceramist discussed the use of the new Press Multi ingot with the dentist, explaining that it was made from multiple gradiated translucencies, with the gingival being the least translucent and the incisal being the most translucent. They decided that this ingot would provide the desired esthetics.
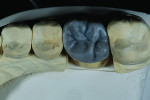
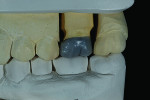
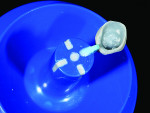
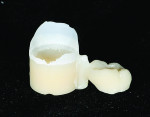
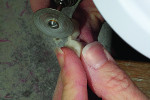
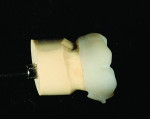
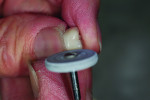
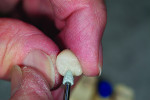
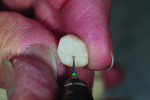
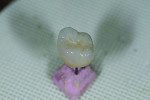
A wax-up of the restoration was created to full contour on the model (Figure 1 and Figure 2). The Press Multi ingot sprue was placed on the crown wax-up (Figure 3), after which it was placed on the sprue former (Figure 4), which is used only for this particular ingot. Care was taken to wax the unused slots to avoid breakage of sharp angles during the pressing process.
The wax-up was then invested using a speed vacuum (PressVest Speed, Ivoclar Vivadent) (Figure 5). A 200-gram quantity of investment was used (Figure 6) and mixed in the vacuum for a full 2.5 minutes (Figure 7). Following this process is essential to avoid investment breakdown. To avoid trapping an air bubble, the investment was applied to the occlusal crown surface (Figure 8). Investment also was applied to the inside of the crown wax-up, and the investment ring was filled (Figure 9). The ring was set on the bench for 30 minutes and then directly burned out in the furnace at 1562° F for 1 hour.
Other components of the press system were used to prepare for pressing. These included an Alox plunger (Alox Plunger, Ivoclar Vivadent) that would be used to press the softened ingot into the hollow space in the investment ring, and a one-way plunger to prevent the ingot from sticking to the Alox Plunger during pressing (Figure 10). The appropriate lithium disilicate ingot was selected with the prescribed shade requirements. For this case, the gingival shade was 430 and the incisal was D2, making a C1 ingot ideal for easy staining.
The investment ring was seated upside down on the ringer holder to allow the wax to run out while heating up in the furnace (Figure 11). The C1 ingot was placed face up in the ring, followed by the one-way plunger and Alox plunger. The investment ring then was placed in the pressing furnace (Programat EP 5000, Ivoclar Vivadent) (Figure 12), and pressing was initiated using the Multi Ingot 200-gram program (Figure 13).
The finished press was allowed to cool (Figure 14), and the sprue channel removed using a diamond disk (Figure 15). Care was taken to avoid hitting the crown with the diamond disk. The restoration then was divested by first blasting the investment from the crown using 80-micron glass beads at 60 psi (Figure 16) and then placing it in an investment liquid (IPS e.max Press Invex, Ivoclar Vivadent) for 20 minutes to soften the surface reaction layer that formed during the pressing procedure (Figure 17). A final blast was performed with 100-micron aluminum oxide to clean any remaining investment from the crown.
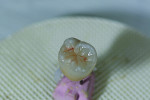
The pressed restoration was removed from the sprue holder, with care not to overheat it (Figure 18). The crown was seated on the model (Figure 19) and then rubber wheeled using a white diamond impregnated rubber wheel (EVE Universal 22, EVE Ernst Vetter, eve-rotary.com) (Figure 20). The occlusal grooves were first refined using a fine-point Cardinal 8002.040 HP (Cardinal Rotary Instruments, cardinalrotary.com) (Figure 21), and then again using a round Komet ZR 6801 FG 010 (Komet USA, kometusa.com) (Figure 22). Note that to prevent cracking the crown, a point should not be used to clean the occlusal grooves. To prepare for staining and glazing, the crown was lightly blasted and steamed (Figure 23).
To characterize the monolithic posterior crown restoration, a variety of stains were placed to respectively recreate the 430 using IPS e.max Shade 3 gingival, as well as the D2 using IPS e.max Shade 4 (Figure 24). The first stain was completed by applying IPS e.max dark blue, along with a mixture of Blue and Pink, to create the violet that would accentuate the D2 incisal. A slight amount of Shade 4 was placed in the central occlusal groove of the occlusal (Figure 25). This first stain was fired in a Programat P700 set to the IPS e.max Stain and Glaze program.
The second stain focused on the occlusal grooves, for which a mixture of IPS e.max Mahogany and Orange were used. In addition, a small amount of white was placed on the occlusal cusp tips (Figure 26). This second stain was fired and the shade verified (Figure 27).
Conclusion
IPS e.max Press Multi ingots are changing the way laboratory ceramists fabricate posterior restorations using pressing techniques. Because the ingots demonstrate a lifelike shade progression from the dentin region to the incisal areas, they enable ceramists to achieve production efficiency and esthetic excellence when creating multidimensional restorations in a monolithic form (Figure 28).
References
1. Kurbad A. Three-dimensionally layered ceramic blocks. Int J Comput Dent. 2010;13(4): 351-365.
2. Reich S, Hornberger H. The effect of multicolored machinable ceramics on the esthetics of all-ceramic crowns. J Prosthet Dent. 2002;88(1):44-49.
3. Della Bona A, Nogueira AD, Pecho OE. Optical properties of CAD-CAM ceramic systems. J Dent. 2014;42(9):1202-1209.
4. Altamimi AM, Tripodakis AP, Eliades G, Hirayama H. Comparison of fracture resistance and fracture characterization of bilayered zirconia/fluorapatite and monolithic lithium disilicate all ceramic crowns. Int J Esthet Dent. 2014;9(1):98-110.
About the author
Glynn Watts, CDT, DTG
President/Owner
Advantage Dental Design Lab
Tallahassee, FL