Balancing Occlusal Stability and Esthetics
How to establish long-term success in complex implant cases
Peter Pizzi, CDT, MDT, FNGS
Many new material and restorative options have provided technicians with the additional tools needed to meet today’s patient expectations. The complexity of the new technologies, techniques, and materials has made tasks that once were challenging now seem simple in comparison. The new normal for today’s technician is collaborating virtually for implant placement planning, selecting from myriad material choices the one best suited for the case, and using pink ceramic material to restore the loss of gingiva in critical areas. The evolution of technicians and the higher demands in patients’ expectations must continue to find equilibrium, even as technicians’ challenges become more daunting.
The technician’s understanding of white esthetics will always dominate the profession. However, a technician who can restore implant-driven cases or those that incorporate gingival components is becoming more common. In each of these scenarios whether implant-driven or pink ceramic-driven, dental teams must always consider the patient’s functional parameters and facial features. When restoring a patient’s oral situation, part of the technician’s role is to have a solid understanding of occlusion in order to protect the long-term durability of restorations in a working environment. Making the team’s efforts look highly esthetic and natural is only a small percentage of the work of dental technologists. Choosing the appropriate materials, properly supporting the facial appearance, and balancing the patient’s occlusal stability should always be the dental team’s primary goals. Without knowing these three key components, the team is not taking the patient’s long-term stability into account.
Case Report
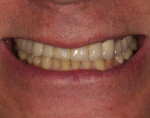
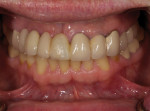
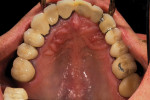
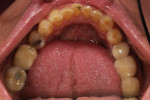
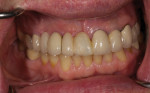
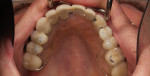
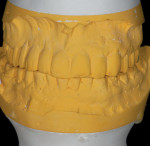
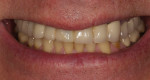
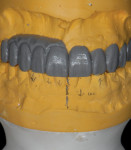
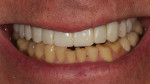
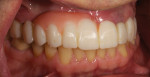
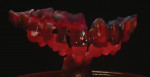
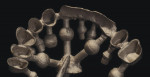
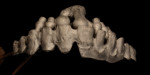
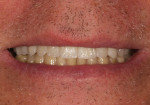
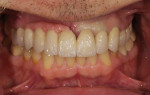
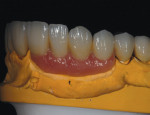
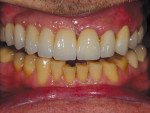
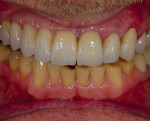
Typically, a patient presents with subpar restorations that lead to the patient’s major complaint that the work is esthetically unacceptable. (Figure 1 through Figure 3). As a technician, the author avoids making judgments on the previous dental team’s work because each case has a story and its own limitations. Without knowing all the circumstances, drawing conclusions may be unfair. Although this patient’s chief complaint was the esthetics of his restored smile, the task at hand was to evaluate the etiology of the patient’s present condition. Facially, the wear and chipping exhibited in the anterior could have been an indication of problematic occlusal wear or related to the patient’s functional habits. On closer examination of the occlusal surfaces, it was determined that one major wear facet existed in the posterior (Figure 4 and Figure 5). The patient informed the dental team that the previous restorative dentist had adjusted the restorations into that position after seating. The lingual surface of the anterior showed more aggressive wear and possible breakage of the existing restorations.
During the evaluation, the patient’s facial features were also taken into consideration for the final esthetic results. A slight decompression was noted on the patient’s right side of the face, indicating a possible negative bony-architecture support and needing to be addressed during the process to improve the final results (Figure 6 and Figure 7).
Occlusion
Treatment for this case involved a discussion on occlusion. The primary focus for the team, based on the visible wear patterns, was on the envelope of motion, which is the full movement that the mandibular arch can achieve as dictated by the bony structures. The envelope is where the mandibular incisal edge works in relationship to the maxillary tooth position. This working, or functioning, position can be the difference between acceptable or problematic function. Periodontal prosthodontist John C. Kois, DMD, MSD, classifies this principle into three basic types of envelopes: 1) acceptable function; 2) dysfunctional envelope; and 3) constricted envelope.
Acceptable function allows working intraorally without any major changes to the patient’s functional relationship. Placing single units to address esthetic challenges can be performed without the risk for damage to restorative materials.
Dysfunctional envelope is present when damage and wear to the system is visible. Concern needs to be taken in regard to the functional parameters of the patient and the restorative materials selected. Posterior wear, anterior wear, migration, or any sign of malfunction will need to be addressed before restorative work can begin in order to prevent placing the restorative options in harm’s way.
Constricted envelope can be extremely treacherous for restorative materials in the esthetic zone, and an understanding of the etiology of the situation is critical. Anterior wear is usually aggressive in a constricted envelope and, in some situations, has little effect on the posterior teeth.
To fully understand the patient’s functional envelope and occlusal situation, the team used a Kois deprogrammer to find the centric relationship (CR), which helped determine that the patient was working in a constricted envelope. The first goal was to remove the constriction. The options were as follows:
orthognathic surgery
orthodontics
restorative
Although each choice presents its own pros and cons, not all patients are in need or accepting of one or all these steps. Based on the esthetic challenges presented by this patient, the dental team chose the restorative option of treatment. The occlusal vertical dimension (OVD) would need to be changed in order to remove the constriction. Whenever the OVD is altered, working in a CR position is a must.
Casts were taken and mounted in the CR position. The mounting and the patient’s photographs were evaluated to confirm the transfer of information (Figure 8 through Figure 11). Once the dental team was confident in the transfer of information based on the photographs, a diagnostic wax-up was begun. The wax-up was accomplished based on the horizontal reference of the transferred information. A gingival component was introduced to the wax-up to reconstruct the negative bony architecture and allow evaluation of the facial support (Figure 12). The wax-up was transferred to the patient via a putty matrix as a provisional (Figure 13 and Figure 14) to evaluate the esthetic and functional parameters that had to be considered. Once the new vertical dimension had been established, the horizontal esthetic plane was photographed and discussed with the dental team. Although the author and dentist were accepting of the esthetic plane, both members believed that the gingival support could be better. The clinician added pink acrylic to improve the facial support. Once the dental team and patient were accepting of the provisionals and proposed esthetic outcome, the choice of restorative material needed to be evaluated.
Materials
Today, myriad restorative material options are available. Although this is a positive trend, it does place responsibility on technicians to understand each of the restorative materials and learn how to use them either individually or together. Large-span bridge frameworks are seen less often in the laboratory due to dentistry’s efforts to save tooth structure and the increased number of implants being placed. For technicians, this allows for much more control of the substructures and the firing parameters for ceramic materials. This patient presented with an edentulous area in the positions for teeth Nos. 6 through 8. The previous bridge had spanned this area with abutments on teeth Nos. 4, 5, 9, and 10 through 13. Because the patient was not a candidate for implants without a major bone graft and sinus lift, single-implant treatment was not an option for restoration. The author and dentist decided to fabricate a long-span bridge to meet the patient’s esthetic and financial concerns. Because of the length of the span, a metal framework with porcelain-fused-to-metal crowns was chosen as the final restorative option.
The Framework
The evolution of materials and processing techniques has provided technicians with alternative methods for fabricating long-span metal bridges. Although conventional hand waxing still plays an important role in the design and fabrication of bridge frameworks, alternative methods such as CAD-designing the framework for automated milling out of wax or metal or using that same CAD creation for selective laser-sintered metal frameworks, to milling a metal particle-infused wax that is then sintered to hardness all offer viable methods of processing in the laboratory. When this case presented to the author, he was using a resin injection technique and conventional casting. A putty matrix of the provisional was fabricated and transferred to the working prepped cast, and resin was injected to fill the void. Because the provisional was accurate, this resin prototype could be cut back and contoured to support the final ceramic (Figure 15). The resin framework was invested and placed in a pressure vessel before the burnout and final induction casting. The combination of the pressure vessel and induction casting produced a very clean and accurate casting (Figure 16 through Figure 18). Fitting time and cleanup was minimal, and the frame was ready for the final ceramic based on the provisional’s esthetic guideline. Ceramic layering was completed. Although the author does not typically request a try-in of cast frameworks, the dental team agreed that this would be best in order to evaluate the gingival color and position (Figure 19 and Figure 20). A second ceramic bake was performed, and the final pink ceramic was added during the glazing process.
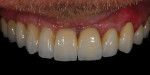
After polishing, the final restoration was inserted and cemented, and the patient and dental team accepted the final esthetics (Figure 21 through Figure 25).
Conclusion
This case demonstrates how a technician who is well-versed on the complexities of modern materials and techniques is an indispensible partner on the dental team.
Acknowledgment
Clinical dentistry for this case was performed by Michael Ricciardi, DDS.
About the Author
Peter Pizzi, CDT, MDT, FNGS
Owner and Manager
Pizzi Dental Studio Inc.
Staten Island, NY