AAE/AAOMR Recommendations for the Use of CBCT in Endodontics
Case examples and discussion
By Trent Lally, DDS, MSD
Limited field of view (FOV) cone-beam computed tomography (CBCT) has become a staple in endodontic practices. Its advantages over 2-dimensional imaging and usefulness in endodontics have been well-documented in dental literature.1,2 It is a useful tool when navigating clinically complex endodontic scenarios. Traditional periapical images only provide a 2D image of a 3D structure. Oftentimes, clinical interpretation of conventional radiographs can be obstructed by superimposition of the teeth and the surrounding dentoalveolar structures.3 Due to the placement of traditional sensors intraorally, conventional radiology often results in geometric distortion (eg, foreshortening, elongation) of the resultant image. The zygomatic process, maxillary and mandibular tori, oblique ridges, anterior nasal spine, and other anatomical structures frequently obscure the view of the root apex.
Although CBCT is very useful clinically, the large majority of endodontic cases are treated and completed using conventional imaging. After a comprehensive clinical evaluation, cases should be carefully evaluated to determine whether or not CBCT is indicated or could provide an advantage over conventional imaging alone. In 2010, the American Association of Endodontists (AAE) and the American Academy of Oral and Maxillofacial Radiology (AAOMR) released a joint position statement on the use of CBCT in endodontics.4 In 2015, the organizations updated their position statement and added 12 recommendations for the use of CBCT.5 The recommendations emphasize that CBCT should be used only when the patient’s history and clinical examination indicate a benefit that outweighs any potential risks. In other words, in the absence of specific clinical signs and symptoms, routinely using CBCT for diagnosis is not recommended.5 Clinicians should utilize CBCT only when the imaging needs cannot be met by intraoral radiography.6 AAE states that conventional intraoral radiography remains the most cost-effective, high-resolution imaging modality for most endodontic treatments.6
For those specific scenarios in which additional information may be needed, CBCT scans can offer supplementary image data that is likely to improve the outcome of a case. The 2015 AAE/AAOMR statement offers several recommendations to clinicians regarding the use of CBCT. This article highlights several of the recommendations from the 2015 AAE/AAOMR statement regarding the use of CBCT and provides clinical cases as examples. The remaining recommendations were omitted because they simply reinforce the importance of intraoral radiographs in routine preoperative and postoperative assessment, as well as implant planning.
Recommendation 2: Limited FOV CBCT should be considered the imaging modality of choice for diagnosis in patients who present with contradictory or nonspecific clinical signs and symptoms associated with untreated or previously endodontically treated teeth.
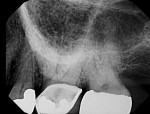
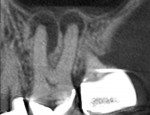
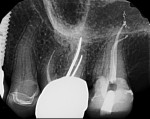
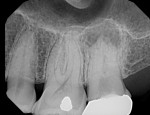
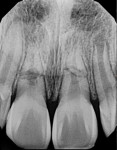
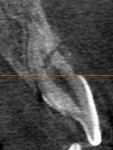
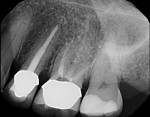
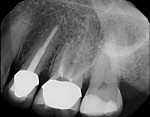
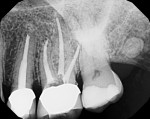
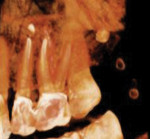
In case 1, A 61-year-old female presented to the office with the chief complaint of feeling “pressure” in her upper right quadrant. Clinical findings were inconclusive because tooth No. 14 and tooth No. 15 were nonresponsive to both periapical and pulpal testing. A small volume CBCT scan was taken to further evaluate the sextant. Note the large periapical radiolucencies on the buccal roots that could not be identified on the 2D periapical image (Figure 1 and Figure 2).
Recommendation 3: Limited FOV CBCT should be considered the imaging modality of choice for initial treatment of teeth with the potential for extra canals and suspected complex morphology, such as mandibular anterior teeth, and maxillary and mandibular premolars and molars, and dental anomalies.
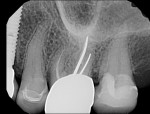
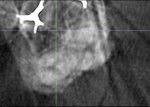
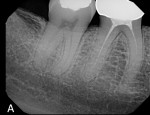
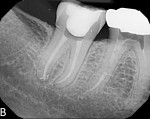
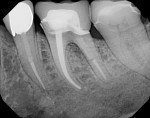
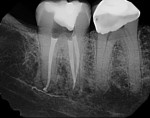
Case 2 involves a 68-year-old female who presented with a chief complaint of thermal sensitivity after a carious pulpal exposure during crown preparation. The tooth was diagnosed with symptomatic irreversible pulpitis, and root canal therapy was recommended. Upon access, both a buccal and palatal canal were located and instrumented. A CBCT scan was recommended to rule out the possibility of a calcified distal buccal canal. A cross section of the buccal root confirmed the presence of only one buccal canal, so the case was obturated (Figure 3 through Figure 5). Without the CBCT scan available, a clinician would have had to trough in order to rule out the presence of a third canal, which would have unnecessarily weakened the remaining tooth structure, possibly risked perforation, and increased the treatment time. Sometimes, CBCT scans can be just as useful in ruling out the possibility of hidden canals as they are in locating missing canals.
Recommendation 4: If a preoperative CBCT has not been taken, limited FOV CBCT should be considered as the imaging modality of choice for intra-appointment identification and localization of calcified canals.
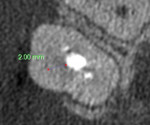
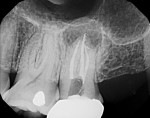
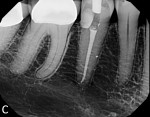
In case 3, a 37-year-old female was referred to the office for root canal therapy on tooth No. 15 prior to replacement of her crown. She reported no pain or swelling; however, a periapical radiolucency was noted. The tooth was diagnosed with pulp necrosis and asymptomatic apical periodontitis for which root canal therapy was recommended. The tooth was accessed and the mesial buccal and palatal canals were located. Because the distal buccal canal could not be located due to severe calcification, calcium hydroxide was placed, and a CBCT scan was taken to help identify the location of the canal. Although the canal itself could not be visualized on the image, its approximate location was measured to be 2 mm towards the distal buccal line angle (Figure 6 through Figure 8). Searching for a calcified canal in this manner reduces the risk of perforation. The canal was then located and the case was obturated.
Recommendation 6: Limited FOV CBCT should be considered the imaging modality of choice if clinical examination and 2D intraoral radiography are inconclusive in the detection of vertical root fracture.
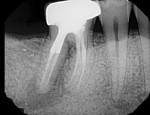
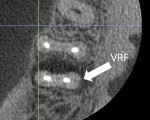
The 44 year-old male in case 4 was referred for retreatment of tooth No. 30. The patient presented with a sinus tract and an 8-mm isolated probing depth on the distal lingual line angle. A CBCT scan was taken, which revealed a potential vertical root fracture adjacent to the narrow probing depth (Figure 9 and Figure 10). Because of the questionable prognosis with retreatment or apicoectomy, extraction was recommended to the patient, thus saving time and financial resources.
Recommendation 7: Limited FOV CBCT should be the imaging modality of choice when evaluating the nonhealing of previous endodontic treatment to help determine the need for further treatment, such as nonsurgical, surgical, or extraction.
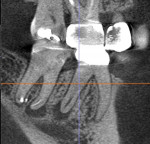
Case 5 involves a 51-year-old patient who presented to the office for a reevaluation of tooth No. 30 and tooth No. 31. When the patient was seen 7 months earlier by another endodontist, tooth No. 30 was asymptomatic, and tooth No. 31 was painful when exposed to heat and cold. Retreatment was recommended for tooth No. 30, and root canal therapy was recommended for tooth No. 31. During the retreatment of tooth No. 30, the previous provider encountered a hard-set, paste-type obturation material that he could not remove from the mesial canals. Calcium hydroxide was placed in the distal canal, and then extraction was recommended to the patient. After root canal therapy was completed on tooth No. 31, and it was restored with a crown, both teeth presented with periapical radiolucencies (Figure 11 through Figure 13).
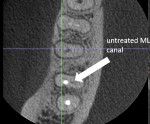
A CBCT scan was taken to further evaluate both teeth (Figure 14 and Figure 15). Two important findings were noted: First, the radiolucency on tooth No. 30 was limited to the distal canal. Second, an uninstrumented mesial lingual canal was noted on tooth No. 31. Both lesions were addressed through nonsurgical endodontic retreatment.
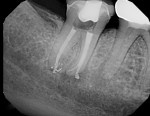
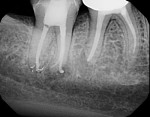
Because it was symptomatic, tooth No. 31 was treated first. The uninstrumented canal was successfully located and treated. Tooth No. 30 was treated at a subsequent visit (Figure 16 and Figure 17). The mesial buccal canal obturation was improved, but the hard-set material prevented complete obturation to the apex. However, if this root were to develop a lesion in the future, it could be addressed with apicoectomy. Both teeth were coronally restored with composite resins.
Recommendation 8: Limited FOV CBCT should be the imaging modality of choice for nonsurgical retreatment to assess endodontic treatment complications, such as overextended root canal obturation material, separated endodontic instruments, and localization of perforations.
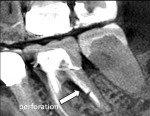
In case 6, a 61-year-old female patient was referred for evaluation of tooth No. 19, which had undergone root canal treatment 5 years earlier. She did not report any pain or swelling. A lateral radiolucency was noted in the furcation, and a resin-type post was present in the distal root. A suspected strip perforation was confirmed with the CBCT image (Figure 18 and Figure 19). The prognosis was determined to be unfavorable due to the size and long-standing nature of the perforation, so extraction was recommended.
Recommendation 9: Limited FOV CBCT should be considered as the imaging modality of choice for presurgical treatment planning to localize root apex/apices and to evaluate the proximity to adjacent anatomical structures.
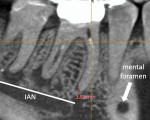
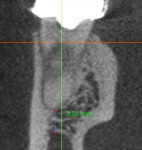
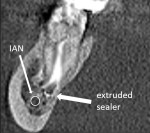
Case 5 also can be used as an example of presurgical planning. In the case, the goal was to address the periapical lesion on the distal of tooth #30 through nonsurgical therapy. Because completely negotiating the mesial canals to the apex was not achievable, a possibility exists that this root may develop a lesion in the future. Although the proximity of the root apex to anatomic structures can contraindicate surgical treatment, in this case, the preoperative CBCT image confirmed that the root apex was approximately 4 mm to 5 mm from the inferior alveolar nerve canal, so endodontic root end surgery remained a feasible treatment option (Figure 20 and Figure 21). In addition, while incising or reflecting tissue, it is important to note the location of the mental foramen in order to prevent severing or impinging the inferior alveolar nerve or artery.
Recommendation 11: Limited FOV CBCT should be considered the imaging modality of choice for diagnosis and management of limited dentoalveolar trauma, root fractures, luxation, and/or displacement of teeth and localized alveolar fractures, in the absence of other maxillofacial or soft tissue injury that may require other advanced imaging modalities.
The 11-year-old patient in case 7 fell forward and struck his maxillary central incisors on concrete. Since the incident occurred, he reported no pain or swelling, and both teeth were non-tender to percussion and palpation. Tooth No. 8 exhibited a diminished response to cold, while tooth No. 9 exhibited a normal response. A CBCT scan was taken to further evaluate tooth No. 8 and determine if any bone loss occured adjacent to the horizontal fracture lines (Figure 22 and Figure 23). Upon examination, the surrounding bone appeared within normal limits. No treatment was recommended at this time; however, the patient was scheduled to be reevaluated for signs and symptoms of pulp necrosis at 3 months, 6 months, 12 months, and yearly thereafter.
Recommendation 12: Limited FOV CBCT is the imaging modality of choice in the localization and differentiation of external and internal resorptive defects and the determination of appropriate treatment and prognosis.
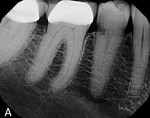
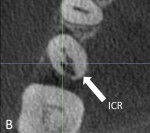
In case 8, a 57-year-old female was referred for evaluation of tooth No. 29. After a Class 2 invasive cervical resorption lesion was noted on the periapical image, a CBCT scan was taken to evaluate the true extent of the lesion (Figure 24 through Figure 26). When examining the transverse plane, the resorption was in close proximity to the canal space. Root canal therapy was completed on tooth No. 29 so that the lesion could be more aggressively treated. The affected tissue was surgically removed, then the resorption was treated with trichloroacetic acid and restored with Geristore (DenMat).
Discussion
CBCT scans can be beneficial at almost all stages of treatment. Preoperatively, they can be used for treatment planning, diagnosis, assessment of resorptions, identification of missed canals, evaluation of traumatic dental injuries, identification of possible vertical root fractures, and endodontic presurgical planning.
Case 1 provides an example of the superimposition of anatomical structures, such as the zygoma, that can prevent the detection of periapical lesions. In addition to those obscured by anatomy, CBCT can also detect periapical lesions that are not large enough to be seen on conventional periapical radiographs. In order for a lesion to be visualized on conventional radiographs, it must involve some degradation of the cortical bone, thus any lesions limited to the cancellous bone can go undetected.7
Case 2 and case 3 represent the use of intraoperative CBCT scans. In cases involving calcified canals, clinicians should first access the chamber and make a conservative search for the canal. If the canal does not present itself, than a limited volume CBCT scan may be taken. Information from the scan serves to orient the clinician, so he or she can locate the canal at the next appointment. Oftentimes, crowns will be angulated to correct occlusion despite alteration of the coronal anatomy. This can make finding calcified canals difficult if our usual reference points, such as cusps and fossae, have moved. In both cases, the images could have been taken preoperatively. However, because the presence of the canals in case 2 was suspected based on the preoperative periapical radiograph, if all of the canals had been located, there would have been no need for a CBCT scan. Therefore, taking one preoperatively would have provided little diagnostic benefit, while also exposing the patient to unnecessary ionizing radiation. In addition, as case 3 demonstrates, accessing first not only gives the clinician the opportunity to perform a conservative search for the canal, but also to use the depressions created from troughing as reference points to locate the canal should a CBCT scan be necessary. Other authors have outlined additional intraoperative uses of CBCT, which include the evaluation of unexpected anatomic findings and the assessment of iatrogenic errors, such as perforation and events associated with fractured instruments and extruded obturation materials.8
Case 5 was also heavily influenced by the information obtained from the CBCT scan. Initially, tooth No. 30 was recommended for extraction by a previous endodontist. However, the patient expressed a desire to maintain the tooth. The tooth was reevaluated, and it was determined that the lesion on the distal canal could be addressed by treating the canal space. This lesion was not present at the patient’s initial visit and likely developed as a result of incomplete treatment and failure to properly seal the access. Although the discovery of the hard-set paste material presented a hindrance to treating the mesial canals, it was determined from measurements made on the CBCT that an apicoectomy could address this root should the tooth develop a lesion in the future. Tooth No. 31, however, could not be addressed surgically because the inferior alveolar nerve canal prevented access to the root tips. Fortunately, it was determined that an untreated canal was present, and that it could be located using the mesial buccal canal as a reference point.
Postoperatively, CBCT scans can be used to evaluate overextended or overfilled obturation materials. Both the inferior alveolar nerve canal and the mental foramen can be in close proximity to the mandibular molar roots and mandibular premolar roots.9,10 Extruded materials may appear close to these structures and can result in involvement of the nerve.11 If nerve involvement is suspected, a CBCT scan can and should be taken. Another appropriate use of CBCT is in the assessment of cases involving persistent pain for which a CBCT scan was not initially taken. This may identify missed canals, iatrogenic errors, and potentially nonodontogenic sources of persistent pain (Figure 27 through Figure 31). It’s important to evaluate the dentoalveolar structures, bone, sinuses, and soft tissue when assessing the scan.
Clinically, CBCT provides a significant amount of additional information to a case. Ultimately, this is due to its ability to eliminate the superimposition of the surrounding structures. For selected cases, CBCT can have a large impact on both diagnosis and treatment outcomes.
References
1. Patel S, Dawood A, Mannocci F, Wilson R, Pitt Ford T. Detection of periapical bone defects in human jaws using cone beam computed tomography and intraoral radiography. Int Endod J. 2009;42(6):507-515.
2. Cotton TP, Geisler TM, Holden DT, Schwartz SA, Schindler WG.. Endodontic applications of cone-beam volumetric tomography. J Endod. 2007;33(9):1121-1132.
3. Schwartz SF, Foster JK. Roentgenographic interpretation of experimentally produced bony lesions. Part I. Oral Surg Oral Med Oral Pathol. 1971;32(4):606-612.
4. AAE, AAOMR.. Use of cone-beam computed tomography in endodontics Joint Position Statement of the American Association of Endodontists and the American Academy of Oral and Maxillofacial Radiology. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2011; 111(2):234-237.
5. AAE, AAOMR. AAE and AAOMR joint position statement: use of cone-beam computed tomography in endodontics 2015 update. J Endod. 2015;41(9): 1393-1396.
6. Cone Bean-Computed Tomography in Endodontics. ENDODONTICS: Colleagues for Excellence. Summer 2011. https://www.aae.org/uploadedfiles/publications_and_research/endodontics_colleagues_for_excellence_newsletter/ecfe%20summer%2011%20final.pdf. Accessed July 20, 2017.
7. Bender IB, Seltzer S. Roentgenographic and direct observation of experimental lesions in bone: I. J Am Dent Assoc. 1961;62(2):152-160.
8. Ball RL, Barbizam JV, Cohenca N. Intraoperative endodontic applications of cone-beam computed tomography. J Endod. 2013;39(4):548-557.
9. Denio D, Torabinejad M, Bakland LK. Anatomical relationship of the mandibular canal to its surrounding structures in mature mandibles. J Endod. 1992;1 8(4):161-165.
10. Phillips JL, Weller RN, Kulild JC. The mental foramen: 1. size, orientation, and positional relationship to the mandibular second premolar. J Endod. 1990;16(5):221-223.
11. Mohammadi Z. Endodontics-related paresthesia of the mental and inferior alveolar nerves: an updated review. J Can Dent Assoc. 2010;76:a117.
About the Author
Trent Lally, DDS, MSD
Private Practice
Phoenix, Arizona