Personal Barriers Protect Dental Personnel
Eve J. Cuny, RDA, MS
During the course of a working day, dental healthcare personnel (DHCP) can expect to encounter a wide range of materials that present the possibility of either injury or illness. Droplets containing blood and saliva that result from dental procedures present an inhalation and contact risk; sharp contaminated instruments present a contaminated percutaneous injury risk; and chemicals used for disinfection and dental treatment present an inhalation or contact risk. Encounters with all of these require the use of prudent precautions to avoid hazardous exposures. In addition to reducing the opportunity for exposure by substituting less hazardous substances and minimizing spray and spatter of body fluids, DHCP should select personal protective equipment suitable to the type and degree of exposure that they anticipate. All chemical products should have a Material Safety Data Sheet (MSDS) that details the types of hazardous exposures associated with the product (eg, damage to eyes, ingestion hazard, skin irritation, etc), and the appropriate protective measures. Many materials used in the manufacture of medical gloves will not protect against chemical exposures.
Regulations and Guidelines OSHA
The Occupational Safety and Health Administration (OSHA) regulates workplace safety in the United States either through federal regulation or state-sponsored OSHA programs. In dentistry, one of the areas covered by the Bloodborne Pathogens Rule1 is the use of personal protective equipment (PPE). There are no specific requirements regarding the types of materials for PPE. Rather, the regulations require that the employer assess the potential for exposure based on the nature of procedures typically done in a particular practice and select the appropriate protective attire.
The intention of PPE in dentistry is to prevent workers' skin, eyes, nose, mouth, and other mucous membranes from coming into contact with a patient's blood or other potentially infectious materials (OPIM), including saliva. Other requirements include providing PPE in appropriate sizes, replacing when necessary, and maintaining and laundering items as needed. All responsibility for providing and maintaining PPE and ensuring its use lies with the employer. The dentist/employer may not allow an employee to decline the use of PPE when there is a potential for exposure. For instance, the employer may not allow an assistant or hygienist to skip wearing a mask during procedures where there will be spray or spatter because they find it uncomfortable.
CDC
The Centers for Disease Control and Prevention issues guidelines and recommendations on numerous topics, including infection control. The Guidelines for Infection Control in Dental Health-Care Settings—2003 explain the various types of PPE and provide guidance in the use and selection of gloves, gowns,masks, and eyewear.2 In addition, the guidelines address such issues as jewelry, fingernails, and the storing and dispensing of handcare products. Although the CDC is not a regulatory agency, the guidelines from the CDC often serve as the basis for regulations by federal and state agencies.
Blood Exposure
The greatest concern among most DHCP is exposure to blood and other body fluids that may contain blood. The CDC guidelines for infection control in dentistry emphasize the importance of Standard Precautions.2 Standard Precautions expand the concept of Universal Precautions, which consider all blood and body fluids that might contain blood as infectious because some patients with bloodborne infections may be unaware of their status. Standard Precautions include not only blood and body fluids suspected of containing blood, but all body fluids, excretions, and secretions with the exception of sweat. The infection control precautions taken by the office team should be consistent for all patients and not based on the infectious status of the patient. PPE is a major component of Standard Precautions.
Personal Protective Equipment
The use of rotary handpieces, air/water syringes, and other instruments creates a spray that contains droplets of water, saliva, blood, microorganisms, and other debris. The smallest particles of these are aerosols. Aerosols are particles that are small enough to enter the respiratory system of individuals who are in their presence. Aerosols are capable of remaining suspended in the air for prolonged periods of time, and can be inhaled into the respiratory system of DHCP who are not wearing appropriate PPE.3 Both droplets and aerosols may contain infectious particles from the body fluids of the patient undergoing treatment.
Masks, Eyewear and Face Shields
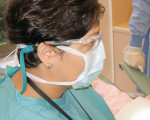
A surgical mask with at least 95% bacterial filtration efficiency will protect DHCP from the large-particle droplets generated during dental procedures. The mask also protects patients against microorganisms generated by the wearer. In fact, in the beginning, masks were there to protect surgical sites from infection by contamination from the healthcare worker. It was only in later years that workers began viewing the mask as a protective means to prevent patient-to-worker disease transmission. Outer contamination of the mask from droplets, spray, and touching, as well as from moisture caused by breathing in the mask, increases the resistance to airflow through the mask, causing more airflow to pass around the edges of the mask. This increases the risk of inhalation of aerosols. For these reasons, masks should be changed when they become wet. DHCP should avoid touching the outside of the mask with contaminated gloves to help prevent the opportunity for cross-contamination later when removing the mask.
Anytime that it is necessary to wear a mask, it is also necessary to wear eye protection (Figure 1). The same droplets and aerosols that may enter the respiratory system may also enter the eyes of the DHCP, creating a risk of disease transmission. Numerous infections, including herpes simplex and hepatitis C, can transmit via contact with the eyes. Because of the nature of the spray that dental devices generate, eye protection should either have side shields or consist of a chin-length face shield.
Protective Clothing
Protective clothing, usually a gown or lab coat, protects skin, street clothes, and work clothes from contact with blood and OPIM. The clothing must be adequate to cover all areas exposed to droplets from dental devices during the procedure and during clean-up or laboratory work. There are no regulations or guidelines defining the type of material or other properties, such as fluid resistance for protective clothing. Because of the nature of most dental procedures, a coat or gown with long sleeves is necessary to protect the forearms from spray (Figure 2). DHCP should change clothing daily or when it becomes visibly soiled and as soon as feasible if penetrated by blood or OPIM. OSHA requires the removal of all protective clothing before leaving the work area. OSHA also requires that the employer launder or replace the protective clothing. This requirement does not extend to a uniform or scrubs worn under the gown or lab coat. These items are considered the work clothes and are not part of the PPE.
Gloves
Medical gloves protect DHCP from contact with patient's blood and OPIM and protect the patient from microorganisms that may be present on the DHCP's hands. Medical gloves are for single-use only and should not be washed or decontaminated for reuse. If a glove becomes cut, torn, or punctured during use, DHCP should remove their gloves, wash their hands and re-glove before continuing the procedure. Hand washing is an important part of gloving, since wearing gloves does not eliminate the need for proper hand hygiene. Bacteria on a DHCP's hands may contaminate gloves during donning, and small imperceptible defects in gloves and the removal of gloves may result in the contamination of the DHCP's hands. Therefore, it is important to perform hand hygiene procedures before donning gloves and again after removing gloves.
Nonsterile medical exam gloves are appropriate for most routine dental procedures. These gloves are available in a wide variety of materials including latex, vinyl, nitrile, and many synthetic formulations. Gloves are not impervious to tears, cuts, holes, and damage due to exposure to chemicals such as germicides, antiseptics, resins, and bonding agents. There are steps DHCP can take to minimize the risk of glove damage during use. To maximize glove performance, DHCP should consider maintaining short fingernails, eliminating hand jewelry, and avoiding injury with sharp instruments and devices.
The CDC recommends the use of sterile surgical gloves for oral surgical procedures. Sterile gloves are more rigorously regulated than exam gloves, providing an extra layer of assurance for glove performance. Additionally, sterile gloves minimize the transmission of microorganisms from the hand of surgical DHCP to patients.
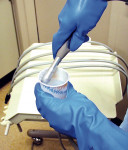
Some DHCP prefer to use double gloves when treating patients. There is a lack of evidence showing that double gloves are more effective in preventing disease transmission than single gloves. However, there is evidence that that there is a lower frequency of inner glove perforation and visible blood on the surgeon's hands when double gloves are worn. Studies specific to dentistry show that the perforation of outer latex gloves was greater during longer procedures, and that the highest rate of glove perforation occurred during oral surgical procedures. Because double gloving does not appear to reduce either manual dexterity or tactile sensitivity, it remains a personal, professional decision as to whether or not to double glove. Heavy-duty gloves are not appropriate for patient care, but protect workers' hands during clean-up and when handling certain chemicals (Figure 3).
Conclusion
Instrument reprocessing using appropriate cleaning methods and materials is an important part of the dental infection-control program. Personnel responsible for this important duty must receive proper training in the rationale for the procedures and the potential consequences of failure to follow all of the appropriate steps. Blood, tissue, and other debris left on dental instruments through the sterilization cycles may impair the sterilization process.
References
1. Kohn WG, Collins AS, Cleveland JL, et al. Guidelines for infection 1. Department of Labor, Occupational Safety and Health Administration. Safety and Health Topics: Bloodborne Pathogens and Needlestick Prevention page. Available at: https://www.osha.gov/SLTC/bloodbornepathogens/. Accessed February 26, 2007.
2. Kohn WG, Collins AS, Cleveland JL, et al. Guidelines for infection control in dental health-care settings—2003. MMWR Recomm Rep. 2003;52(RR-17):1-61.
3. Harrel SK, Molinari J. Aerosols and splatter in dentistry: a brief review of the literature and infection control implications. J Am Dent Assoc. 2004:(135)4;429-437.
About the Author
Eve J. Cuny, RDA, MS
Assistant Professor, Director of Environmental Health and Safety
University of the Pacific Arthur A. Dugoni School of Dentistry
San Francisco, California