Standards of Infection Control: Surfaces in the Dental Operatory Environment
All dental professionals must be aware of dental surface infection control standards to protect themselves and their patients
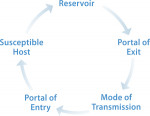
The all-important goal of infection control is to break the chain of disease transmission. Dental healthcare providers (DHCP) must consider every possibility, including cross-contamination, and use the appropriate methods and procedures that break the chain of transmission. Cross-contamination can occur from person to person, from person to object, or from surface to person (Figure 1).
Following the Standards
Standards are defined as the minimum of what must be done to prevent the transmission of infectious agents. Never consider a patient “safe” because of his or her medical history, ethnicity, age, or other personal factors. Every patient must be considered a potential risk for infection. Many people do not fully disclose their medical history and conditions on their medical history forms because they are either embarrassed or do not see the need to disclose them. Some patients are unaware that they even have a communicable disease. Therefore, DHCP must meet infection control standards with each and every patient.
One infection control standard that is often overlooked is how various surfaces should be treated differently. Surfaces in the dental operatory are divided into two categories: clinical and housekeeping.
Clinical Contact Surfaces
Clinical contact surfaces are those that can be directly contaminated by either direct spray from the patient’s mouth and devices used during treatment, or by contact with gloved hands. Clinical contact surfaces may serve as a source of cross-contamination to other instruments, devices, hands, and gloves. Some examples of clinical contact surfaces include dental radiographic equipment, countertops, chairside computer components, light handles and switches, and controls on dental units and chairs.
Housekeeping Contact Surfaces
Housekeeping surfaces, such as doors, walls, and sinks, do not require the same rigorous decontamination procedures as clinical contact surfaces. The majority of housekeeping surfaces need only to be routinely cleaned with a detergent and water. An Environmental Protection Agency (EPA)-registered hospital disinfectant may be used if it is suspected that these surfaces have been contaminated with blood or bodily fluids. Mops and cloths should be cleaned, rinsed, and allowed to dry between uses. If there is visible blood contamination, the housekeeping surface should be carefully cleaned, followed by application of an EPA-registered hospital disinfectant.
Conclusion
By following the CDC guidelines correctly, all dental practitioners, including dental assistants, can do their part in making the dental operatory and dental practice safe from infectious agents. It is the responsibility of all clinical dental staff to know what these guidelines recommend and to stay updated on any additional information regarding infection control in the dental practice.
Source
Centers for Disease Control and Prevention. “Guidelines for Infection Control in Dental Health-Care Settings – 2003.”Available at: https://www.cdc.gov/mmwr/preview/mmwrhtml/rr5217a1.htm. Accessed June 18, 2014.