Evolving with Implant Dentistry
Implement digital technology to enhance accuracy, predictability, and efficiency
Scott Frank, DDS
Dental implants osseointegrate. This is great news, but certainly old news. Today, dental implants are well accepted as a valid and predictable treatment modality in dentistry. However, to get here, implant dentistry has undergone an evolution through the decades. In the 1980s, studies and efforts focused on the success rates and predictability of osseointegration.1 By the 1990s, osseointegration was well accepted and restorative-driven implant placement was developed to enhance restorative outcomes.2,3 Additionally, hard and soft tissue regeneration emerged to address deficits to enhance dental implant placement.4
In the 2000s, attention was directed toward anatomic and esthetic implant placement.5,6 Parameters such as implant depth, implant-tooth distance, implant-implant distance, and labial-palatal implant position were established to strive for ideal gingival margin position and papilla maintenance/regeneration.7-11 The benefits of immediate implant placement and immediate provisionalization were introduced as well.12,13
And now, in the 2010s, digital technology affords accurate planning and implementation, which leads to less patient visits, shorter treatment time to restoration, fewer complications, and more predictable outcomes.
So what, exactly, is digital technology in dentistry? Essentially, it refers to technology in dentistry that uses computers. Currently, most dentists are using some form of digital dental technology in their practice. Such technology might include digital radiology, intraoral imaging, CAD/CAM restorations, practice management software, electronic medical records, caries diagnosis, and shade matching. In addition, the use of digital technology has also improved implant dentistry, including the implementation of cone-beam computed tomography (CBCT) scanning, intraoral optical scanning (ie, digital impressions), implant planning software, and 3-dimensional printing/milling (eg, CT generated surgical guides, models, provisionals, final restorations). The seamless integration of digital technology results in higher precision and accuracy with enhanced efficiency and simplicity.
Utilizing digital implant technology can lead to many benefits for patients and for the practice. One significant benefit is enhanced diagnosis, treatment planning, and communication. Analog work-up involves a time-consuming process of creating models and provisionals and relating wax-ups to superficial anatomy, whereas digital implant dentistry allows the practitioner to create virtual restorative “wax-ups” in minutes. More importantly, the proposed restoration can immediately be related to superficial and deep anatomy. Anatomical deficiencies, vital structures, osseous contours, and volume can be quickly evaluated as related to the proposed implant position to create an ideal restoration.
In addition, the virtual restoration and proposed implant position can be easily shared with colleagues for collaboration as well as with patients to educate them about proposed treatments. Once finalized, a surgical guide can be fabricated, allowing for a predictable and efficient transfer of the virtual plan to the patient.
Another significant benefit is increased probability of immediate implant placement. The patient experience is greatly enhanced when implants can be immediately placed. This results in a shorter time to completion and less appointments.
For a single tooth, the number of appointments is reduced from 10 visits to 6 visits. Total treatment time can be reduced from 8 to 10 months to 3 to 4 months. Oftentimes, an immediate provisional restoration may be placed, eliminating the need for removable provisional prostheses.
Because implants are placed ideally per the virtual surgery, optimal esthetics become predictable. Without digital implant technology, it is difficult, if not impossible, to complete the osteotomy within the socket while ensuring primary stability and ideal implant position for an esthetic restoration. Utilizing digital technology also allows for optimization of the best available bone prior to surgery. Rather than evaluating and planning during surgery, clinicians can immediately implement the virtual surgical plan.
It can be difficult to “make a hole within a hole,” therefore, CT-guided placement of an implant within a socket is much more practical and predictable. In addition, because digital implant dentistry utilizes a flapless or minimal flap technique with shorter surgery time, patients report less postoperative pain and swelling.
Another benefit of digital implant dentistry results from the accuracy of implant placement. Digital impression eliminates the concerns associated with distortion from traditional impressions and models. Digital impressions can be immediately assessed and quickly rescanned when indicated. A virtually planned, restoration-driven approach eliminates unsupported materials, undesirable screw access, and poor esthetics. Even experienced surgeons acknowledge less than favorable results occur occasionally when using analog surgical guides or no guide. In these situations, the utilization of CBCT scans post-implant placement has revealed unintended proximity to vital structures and atypical anatomy, perforation of a lingual concavity, and injury to nerve structures or the maxillary sinus. Immediate placement and provisionalization results in improved tissue esthetics, reduced chair time leads to improved profitability, and great patient experiences are typical.
Much research exists debating the true accuracy of fully guided implant placement utilizing digital technology. Numerous articles conclude that implants placed utilizing digital planning achieve higher precision and accuracy in shoulder, apex, and angulation.14-17 However, despite the improvement from non-digitally planned templates, a margin of error still exists, and it is statistically significant enough to debate whether the result is truly “accurate.”
This is important to consider, especially when intending to place fully prefabricated provisionals based on virtually planned dental implants. A high level of accuracy in depth, angulation, and rotational position is required to ensure that a completely pre-fabricated abutment and restoration will seat to a planned position. Although promising, the successful and predictable delivery of a prefabricated provisional on a virtually planned implant is still an emerging concept and not consistent at this time. Currently, achieving the benefits of digital implant technology is dependent on accurate implant placement in which the final position is predictable and results in ideal esthetic restorations with less surgery.
The following case demonstrates how digital implant dentistry benefits the implant surgeon, the restorative doctor, and most importantly, the patient.
Case Report
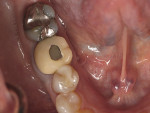
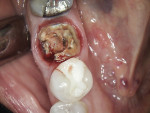
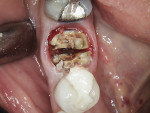
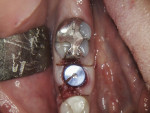
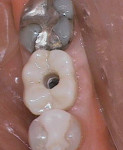
A 62-year-old healthy female presented with recurrent caries on tooth No. 30 (Figure 1). Tooth No. 30 was deemed non-restorable, and implant reconstruction was advised. A digital workflow was initiated for the flapless removal of tooth No. 30 and immediate implant placement.
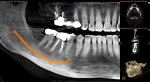
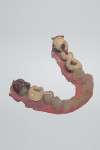
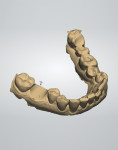
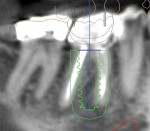
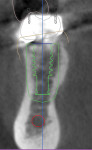
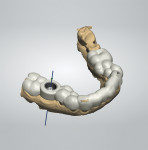
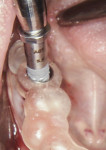
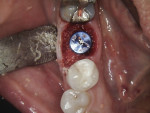
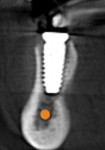
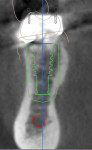
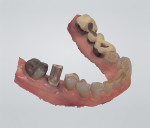
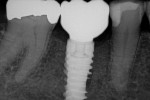
A CBCT image (Figure 2) and digital impression (Figure 3) were obtained for diagnosis and treatment planning. To facilitate this, the CBCT image and impression were merged into the implant planning software for evaluation. Tooth No. 30 was removed from the virtual model, and a virtual restoration was created (Figure 4). Next, the vital structures and osseous anatomy were identified, and a virtual implant was planned (Figure 5 and Figure 6). A virtual fully guided surgical template was created (Figure 7) and then sent to the in-office printer for guide fabrication (Figure 8 and Figure 9). Using a flapless technique, the crown of tooth No. 30 was removed, and the necrotic roots were sectioned and surgically removed (Figure 10 and Figure 11). Following this, the CT template was placed, the osteotomies were completed, and the implant was placed in a guided fashion with 60 Ncm of torque (Figure 12 and Figure 13). After the osseous socket was grafted with allogenic bone, a healing abutment was placed, and the tissue was stabilized without mobilization using 3-0 chromic sutures (Figure 14 and Figure 15). An immediate post-operative CBCT scan was used to verify that the implant was placed as planned (Figure 16 and Figure 17).
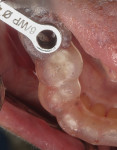
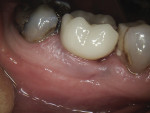
At 8 weeks following placement, the implant was confirmed to be osseointegrated. A final digital impression was obtained during the same visit using a scan body to capture the implant position (Figure 18). Next, the digital impression was uploaded to Artistic Dental Studio for fabrication of a model-less, screw-retained monolithic zirconium crown, which was delivered to the patient at 9 weeks following implant placement. The implant was ideally placed creating a centric screw access and well-supported ceramics for long-term predictability (Figure 19 through Figure 21).
Discussion
The benefits of digital implant technology for patients and practitioners are becoming clear. However, there is a natural evolutionary continuum through which experienced implant surgeons must first progress, which includes four stages:
1. Denial. The denial stage is characterized by the justification to not embrace digital implant dentistry. Thoughts include “it’s not necessary,” “it’s too expensive,” and “the technology is not yet developed.” It is often difficult for a clinician to significantly change his or her habits, and introducing digital implant technology requires notable changes. When learning new techniques and technology, the need for additional time and energy can cause discomfort. For some, this discomfort is undesirable and avoided.
2. Exception. Invariably, there will be a dental implant case that presents significant challenges for which precise implant placement becomes critical to avoid anatomic or esthetic challenges. With “exceptional” cases, digital implant technology may be recognized as beneficial. Although the unfamiliar process may be uncomfortable, obtaining the desired result is rewarding. Clinicians may experience multiple “exceptional” cases wherein they embrace the technology, but still reserve it for unusual patient circumstances.
3. Acceptance. As more “exceptional” cases are completed, a level of comfort with the technology, benefits, and costs develops. Clinicians begin to consider that if digital implant technology allows for more predictable outcomes in challenging scenarios, perhaps using it to obtain ideal outcomes for every patient is reasonable.
4. Adoption. Utilizing the available technology to obtain the best possible results in all cases becomes routine. The clinician realizes that any tool that enhances accuracy and predictability is ideal, and the benefits for patients and the practice become abundantly clear.
Once the acceptance stage is reached in the digital implant evolutionary progression, decisions will be made as to how and when to embrace the technology. Offsite services are available that require minimal to no purchases of equipment. DICOM and STL files may be uploaded for virtual planning, but a “closed platform system” requires surgical guide fabrication by the vendor. Analog models may also be sent to off-site vendors and converted to an STL file for virtual fabrication. Although in-house solutions require an initial capital expenditure and doctor/staff training, they allow for quick turnaround and cost-effectiveness long-term. Regardless of how the technology is implemented, when to adopt the technology is clear: the time is now. There will always be newer, faster, cheaper, and better technologies available. Embracing digital implant dentistry today positions doctors and their practices to benefit from the adoption and implementation of emerging advancements in digital technology tomorrow.
Conclusion
Digital technology is changing and enhancing many facets of daily life from the phones that we use to the cars that we drive. Dentistry is no exception. With digital technology, enhanced accuracy, predictability, and efficiency are realized from the initial diagnosis to the planning, communication, and implementation of proposed treatments. The benefits of digital implant dentistry are significant, thus it should be utilized to obtain the best possible outcome for every patient, whether the case is simple or complex. Recognize the stages of the digital implant evolutionary continuum, identify and understand the stage in which you currently exist, and plan to evolve. The future of digital implant dentistry is now.
References
1. Brånemark PI. Osseointegration and its experimental background. J Prosthet Dent. 1983;50(3):399-410.
2. Garber DA, Belser UC. Restoration-driven implant placement with restoration-generated site development. Compend Contin Educ Dent. 1995;16(8):796, 798-802, 804.
3. Minoretti R, Merz BR, Triaca A. Predetermined implant positioning by means of a novel guide template technique. Clin Oral Implants Res. 2000;11(3): 266-272.
4. Bahat O, Fontanesi RV, Preston J. Reconstruction of the hard and soft tissues for optimal placement of osseointegrated implants. Int J Periodontics Restorative Dent. 1993;13(3):255-275.
5. Jovanovic SA. Bone rehabilitation to achieve optimal aesthetics. Pract Periodontics Aesthet Dent. 1997;9(1):41-51.
6. Tischler M. Dental implants in the esthetic zone. Considerations for form and function. N Y State Dent J. 2004;70(3):22-26.
7. Salama H, Salama MA, Garber D, Adar P. The interproximal height of bone: a guidepost to predictable aesthetic strategies and soft tissue contours in anterior tooth replacement. Pract Periodontics Aesthet Dent. 1998;10(9):1131-1141.
8. Tarnow DP, Cho SC, Wallace SS. The effect of inter-implant distance on the height of inter-implant bone crest. J Periodontol. 2000;71(4):546-549.
9. Choquet V, Hermans M, Adriaenssens P, Daelemans P, Tarnow DP, Malevez C. Clinical and radiographic evaluation of the papilla level adjacent to single-tooth dental implants. A retrospective study in the maxillary anterior region. J Periodontol. 2001;72(10):1364-1371.
10. Tarnow D, Elian N, Fletcher P, Froum S, Magner A, Cho SC, et al. Vertical distance from the crest of bone to the height of the interproximal papilla between adjacent implants. J Periodontol. 200;74(12):1785-1788.
11. Ishikawa T, Salama M, Funato A, Kitajima H, Moroi H, Salama H, et al. Three-dimensional bone and soft tissue requirements for optimizing esthetic results in compromised cases with multiple implants. Int J Periodontics Restorative Dent. 2010;30 (5):503-511.
12. Zeren KJ. Minimally invasive extraction and immediate implant placement: the preservation of esthetics. Int J Periodontics Restorative Dent. 2006;26(2):171-181.
13. Funato A, Salama MA, Ishikawa T, Garber DA, Salama H. Timing, positioning, and sequential staging in esthetic implant therapy: a four-dimensional perspective. Int J Periodontics Restorative Dent. 2007;27( 4):313-323.
14. Shen P, Zhao J, Fan L, Qiu H, Xu W, Wang Y, et al. Accuracy evaluation of computer-designed surgical guide template in oral implantology. J Craniomaxillofac Surg. 2015;43(10):2189-2194.
15. Geng W, Liu C, Su Y, Li J, Zhou Y. Accuracy of different types of computer-aided design/computer-aided manufacturing surgical guides for dental implant placement. Int J Clin Exp Med. 2015;8(6):8442-8449.
16. Beretta M, Poli PP, Maiorana C. Accuracy of computer-aided template-guided oral implant placement: a prospective clinical study. J Periodontal Implant Sci. 2014; 44(4):184-193.
17. Scherer U, Stoetzer M, Ruecker M, Gellrich NC, von See C. Template-guided vs. non-guided drilling in site preparation of dental implants. Clin Oral Investig. 2015;19(6):1339-1346.