Phasing Restorative Treatment
Increasing case acceptance while reducing stress
Zachary S. Sisler, DDS
Phasing treatment for patients allows ideal restorations to be accomplished in an affordable and reasonable manner. Planned and executed during the course of 3 years, the following case (and winner of the 2017 Dawson Academy Study Club Challenge) demonstrates how to successfully phase treatment so that both ideal esthetics and function can be achieved over time.
Case Presentation
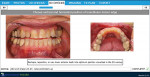
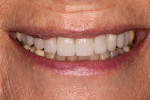
The patient, a 73-year-old female, presented with a chief complaint of unsatisfactory esthetics. During the initial comprehensive exam, moderate wear was found on the anterior teeth, resulting from suspected envelope of function issues (Figure 1).
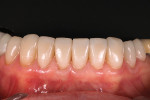
Her clinical findings and photographs were placed into the Dawson Diagnostic Wizard® (The Dawson Academy, www.thedawsonacademy.com). Of note was a high desire for esthetics, lateral pole clicks upon translation in both temporomandibular joints, and Dawson classification II (centric relation-maximum intercuspation discrepancy).1 The 2-dimensional analysis depicted that the upper incisal edge position was short of the inner vermilion border of the lower lip (Figure 2) due to the exhibited wear. Additionally, there was a lack of incisal embrasure and poor tooth form.
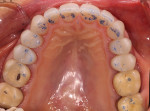
During the 3-dimensional analysis, the concavity of the lower anterior teeth was apparent and needed to be restored to a level plane (Figure 3). On the upper teeth, the goal would be to add length at the incisal edge to restore the anterior guidance that had been lost over time. This would also enhance the esthetic appeal to give a nice blend from anterior to posterior teeth.2
An ideal treatment plan for function and esthetics was developed to entail a full mouth rehabilitation. The patient was reluctant to accept this plan; therefore, a minimal plan was presented to prevent any further deterioration. The revised option consisted of an equilibration and eight crowns on teeth Nos. 5 through 12, along with bonded incisal composites on teeth Nos. 22 through 27. The patient ultimately decided to move forward with an “in-between” treatment plan involving an equilibration and crowns on teeth Nos. 4 through 13. This was chosen in an attempt to gain better esthetics on the upper, while maintaining bonded incisals on teeth Nos. 22 through 27.
Initial Treatment
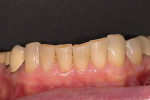
A silicon matrix was made from the diagnostic wax-up and transferred into the mouth to bond Nos. 22 through 27 with composite in a predictable fashion (Figure 4 and Figure 5).3 The provisionals were tested with the newly added length to ensure an adequate anterior guidance before placing final restorations.4 Additionally, the patient wanted to go with a whiter shade in the final restorations. Even though the patient was functionally stable at this point, the esthetics resulted in multiple shade variations between the new and old restorations (Figure 6).
Second Phase of Treatment
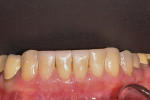
Two years later, the patient returned to upgrade the esthetics of her lower anterior teeth. In keeping treatment consistent, she chose to complete teeth Nos. 20 through 29 to achieve a better shade match and symmetry with the upper teeth that were previously restored (Figure 7). It is important to note that the sound occlusal foundation established in the transitional bonding could predictably be transferred into the final porcelain restorations while maintaining stable centric stops with anterior guidance in harmony with the envelope of function (Figure 8).5
Final Thoughts
Learning to phase treatment, as taught in The Dawson Academy Core Curriculum, is crucial. Phasing treatment allows the cost of treatment to be spread out over time, making it affordable for patients. Secondly, phasing treatment offers a much less stressful process than performing the full mouth rehabilitation all at once. Throughout this entire case, stable centric stops were maintained on posterior teeth, which made it easy to communicate vertical dimension to the lab. Although the patient initially was reluctant and not ready to accept a full mouth rehabilitation, performing it in smaller increments allowed the opportunity to gain her confidence and trust (Figure 9).
Acknowledgment
The author would like to thank Rick Shafer at Bay View Dental Lab for his beautiful porcelain work on this case.
References
1. Dawson P. Classification of occlusions. In: Functional Occlusion: From TMJ to Smile Design. St. Louis, MO: Mosby; 2007:103-112.
2. Olitsky J. Seven worst violations of smile design: achieve better esthetics by understanding common mistakes. Inside Dentistry. 2015;11(9).
3. Cranham J, Finlay S. Timeless principles in esthetic dentistry. Journal of Cosmetic Dentistry. 2012; 28:64-73.
4. Seeseman M. Diagnostic full-coverage provisionals for accurately communicating esthetic and functional. FERD – Provisionalization. 2008;2(2).
5. Rosenstiel S, Land M, Fujimoto J. Principles of occlusion. In: Contemporary Fixed Prosthodontics. 4th ed. St. Louis, MO: Mosby; 2006:110-144.
About the Author
Zachary S. Sisler, DDS
Dawson Academy Ambassador
Private Practice
Shippensburg, Pennsylvania
For more information, contact:
The Dawson Academy
888-844-0502
www.thedawsonacademy.com