New Option for a Common Esthetic Compromise in Fully Edentulous Maxillary Implants
Helping to solve a longstanding quandary
The restoration of the fully edentulous maxillae is among the most difficult of prosthetic procedures. The most common esthetic challenge is the placement of implants in an exaggerated labial-cervical position in the premaxillae. Accounting for this difficulty is the lack of appropriate presurgical planning and prosthetically driven surgical guides.1 When this factor is combined with the issue of implant placement in the long axis of the available maxillary ridge, an esthetic compromise becomes inevitable.
Historically, the technician had to develop a substructure/suprastructure prosthesis to hide the unsightly screw-access holes. This approach complicates fabrication and significantly increases the restorative cost.
Now, the laboratory community has the option of incorporating PRISM 24° Angled Access Channels into the substrate. This patented process utilizes a hexalobular driver/screw head combination, providing a unique principle of engagement. The new technology provides the following restorative benefits:
• The elimination of “space eating” angled abutments reduces the required vertical restorative space by 3 mm to 5 mm.
• The favorable repositioning of the screw-access holes to appropriate esthetic positions improves simplification of production of the restoration, aiding cost control of the final result.
Case Study
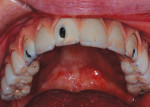
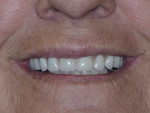
A patient presented with an existing maxillary fixed detachable restoration supported by 5 implants. The original restoration was a CAD/CAM-milled titanium substrate veneered with tooth- and gingiva-shaded composite resins (Figure 1).
The evaluation revealed the retaining screws securing the anterior implants emerged from the facial aspects of teeth Nos. 6, 8, and 11. The initial attempt to improve the resulting esthetic compromise had involved placing veneers over the affected teeth. Upon repeated debonding and fracture of the veneers, composite resin was used to cover the screw-access openings. Eventually the composite had discolored and broken down, leading to an esthetic failure.
The implants were well-integrated, and a replacement prosthesis was indicated. A second thorough diagnosis suggested the ideal retreatment that would meet the patient’s periodontal, esthetic, and functional needs should be the use of an implant-retained overdenture.2 The patient adamantly refused a removable appliance.
As previously discussed, the unfavorable emergence of the anterior fixtures presented a significant esthetic compromise.
The PRISM 24° access channel driver/screw combination, recently introduced by Preat Corporation, was selected to address this situation (Figure 2). The revolutionary restorative solution provides the opportunity to redirect unfavorable emergence positions in the esthetic zone.
Clinical Procedure
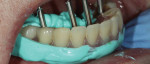
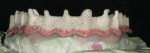
The case was impressed using the open-tray technique, “picking up” the existing restoration (Figure 3 and Figure 4). This approach requires the syringing of material between the interior surface of the prosthesis and residual ridge, capturing the current position of the soft tissue. The external surfaces were captured with a loaded tray with access holes exposing the guide pins.
This technique proves to be efficient and extremely accurate due to the use of the clinically verified inter-implant and occlusal relationships provided by the existing appliance, eliminating the need for occlusal rim and cast-verification indices and corresponding patient appointments.
Laboratory Procedure
The technician loaded the appropriate analogs onto the impression copings and poured the beaded and boxed impression to create the master cast. After articulation, a putty matrix relating the maxillary teeth to the mandibular arch was accomplished (Figure 5).
For the study cast, the technician impressed the appliance and poured in gypsum. This provided the information required to match the existing teeth.
New prosthetic teeth were set on a screw-retained baseplate and returned to the clinician for try-in to confirm the occlusion and the esthetic arrangement of the teeth. After successful completion of the try-in, a new putty matrix was developed relating the new prosthetic teeth and arrangement to the opposing arch and master cast.
Selective Laser-Melted Implant Bar Fabrication
Selective laser melting (SLM) was chosen for fabrication. This technology is commonly referred to as additive technology. This recent adaptation of additive technology to the dental manufacturing community is also called rapid prototyping or printing. In general-manufacturing circles, milling has been replaced in large part by this more efficient process. In all developing technology, becoming cost appropriate for the intended user develops with time. Currently, these processes are cost-effective only in central manufacturing business models and when applied to multiple-unit implant prostheses.3
The master cast, wax set-up, and prescription were sent to Preat Corporation for fabrication of the SLM titanium bar.
An additional clinical benefit is realized when the “pearl” macroretentive surface is utilized. This enhanced retention feature is possible only with SLM fabrication technology.
Through this direct manufacturing process, the efficiency and dimensional adaptation of metal dental device fabrication is dramatically improved by elimination of the traditional wax pattern fabricating, investing, and casting steps. The virtually unlimited design possibilities that can be accomplished with additive technology have proven to be possibly the greatest advantage in hybrid implant bar applications.
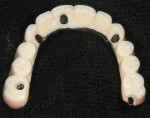
After receipt of the bar, the technician conditioned the bar with bonding agent and applied composite opaque to the surface with A-2 and gingival shades accordingly (Figure 6). The case was processed utilizing the appropriate tooth-shaded and gingival resins.
The successful retreatment accomplished for this patient illustrates recently developed options for corrected emergence and enhanced surface macroretention of resin to the supporting substrate (Figure 7 and Figure 8).
Conclusion
The rapid development of digital technology is positively impacting the restorative team’s ability to constantly improve the caliber of prosthodontic treatment. The dental professional is challenged to stay abreast of the advancements available. Analog processes are being complemented by more digital options, yet patients remain dependent on the team’s didactic thinking for diagnostic input and treatment planning. Because of the availability of these tools, the restorative team becomes more efficient and more consistent.
Acknowledgment
The author thanks Christopher Wine, DDS, the clinician who treated the patient.
References
1. Greenstein G, Cavallaro J, Tarnow D. Practical application of anatomy for the dental implant surgeon. J Periodontol. 2008;79(10):1833-1846.
2. McAndrew K. Treating the edentulous patient with dental implant therapy: a review of treatment considerations. Vistas. 2009;2(2):9-13.
3. Jacobs P. Rapid Prototyping & Manufacturing: Fundamentals of Stereolithography. Dearborn, MI: Society of Manufacturing Engineers; 1992.
David Avery, CDT, TE, is Director of Professional Services for Drake Precision Dental Laboratory in Charlotte, NC.
For more information, contact:
Preat Corporation
800-232-7732
Disclaimer: The statements and opinions contained in the preceding material are not of the editors, publisher, or the Editorial Board of Inside Dental Technology.