Overcoming Obstacles to Provide an Esthetic Anterior Implant
A treatment plan for success
David Hornbrook, DDS
One of the most challenging restorative situations faced by dentists is replacing a missing anterior tooth with an implant while providing lifelike esthetics and harmony with the surrounding natural dentition or adjacent all-ceramic restorations.1 The challenges involved include placing the correct implant, managing soft tissue contours before and after the implant is placed, utilizing provisionalization that corrects gingival embrasure defects, choosing an implant abutment that provides a dentin shaded preparation, and selecting a definitive restoration. While a metal abutment (either stock or custom) provides long-term durability and strength, it can compromise the esthetic value of the final restoration and limit the restorative options available. This is especially true when the implant restoration is placed adjacent to natural teeth or additional all-ceramic restorations.2,3,4
Case Presentation
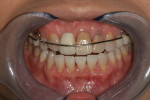
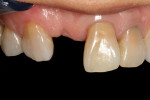
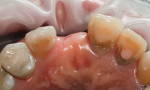
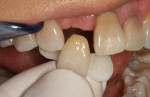
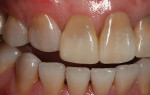
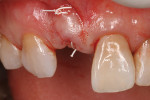
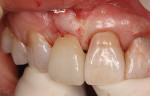
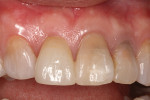
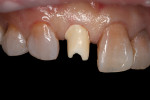
A 35-year-old female presented for a clinical exam with the desire to replace her missing central incisor and improve the appearance of her smile. At the time of presentation, she was utilizing a flipper to replace the missing tooth (Figure 1). She reported that she experienced trauma to the front of her mouth as a teenager, which resulted in the fracture of her maxillary right central incisor and the need for endodontic treatment on her maxillary left central and lateral incisors. The fractured right central was endodontically treated and restored with a metal post and a porcelain-fused-to-metal crown. In her early 20s, a vertical fracture of the root was diagnosed, so her treating dentist extracted the tooth and fabricated a maxillary flipper. She also reported that her mother was given tetracycline while she was pregnant, which resulted in tetracycline banding and staining on her remaining teeth, and that her maxillary right canine suffered from bony impaction (Figure 2 and Figure 3). Periodontal and temporomandibular joint disorder exams were within normal limits, and there were no other dental or health complications assessed that would delay or compromise further treatment. The patient’s goal was to replace her maxillary flipper and have a white and attractive smile. To facilitate this, the treatment plan was to perform a soft tissue graft, followed by implant and custom abutment placement. Next, ceramic restorations were to be placed on the abutment and her remaining maxillary anterior teeth and premolars.
Restorative Treatment Phase 1
The preliminary treatment plan began with referral to a periodontist to evaluate the patient for implant placement. It was determined by the periodontist that, to achieve ideal aesthetics, a connective tissue graft was warranted prior to implant placement. To help form the edentulous space and develop interproximal papilla, he recommended that a fixed bridge be fabricated and placed prior to the surgery, then removed, modified as necessary, and replaced at time of surgery to maintain the space until implant placement.5
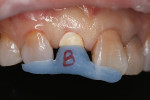
Due to the patient’s lack of anterior coupling, no tooth structure was removed from the lingual to facilitate the room required for the wings of the bridge. Typically, the lab prefers at least 1.0 mm clearance between the mandibular opposing teeth and the lingual preparations of the wings. Prior to fabrication, the laboratory created an ideal ovate pontic into the stone model. Next, a milled polymethylmethacrylate (PMMA) winged bridge was fabricated. PMMA was chosen due to its high esthetics, affordability, accurate fit, and ability to be modified at the time of placement and during healing by either removing material with a finishing disc or adding it using a flowable resin (Figure 4).6,7 After lab fabrication, a diode laser (Picasso Lite, AMD Lasers) was used to create an ovate pontic site into the ridge, and the bridge was lightly bonded into place by spot etching the lingual surface with phosphoric acid and then using a light-polymerized flowable resin. The PMMA yielded a very esthetic and stable provisional until the time of surgery arrived (Figure 5 and Figure 6).
Periodontal Surgery
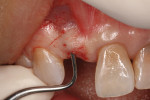
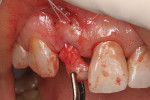
At time of gingival surgery, the surgeon removed the PMMA provisional, and a semi-circular incision was made at the ideal location for the new emergence of tooth No. 8. The incision was used to create the future ovate pontic shape and ideal emergence profile (Figure 7). An N-6900 microsurgical blade was used to create a tunnel for the placement of a connective tissue graft for ridge augmentation. This blade can also provide tactile sensation to determine the underlying bony topography. The microsurgical blade was inserted past the muco-gingival junction, and the dense fibrous connective tissue of the keratinized gingival tissue was freed to create a tunnel for a graft placement. A connective tissue graft harvested from the palate was used to help create a natural root prominence. A GORE-TEX® suture was inserted above the muco-gingival junction, lassoing the connective tissue graft and then exiting again in the alveolar mucosa near the original entry point. Delicate microsurgical tissue forceps are used to help guide the graft into position inside the tunnel (Figure 8). In this manner, the connective tissue graft was pulled into position to create a natural prominence of the missing tooth root, and the suture was tied off at the apical end (Figure 9). A coronal suture was also placed to stabilize the incisal end of the graft. After the graft was placed, the ovate pontic was modified and bonded into place using a flowable resin (Figure 10).8 After 2 weeks, healing was evaluated to determine surgical success and that the bridge was still tightly in place (Figure 11). This PMMA bridge remained in place for 3 months. After the 3-month healing period, a Nobel Biocare implant was placed and covered with soft-tissue, and the PMMA bridge was bonded back into place.
After an additional 3 months of healing, the implant was uncovered, and an implant transfer post was placed. Complete seating was verified using radiographs. After the impression was complete, an opposing impression and facebow transfer were taken. Next, a provisional abutment was put into place, the wings were cut off of the PMMA provisional bridge, and the pontic was hollowed out, filled with a Bis-acryl (Luxatemp, DMG), and placed over the provisional abutment. This abutment was then removed, and ideal contours were created between the hollowed out PMMA pontic and the margins of the provisional abutment. This provisional was then screwed into place.
Laboratory Procedure Phase 1
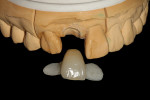
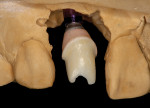
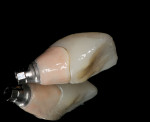
The decision was made to utilize an “H” abutment as the custom abutment. The “H” abutment incorporates a lithium disilicate that was waxed, pressed, shaded, and bonded to a titanium base. For the preparation component of the abutment, a shade was chosen to match the adjacent teeth, and a gingival shade (Gingival Shade Guide, Ivoclar) was chosen to match the surrounding gingival tissue (Figure 12).9 The coronal aspect of the lithium disilicate was etched with hydrofluoric acid to enhance adhesion to the overlying definitive restoration, and any subgingival part of the abutment was glazed and then polished. After abutment fabrication, an esthetic wax-up was done to meet smile design criteria, which included the remaining anterior dentition. After involving the patient in selecting a shade for the final restorations, a custom PMMA provisional was placed over the custom “H” abutment to blend into the wax-up and to be placed at the time of preparation and provisionalization of the remaining anterior teeth (Figure 13). Due to very accurate marginal integrity, the author prefers to place a lab fabricated PMMA provisional over the abutment. This allows the patient to floss normally around the implant abutment while in provisionals and ensures a healthy tissue response.
Restorative Treatment Phase 2
The abutment was seated into place using an acrylic jig to ensure correct orientation (Figure 14) and then torqued down using the manufacturers specifications (Figure 15). The remaining anterior teeth were prepared as conservatively as possible for all-ceramic restorations, impressed, and provisionalized. The PMMA provisional was cemented using a resin-based provisional cement (TelioLink, Ivoclar), and after the remaining provisionals were fabricated using a putty matrix of the wax-up and a Bis-acryl resin (Luxatemp, DMG), they were also cemented with the resin-based provisional cement (TelioLink, Ivoclar).
Laboratory Procedure Phase 2
The laboratory poured the models and, using the lost-wax casting technique, fabricated, pressed, cut back, and layered e.max lithium disilicate (Ivoclar) restorations over the abutment and the other anterior preparations.10 These restorations were then internally etched with hydrofluoric acid and sent to dental office.
Restorative Treatment Phase 3
Finally, the provisionals were removed, and all restorations were tried-in to verify accurate margination and esthetics. After try-in, the internal surface of the restorations was cleaned with phosphoric acid, rinsed, and dried. Next, a silane coupling agent was applied to the internal surface, allowed to sit for 60 seconds, and then thoroughly air-dried.11 A thin layer of unfilled resin (Porcelain Bonding Resin, Bisco) was applied to this internal surface and air-thinned, but not light-polymerized. The natural teeth were etched with phosphoric acid and rinsed thoroughly. To remove any contaminants, the “H” abutment was cleaned using a chlorhexidine scrub (Consepsis Scrub, Ultradent) and then etched with phosphoric acid as well. A dentinal primer (All-Bond 3, Bisco) was placed on all natural teeth in multiple coats, air-dried thoroughly, and then light-polymerized for 10 seconds per tooth. Next, a silane coupling agent was applied to the “H” abutment (Ceramic Primer, Bisco), allowed to sit for 60 seconds, and then air-dried thoroughly. All of the restorations were seated at one time using a light-polymerized resin cement (Variolink Veneer, Ivoclar) and the “Tack & Wave” technique.12 Excess resin cement was removed using a scaler, occlusion was checked and adjusted as needed using finishing diamonds (Brasseler), and the final polishing was completed with Diamond polishing paste (DiaShine, VH Technologies).
Conclusion
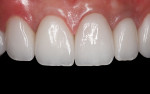
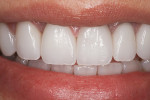
Success with anterior implants is a result of choosing the correct treatment plan and using the correct materials. Taking control of tissue contours prior to implant placement and during healing is paramount to achieving ideal tissue contours and maintaining interproximal gingival embrasures. Using a tooth-colored, bondable, custom abutment, such as the “H” abutment, provides an excellent foundation and an optimal base for an implant-supported crown to match either natural dentition or adjacent esthetic restorations. This case demonstrates an example of the materials needed and the teamwork required among the clinician, ceramist, and periodontist to yield optimal results and patient satisfaction (Figure 16 and Figure 17).
Disclosure
The author acknowledges that he has no financial interest in any of the products or techniques discussed in the case presentation. He would like to thank Utah Valley Dental Lab for fabrication of the abutment and definitive ceramic restorations and Dr. Peter Nordland, La Jolla, California, for his periodontal expertise and implant placement.
References
1. Cicciu M, Bereta M, Risitano G, Mairona C. Cemented-retained vs screw-retained implant restorations: an investigation on 1939 dental implants. Minerva Stomatol. 2008;57(4):167-179.
2. Sadid-Zadeh R, Liu PR, Aponte-Wesson R, O’Neal SJ. Maxillary cement retained implant supported monolithic zirconia prosthesis in a full mouth rehabilitation: a clinical report. J Adv Prosthodont. 2013;5 (2):209-217.
3. Sailer I, Zembic A, Jung RE, Hammerlee CH, Mattiola A. Single-tooth implant reconstructions: esthetic factors influencing the decision between titanium and zirconia abutments in anterior regions. Eur J Esthet Dent. 2007;2(3):296-310.
4. Gupta A, Jain D, Sangwan A, Chhabra S. Abutment options for compromised situation in esthetic zone-case reports. IOSR Journ of Dent and Med Sciences. 2015;14(8 Ver. II):30-37.
5. Salama H, Salama M, Garber D, Adar P. Developing optimal peri-implant papillae within the esthetic zone: guided soft tissue augmentation. J Esthet Dent. 1995;7(3):125-129.
6. Strassler H. In-office provisional restorative materials for fixed prosthodontics. Inside Dentistry. 2009;5(4). https://www.dentalaegis.com/id/2009/04/in-office-provisional-restorative-materials-for-fixed-prosthodontics.
7. Karaokutan I, Sayin G, Kara O. In vitro study of fracture strength of provisional crown materials. J Adv Prosthodont. 2015;7(1):27-31
8. Yoo, A, Bear A. Attached gingiva and dental implants. PerioImplant Advisory. 2014;5.
9. Hornbrook DS. Case report using the “H” abutment: achieving esthetics, strength, and predictability for the anterior implant. Compend Cont Educ Dent. 2015; 36(3):192-201.
10. Tysowsky GW. The science behind lithium disilicate: a metal-free alternative. Dent Today. 2009;28(3): 112-113.
11. Alex G. Preparing porcelain surfaces for optimal bonding. Compend Contin Educ Dent. 2008;29 (6):324-335.
12. Hornbrook DS. The “Tack & Wave” technique for placement of all-ceramic veneers. Contemporary Esthetics and Restorative Practice. 2002;6(4):36-48.
About the Author
David Hornbrook, DDS
Private Practice
San Diego, California